In-Office Posterior Crowns
Using lithium disilicate and in-office CAD/CAM for replacing posterior PFM restorations.
John Schwartz, DDS
Dentists are often faced with the need to replace existing porcelain-fused-to-metal (PFM) crowns in the posterior segment with equally durable, yet esthetic, alternatives when patients present with deteriorating restorations. Historically, this has required replacement with another PFM restoration.1 In more recent years, high-strength, metal-free ceramics characterized by a dull, overly opaque appearance also have been used.1 Sometimes, however, patients are left with less than desirable esthetic results.
Lithium Disilicate
As a restorative material, lithium disilicate (IPS e.max® CAD, Ivoclar Vivadent, https://www.ivoclarvivadent.com) offers many options and benefits for single-tooth restoration.2 The material has the ability to produce highly esthetic results that have been reported by the manufacturer to be 2.5 to 3 times stronger than conventional glass-ceramic restorations.2 It can be pressed or machined in the dental laboratory,2 and with its high strength (360 MPa to 400 MPa) it offers a number of options for cementation and seating.3
Lithium-disilicate restorations can either be veneered using highly esthetic materials or fabricated to full contour and given characterization effects with staining materials.2 The material is also appropriate for use with severely discolored teeth or titanium abutments, as lithium-disilicate restorations can cover unnatural coloring as well as provide the correct opacity to the final restoration.4
IPS e.max CAD
IPS e.max CAD was developed to take advantage of the impressive qualities of lithium disilicate and provide a high-performance restoration that demonstrates high esthetic value as well as ease of use.2 IPS e.max CAD is designed to use the efficiency of CAD/CAM processing-whether in the dental office or in a laboratory-to create restorations that are stronger than those made with conventional materials.2 Because of its ability to be machined in an intermediate state, the technician in the laboratory or the dentist in the office can manually adjust or cut back the material while it is in this "soft" state, allowing the fit to be checked and corrected as required by the treatment plan and the patient's preferences.2
IPS e.max CAD is indicated for veneer, inlay, and partial- to full-crown restorations for individual teeth,2 and allows these restorations to be conventionally placed, so that no new materials or techniques are required.4 The material crystallizes at 850°C in just 20 to 30 minutes. When the crystallization process is complete, it exhibits its final strength of 360 MPa and highly esthetic characteristics, such as shade, translucency, and brightness.4
IPS e.max CAD comes in block form and is available in three different levels of translucency, including high translucency (HT), low translucency (LT), and high opacity (MO), as well as two sizes.2 Depending on the specific case, IPS e.max CAD allows laboratory technicians (or dentists, if using in-office CAD/CAM) to choose the appropriate block and processing technique, such as staining, cut-back, or layering.2
Chairside CAD/CAM
In-office CAD/CAM technologies, such as the E4D Dentist CAD/CAM system (D4D Technologies, https://www.e4d.com), enable dentists to scan, design, and mill restorations in the office.5 This is most useful in high-volume practices where flexibility and higher production is a must. Dentists can scan the tooth or teeth to be restored and send the restoration specifications over the Internet to the E4D "studio" (ie, the computer where the restoration will be designed), so that the restoration may be designed and milled. With the E4D Sky Network, the entire case, scanned or designed, can be sent to the studio with just one click of a button. This feature allows dentists to move from one patient to the next easily and efficiently. The E4D system can be used to produce one-visit lithium-disilicate restorations (ie, IPS e.max CAD) with exceptional esthetics and high strength.4
Case Report
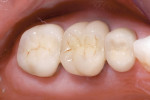
A 45-year-old woman presented with a chief complaint of not being happy with the appearance of tooth No. 13 (Figure 1). She complained that it looked "fake" and made her self-conscious in public situations, as she felt that people stared at it.
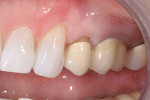
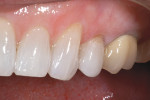
Clinical and radiographic examination revealed generalized chronic, mild gingivitis, with pockets limited to 3 mm or less; mild recession; and minimal root exposure (Figure 2). The patient also presented with an anteriorly bleached dentition and posterior PFM molar crowns of average color, shape, and marginal integrity, which showed gingival shadows and opaque cervical thirds. Radiographic analysis revealed that tooth No. 13 was an all-ceramic crown, and marginal caries were present on teeth Nos. 13 and 15.
Treatment Plan
The treatment plan for this case consisted of replacing the crowns on teeth Nos. 13 and 15, which would be milled from a lithium-disilicate material and bonded into place using a total-etch, dual-cure bonding system. The patient was offered the opportunity to replace the crown on tooth No. 14 for appearance-related reasons, but she declined.
One-Visit Clinical Protocol
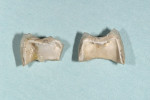
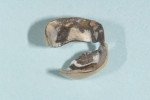
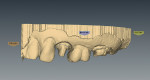
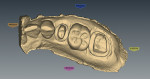
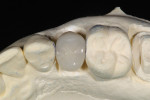
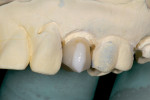
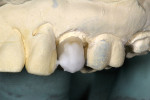
The patient was anesthetized with local anesthetic (eg, 2% lidocaine with 1:100,000 epinephrine). The old crowns were removed by sectioning, after which caries were removed (Figure 3 and Figure 4). Teeth Nos. 13 and 15 were reshaped with 1.2-mm shoulder margins and 2-mm occlusal clearances. A polyvinyl siloxane (PVS) impression was taken, models were poured, and the prepared tooth margins were trimmed, after which they were scanned into the in-office CAD/CAM instrument (E4D) (Figure 5 and Figure 6).
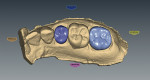
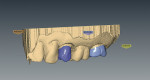
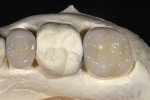
The restoration was designed virtually, using a computer and the E4D restoration design software. An HT-A1 block was milled according to the CAD/CAM design (Figure 7 and Figure 8). Once milled, the molar crown was stained and glazed during the crystallization firing process. The bicuspid crown was crystallized and stained for internal characterization (Figure 9). IPS e.max S1 enamel, Effect 1, and Effect 3 porcelain powders were then fired on the facial surface to complete the bleach characterization process and match the shade and characterization of the dentition (Figure 10, Figure 11, Figure 12). The intaglio surface was etched with hydrofluoric acid for 20 seconds, followed by a complete rinse. The restoration was then silanated for 1 minute, and an unfilled resin was lined to lower the surface tension for the cement.
The teeth were prepared for cementation by cleaning the surfaces with pumice and water. Multilink® A&B solution (Ivoclar Vivadent) was then applied. Excess material was removed with pressurized air, and the preparation was allowed to sit for 30 seconds. The transparent shade of Multilink® Automix-Plus (Ivoclar Vivadent) was then loaded into the crowns, after which they were seated using the wave cementation technique (Figure 13), and light-cured for 1 minute.
Conclusion
This case is a significant example of how PFM restorative technology can be visually compared to today's durable and esthetic all-ceramic technologies that can be cemented using conventional cement and techniques.3 Using lithium-disilicate material (ie, IPS e.max CAD), clinicians can fabricate strong and natural-looking posterior crowns in the office, and predictably bond them into place (Figure 14).4 In this author's opinion, lithium disilicate satisfies esthetic requirements far better than other high-strength, metal-free materials.1 Best of all, the case presented here was completed in one visit.
References
1. Walia S, Thomas PM, Sandhu H, Santos GC Jr. Restoring esthetics with metal-free ceramics: a case report. J Can Dent Assoc. 2009; 75(5):353-355.
2. Baltzer A. All-ceramic single-tooth restorations: choosing the material to match the preparation-preparing the tooth to match the material. Int J Comput Dent. 2008;11(3-4):241-256.
3. Reich S, Uhlen S, Gozdowski S, Lohbauer U. Measurement of cement thickness under lithium disilicate crowns using an impression material technique. Clin Oral Investig. 2010 May 12.
4. Puri S. Comprehensive dentistry using chairside cad/cam technology: a case report. Dent Today. 2009;28(4):92, 94, 96.
5. Kurbad A, Reichel K. Cad/cam-manufactured restorations made of lithium disilicate glass ceramics. Int J Comput Dent. 2005;8(4):337-348.
About the Author
John Schwartz, DDS
Private Practice
Metairie, Louisiana