Predictable Outcomes in the Esthetic Zone
Demand for esthetic outcomes increases as more implants are used in the esthetic zone, and younger patients present in larger numbers for implant therapy in the new era of single-tooth and partial-arch reconstruction.
Applications of implant therapy have evolved from their initial use of supporting prostheses in edentulous mandibles with hybrid restorations. For these patients maintaining osseointegration and retention of the prosthesis were the primary goals of therapy. The restorations were generally moderately esthetic at best, focusing primarily on prosthesis function, retention, and cleansability.
Over the years that followed the introduction of endosseous implant dentistry in the 1970s and 1980s, dentists began to use dental implants in new ways. Once the concept of osseointegration was accepted, clinicians sought to use dental implants to replace failed or missing teeth in an assortment of scenarios including partial- and full-arch restorations, as well as single-tooth replacement. Additionally, implants were increasingly placed in the anterior segment in younger patients. In the early years, implant patients typically had a long history of attachment loss and tooth destruction resulting from caries. Today, these patients are still represented. However, younger patients are increasingly presenting for implant therapy as the era of full-mouth reconstructions gives way to single-tooth and partial-arch reconstruction. This evolution provided a new set of tools for dentists. By the same token, these new applications created a unique set of problems. Where implant therapy initially focused on prosthesis retention, esthetics is increasingly more demanding as implants are used in the esthetic zone.
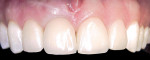
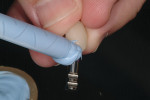
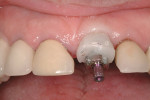
Today, implant-supported restorations are used for routine tooth replacement throughout the dentition with increasing demands placed on achieving natural-looking outcomes. The goal of therapy is to provide patients with an indistinguishable tooth replacement. To this point, Figure 1 and Figure 2 demonstrate a ceramo-metal implant-supported restoration inserted 2 years earlier for an otherwise healthy 32-year-old woman. Tooth No. 8 was lost as a result of recurrent symptomatic apical pathology despite several attempts at endodontic therapy. The tooth was ultimately replaced with an implant-supported restoration.
The anterior maxilla presents the greatest challenges for dentists and laboratory technicians in achieving esthetically pleasing outcomes with dental implants. The challenges can be broken down into two categories: patient-driven versus implant-driven. Patient-driven challenges include hard and soft tissue topography and volume, the nature of adjacent teeth, occlusion, gingival display, biotype, and patient expectations, to name a few. The International Team for Implantology’s recent publication of The SAC Classification in Implant Dentistry clearly delineates methods to identify these challenges and categorizes case types based upon the skill set required by the dental team in order to meet expectations (SAC stands for straightforward, advanced, and complex).1 Additionally, it describes realistic, reproducible outcomes, offering clinicians guidelines to educate patients about expectations given a specific case type.
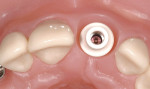
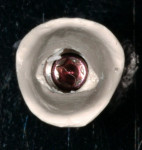
Implants themselves offer additional obstacles to predictably achieving natural-looking outcomes in the esthetic zone. Figure 3 demonstrates this challenge: implants are cylindrical in design as are impression copings and laboratory analogs, as well as most healing abutments and stock abutments. On the other hand, natural teeth demonstrate non-cylindrical cross-sections in the cervical zone. By example, maxillary anterior teeth have a triangular cross-section in the cervical zone as described by Wheeler in his description of dental anatomy.2 This is critical in developing and supporting the correct crown emergence through the transition zone between the implant and the supragingival environment.
Jemt and coworkers demonstrated that the shape of the peri-implant soft tissue was most quickly trained to the correct shape using provisional restorations versus healing abutments.3 The ITI’s Consensus Statement on the Use of Provisional Restorations states: “To optimize esthetic treatment outcomes, the use of provisional restorations with adequate emergence profiles is recommended to guide and shape the peri-implant tissue before definitive restoration.” 4 Predictably achieving natural-looking outcomes in the esthetic zone can best be achieved by mimicking the dentition’s crown emergence profile in the provisional restoration and ultimately communicating this information to the laboratory technician for fabrication of the final prosthesis.
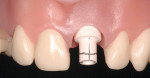
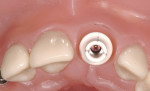
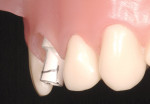
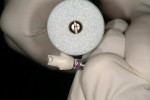
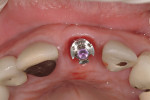
Given the challenges set forth by implant designs, it is critical to develop the transition zone by creating natural contours in a provisional restoration. Figure 4, Figure 5, Figure 6, Figure 7, Figure 8, Figure 9, Figure 10, Figure 11, and Figure 12 demonstrate the customization of a Straumann® Bone Level temporary abutment (Straumann USA, LLC, www.straumann.us). The abutment is marked in the mouth, identifying the buccal midline, the gingival zenith, buccal-palatal position of the peak of the papilla and desired incisal height of the abutment. The abutment is then removed from the mouth, placed on an appropriate implant analog and reduced to the desired contours to support a provisional restoration. Note that in addition to creating the supragingival contours, the tissue surface of the abutment is prepared as well to create a triangular cross-sectional shape mimicking the maxillary incisor’s natural shape at the cervical region. The tissue surface must be highly polished, in this case using a rubber wheel, to avoid bacterial accumulation in the subgingival environment.
In addition to creating a suitable cross-sectional shape for the transition zone, it is critical to create a scalloped interproximal form as well. This will lend itself to supporting the interproximal papilla. In the instance of cement-retained restorations, the interproximal scallop allows for coronal positioning of the cement line. This provides easy access for cement removal during crown placement.
The provisional restoration is then relined to fit the prepared abutment. The provisional restoration can be either screw- or cement-retained. Each treatment option offers unique benefits and disadvantages that will not be addressed in this discussion. Although the initial shape of the transition zone is round, following several months of tissue training with the provisional restoration and anatomically correct provisional abutment, the cervical tissues develop a “natural” shape conducive to supporting an esthetically pleasing final restoration. The provisional restoration should remain in place for no less than 8 to 12 weeks to allow for soft tissue development and maturation.
However, developing the transition zone is only part of the process in achieving a natural-looking restoration in the esthetic zone. An indistinguishable final restoration requires the laboratory technician to replicate the tissue contours developed by the provisional restoration. Traditionally, clinicians remove the provisional restoration and impression the implant and surrounding tissues using a cylindrically shaped impression coping using a polyvinyl or polyether impression material (Figure 13 and Figure 14). In the most capable hands, the process of placing an impression coping and syringing material into the new gingival sulcus as well as seating the filled impression tray takes several minutes. Given that the peri-implant tissues lack the resilience necessary to maintain their form once the provisional restoration is removed, the tissues subtly collapse. As a result, traditional implant impressions fail to capture the tissue contours developed by the previously described soft tissue development process. This is evidenced by the fact that gingival tissues blanch upon reseating the provisional restoration only moments after it is removed from the mouth.
Ideally, clinicians must transmit the newly developed tissue contours to the laboratory technician in a rigid manner. A custom impression coping should be fabricated to communicate this information. To accomplish this task, the provisional restoration is removed from the mouth and attached to an implant analog. A fast-setting impression or bite registration material is then applied to the cervical third of the restoration, and the analog is placed into a medicine cup filled with the same material. Figure 15, Figure 16, Figure 17, Figure 18, Figure 19, Figure 20 and Figure 21 demonstrate this process using GC Exabite™ II vinyl polysiloxane bite registration material (GC America, www.gcamerica.com). Once it is set, the provisional restoration and abutment are removed, leaving the implant analog in place along with an exact rigid replica of the transition zone. The buccal aspect should be marked on the impression material to facilitate proper seating of the custom impression coping. Next, an impression coping is attached to the implant analog, and a rigid, self-curing material is applied to fill the soft tissue replica. In this instance, a bis-acrylic composite (Luxatemp®, DMG, www.dmg-america.com) fills the transition zone and locks onto the open tray impression coping. Once the material sets, it is marked on the buccal aspect as described above. The custom impression coping is now removed from the implant analog, providing the clinician a rigid duplicate of the developed soft tissue complex.
At this point, the custom impression coping is seated appropriately in the patient’s mouth. Note the tissue blanching seen in Figure 22 as discussed earlier. Impression material is then syringed around the custom impression coping in a traditional fashion, and a filled impression tray seated. In this instance, Exaimplant™ hydrophilic vinyl polysiloxane impression material (GC America) is used with a stock impression tray that is customized with an access hole for the impression coping. Once the impression material is set, the impression coping is loosened and the tray is removed from the mouth. A laboratory analog is attached to the custom impression coping, and a stone model can be poured.
The laboratory technician now has the information necessary to replicate the transition zone in the final restoration, along with the height and location of the interproximal papilla and gingival zenith to achieve an ideal crown-emergence profile. The custom impression technique provides this information rigidly and does not require a soft tissue model or subjectively developing the crown-emergence profile in the dental laboratory.
Patients desire indistinguishable tooth replacement, particularly in the esthetic zone. With natural teeth this can be challenging. Implant-supported restorations offer greater challenges, not the least of which is developing the transition zone between the cylindrically shaped implant collar and the supragingival environment. Developing the soft tissue complex with a suitably designed provisional restoration is the most predictable way to accomplish this task. Communicating the exact dimension of the transition zone to the laboratory technician is easily achieved as well by using a custom impression coping. Together, these steps allow the restorative dentist and laboratory technician to accomplish natural-looking, implant-supported restorations in the esthetic zone.
Acknowledgments
The authors would like to acknowledge Drs. Joel Gale and Norman Lurie for their restorative dentistry performed on these patients.
References
1. Dawson A, Chen S, Buser D, et al. The SAC Classification in Implant Dentistry. Hanover Park, IL: Quintessence Publishing Company; 2009.
2. Ash MM, Nelson S. Wheeler’s Dental Anatomy, Physiology and Occlusion. Philadelphia, PA: Elsevier/WB Saunders Company; 1993.
3. Jemt T. Restoring the gingival contour by means of provisional resin crowns after single-implant treatment. Int J Perio Rest Dent. 1999;19(1):20-29.
4. Belser U, Martin W, Jung R, et al. Implant Therapy in the Esthetic Zone: Single-Tooth Replacements. Hanover Park, IL: Quintessence Publishing Company; 2007.
About the Authors
Frederic J. Norkin, DMD
Adjunct Associate Professor
Department of Periodontology
College of Dental Medicine
Nova Southeastern University
Fort Lauderdale, Florida
Private Practice
Florida Institute for Periodontics & Dental Implants
Boca Raton, Florida
Samuel ZFAZ, DDS
Adjunct Associate Professor
College of Dental Medicine
Nova Southeastern University
Fort Lauderdale, Florida
Private Practice
Florida Institute for Periodontics & Dental Implants
Boca Raton, Florida
Jeffrey Ganeles, DMD
Adjunct Associate Professor
College of Dental Medicine
Nova Southeastern University
Fort Lauderdale, Florida
Clinical assistant Professor
Goldman School of Dental Medicine
Boston University
Boston, Massachusetts
Private Practice
Florida Institute for Periodontics & Dental Implants
Boca Raton, Florida