Clinical and Esthetic Considerations in the Treatment of Sports-Related Trauma to Anterior Teeth
Successful treatment planning despite time constraints in a case involving a college-bound athlete
When approached in a collaborative, team-oriented manner, treatment for sports-related injuries of the anterior teeth in children and adolescents can have a winning outcome. The ideal treatment for patients who present with anterior tooth fractures as a result of sports-related injuries must consider factors such as the condition and prognosis of the injured teeth, esthetics, longevity, age of the patient, length of time and commitment required for the treatment(s), social and financial aspects, and multidisciplinary requirements (eg, orthodontics, endodontics, periodontics).
Whatever other considerations may apply, endodontic and restorative concerns must play a primary role when treating tooth fractures. Exposed dentinal tubules are vulnerable to bacterial invasion into the endodontic system, requiring the application of a protective dressing as part of the immediate endodontic emergency treatment. Once the dentin is sealed, restorative treatment can be performed at a subsequent stage.1
The most frequent types of traumatic dental injuries to permanent teeth—most commonly the maxillary central incisors—are enamel fractures, enamel and dentin fractures, and enamel and dentin fractures with pulp exposure. Depending on the levels of trauma, as well as the social/psychological aspects of treatment, injured teeth can be treated through such cosmetic approaches as direct composite layering technique, laminate veneers and ceramic crowns over the teeth, and/or implants.
To restore function and esthetics in less severe cases, the fractured tooth fragment can be reattached using adhesive protocols. If reattachment is difficult or not possible, current composite materials provide superior esthetic results. Particularly in cases involving immature teeth with an extensive coronal pulp dimension, minimally invasive direct composite restorations are preferred over more invasive indirect restorations. 1
Ensuring that future treatment is based on a solid foundation of healthy and stable tooth structure and gingival architecture is of paramount importance in treatment planning. Consequently, time factors and the age of the patient are important variables that must be considered during treatment planning. This is especially true when deciding whether to preserve traumatized teeth by root canal treatment or to extract fractured teeth and replace them with implants.
When determining whether an injured tooth with a questionable prognosis should be kept or replaced by an implant, it is important to consider local, site-specific factors as well as more general patient-related aspects.
Time constraints imposed by patients or their parents further compound the challenges involved in achieving the most ideal esthetic and functional results in cases of traumatic tooth injuries. When this occurs, the most appropriate—preferably conservative—options that can provide the patient with the most long-term and functional results should be considered.
In some cases, reattachment of tooth fragment provides esthetic results while being minimally invasive. Its main advantage is that all the alternative methods are still available in the event of failures and/or refractures.
Treatment-planning considerations sometimes may require less than ideal compromises to arrive at an outcome that most satisfactorily meets the overall needs and expectations of the entire dental team. Therefore, a multi-disciplinary approach that ensures the endodontic and periodontal health of the patient, while also incorporating the use of restorative materials that support a long-term and esthetic result, is needed. The following case presentation supports such a multidisciplinary approach.
Additionally, patients should be fully informed of the ideal treatment versus what is being recommended as preferred given their established parameters. Only after full disclosure is given and consent is received can a case such as the following be undertaken.
Case Presentation
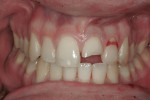
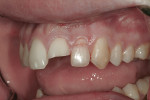
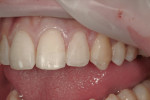
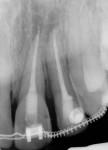
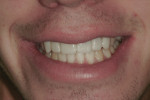
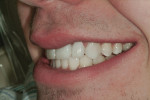
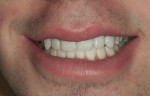
A 17-year-old male patient presented for emergency care after sustaining a sports injury affecting teeth No. 9 through No. 11. Fractures included the bottom third to half of tooth No. 9 and about 90% of tooth No. 10, which was barely attached (Figure 1 and Figure 2). Immediate endodontic treatment was initiated on teeth No. 9 and No. 10, and the fractured tooth pieces were bonded back into place with composite (Figure 3).
A pulpotomy was performed on teeth No. 9 and No. 10, and root canals were completed 2 days later; no posts were placed at any point during the treatment process. To re-bond the tooth fragments, a total-etch technique was used (Ultra-Etch®, Ultradent Products, Inc., www.ultradent.com; One-Step®, Bisco, Inc., www.bisco.com; Filtek™ Supreme Flowable, 3M ESPE, www.3mespe.com) and the adhesive materials were cured for 20 seconds with an LED curing light (Bluephase®, Ivoclar Vivadent, www.ivoclarvivadent.com).
The patient was referred to an orthodontist to determine if tooth No. 10 could be extruded rapidly, since the fracture involved most of the coronal portion of the tooth and extended subgingivally on the palatal. This option appeared the most prudent course of action compared to the more aggressive alternatives.
Radiographic and clinical examination revealed that the fracture line was at or just below the alveolar crest of bone on the lingual aspect of the tooth. Given the gingival extent of the fracture on No. 10, it could not properly be restored without violating the biologic width. Further evaluation of the crown length, coupled with the cosmetic location of the tooth, made standard osseous crown lengthening procedures not ideal.
Two orthodontic methods were discussed to expose the subgingival defect on tooth No. 10: slow eruption of the tooth followed by osseous crown lengthening2,3 and rapid eruption of the tooth coupled with circumferential fibrotomies.4,5
After a full disclosure and comprehensive discussion of all the available options with the patient and his parents, along with the advantages and disadvantages of each, a conservative treatment plan was developed. The treatment plan combined the previously performed endodontic treatment to save the traumatized teeth, orthodontics to rapidly extrude the tooth, a fiberotomy around the tooth as it is extruded downward, and lithium disilicate veneers (IPS e.max®, Ivoclar Vivadent) on teeth No. 6 through No. 11.6
Completing the endodontic treatment would provide tooth health during the orthodontic treatment and stabilize the pulpal situation of the two fractured teeth. The orthodontic treatment to extrude tooth No. 10 would provide ferrule and biologic width for the restoration and maintain gingival esthetics.7,8
The fiberotomy around tooth No. 10 would also help contribute to its esthetics, as well as patient comfort and satisfaction, by helping correct gingival margin discrepancies and prevent unwanted regression to the tooth’s pre-orthodontic condition.2,9
Orthodontic Protocol
The patient had undergone previous orthodontic treatment, and his upper teeth were otherwise well aligned. He presented with some mild lower anterior spacing that he and his parents elected to close with orthodontic appliances to create more room (overjet) for the upper anterior restorative work.
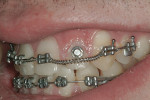
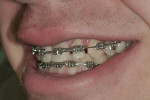
Stainless steel, .022-inch slot brackets were placed on teeth No. 5 through No. 9, No. 11, and No. 12 in a level fashion on the middle third of the teeth. For tooth No. 10, a stainless steel button was placed as gingival as possible. Additionally, the incisal edge of No. 10 was equilibrated to provide ample eruption room. A .018-inch stainless steel wire was placed with a passive coil spring in the No. 10 area to maintain exact arch length during extrusion. A .030 elastic thread tied from the button on No. 10 to the arch wire was used to apply orthodontic eruption pressure (Figure 4 and Figure 5).
The patient was re-appointed every 1 to 2 weeks to replace the elastic thread and reactivate the extrusion forces. At approximately week seven, the restorative dentist performed a circumferential fibrotomy and removed some excess buccal and lingual hyperplastic tissue. In week 8, the eruptive forces on No. 10 were stopped, and a bracket was placed to stabilize its vertical position. An elastic chain also was used to center the tooth horizontally in its space (Figure 6).
Following an additional 6 weeks of stabilization, the orthodontist removed the wire and sent the patient to the restorative dentist so an impression could be taken for the diagnostic wax-up. The ceramist removed the brackets from the model and waxed up what would be the ideal shapes and contours of the teeth. The wires were replaced.
Following an additional 2 weeks of stabilization, the orthodontic appliances were removed (Figure 7). The restorative dentist prepared teeth No. 6 through No. 11 the same day and placed a splinted provisional.
To enable establishment of ideal finish lines, it would have been preferable to schedule a thorough hygiene appointment for 2 weeks post-braces removal and prior to preparation to allow tissue irritation and inflammation—which prohibits a thorough cleaning—to subside.
Preparation & Provisionalization Protocol
Veneer preparations were completed on teeth No. 6 through No. 8 to facilitate an esthetic and uniform appearance. An “aggressive veneer” preparation was performed on tooth No. 9, taking the incisal edge to the fracture line. A crown preparation was performed on tooth No. 10, which was now a very small tooth, since it was 80% root and very narrow. Tooth No. 11 received a simple veneer preparation, because it had sustained a fracture line across the facial that was palpable, but not symptomatic, from the trauma.
The patient’s tooth shade was determined to be 040. To provisionalize the teeth, the preparations were coated with a desensitizer (Telio CS Desensitizer, Ivoclar Vivadent) and then a primer (OptiBond FL® Primer, Kerr Corporation, www.kerrdental.com). The idealized wax-up was used to create a matrix (Sil-Tech®, Ivoclar Vivadent) for the provisional restorative material (Luxatemp®, DMG America, www.dmg-america.com). The matrix loaded with provisional material was seated on the preparations, and the provisionals were “locked in,” polished, and adjusted intraorally. The patient left for college that day with the provisional restorations in place (Figure 8 and Figure 9).
Cementation Appointment
The patient returned for placement of the definitive restorations, which were completed according to standard total-etch adhesive protocol (Ultra-Etch, Ultradent; ALL-BOND 3® adhesive, Bisco; Variolink® Veneer cement in shade +1, Ivoclar Vivadent). Upon seating, the restorations were cured for at least 20 seconds per tooth from the buccal and lingual aspects.
Discussion
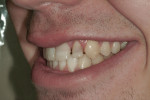
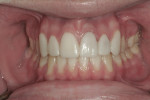
The patient was well pleased with the esthetic outcome of the case (Figure 10 through Figure 12). However, from a dentist and laboratory perspective, the esthetic outcomes of the case could be critiqued. The patient’s time constraints placed certain restrictions and limitations on the treatment; due to the pressure to complete treatment, certain aspects of treatment were hurried, allowing insufficient time for soft-tissue healing prior to placement of the final restorations. Since teeth No. 9 and No. 10 were darker than teeth No. 7 and No. 8, an opaquer was required in the restorations, which caused them to appear more opaque than desired.
Conclusion
Although the case presented some minor esthetic limitations, it did provide the patient with an acceptably esthetic treatment in time for him to begin college. By incorporating conservative approaches to treatment and combining other dental disciplines, the teeth traumatized in the sports injury could be saved in a safe and conservative manner that offered patient satisfaction in terms of treatment completion and teeth function, durability, periodontal health, tooth structure stability, and esthetics. This conservative approach has established a solid foundation for the patient and his dental team should he need to or wish to pursue treatment alternatives, such as implants, at a future date.
References
1. Krastl G, Filippi A, Zitzmann NU, et al. Current aspects of restoring traumatically fractured teeth. Eur J Esthet Dent. 2011;6(2):124-141.
2. Kawanami M, Andreasen JO, Borum MK, et al. Infraposition of ankylosed permanent maxillary incisors after replantation related to age and sex. Endod Dent Traumatol. 1999;15(2):50-56.
3. Nugala B, Kumar BS, Sahitya S, et al. Biologic width and its importance in periodontal and restorative dentistry. J Conserv Dent. 2012;15(1):12-17.
4. Medeiros RB, Mucha JN. Immediate vs late orthodontic extrusion of traumatically intruded teeth. Dent Traumatol. 2009;25(4):380-385.
5. Fricke LL, Rankine CA. Comparison of electrosurgery with conventional fiberotomies on rotational relapse and gingival tissue in the dog. Am J Orthod Dentofacial Orthop. 1990;97(5):405-412.
6. Kocadereli I, Taşman F, Güner SB. Combined endodontic-orthodontic and prosthodontic treatment of fractured teeth. Case report. Aust Dent J. 1998;43(1):28-31.
7. Addy LD, Durning P, Thomas MB, McLaughlin WS. Orthodontic extrusion: an interdisciplinary approach to patient management. Dent Update. 2009;36(4):212-218.
8. Goldberg PV, Higginbottom FL, Wilson TG. Periodontal considerations in restorative and implant therapy. Periodontol 2000. 2001;25:100-109.
9. Yoshinuma N, Sato S, Makino N, et al. Orthodontic extrusion with palatal circumferential supracrestal fiberotomy improves facial gingival symmetry: a report of two cases. J Oral Sci. 2009;51(4):651-654.
About the Authors
Brent A. Engelberg, DDS
Private Practice
Arlington Heights, Illinois
Jerome A. Jarosz, DDS, MS
Private Practice Specializing in Orthodontics
Arlington Heights, Illinois
Brad Jones, CDT, FAACD
Owner
Smiles, Inc.
Boise, Idaho