Using Technology to Restore Missing Dentition and Restore a Smile
Technologists face a shift in thinking and fabrication processes.
The term “paradigm shift” was coined 50 years ago by Thomas Kuhn in his book The Structure of Scientific Revolutions.1 In the book, Kuhn argues that scientific advancement is not evolutionary, but rather is a “series of peaceful interludes punctuated by intellectually violent revolutions,” and as a result of those revolutions, “one conceptual world view is replaced by another”.
Think of a paradigm shift as a transition from one way of thinking to another. It is a revolution, a transformation, or a sort of metamorphosis. It does not just happen, but rather is driven by agents of change. A paradigm shift is a constant. How much of it you recognize, internalize, or apply depends on how receptive you are to change.
For example, the www.ideafinder.com/history/inventions/printpress.htm">printing press, the production of books, and the use of common language changed the culture of people and had a direct effect on the scientific revolution. Johann Gutenberg’s invention in the 1440s of movable type was an agent of change. Books became readily available, smaller, and easier to handle as well as inexpensive to purchase.
Similarly, agents of change are driving a new paradigm shift in our personal lives today. The signs are all around us. For example, the introductions of the personal computer and the Internet have impacted both personal and business environments and are the stimulus for a paradigm shift. Newspaper publishing has morphed into websites, blogging, and web feeds. The Internet has enabled and accelerated the creation of new forms of human interactions through instant messaging, Internet forums, and social networking websites.
The dental technology industry is experiencing a similar shift. Since the inception of our industry, the accepted methods for fabricating fixed and removable prosthetics had incorporated the “lost-wax process.” The lost-wax process has been the best method for capturing exquisite detail and precision that could not otherwise be produced, given the complexity of the design. This process allows anything modeled in wax to be recreated fully into various metals and ceramic materials. However, the incorporation of computer-aided-design (CAD) and computer-aided-manufacturing (CAM) into the field of dental technology is changing the fundamental process by which our industry has been fabricating restorations, thus causing the paradigm shift we see today. The following case presentation is an example of this new shift.
The Challenge
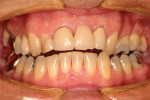
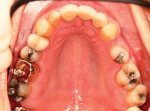
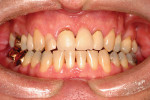
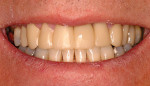
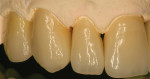
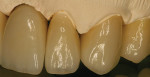
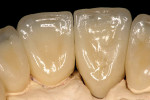
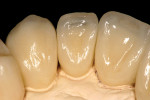
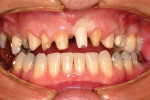
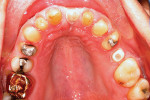
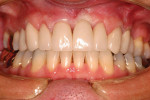
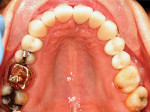
The patient presented to the dentist, and a treatment plan was instituted including tooth straightening. The patient was missing tooth No. 9, which had been replaced by an existing porcelain-fused-to-metal bridge. Tooth No. 13 also was missing, and tooth No. 12 had rotated and shifted into the open space. Following orthodontic treatment, restorative treatment called for implant placement to replace teeth Nos. 9 and 13. The patient was also unhappy with discolored fillings and an unpleasing anterior bridge (Figure 1 and Figure 2). Following the tooth-straightening procedure, the patient was ready for a new smile (Figure 3 and Figure 4).
The laboratory received the impressions, bite registration, and a model of the temporaries designed from the dentist’s wax-up, including transfer hardware. The dentist had produced a diagnostic wax-up and had fabricated temporaries based upon the wax-up. Photographs of the temporaries were also included (Figure 5).
Instructions were received with the case to fabricate custom zirconia abutments for teeth No. 9 and No. 13 and to fabricate IPS e.max® (Ivoclar Vivadent, www.ivoclarvivadent.com) crowns for teeth Nos. 6 through 11. Porcelain-fused-to-zirconia restorations were prescribed for teeth Nos. 4, 5, 12, and 13. The impressions were disinfected and the models were poured, pinned, and based according to laboratory protocol.
The Technology
Using the Origin® Intelligence™ scanner (B&D Dental Technologies, www.origincadcam.com), the models were scanned.
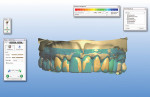
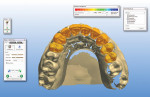
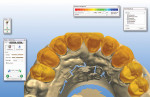
Traditionally, this case would be approached by duplicating the temporary model with a silicone matrix and injecting the mold with wax to reproduce the dentist’s temporary design. That wax-up would then be refined, invested, and pressed with the prescribed ceramic material. This technique is very time-consuming and labor-intensive. One of the unique benefits of current CAD/CAM technology is that in the design phase of the procedure, diagnostic wax-ups or temporary models can be scanned and incorporated into the design of the entire case—providing a highly accurate blueprint for the final restorations and a significant savings in labor (Figure 6 and Figure 7).
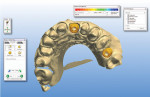
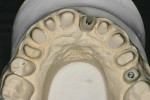
Origin® Custom Hybrid Abutments (B&D Dental Technologies) were chosen to provide the esthetic advantages of shaded zirconia. The close-tolerance, machined titanium interface provides an accurate fitting surface with the implant. The zirconia abutments were designed, milled from Origin® HS™ Zirconia (B&D Dental Technologies), sintered, and then cemented to the titanium interface for teeth Nos. 9 and 13. Using the ORIGIN® Intelligence™ implant module, the construction of custom zirconia implant abutments was easy and straightforward. The abutments were then screwed into the implant analogs and checked for accuracy and final inspection before scanning for fabrication of the restorations (Figure 8 and Figure 9).
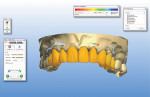
Upon completion of the custom zirconia abutments, the models were scanned and the restorations were then designed. Slight modifications were made to the temporary designs to reflect a more symmetrical proposal. These modifications were then e-mailed to the dentist for final approval before proceeding with the case (Figure 10 and Figure 11).
The six anterior restorations were designed in full contour, and the posterior zirconia restorations were designed with facial cutback for porcelain (Figure 12).
Following the design process, the crowns were then milled using IPS e.max® CAD blocks (Ivoclar Vivadent) and Origin® Live™ zirconia. After the anterior IPS e.max crowns were milled and the zirconia restorations were colored and sintered, the fit and occlusion were verified on the articulated model (Figure 13 and Figure 14).
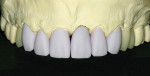
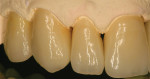
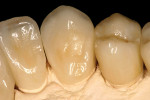
To obtain maximum esthetics the incisal/facial areas of the anterior crowns were cut back prior to the crystallization phase. The restorations were then crystallized according to the manufacturer’s guidelines. Following crystallization, the anterior restorations were layered with various IPS e.max porcelains to produce the desired incisal effects. IPS e.max porcelain was also used on the posterior porcelain-fused-to-zirconia crowns as well. The crowns were final-contoured and glazed (Figure 15 through Figure 20).
The restorations were delivered to the dentist, who removed the temporaries and torqued the custom zirconia abutments into place (Figure 21 and Figure 22). The crown restorations were then tried in, minimal adjustments were made, and then they were cemented into place (Figure 23).
Comparing the final outcome to the preoperative condition in Figure 1 and Figure 2, the esthetic and functional results that can be achieved by using technology can be seen (Figure 24
and Figure 25).
The Future
Becoming familiar and comfortable with any technology requires applying oneself to change. Change is difficult. Human beings resist www.schulersolutions.com/resistance_to_change.html change; however, the process was set in motion long ago, and we will continue to adapt and create our own experience. It all begins in the mind of the technologist. What is perceived—whether conventional or unconventional, conscious or unconscious—is subject to the limitations and distortions produced by an inherited and socially conditioned nature. However, perceptions are not restricted and are able to change. Once mastered, this technology can significantly reduce the amount of labor needed to produce highly esthetic and extremely accurate results and will continue to “shift” our thinking far into the future.
References
1. Kuhn TS. The Structure of Scientific Revolutions. 2nd ed. Chicago, IL: The University of Chicago Press; 1970.
About the Author
Lewis Sharp, CDT
Chief Executive Officer
Sharp Dental Lab
Elko, Nevada
Fig 1 and Fig 2. Preoperative and pre-straightening photographs.
Fig 3 and Fig 4. The patient following straightening and pre-restorative treatment.
Fig 5. Photograph of the temporaries from the dentist’s wax-up.
Fig 6. A model of the temporaries.
Fig 7. A 3D representation showing the temporary situation.
Fig 8. A proposal of the custom zirconia abutments.
Fig 9. The zirconia abutments on the working model.
Fig 10 and Fig 11. A 3D proposal of the final restorations.
Fig 12. The design of the posterior cutback.
Fig 13 and Fig 14. The milled restorations prior to crystallization.
Fig 15 through Fig 20. The final restorations.
Fig 21 and Fig 22. The zirconia abutments were placed in the mouth and torqued down.
Fig 23. The final restorations in place.
Fig 24 and Fig 25. Postoperative views of the patient.