The New Generation of Self-Adhesive Resin Cement
Jeff T. Blank, DMD
Simplifying ceramic onlay cementation for fast, easy, and sensitivity-free results.
With the advent of modern ceramics and state-of-the-art adhesive dentistry, clinicians may now predictably restore many large failing amalgams and moderate to severe carious lesions more conservatively by using all-ceramic inlays and onlays. Though full-coverage all-ceramic crowns are often indicated, to routinely default to crowns when sufficient buttressing tooth structure remains dictates overly aggressive preparation and senseless amputation of healthy tooth structure. Properly bonded ceramic inlays and onlays permit the clinician to remove only the affected/damaged portion of the tooth and leave the healthy surrounding enamel and dentin intact. This type of treatment represents the most conservative restorative option in many cases.
Choosing the Proper Cement
All-ceramic inlays and onlays should be cemented with a resin cement system.1 Resin cements are capable of high bond strengths to both properly treated porcelain (depending on the porcelain system) and to enamel and dentin. Resin cements are the least soluble and have the highest compressive and tensile strength of all currently available cement systems.2 Though light-cure-only resin cement systems can be used to cement all-ceramic inlays and onlays, some clinicians prefer to use dual-cure systems with opacious ceramics for deep cavity forms or in any clinical situation where adequate curing-light intensity to the base of the restoration is uncertain. Using the "wave technique" (in which the clinician seats the restoration and "waves" the curing light over the residual excess to initiate polymerization but not complete the cure), the excess cement around the margins and within interproximal spaces can be easily removed in the gel state, and a more definitive light-curing phase can continue the polymerization. In deep areas where complete light activation is questionable, the dual-cure autopolymerization mode ensures final set of the resin cement.
Proper cement selection and bonding protocols are extremely important to the long-term success of these restorations. Many clinicians prefer to cement all-ceramic inlays and onlays with self-etching, dual-cure resin cements. The advantages of these systems are that, once mixed, they contain both the self-etching adhesive and dual-cure resin cement in a single formulation, so a separate bonding adhesive is not required. This significantly reduces the number of steps, leaving less room for operator error. Self-etching, dual-cured resin cements can be dispensed directly into the preparation or onto the restoration surface and seated much like conventional cement systems.
One of the first self-etching, dual-cure resin cements was RelyX™ Unicem Self-Adhesive Resin Cement (3M ESPE, https://www.3mespe.com). The original formulation contained the precise ratio of catalyst/base in a dispensing capsule. The capsule was activated and mixed in an amalgam triturator, placed in a dispensing gun, and injected into the cavity form through a convenient, optimally sized cannula tip. This dispensing system eliminated the need for hand mixing, which is messy and difficult to dispense into the preparation, and ensured proper catalyst/base ratios and exact mixing time. RelyX Unicem possessed acceptable bond strength3 and desirable handling and clean-up characteristics.
The New Generation of Self-Adhesive Resin Cement
The latest innovation in self-etching, dual-cured resin cement is RelyX™ Unicem 2 Automix Self-Adhesive Resin Cement from 3M ESPE. This material represents the next generation of automix resin cement, ideal for luting all-ceramic inlays and onlays.4,5 Building on the original RelyX Unicem cement formulation and its proven 7-year clinical history, RelyX Unicem 2 Automix cement offers advancements in shear bond strength, long-term bond strength, and resistance to discolorations, as well as virtually no postoperative sensitivity.6 Additionally, this latest formulation reaches a neutral pH in roughly 24 hours, rendering the resin cement hydrophobic and resistant to nanoleakage of dentinal fluid. A number of researchers have reported that some simplified adhesives and resin cement systems are too hydrophilic, and porous channels called "water trees" can form during polymerization, which can lead to incomplete cross-linking, poor physical properties, unreacted monomers reaching the pulp, and reduced bond strength.7,8 However, RelyX Unicem 2 Automix cement has been formulated to render a hydrophobic seal over open dentinal tubules through faster acid neutralization time and improved chemistry.
The most distinct advantage of RelyX Unicem 2 Automix cement is that it is dispensed from a dual-barreled automix syringe and convenient spiral mixing tip. Depending on the cavity size, a very small endodontic tip or a larger intraoral tip can be attached to the wide mixing tip for precise cement application in any cavity form, or even directly into an endodontic canal. RelyX Unicem 2 Automix cement comes in three shades-Translucent, A2 Universal, and A3 opaque-offering the needed range to allow any restoration to disappear into the surrounding tooth structure.
Case Presentation
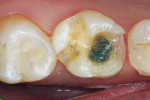
A patient presented to the office with a large, cariously involved amalgam on tooth No. 3. While it was initially suspected that a full-coverage crown might have been necessary, upon removal of the failing restoration and recurrent decay it was determined that there was sufficient remaining tooth structure to permit a more conservative porcelain onlay. The mesial-buccal cusp was completely undermined with decay; therefore, it was reduced for porcelain coverage. A final impression and a bite registration were taken and a temporary restoration was placed. The patient returned in 2 weeks for cementation of an all-ceramic, laboratory-processed porcelain onlay.
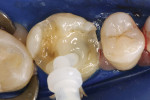
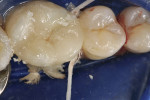
The patient was anesthetized and the provisional restoration was removed (Figure 1. The restoration was inspected for proper hydrofluoric acid-etching and for fit on the master model (Figure 2. It was tried in with a small amount of water and assessed for fit, marginal seal, and interproximal contact. Once verified for accuracy in the mouth, the inner surface was cleaned with acetone and silanated (Figure 3.
RelyX Unicem 2 Automix cement in a translucent shade was chosen to cement this case for its no-mix, easy to dispense delivery system, high bond strengths, excellent handling properties, color stability, adequate working time, and ease of clean-up of the residual cement.
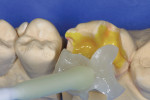
A rubber dam was placed and tooth No. 3 was ligated around the cervical neck with floss for ideal isolation and to ensure that the dam material would not interfere with the seating of the restoration. The cavity preparation was cleaned with Gluma® Desensitizer (Heraeus, https://www.heraeus-dental-us.com) and air-dried. Because of the open cavity form, the intraoral tip of the cement was attached to the wide mixing tip to ensure full distribution along all aspects of the preparation. The intraoral tip was placed directly into the cavity form and an even layer of RelyX Unicem 2 Automix cement was expressed with gentle finger pressure (Figure 4. The all-ceramic onlay was pulled from the working die using a wax applicator and placed into the preparation. An amalgam condenser was used to firmly seat the restoration (Figure 5.
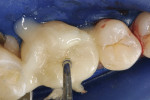
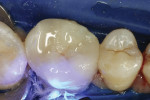
Using the "wave technique," an LED curing light was waved over the restoration from the buccal and lingual surfaces for approximately 5 seconds. This technique begins the polymerization of the residual cement, but only to the gel/semi-solid state. Excess residual cement was then easily removed with a sickle scaler (Figure 6 and the interproximal material was cleared with floss (Figure 7. More than adequate working time with full operatory lighting enabled complete removal of the residual cement in less than 2 minutes. Once all excess resin cement was removed, a glycerin gel (DeOx®, Ultradent Products, Inc, https://www.ultradent.com) was placed over all of the cavosurface margins to inhibit the formation of an air-inhibited layer at the cement interface, which can lead to marginal ditching and staining by chromagenic foods and beverages. The final light-cure of 1 minute per surface was initiated (Figure 8. A composite-impregnated cup (Enhance®, DENTSPLY Caulk, https://www.caulk.com) was used to remove and smooth any bonded excess along the margins. The rubber dam was removed and the occlusion was refined with a fine diamond.
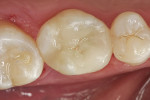
Figure 9 shows the completed restoration. Note that the cement's translucent shade permitted a seamless, vital, monoblock restoration while conserving tooth structure.
Conclusion
Conservative, well-bonded, all-ceramic inlays and onlays are often the ideal restorations for moderate to large cavity forms. The success of these restorations often relies on the efficiency and durability of the bond interface between the tooth and the ceramic. RelyX Unicem 2 Automix cement exhibits ideal handling, physical properties, and ease of clean up, coupled with exceptional bond strength, color stability, and hydrophobic seal of dentinal tubules. The new Automix dual-barreled syringe and choice of two sizes of dispensing tips make this product an excellent choice for not only all-ceramic inlays and onlays, but all-ceramic crowns and laboratory-processed composite as well.
Disclosure
The author has received an honorarium from 3M ESPE.
References
1. Kramer N, Lohbauer U, Frankenberger R. Adhesive luting of indirect restorations. Am J Dent. 2000;13(Spec No):60D-76D.
2. Yoshida K, Tanagawa M, Atsuta M. In-vitro solubility of three types of resin and conventional luting cements. J Oral Rehabil. 1998;25(4):285-291.
3. 3M ESPE. RelyX Unicem Technical Product Profile. Available at: https://multimedia.mmm.com/mws/mediawebserver. Accessed October 11, 2010.
4. Taschner M, Frankenberger R, Petschelt A, Kramer N. IPS Empress inlays luted with a self-adhesive resin-cement after two years. J Dent Res. 2007;86(Spec Iss B):0013.
5. Peumans M, De Munck J, Van Landuyt K, et al. 2-year clinical effectiveness of a self-adhesive luting agent. J Dent Res. 2008;87(Spec Iss C):0331.
6. 3M ESPE. RelyX Unicem 2 Automix Self-Adhesive Resin Cement Technical Product Profile. Available at: https://multimedia.3m.com/mws/mediawebserver. Accessed October 11, 2010.
7. Tay FR, Pashley DH. Water treeing-a potential mechanism for degradation of dentin adhesives. Am J Dent. 2003;16(1):6-12.
8. Chersoni S, et al. In vivo and in vitro permeability of one-step self-etch adhesives. J Dent Res. 2004;83(6):459-464.