Creating Youthful and Valuable Restorations for a High-Profile Patient
Executing excellence through dental team collaboration.
By Pinhas Adar, CDT, MDT; and Michael R. Sesemann, DDS
If knowledge were the only requisite for success, virtually everyone would be successful, especially with the wealth of information currently available through avenues like the Internet and the news media. An action plan also is essential. Given the onslaught of product introductions from dental manufacturers vying for business, dental professionals face the ongoing challenge of keeping up with the barrage in order to make informed selections of the best products that not only meet their clinical and esthetic requirements but also their patients’ demands.
A Plan of Action
Essentially, dentists and dental ceramists are business owners, and in business, time is money. Yet, rather than selling a product such as a crown, for instance, dental professionals are providing a service that requires considerable skill and time. Instead of asking their patients to purchase a product or procedure, dental professionals are asking for an investment in their expertise and time to exercise these skills and knowledge. Therefore, dental professionals must determine the types of products and systems to employ in their daily procedures in order to maximize their most valuable commodities—time and service.
Technology is a great time saver and represents a rich profit source. However, before investing in any technology, it is important to consider five factors for success.
1. Favorable market trend.
2. Product uniqueness. For dental professionals, this translates into their skill levels and how these can be used to marketplace advantage.
3. Partnerships with companies with proven longevity, reliability, and quality. If dental professionals purchase costly equipment and/or technology, they want assurance the company and technology will be around if future services and/or upgrades are required.
4. Favorable return on investment (ROI) compensation. If laboratories or dentists invest $100,000, what can they expect as an ROI for their businesses?
5. Perfect timing.
Dental ceramists and their dentists should embrace technology, but they must not be ruled by it. Patients should feel as if technology is an enhancement, not a replacement, for a dental professional’s personal service. The “personal touch” remains an important element of patient satisfaction and retention. In fact, the patient whose case is highlighted here—a woman renowned throughout the dental industry—has commented that it is the value of how she felt during interactions with the ceramist and dentist that provided the value and affirmation for her decision to proceed with treatment, saying that “It was how I felt that allowed me to make the decision in choosing this ceramist and dentist because I felt they would take care of me, and I felt safe. I trusted them to a great degree not just because of their training and leadership, but also because of their humility, which allowed them to connect with me like a normal person. Their relationship with me was transformational, not transactional.”
Therefore, as ceramic artists, we must use technology to our benefit, employing it to more effectively and productively enhance our own skill levels and the services we provide to our patients. The bottom line comes down to attitude: opening our minds—and businesses—to different technological opportunities to favorably position ourselves in the marketplace.
Digital photography is an excellent example of dentistry’s effective use of technology. Not only is this time-saving technology helpful in capturing patients’ preoperative status, step-by-step treatment procedures, and postoperative results, it also serves as an effective educational tool for all treatment team members with their patients, and as a communication tool between ceramists and dentists. To maximize communication between all dental team members, web and video cameras are other effective tools in the modern dental team’s arsenal.
When it comes to product selection for a patient’s treatment plan, several factors must be considered from tooth structure, color, spacing issues, and teeth mobility to the patient’s needs and desires. Depending on the case specifications, certain dental products and/or procedures will be more indicated than others.
The case presentation discussed in this article illustrates the versatility, ease of use, and optimal clinical and esthetic results possible with the proper application of a team-based approach to the use of IPS e.max® pressible technology (Ivoclar Vivadent, www.ivoclarvivadent.com).
Case Presentation
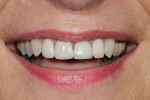
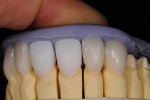
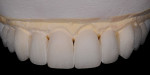
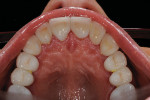
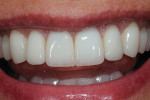
A female patient presented seeking improved esthetics and full-mouth reconstruction for her smile for personal and professional reasons. A dynamic and vibrant personality with a high-profile career in the dental industry, she wanted a smile that was equally impactful. Clinically, she presented with an extensive amount of dentistry that had been done on an as-needed basis. She was conscious of the different optics resulting from the various materials used, and their contrasting appearance with one another as well as with adjacent natural teeth. Bilateral disharmonies and different clinical crown heights were evident (Figure 1).
After a comprehensive evaluation and discussion involving all dental team participants—dentist, patient, and laboratory technician—a diagnostic wax-up was created to show the patient the proposed final result and secure her approval.1,2
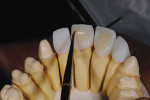
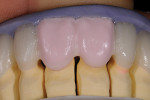
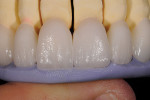
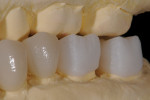
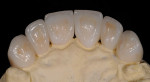
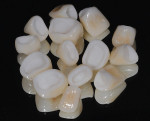
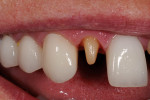
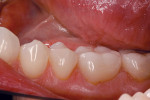
After the dentist took the impression, index, and fabricated the temporary restorations from the wax-up, he photographed the temporaries and sent them electronically to the ceramist—the model of the provisional restorations was also provided. He also transmitted information on the patient’s tooth structure, the preparation guide, and color specifications (Ivoclar stump shade, shade guide, desired shade, and existing shade of patient’s natural teeth) (Figure 2 and Figure 3). With these aids as reference points to the desired outcome,8, 9 the ceramist opted to use a medium-opacity ingot from the IPS e.max (MO-0) family (Figure 4). The sufficient brightness of the ingot would support the value of the color as well as provide options for layering the ceramic according to patient preference.
Laboratory Protocol
The ceramist poured the model from the dentist-provided impressions. A full-contour wax-up was created. Cutback was minimal to determine how much layering would be necessary. The restorations were pressed and fitted to the models. Using teeth Nos. 8 and 9 as trial custom shade guides, the ceramist painted glazed liquid on the surface of the pressed crowns and sprinkled orange IPS e.max powder to create the first bake wash layer (Figure 5). IPS Empress multipurpose shade was applied buccally and lingually to slightly tone down the crowns before proceeding with the bake (Figure 6). The two crowns were fired; No. 8 was more like the 1M1 Vita® shade, and No. 9 was slightly darker.
At this stage, there was a three-dimensional visual of the actual restorations, enabling all parties to preview the final outcome and make any necessary or desired adjustments before the case was completed. The patient presented for a trial restoration try-in. Typically, this is the time in a patient’s treatment plan to elicit his/her reaction to the restoration by asking a series of questions, most notably whether he/she sees a difference between the restorations and natural teeth. It is recommended that someone close to the patient, such as a spouse or parent, also be at the appointment to help in the final shade selection. Quite often, most patients do not see a difference, and the restorative process can proceed as planned. If a difference is perceived, the patient can clearly verbalize what he/she sees and finalize a preference.
Keep in mind that esthetics, including color choice, is subjective. Therefore, for best patient satisfaction, the patient must participate in the decision-making process. Ultimately, the patient should decide based on his/her preference for comfort, function, phonetics, and esthetics. In this specific case, once the patient expressed her preference, the restorations were further modified.
A unique aspect of these particular restorations was how the brightness of the MO-0 was used in the cutback stage. The cervical area around the tooth was reduced minimally in order to overlay the ceramic slightly less on the bulky area, thus allowing the ingot’s brightness to come through. Cutting and fettering the incisal edge created natural incisal effects. While minimal, this preparation was key because it used the ingot as a support for the value, which should not be dropped. It would not make sense to cut back completely, create a thin coating, and then attempt to rebuild the needed brightness when the ingot serves that purpose.
Next, the cervical dentin, which has some translucency, was used to further enhance a natural effect. Then the dentin shade was overlaid in full contour, using the index to determine the final length for the build-up. After the dentin cutback, a space was created for the incisal edge using high-value enamel (TI1), bleach, and Opal Clear (OE1). To minimize grayness, the OE1, which exhibits a bluish opal translucency, was mixed with the neutral translucent to dilute it slightly. The mixture was applied in a segmented lateral build-up, similar to a piano key. To create the incisal wall canvas, mamelon effects (mamelon light and salmon mixed half-and-half) were applied. As an overlay to that build-up, a thin layer of the OE1/neutral translucent mixture was used. The crowns were baked and re-fitted on the model. Then, the silicone index was tried-in to verify that the length matched that of the patient-approved temporary (Figure 7, Figure 8, Figure 9).
The cutback reduction for the upper posterior teeth required a minimal layering technique. Fabricated thickest for strength, the pressed material core for the posterior teeth was still able to achieve the same enhanced esthetics (ie, ceramic finish) as the anterior teeth due to this layering concept (Figure 10). After all of the units were shaped and texturized on the model, the contact points were checked, the soft tissue was removed to eliminate interference, interproximal spacing was closed, and contacts were tightened to help ensure minimal chairside time (Figure 11).
A different fabrication method was used for the lower posterior teeth. In order to blend with the natural color of adjacent teeth, it was determined that the HD translucent ingot (A1) would be used with the staining technique and IPS e.max stains to obtain the shade characteristic exhibited by the patient’s natural teeth (Figure 12).
The patient presented for a restoration try-in. Mach-2® die silicone (Parkell, Inc., www.parkell.com) was used to stabilize the crowns and check the contact points and bite for final patient approval for shape, color, and alignment (Figure 13, Figure 14, Figure 15, Figure 16). Once all of the dental team members were satisfied, the dentist placed the permanent restorations (Figure 17).
Discussion
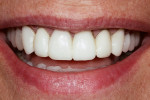
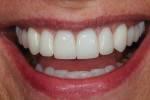
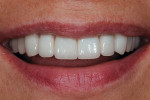
This case illustrates the suitability of the IPS e.max layered version of crown restorations for customizing the shape and shade for this particular patient. Despite its monolithic character, the staining technique nevertheless enabled the use of one pressed color to obtain a natural look that blended in well with natural adjacent teeth (Figure 18). Proper ingot selection and precise knowledge of what tooth structure was being worked on to ensure exact color blending with the tooth’s substructure was instrumental in the successful outcome. The patient, whose career often requires on-stage appearances, was highly pleased with the outcome—a healthy, natural- and youthful-looking, bright smile that “popped” and exuded powerful confidence (Figure 19 and Figure 20).
Conclusion
The key to a successful outcome is to have a clear, unified vision of the desired objective, then formulate a solid strategy to achieve it, including maintaining a practical system, proper methodology, consistent and superior service, and effective dental team communication. For the team—including the patient—how that objective is achieved is not measured primarily in cost, but in value.
Patient experience is critical. People appreciate the personal contact, attention, and care while valuing the human connection. Patients are making an emotional and financial investment, not so much in a treatment or restoration, as they are in the dentist and dental ceramist providing that treatment or restoration. Therefore, dental professionals need to “sell” their expertise in selecting and using the proper technology to best execute patients’ clinical and esthetic needs and expectations in the most time-effective, profitable, and convenient ways for all parties involved.
While financial gain is not the main goal, money represents the well-earned reward for accomplishing good and providing excellence. In order to reap the former and fulfill the latter, dental professionals must aim to execute excellence every time they approach any endeavor to provide high-value patient experiences and foster collaborative dental team communication.
References
1. Kahng LS. Patient-dentist-technician communication within the dental team: Using a colored treatment plan wax-up. J Esthet Restor Dent. 2006;18(4):185-195.
2. Adar P. Avoiding patient disappointment with trial veneer utilization. J Esthet Dent. 1997;9(6):277-284.
3. Nanchoff-Glatt M. Clinician-patient communication to enhance health outcomes. J Dent Hyg. 2009;83(4):179.
4. Terry DA. Aesthetic and Restorative Dentistry: Material Selection and Technique. Hanover Park, IL: Quintessence Pub Co; 2009:152-153.
About the Authors
Pinhas Adar, CDT, MDT
Owner
Oral Design Center
Atlanta, Georgia
Michael R. Sesemann, DDS
Founder
Nebraska Institute of Comprehensive Dentistry
Omaha, Nebraska