Creating Proper Space in the Esthetic Zone
A systematic approach to predictable space management throughout treatment.
In the consultation appointment for esthetic treatment, the assessment is divided into a conventional evaluation through radiographs, photographs, diagnostic models, and a smile analysis focusing on the patient’s esthetic requests. The clinician’s ultimate goal is to give the patient a brilliant smile by creating an esthetic arrangement with proper proportion in relation to the face. For this reason, the clinician must follow a systematic approach to predictably manage patients seeking esthetic treatment.
Space in the anterior dentition is bothersome to the patient and unsettling to the restorative dentist. Therefore, closing space may have a dramatic effect on the esthetic appearance of the anterior teeth. Although it is usually easy to close diastemas, long-term success is dependent upon the accuracy of the diagnosis. For example, if the spacing is habitual, it may relapse after the definitive prostheses are delivered. Once the correct diagnosis is determined, the clinician can focus on treating the space. This article will explore the leading causes of diastemas and present a systematic approach to predictable space management throughout treatment.
Space Analysis
Many factors can contribute to spacing in the maxillary anterior dentition. Some of these include: (1) improper axial inclination of the roots of the maxillary anterior teeth; (2) tooth size discrepancies (narrow maxillary lateral incisors); (3) pernicious habits such as thumb- or finger-sucking, lip-biting, or tongue-thrusting; (4) deleterious occlusal patterns which tend to place lateral forces on the maxillary anterior teeth; (5) the anatomy of the teeth (central incisors with larger mesiodistal dimensions at the cervical portions of the teeth than at the incisal edges); (6) increased interarch width compared to the mesiodistal width of the teeth; and (7) muscular imbalances in the oral region.1
When addressing diastemas in the maxillary anterior region, the clinician must first pinpoint the location(s) of the spacing. This is the most important step and includes whether or not the spacing is localized or generalized and if the maxillary and/or mandibular arches are involved. Next, the clinician must determine the amount of space with relation to the tooth length to decide whether or not the space can be masked by prosthetic treatment only. The third and final step is to discover the etiology behind the anterior spacing and determine if there is an occlusal component.
Establishing Symmetry: Proportions, Display, and Length
To create symmetry in the esthetic zone, it is important to establish the correct proportions, display, and length. Known as the “PDL” of symmetry, these three entities need to be implemented at the central position. Establishing the length should be the first of the three entities to be determined. The overall average measurement from the gingiva should be at least 10.5 mm. It can be checked by analyzing tooth exposure at rest and through phonetic testing. Once the length is determined, the proportions and overall dominance of the centrals can be made. All three entities are captured in the esthetic wax-up and implemented in the definitive restorations. To avoid fabricating central incisors that have short/fat and long/narrow proportions,3 the mesiodistal width of the central incisor should be 75% to 85% of its length.2 The display of the central incisors, which should be dominant, is created by placing the central incisor in a forward position in relation to the lateral incisors and by increasing the overall dimensions compared with the adjacent teeth. The lateral incisors should never compete for attention.4 As gender teeth, they need to be delicate in women and coarse in men.
Treatment Progression
Diagnostic Evaluation
At the diagnostic evaluation, the clinician interviews the patient to discuss his or her chief concerns. After the conventional evaluation with charting and periodontal, occlusal, and radiographic assessment along with diagnostic models and photographs, the clinician can study the case without the patient in the office. This allows the clinician to gauge future treatment before the patient attends the esthetic consultation.
Smile Analysis
The smile analysis is most beneficial after all diagnostic information is gathered. During this time, the clinician can pinpoint the esthetic problems that the patient faces and further educate the patient about these dilemmas before treatment is rendered. The patient is also allowed to state three esthetic problems that he or she would like solve. Furthermore, composite can be added to show the patient the direction of the clinician’s vision.
Esthetic Wax-Up
An esthetic wax-up captures the contour, proportions, and color found in the natural dentition. It is a composite sketch of the clinician’s vision of the appearance of the future restorations on the smile analysis. The esthetic wax-up, which uses denture teeth or tooth-colored wax, offers everything that the traditional diagnostic wax-up offers, but adds an additional dimension by incorporating natural tooth color. It allows the patient to see the difference between varying degrees of brightness, value, and color before placing the wax-up. Once the wax-up is completed, an addition silicone impression is taken to transfer the proposed plan to the mouth. This allows the clinician to arrange various esthetic elements into proper proportions and relate them to the face. It provides an avenue for the technician and dentist to communicate with digital imaging to confirm that the wax-up satisfies the recommendations stated on the checklist.
Preview
A preview, a vision of the proposed plan reproduced by the wax-up and transferred to the mouth, allows the patient to preview the future restorations before the teeth are prepared. This is usually performed with bis-acryl or a composite-type material. The preview is not complete until the patient and dentist agree upon the final plan. It is important that the length, proportion, and fullness are precisely estimated before proceeding to the preparation phase. After the preview is completed, an alginate impression is taken so that occlusal and facial reduction indexes and addition silicone matrix can be fabricated. Because the provisional restorations will be made from the preview instead of the wax-up, fewer alterations will be needed when delivering the provisional restorations. The preview, rather than the wax-up, will be used to facilitate acceptance of the smile design plan.5
Preparation Design
The preparation design will be based upon the preview models. Occlusal and labial indexes can be fabricated along with an addition silicone stint to ensure that there is adequate reduction during the preparation procedure. The stint allows the clinician to place the preview back into the mouth with bis-acryl, creating the proposed dimensions of the final restorations. During the preparation phase, the reduction can be assessed with the previously fabricated indexes. Many clinicians tend to use the wax-up as their guide, but if not verified in the mouth prior to preparing the teeth, the reference position may be lost. This may cause inaccurate reduction, which in turn affects the final preparation design.
Final Impression
Once the preparations are completed, multiple impressions are taken using polyvinylsiloxane impression material. Soft tissue retraction is performed only when the margins are located subgingivally. This prevents vertical forces from penetrating into the attachment apparatus and causing localized gingival recession. Note that only one impression should be used for the fabrication of the definitive restorations; other can be kept in the office in case the other impression is damaged or lost.
Provisional Fabrication
The provisional restoration or “prototype” is the replicate of the desired plan. After the veneer preparations are completed, each tooth to receive a provisional restoration is spot-etched and spot-bonded. The provisional material is placed into the stint fabricated from the impression taken from the mock-up and then placed into the mouth. After the provisional material is set, the excess is removed, contoured, and polished. One of the central-incisor prototypes is removed and an additional trial-unit impression is taken to fabricate the trial-unit model. The remaining central incisor prototype is spot-bonded into position and the patient is dismissed.
Ceramic Selection
The wide range of ceramic systems may overwhelm clinicians. Feldspathic-like glass or highly filled leucite-containing glass–ceramic are the two systems most commonly used when placing veneers in the anterior dentition. However, it is important to select a porcelain system that has a high flexural strength, is esthetically pleasing, and is less abrasive to the natural dentition.6 The durability of the ceramics are enhanced by adding primary crystals to the glassy matrix. Three primary crystals, leucite, lithium disilicate, or fluorapatite, can be added. Ivoclar Vivadent (www.ivoclarvivadent.com) has developed an improved pressable ceramic system (IPS e.max®) by adding lithium oxide to aluminosilicate glass to form lithium-disilicate crystals. Lithium-disilicate glass ceramic was first introduced by Ivoclar as Empress® II. IPS e.max evolved from Empress II by increasing the crystalline volume (70%) and improving the crystalline size.7 Therefore, the flexural strength of e.max was increased to 360 MPa, which is three times that found in Empress II. e.max can be very translucent due to the relatively low refractive index of the lithium-disilicate crystals.8,9
Trial Unit
A trial unit is a porcelain replica of the desired shade, shape, and contour of the future restorations. This unit, usually a maxillary or mandibular central incisor, is selected because of its anterior position in the mouth. It is fabricated from a trial-unit model, which contains one prepared tooth among the adjacent provisional restorations. At the try-in appointment, the provisional restoration is removed and the trial unit is placed for patient approval. The clinician can adjust the length, midline, and overall contour of the restoration. As soon as the patient accepts the trial unit, he or she signs a trial-unit approval form. At this time, the other provisional restorations can be assessed, giving the patient the ability to choose one tooth located on either side of the arch that is more esthetically pleasing. Digital images are taken with the trial-unit in place, allowing the technician to copy the provisionals selected in the definitive restorations.
Model Preparation and Laboratory Prescription
The dentist should first mount the maxillary model of the provisionals on a semi-adjustable articulator using a facebow to ensure that the orientation of the provisional restorations is parallel to the horizon. The mandibular model is mounted to the provisional model with a centric bite registration interposed. Once the mounting is verified for accuracy, occlusal and labial indexes of the prototypes are made with addition silicone. The silicone indexes, mounted models, articulator, bite registration (prepared teeth), and final impression are sent to the master technician.
A detailed laboratory prescription specifies all desired entities of esthetics, occlusion, and ceramic material used to fabricate the final veneer restorations. In the prescription, the patient is introduced first, followed by the material to be used in the case. The clinician chooses one tooth from each specific group to copy, for example, right central incisor, left lateral incisor. Then, specific alterations can be recorded using the final provisional template. Finally, the shade is depicted using a schematic drawing of the anterior dentition. This includes outlining the halo, surface anatomy, coronal extent of cervical shade and its relation with the incisal area, and shade progression from cervical to incisal third. This detailed prescription provides the technician with enough information to fabricate the case.
Fabrication
The technician will prepare a solid model and a die model of the preparations. The provisional model will serve as the main source of information to guide the technician during the fabrication of the definitive restorations. Throughout the manufacturing process, the technician can communicate with the clinician via digital photography and e-mail. The die model will be used to fabricate each individual restoration, paying close attention to the marginal adaptation. After the units are completed, each restoration will be placed onto the solid model to check interproximal fit.
Adhesive Cementation
As soon as the case is delivered to the clinician, all units are verified for accuracy. The laboratory prescription is reviewed to make sure that the technician followed all of the details stated in the prescription. Then the interproximal and marginal fit of each unit is checked on a solid model. Once the clinician has reviewed everything, the final restorations are ready for delivery.
During the delivery appointment, the provisional restorations are removed and the preparations are cleaned using flour pumice. Each unit is tried in the mouth using glycerin or clear try-in gel. Because these are veneer restorations, the fitting sequence of each restoration needs to be assessed. Next, the interproximal contact and marginal fit are verified. The occlusion is adjusted and the porcelain is polished on the die-model before final delivery. The adhesive cementation process will be discussed in the case presentation. To guard against any unwanted occlusal forces, an acrylic night appliance is delivered to the patient.
Case Presentation
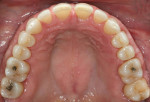
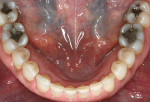
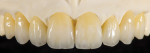
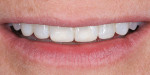
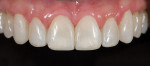
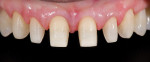
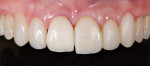
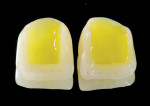
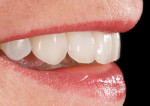
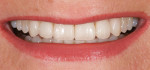
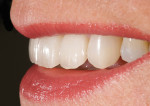
A 52-year-old woman first presented with the chief concern of diastemas between the four maxillary incisors (Figure 1, Figure 2, Figure 3 and Figure 4). The temporomandibular joint (TMJ) and functional analysis revealed that there was crepitus upon opening and closing in the right joint with minor wear on the maxillary and mandibular dentition. This wear pattern is unrelated to patients who are known bruxers (Figure 5 and Figure 6). The patient wore a splint for 2.5 months, during which time no posterior trigger caused the mandible to position itself anteriorly. Initial and subsequent interviews of the patient and her spouse revealed no known pernicious habits as causative factors for the anterior spacing. The study models mounted in centric relation (CR) revealed that CR equaled maximum intercuspation (MI) position with both condyles fully seated. There were no maxillary constrictions or discrepancies with the envelope of function. The patient had Class I skeletal and dental relationships assessed at the first molar position. With that said, all occlusal parameters were within normal limits and consistent with the patient’s age.
Smile analysis revealed that the spacing was caused by increased maxillary interarch width in relation to the mesiodistal width of the incisor teeth. Further analysis revealed that the central incisors measured 9.5 mm. A thorough periodontal examination showed healthy tissue, with slight bone loss on the buccal surfaces of the maxillary premolars that corresponded with abfraction lesions. Gingival probing revealed no indication of inflammation or generalized bleeding. The only signs of possible destructive forces were the buttress bone located adjacent to the maxillary and mandibular premolar teeth and the slightly recessed areas adjacent to the maxillary premolar teeth. There were no clinical or radiographic signs of decay.
Wax-Up
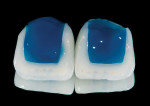
An esthetic wax-up was done from first bicuspid to first bicuspid (Figure 7). The length of the central incisors was increased to 11 mm. Consequently, when the width was added to the central incisors, the width was about 80% of the length that satisfied the width-to-length ratio. The interproximal contact was first established in a more labial position. As the proportions were modified, the interproximal contact migrated more lingually. After the wax-up was finished, it was duplicated using alginate and an addition silicone stint (3M Express Light Body Fast Set, 3M ESPE, www.3mespe.com) was fabricated to transfer the wax-up to the mouth.
Preview
The wax-up was transferred to the mouth by injecting Integrity® (DENTSPLY, www.dentsply.com) into an addition silicone impression (Figure 8 and Figure 9). The length, width, and overall position of the central incisors were evaluated using rest position and phonetics. It is imperative that the central incisors remain symmetrical to one another because they are at the center of the esthetic zone. The lateral incisors and canines may vary slightly due to the off-center position. Next, the tooth-to-tooth proportions were assessed to ensure that there was a harmonious transition among all the anterior teeth. Finally, all teeth were checked against the face and agreed upon by the patient. Two alginate impressions of the resin additions were made to fabricate the reduction guides and silicone matrix for the future provisional restorations.
Preparation
Because wax was not added to the labial surface, the preparation design required more aggressive reduction on the mid-facial and incisal thirds. The overall preparation design called for facial reduction of 0.3 mm at the cervical third, 0.5 mm mid-facially, and 0.7 mm incisally, along with 2 mm of incisal reduction from the preview. Once the reduction grooves were completed, the excess material was removed and the reduction grooves were eliminated. The preparation was carried interproximally and extended as far lingually as possible. All margins were located equal to the gingival margin except in areas with interproximal spacing. The margins in these areas were positioned 0.5 mm subgingivally so that the porcelain would have a natural emergence. All line angles were rounded and the margins were chamfered so the contact lens effect could be used at the veneer margins. The final preparation was moderately reduced to ensure that there was a periphery of enamel (Figure 10).
Provisionalization
After the preparation was completed and thoroughly cleaned with 0.12% chlorhexidine gluconate, the preparation was spot-etched, rinsed, and bonded into position using Adper™ Single Bond Plus (3M ESPE). Provisional material was injected into an additional silicone impression supported by a metal tray (COE) and seated into position using occlusal and labial force. Interproximal and gingival excess provisional material was removed using an ET3 diamond bur (Brasseler USA, www.brasselerusa.com) followed by a 7901-fluted bur (Brasseler). Lingual excess was removed using a pear-shaped fluted bur (Brasseler).
Evaluation of the Trial Unit
After the provisional units were placed, all but one central incisor was temporarily bonded. A polyvinylsiloxane impression (Express Light Body Fast Set) was taken of the temporaries and the single unit. The single unit was provisionalized and an alginate impression was taken to record the proposed plan. This allowed for a sample veneer or trial unit to be fabricated so the patient could view it before fabrication of the final veneers. The HT BL3 Shade IPS e.max Press ingot was selected to create a more natural-looking restoration. The trial unit was waxed and pressed to full contour followed by the cutback of the incisal third. Internal characterizations were incorporated using layering material (IPS e.max).
The patient returned for the trial-unit appointment and the provisional veneer was removed. The trial veneer was placed using a clear try-in gel (Prevue, Cosmedent, www.cosmedent.com) (Figure 11). The patient and dentist evaluated the midline, length, proportion, color, translucency, and surface texture. After the patient accepted the trial unit, a series of digital images were taken with the trial veneer in place, indicating that the definitive veneers will be fabricated using the trial as a guide. The provisional veneer was spot-bonded once again. The trial unit only facilitates the fabrication of the final veneers, and is not used as one of the final restorations.
Ceramic Selection and Laboratory Fabrication
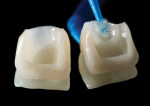
A pressable ceramic (IPS e.max) with high-leucite content was chosen for its increased durability and high translucent properties. Once the laboratory received the case and the model work was completed, the ceramist waxed each laminate to its desired contour using the provisional restorations as a guide. They were sprued, invested, and pressed using the LTA1 ingot (low translucency). After devesting, the sprues were removed and the incisal third of each restoration was cut back. Incisal effects and halo were added along with subtle hypocalcification spots to increase the natural look of each veneer restoration. The veneers were glazed 20º lower than the temperature recommended by the manufacturer and lightly polished to preserve the surface texture.
Laboratory Prescription
The laboratory prescription introduced the patient to the master ceramist followed by the patient’s chief concerns. These concerns were limited to three dilemmas affecting her smile. If the esthetic team can manage those three criteria, the patient is usually very pleased with the final result. Next, the type of restorations and the material selected were specified. Because there were two teeth to be restored in the anterior segment, the clinician identified one provisional restoration from each pair for the technician to copy. The last portion of the prescription described the overall shade, translucency, the amount of halo, and specific characterizations custom to the patient.
Delivery
As soon as the case returns from the laboratory, the clinician places the restorations first on the die model, then on the solid model to check the fit. If the seating of the veneers is identical on both models and each veneer unit corresponds with the directions stated in the laboratory prescription, the restorations are ready to be tried in the mouth. If the clinician encounters an error with the fit or there is a problem with occlusion, the clinician accepts the responsibility and the faulty units need to be altered. However, when the system is followed properly, errors can be kept to a minimum.
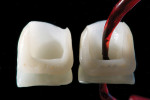
At the time of insertion, the patient was anesthetized, the provisionals were removed, and the prepared teeth were thoroughly cleaned using flour pumice. It is important to avoid using prophy paste or an abrasive containing oil to ensure that bonding is not impeded. Each unit was tried in using clear try-in gel (Prevue). After the patient approved the try-in, the corresponding cement (Insure Clear Light Viscosity, DENTSPLY) was selected and the rubber dam (OptraDam® Plus, Ivoclar) was placed. Note that each unit was etched using 5% hydrofluoric acid for 20 seconds (Figure 12), rinsed under a water stream using a fine bristle brush, etched using 37% phosphoric acid to dilute the hydrofluoric acid for 60 seconds (Figure 13), rinsed a second time, and placed in acetone in an ultrasonic bath for 5 minutes. It is important to avoid placing the hydrofluoric acid on the labial surface of the veneers to avoid etching the surface, which will cause it to appear grainy and white. Each unit was air-dried and silanated (Figure 14) followed by the application of Adper Single Bond Plus to the intaglio surface of each veneer (Figure 15).
To reduce the chance of contaminating the preparations and allow for an easier cementation process, the preparations were groomed prior to receipt of the veneers. The preparations were cleaned using chlorhexidine gluconate 0.12% oral rinse on a cotton pellet, etched for 15 seconds using 37% phosphoric acid, rinsed, and air-dried. A fifth-generation bonding agent (Single Bond Plus) was applied. Starting with both central incisors, the cement was placed in the veneer and the veneer was placed in the mouth. To avoid spacing between the central incisors during the cementation process, the clinician tacked on at the cervical third while holding the central incisor veneers together. Floss was segmented to remove excess interproximal cement. Finally, the restorations were light-cured for 60 seconds on the facial, lingual, and incisal aspect of the tooth. The excess cement was removed using a #12B (Miltex, www.miltex.com) scalpel and the restorations were polished.
The occlusion was checked to make sure that there were no destructive forces to the maxillary anterior dentition (Figure 16, Figure 17, Figure 18 and Figure 19). All anterior centric contacts should be lighter than posterior contacts. The clinician also examined the envelope of function to make sure it was in harmony with the rest of the teeth. All eccentric movements were analyzed, ensuring that the incisal edges of the upper teeth glided against the lower incisors like skates in a ring.
Conclusion
Prosthetic closure without orthodontics can be a predictable option, but first a systematic approach must be followed. This article reviewed the leading causes of spacing in the maxillary anterior dentition and presented a systematic way to predictably manage space through a predetermined plan or wax-up. Once the wax-up is transferred to the mouth, it can be viewed by the patient and verified by the dentist. Remember that the dentist’s ultimate goal is to pay attention to the patient’s esthetic concerns and create an esthetic arrangement that complements the patient’s smile.
References
1. Edwards JG. The diastema, the frenum, the frenectomy: A clinical study. Am J Orthod. 1977;71(5):489-508.
2. Ward DH. A study of dentists’ preferred maxillary anterior tooth width proportions: Comparing the recurring esthetic dental proportion to other mathematical and naturally occurring proportions. J Esthet Restor Dent. 2007;19(6):324-337.
3. Cohen M. Interdisciplinary Treatment Planning: Principles, Design, Implementation. Chicago: Quintessence, 2008:7.
4. Chiche GJ, Pinault A. Esthetics of Anterior Fixed Prosthodontics. Chicago: Quintessence, 1994:22-28.
5. Brooks LE. Smile-imaging: the key to more predictable dental esthetics. J Esthet Dent. 1990;2(1):6-9.
6. McLaren EA, Giordano RA. Zirconia-based ceramics: material properties, esthetics, and layering techniques of a new veneering porcelain, VM9. Quintessence Dent Tech. 2005;28:99-111.
7. Giordano R, McLaren EA. Ceramics overview: classification by microstructure and processing methods. Compend Contin Educ Dent. 2010;31(9):682-688.
8. Albakry M, Guazzato M, Swain MV. Fracture toughness and hardness evaluation of three pressable all-ceramic dental materials. J Dent. 2003;31(3):181-188.
9. Albakry M, Guazzato M, Swain MV. Biaxial flexural strength, elastic moduli, and x-ray diffraction characterization of three pressable all-ceramic materials. J Prosthet Dent. 2003;89(4):374-380.
About the Authors
Tyler P. Lasseigne, DDS, CDT
Private Practice
Baton Rouge, Louisiana
Assistant Clinical Professor
Department of Prosthodontics
Louisiana State University School of Dentistry
New Orleans, Louisiana
Todd C. Slogocki, DMD
Department of Prosthodontics
Louisiana State University
New Orleans, Louisiana
Michael Bellerino, CDT
Trinident Dental Laboratory, LLC
Metairie, Louisiana