Zirconia Composite Restoration
Create new techniques with innovative materials to benefit the patient.
Divergences across multiple implant axes present a number of complications both technically and clinically—particularly when there is no connectivity, as in one-piece and small-diameter implant systems. In this case, we explore a concept that effectively resolves a number of these issues while using a zirconia primary and secondary structure. Here, artificial dentition was used to accomplish the desired tooth positions and esthetic requirements, and a try-in was performed prior to final fabrication of the definitive prosthesis. A creative technique is shown using a clear silicone product combined with a clear flask system, allowing light curing of dental composite in multiple layers while inside the silicone matrix. Staining is also possible between the dentin and enamel layers. The concept highlighted here enabled the technician to meet the needs and desires of the clinician and the patient by creating a restoration that was implant-supported and retrievable by the clinician, while also meeting the patient’s esthetic desires.
The introduction of a variety of newer materials has opened up unlimited options not previously possible. This article highlights a creative implant solution, which was developed for a compromised patient situation.
Case Presentation
The patient presented with ill-fitting dentures that were neither esthetically nor functionally satisfactory (Figure 1). The patient had lived with this type of prostheses since her early 20’s, and it was obvious at the first appointment that her dissatisfaction had affected her self-esteem and how she viewed herself. The patient also seemed to have lost hope that anything could be done to improve her dental situation. Health factors were also a major issue in this case; in fact, the use of denture adhesives over many years left her with hyperzincemia and neuropathy.
After assessing the patient’s condition, the treating dentist chose to place small-diameter implants due to their minimally invasive nature. However, this presented a number of challenges and obstacles to the restorative aspect of this case, especially due the to treating dentist’s request that the prosthesis be retrievable by the clinician at 6-month intervals but not removable by the patient. Here the author will cover the technical steps taken in fabricating the maxillary prosthesis.
Laboratory Protocol
After taking preliminary impressions and a preliminary bite registration, the appropriate teeth were chosen, and a tooth arrangement was set in wax for try-in. The goal here was to satisfy the patient’s request for a more youthful smile and, of course, to improve the functionality of the prostheses.
In order to fulfill these requests, an in-depth model analysis was performed, and natural life-like tooth positions were chosen. Particularly with the anterior teeth, an effort was made to change the shape and contour of the patient’s lips by creating key support areas for the lip line through the position of the maxillary anterior incisors. In addition to this, the vertical dimension was opened approximately 3.5 mm. This approach, which provided the increased central tooth length typically found in youth, greatly improved the appearance of the face, restoring a youthful, vibrant look.
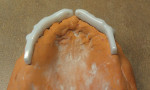
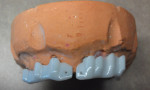
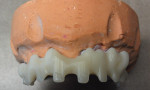
With this initial phase completed, it was time to tackle the technical challenges of creating a semi-fixed restoration over multiple divergent small-diameter implants. After considering a series of options, it was decided that a primary dual bar would be designed and milled in zirconia (Figure 2 and Figure 3). Each bar would be a unilateral structure incorporating two horizontal screws each, and would seat independently because the cross-arch divergence angles would not allow for one structure. The dual bars would also be milled to 0° to allow a secondary zirconia structure to seat intimately over the dual bars. This secondary structure would house the horizontal screw collars and would be the framework upon which composite dentition would be created.
The wax try-in was matrixed, and the zirconia dual bars were designed, milled, and checked for fit. Then the dual bars were polished, and threaded portions were placed for horizontal screw placement using light-curing composite resin cement compatible with zirconia. The dentist placed the primary zirconia dual bar intraorally and took an impression to ensure that the secondary structure would align properly. The secondary zirconia structure was first milled in resin to verify proper support and fit (Figure 4 and Figure 5). At this point, the horizontal screw collars were also luted into the resin structure intraorally to verify alignment (Figure 6). Once this was verified, the final secondary structure was milled and sintered. A portion of this secondary structure would be used as support for gingival simulation, and it was stained prior to sintering.
The original matrix was now used to build wax onto the secondary structure (Figure 7 and Figure 8). A try-in of all components revealed that one of the horizontal screw collars was not properly aligned. The collar in question was removed, and a new collar was placed intraorally into the zirconia secondary structure using light-curing composite resin cement.
The secondary zirconia structure with completed wax-up was now imbedded in putty silicone and placed into the base of the clear flask (anaxdent, www.anaxdent.com). Sprue channels were waxed to the posterior-most points of the wax-up, and the flask was closed and filled with a vacuum-mixed clear silicone and cured under pressure to eliminate any porosity. After curing, the flask was opened and the zirconia structure was cleansed of any residual wax. It was then air-abraded with aluminum oxide at 2-bar pressure. The structure was then steam-cleaned, thoroughly dried, and primed with a coating of Zirkon Bond primer (anaxdent) and light-cured. The structure was placed back in the clear flask, and the flask was closed. Shade A1 Dentin was injected into the mold to ensure that a 45° angle was consistently applied to the flow of composite into the flask, eliminating the risk of any internal air freely flowing out of the secondary sprue channel and trapping any porosity in the composite. The entire flask was put into the Dentacolor XS (Hereaus Kulzer, www.heraeus.com) stroboscopic light-curing unit and cured for two cycles of 90 seconds with a cooling interval between cycles of 3 minutes to 4 minutes (Figure 9 and Figure 10).
After removing and carefully steaming the dentin material, cut-back was performed, and Bond LC (anaxdent) composite primer was applied and light-cured, after which some internal staining was carried out The entire structure was placed back into the clear flask (Figure 11), and Enamel S57 was injected in the same fashion as the dentin. The structure was light-cured to complete the dentate portion of the prosthesis.
At this point in case construction, the gingival simulation could be carried out by hand using gingival shaded flowable composites. Analog pins were placed to provide additional space in the screw accesses to allow for the vinyl polysiloxane (VPS) screw when covered with composite after the prosthesis is finally placed and the horizontal screws engaged.
Due to the bi-lateral divergence of implants and the accuracy achieved in the dual-bar zirconia structures as well as that of the secondary structure, which bound everything together, the prosthesis was extremely stable, yet retrievable.
For final seating, the dual bars were inserted and the secondary structure was screwed into place. A small amount of VPS material was placed over the horizontal screws, and composite was placed over all four screw access holes. All the dentist needs for retrieveability is to remove the composite caps and VPS, unscrew the four horizontal screws, and remove all of the components. When in place, the prosthesis has proved to be very stable, and function has been dramatically improved. In addition, all portions of this prosthesis that oppose tissue are highly polished zirconia surfaces. Although this was an extremely difficult situation, the combination of new techniques and materials are being used in ways not previously imagined, all to the benefit of the patient (Figure 12).
About the Author
Arian Deutsch, CDT
Owner
Deutsch Dental Arts
Surprise, Arizona