High-Risk Esthetically Driven Restoration
Begin with the end in mind
A high-risk esthetically driven restorative case requires the dental team, along with the patient, to have a clear vision of the final outcome. In this case of a 33-year-old woman who wanted to improve her smile, esthetic problems stemmed from a retained deciduous maxillary left canine along with an impacted tooth No. 11. Among a number of concerns was the shape and color of the deciduous canine and the uneven length of the maxillary central incisors. A treatment plan that included orthodontics with removable aligners, occlusal adjustment, composite restorations, extraction and implant placement, indirect porcelain veneers, and a custom abutment and PFM crown was successfully executed in four phases over the course of more than 4 years.
When beginning a high-risk esthetically driven restorative case, it is important for the patient and the dental team to have a clear vision of the final outcome. It is often difficult for patients to articulate what they find esthetically undesirable. Sometimes, they are simply “unhappy” with their appearance. Part of the role of the laboratory is to gain an understanding of the patients’ esthetic concerns and discuss with the entire dental team the solutions that are available. These solutions may involve prolonged treatment plans that span many years before the desired outcome
is acheived.1
Clinical Case Overview
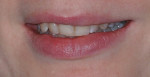
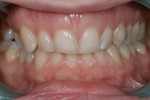
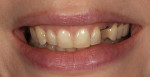
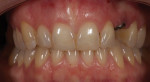
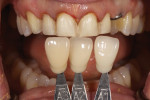
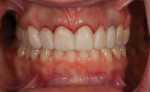
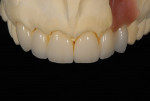
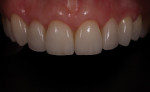
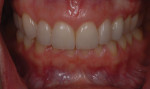
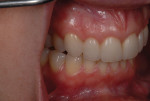
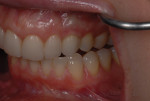
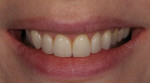
A 33-year-old woman presented for treatment in March 2007 desiring to improve her smile. She was developing a career in art sales and her smile hindered her confidence (Figure 1). She was aware that her front teeth had become shorter in recent years. She was also unhappy with the way the teeth on her right side “dipped in” and her canine (on the same side) “stuck out.” The left side had a retained deciduous canine (tooth H) with an impacted maxillary left canine (tooth No. 11). The shape and color of the deciduous canine was objectionable (Figure 2 and Figure 3).
The patient’s medical history was unremarkable. She had a past history of tobacco use but had been a nonsmoker for many years. Her dental history was limited to recall appointments and simple restorative procedures.
Diagnostic Findings, Risk Assessment, and Prognosis
Prognosis was established by taking the risk assessment into consideration as well as the age of the patient, the presence or absence of the contributing factors of disease, the expected lifespan of the patient, diet, and what the patient did with and to her teeth. Prognosis was determined without considering intervention so the patient could understand the potential outcomes if the disease process was left untreated.
Radiographs showed localized mild horizontal bone loss. Periodontal probe readings were generally 2 mm to 4 mm in depth, with slight bleeding on probing. The patient was placed on a 6-month periodontal recall. Based on existing bone levels, the periodontal diagnosis was deemed AAP type II.
The patient’s biomechanical risk was determined based on her current and past history. The patient presented with no new carious lesions, no structurally compromised teeth, and minimal erosion. She reported no new carious lesions in the past 4 to 5 years. She had some conservative posterior composite restorations and one amalgam restoration.
The patient showed mild to moderate attrition on her maxillary and mandibular anterior teeth with the most notable being on teeth Nos. 8 and 9. She had mild attrition on her bicuspids. The right and left temporomandibular joints were comfortable under load. The patient had no history of abnormal neuromuscular habits or bruxism, but felt as though she had more than one bite. A preliminary functional diagnosis of occlusal dysfunction was made, and later confirmed using the Kois deprogrammer.2
An accurate evaluation of the overall esthetics was challenging because of the patient’s guarded smile. Once relaxed, the patient laughed and it became apparent that she exhibited high lip dynamics. Since both the teeth and the tissue contours were visible in a full smile, the following esthetic deficiencies were noted: incisal edge position 0.5 mm short of ideal, 3 asymmetrical gingival architecture, intra-arch tooth position constricted in the maxillary bicuspid region, and dissatisfaction with the tooth shade.
Treatment Phases
Phase 1: Orthodontics
Removable orthodontic aligners (Invisalign®, Align Technology, Inc., www.invisalign.com) were offered as a treatment and accepted, with the explanation that the use of aligners would provide limited orthodontic intervention. Using the diagnostic wax-up as a guide, the arch was expanded in the bicuspid region on the right side, reducing the arch constriction. The anterior region was expanded slightly to create more space around the deciduous canine to facilitate future implant placement. Correcting the crossbite in the right posterior region was not a predictable move and, therefore, was not attempted. Approximately 1 mm of overjet was left in the maxillary anterior region in anticipation of future occlusal adjustment. Upon completion of the orthodontics, composite was placed on teeth Nos. 8 and 9 to lengthen the incisal edge position by 0.5 mm. With a more harmonized arch and adequate space around the deciduous canine, the teeth were in position to successfully complete implant placement and conservative restorative treatment.
Phase 2: Functional
Six months after completion of the orthodontic treatment, the patient was placed in a Kois deprogrammer to evaluate the occlusion.2 The patient’s first point of contact, with the temporomandibular joints in centric relation, was on the buccal incline of tooth No. 5. A centric relation bite record was made and the models mounted. Evaluation of the models confirmed the initial point of contact on tooth No. 5. A trial equilibration was done on the models to verify that even, simultaneous contacts could be achieved.
The patient returned for occlusal equilibration. Bilateral simultaneous posterior point contacts and canine guidance were achieved intraorally. The patient was functionally stable for 3 years, at which time she was ready to begin restorative treatment. During this time, no chipping or shortening of the direct resin placed on teeth Nos. 8 and 9 was observed (Figure 4).
Phase 3: Surgical
An oral surgeon extracted the impacted canine No. 11 via a palatal access approach. The deciduous canine was also removed at this time. The area was grafted and allowed to heal for 9 months. A 4-mm x 11-mm ASTRA TECH™ implant (DENTSPLY Implants, www.dentsplyimplants.com) was placed,4 and the patient wore a transitional removable partial denture during the healing time of 4 months (Figure 5).
Phase 4: Restorative
Teeth Nos. 6 through 10 were prepared for indirect porcelain veneer restorations (Figure 6). A new diagnostic wax-up was completed before the preparation appointment. Crown lengthening was completed at the time of the tooth preparation with a scalpel and a bone chisel.5 Approximately 0.5 mm of gingiva and bone were removed from teeth Nos. 7 through 9, and the final impression for the definitive indirect restorations for teeth Nos. 6 through 10 as well as the implant-supported crown were taken. Provisional restorations were fabricated with bis-acrylic using a putty matrix fabricated from the diagnostic mock-up. The teeth were spot-etched and the restorations were luted to the prepared teeth with a flowable composite resin (Figure 7).
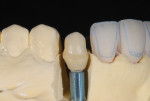
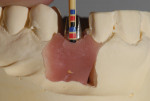
The relationship of the provisionals was transferred to the laboratory using a Kois dento-facial analyzer. The casts were cross-mounted and verified using a palatal index during the mounting procedure. A custom metal abutment for implant No. 11 was chosen because of the need for occlusal guidance. Due to the thin tissue biotype around the canine implant,6 the custom metal abutment was designed with a fluorescent ceramic shoulder material (Figure 8). This supports the transmission of light into the tissue and prevents discoloration of tissue from the metal abutment (Figure 9). The implant restoration was PFM with an angled ceramic margin so that light would be able to enter the restoration (Figure 10). The feldspathic veneers were fabricated using a refractory die technique (Figure 11).
The restorations were placed using a 5th-generation adhesive protocol. The PFM crown was inserted with temporary implant cement after the custom abutment was torqued into place (Figure 12). The occlusion was checked to ensure equal posterior point contacts with canine guidance during function. Long-term tooth position is being maintained using a maxillary hard acrylic nightguard.
Conclusion
By focusing on the diagnosis, respecting risk management, and establishing a clear vision of the final outcome, the treatment was easily phased over the course of more than 4 years. The functional risk was lowered from moderate to low by creating equal simultaneous posterior contacts through occlusal equilibration facilitated by a Kois deprogrammer. The low biomechanical risk was maintained through conservative veneer preparations. The patient was pleased with the final esthetic result, which met her objectives of improved arch form, tooth length, and color (Figure 13 through Figure 15). Treatment goals were met by satisfying the patient’s desire for improved esthetics while respecting risk management, thereby increasing the probability and predictability of long-term success (Figure 16 through Figure 18).
References
1. Kois JC. New challenges in treatment planning: Incorporating the fundamentals of patient risk management. Part 2. Journal of Cosmetic Dentistry. 2011;27(1):110-123.
2. Jayne D. A deprogrammer for occlusal analysis and simplified accurate case mounting. Journal of Cosmetic Dentistry. 2006;21(4):96-102.
3. Misch CE. Guidelines for maxillary incisal edge position-a pilot study: the key is the canine. J Prosthodont. 2008;17(2):130-134.
4. Kois JC, Kan JY. Predictable peri-implant gingival aesthetics: surgical and prosthodontic rationales. Pract Proced Aesthet Dent. 2001;13(9):691-698.
5. Kois JC. Altering gingival levels: the restorative connection, part I: biologic variables. Journal of Esthetic and Restorative Dentistry. 1994;6(1):3-7.
6. Kois JC. Predictable single tooth peri-implant esthetics: five diagnostic keys. Compend Contin Educ Dent. 2004;25(11):895-900.
About the authors
Peter Pizzi, CDT, MDT
Owner and Manager
Pizzi Dental Studio Inc.
New York, New York
Michael T. Ricciardi, DDS
Private Practice
New York, New York