Heroic Restorative Procedures
Existing crowns can be saved with bioactive materials
Robert A. Lowe, DDS
Heroic dental procedures are a part of every dental practice. These treatments take into account the patient’s oral health, lifestyle, finances, and other unique circumstances. Many older patients have difficulty maintaining their teeth in a state of health as their natural ability to repel acid challenges in the oral environment declines. Changes in the quality and quantity of saliva, often due to medical conditions and medications, make root surfaces more susceptible to caries. Many in this demographic are on fixed incomes, and their limited finances preclude “ideal” restorative replacements with dental implants and new fixed prostheses. In many of these cases, bioactive restorative materials give the dentist a useful tool to help extend the life of existing dental restorations that may be subject to recurrent decay and acid attack. The following clinical cases describe heroic dental procedures where failing restorations were fixed rather than replaced using a bioactive restorative material (ACTIVA™ BioACTIVE-RESTORATIVE™, Pulpdent Corporation, www.pulpdent.com ). As a result, the patients received a timely, affordable treatment that saved their existing tooth structure.
Bioactive materials like ACTIVA work favorably in the moist oral environment and help to provide the building blocks of calcium and phosphate ions, to rebuild and fortify affected dentin that has been demineralized by acid attack. They are the first restorative materials that mimic the physical and chemical properties of natural teeth being composed of a bioactive ionic resin matrix, a “shock-absorbing” rubberized resin component, and reactive glass-ionomer fillers.
In the presence of saliva, ACTIVA stimulates apatite formation and the natural remineralization of affected dentin, creating an intimate connection between the restorative material and tooth substance. The result is a seal of the marginal interface that helps prevent microleakage and recurrent decay. In today’s world, this is the new definition of bioactivity in restorative materials. Also, ACTIVA acts like a rechargeable battery of sorts reacting to continuous pH changes in the oral environment to help fortify and recharge the ionic properties of saliva, tooth substance, and the restorative material itself. For this reason ACTIVA is considered a “smart” restorative material.
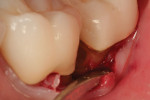
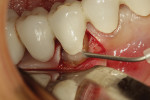
Existing crowns that are in serviceable condition but have root caries beyond the margins can have their clinical “lives” extended if the caries can be removed and replaced with a bioactive material that helps protect and rebuild the ailing tooth structure. Such was the case of a patient in her early 70s (Figure 1) wishing to avoid implant surgery. The use of diode lasers and reflection of “mini flaps” may be necessary, in some cases, to gain access to remove the decay and restore the marginal area.
The key to removing infected dentin is the use of Smartburs® (SS White®; www.sswhitedental.com). Because the specific Knoop hardness of the Smartbur matches that of healthy dentin, it removes only infected dentin. As a result, the entire carious area need not be visualized or inspected to ensure removal of the decay. The dentist simply instruments the area until no more cutting occurs, and then the cavity is ready for placement of the bioactive restorative material.
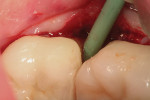
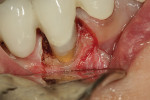
Figure 1 shows the initial instrumentation of a mesial root caries lesion apical to the existing crown margin on tooth No. 18. A polymer round bur (Smartbur II) on an electric handpiece maintained at a constant speed of 6,000 rpm was used to remove infected dentin from the lesion (Figure 2). Once the bur stopped cutting, the lesion was prepared and made ready for the restorative material.
A major challenge with traditional glass-ionomer restorative materials is that the lumen sizes on the tips of the capsules make it impossible to limit the amount of restorative material that is delivered. The result is a mass of excess cement that is difficult to remove and finish in the limited operative space between the teeth. With ACTIVA, however, the mixing tip and bendable metal cannula make it easy to deliver the appropriate amount of restorative material, which reduces the amount of finishing required. Only a few passes of a 30-fluted carbide composite finishing bur should be needed.
Another issue associated with traditional glass-ionomer and composite materials is microleakage and secondary caries. ACTIVA prevents both by stimulating apatite formation and the remineralization of enamel and affected dentin, creating an intimate connection with the restorative material and the tooth.
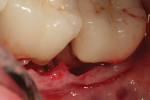
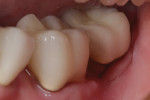
Figure 3 shows the ACTIVA Restorative in place prior to suturing of the flap. Figure 4 shows the “heroic” restorative effort on this second molar 3 years after placement. The margins are intact, and there is no evidence of recurrent decay surrounding the crown or ACTIVA restoration. Application of Embrace™ fluoride varnish (Pulpdent) at regular recare visits can also help extend the serviceable life of the restoration.
Figure 5 shows a different case where ACTIVA was placed in a submarginal preparation on the facial surface of tooth No. 28. As an older person living on a fixed income, the patient was looking for a way to save an existing five-unit bridge. Because of the extent of the carious lesion, a full-thickness mucoperiosteal flap was elevated to gain access for the restorative procedure. Note that the unique delivery system provides the practitioner with convenient dispensing and complete control of placement, enabling precise application of ACTIVA in difficult-to-reach areas and, in this case, limiting delivery of the material to the extent and desired confines of the preparation. Once finished (Figure 6) with a 30-fluted composite carbide-finishing bur (ET 3 UF: Komet USA, www.komet.com), the flap will be sutured to place and allowed to heal.
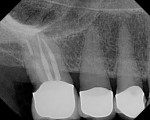
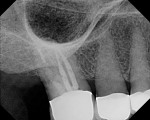
In a third case, another elderly patient presented with root caries in the distal crown margin of tooth No. 3 (Figure 7). Figure 8 shows the defect restored with ACTIVA. Due to limited access, clinical photography was not possible. Without ACTIVA as an option, and the ability to easily place the material in this distal area, it is likely this tooth would not be restorable and would be lost. ACTIVA’s bioactive properties provided a seal at the margin and protected the restoration from microleakage and secondary caries. As a result, the life of the tooth was extended, and the patient was extremely happy.
For more information, contact:
Pulpdent Corporation
800-343-4342
www.pulpdent.com
About the Author
Robert A. Lowe, DDS
Diplomate, American Board of Aesthetic Dentistry
Private Practice
Charlotte, North Carolina