Addressing Everyday Esthetic Challenges
Kevin C. Kopp, DDS, FACP
Dentist are challanged daily with the rigors of esthetic restorative dentistry. Equally challenging is selecting the appropriate dental material. The marketing of dental materials can cause confusion and, at times, complacency. Evidence-based solutions are available.
The challenges of effective hybridization,1 the effects of nanoleakage,2 shrinkage stress,3 appropriate adhesive system,4 composite compatibility,5 strength of composite,6 optical properties,7 color stability,8 and handling characteristics,9 to name a few, are equally as challenging for dental manufacturers. By working together with manufacturers through the sharing of their opinions, dentists can produce trusting relationships and some great solutions.
The following cases illustrate the author’s preoperative clinical evaluation of a new series of products. In all cases, rubber dam isolation was used in combination with cotton roll isolation.
A dual-cured, three-step universal dental adhesive system (ALL-BOND 3™ Universal [Direct/Indirect] Dental Adhesive System, Bisco, Inc, Schaumburg, IL) was selected. ALL-BOND 3 is ethanol-based, hydroxyethylmethacrylate (HEMA) free, hydrophobic, and radiopaque. This total-etch system is considered the gold standard2,10 in adhesive bonding and ethanol wet-bonding, which is a technique that has been tested extensively to show efficacy and clinical relevance.11-13 The composites that were used for treating the described cases were:
- ÆLITE™ All-Purpose Body/Dentin (Bisco, Inc)—a light-cured universal microhybrid composite known for its strength, handling, and color.
- ÆLITE™ Aesthetic Enamel (Bisco, Inc)—a highly reinforced, light-cured nano-filled composite known for its high strength, ease of polishability, and surface gloss.
- ÆLITE™ Aesthetic Enamel Incisal Shades (Bisco, Inc)—three incisal shades of the popular nanofilled composite.
Case 1
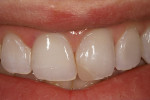
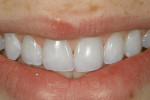
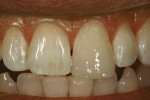
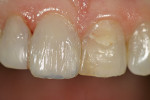
A young woman presented with a previously placed, monochromatic, Class 4 restoration. The challenges offered were duplicating the natural translucency, opacity, high value, and surface gloss of the existing natural dentition (Figure 1).
Shade selection was performed, and preoperative selections of composites were made. To address the challenges previously noted, a dentin/body shade of ÆLITE All-Purpose Body shade A1-O (opaque) was chosen for its strength, color, and opacity. To mimic the natural, youthful enamel, ÆLITE Aesthetic Enamel shade Bleach White (BW) was selected for its high value and translucency. And to provide incisal translucency and a high surface gloss, a layer of ÆLITE Enamel Incisal Clear would be placed.
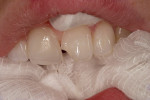
After anesthesia and isolation were obtained, the preexisting, monochromatic, defective restoration was removed using a high-speed handpeice with a diamond bur. A minimally invasive restorative design was accomplished, taking care not to break the mesial interproximal contact. To allow for better resin adaptation, all internal line angles were rounded and smoothed using diamond burs. A slight chamfer was placed around the entire margin to increase the enamel–adhesive surface and allow for adequate bulk of composite14 (Figure 2). The tooth was cleaned with a premixed slurry of pumice, rinsed, and dried.
UNI-ETCH® (Bisco, Inc) (32% phosphoric acid) with benzalkonium chloride (BAC) was used to etch the substrate surfaces totally. (Current self-etch adhesive bonds to enamel and dentin are thought to be more susceptible to degradation,13,15 possibly in part because of inadequate etching. BAC has been shown to leave a residual antimicrobial effect even after rinsing.16) The preparation was etched for 15 seconds and rinsed thoroughly. The excess water was removed with a foam pellet, leaving the surface visibly moist. Equal drops of ALL-BOND 3 parts A and B were mixed in a well for 5 seconds. Following the manufacturer’s instructions, two coats of the adhesive were placed, gently air dried, and light-cured for 10 seconds, followed by placement of one coat of ALL-BOND 3 Resin, which was similarly light-cured.
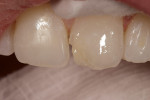
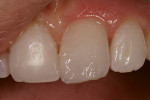
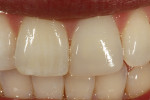
Using an NB composite instrument (Bisco, Inc), a 1-mm to 2-mm thick wall was created to replace the missing dentin structure using ÆLITE All-Purpose Body shade A1-O. Additional composite was added in 1-mm to 2-mm increments and light-cured for 20 seconds to a depth sufficient for adequate color, opacity, and strength. Sufficient space was left to allow for mesial, incisal, and surface enamel composite (Figure 3). ÆLITE Aesthetic Enamel shade BW in conjunction with ÆLITE Aesthetic Enamel Incisal Clear was used to mimic the qualities of natural enamel and allow the natural color of the underlying composite to shine through (Figure 4). Micro-hybrid composites, such as ÆLITE Aesthetic Enamel, can be polished with any existing polishing protocol. In this case, the final surface gloss was excellent (Figure 5).
Case 2
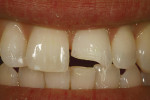
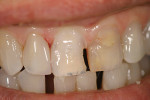
A man presented with a fractured maxillary left central incisor (Figure 6). The challenge was to replace a large amount of tooth structure and create a strong, lifelike restoration using a minimally invasive preparation design. In his clinical practice, the author has found that the key to successful completion of composite restorations is in understanding the very different roles dentin and enamel play in determining color.14 When this is understood, the clinician can choose a composite system that offers the versatility needed to complete challenging cases easily.
Shade determination was accomplished before isolation using a full mock-up. A minimally invasive preparatory design was completed, and the lingual aspect of the chamfer was left short of the occlusal contact area. The preparation was completed and polished with a premix slurry of pumice. A 37% phosphoric acid in semigel consistency with BAC (ETCH-37™, Bisco, Inc) was used. Etch-and-rinse systems have been studied extensively and have shown favorable long-term clinical data.17 The preparation was etched for 30 seconds and rinsed thoroughly. Excess water was removed with a foam pellet, leaving the surface visibly moist. Two coats of the adhesive were placed and cured, followed by one coat of ALL-BOND 3 Resin.
A thin lingual shelf of ÆLITE All-Purpose Body shade A1-O was created to block out the dark oral cavity and act as a reservoir for placement of the dentin layer (Figure 7). The artificial dentin chosen was ÆLITE All-Purpose Body/ Dentin shade A-1. Increments of 1 mm to 2 mm were added and photopolymerized to create contours and depth facial-lingually, interproximally, and incisally in preparation for placement of the artificial enamel. Small amounts of Incisal Clear were also added to provide incisal translucency (Figure 8). The enamel replacement selected was ÆLITE Aesthetic Enamel shade B-1 layered over the Enamel Incisal shade Frost (Figure 9). The final restoration was finished and polished using discs and polishing paste. A thin layer of BisCover™ LV (Bisco, Inc) could have been added if additional gloss was required. Final shade evaluation was accomplished 1 week postoperatively because of the dehydration effect and enamel lightening that occurs during tooth isolation. At the 1-week follow-up, the shade match was evident because the adjacent natural tooth was rehydrated (Figure 10).
Case 3
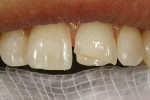
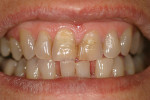
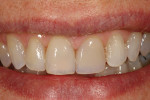
Revitalizing anterior teeth can be the restorative dentist’s greatest and most rewarding challenge. A woman presented with severely worn, fractured restorations. The patient wanted the most conservative and esthetic restorative procedure available. The challenge presented was to bring “life” back to her smile; to create a multilayered, polychromatic, strong restoration and to re-create the incisal length lost through wear (Figure 11).
The patient bleached her teeth for 4 to 6 weeks, stopping bleaching 3 weeks before the appointment to restore teeth Nos. 8 and 9. A shade mock-up was performed after removal of the old restorations. This case required dentin, enamel, and incisal replacement. Shade determination was accomplished and noted. The patient wanted a higher value of luminosity. It was determined that the high chroma of the cervical third of maxillary central incisors could be masked easily with the higher-value, opacious dentin shade selected.
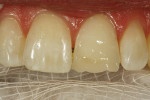
Before administering anesthesia and isolation, preoperative contact and excursions were recorded. The preexisting defective composite restorations and caries were removed using a high-speed handpiece with diamond burs. The enamel was roughened, chamfered, beveled, and rounded per minimal intervention design. The preparations were cleaned with a pumice slurry (Figure 12). Revitalization began with the maxillary right central, ending with the maxillary left central. Mylar matrices were used and bleeding was controlled.
ALL-BOND 3 adhesive was used because of its radiopaque qualities. The preparation was re-isolated and etched using ETCH-37 with BAC. The preparation was etched for 20 seconds (with care not to overetch the dentin) and rinsed thoroughly. The excess water was removed with a foam pellet, leaving the surface visibly moist. Two coats of the adhesive were placed and light-cured, followed by one coat of ALL-BOND 3 Resin.
The shade mock-up showed that the dentin replacement would be ÆLITE All- Purpose Body shade A-2, enamel replacement would be ÆLITE Aesthetic Enamel shade C-2, and incisal replacement would be ÆLITE Aesthetic Enamel Incisal Clear. Composite layering was performed with the use of modeling resin (Bisco, Inc) and the NB instrument kit. Modeling resin was a low-viscosity, HEMA-free composite sculpting/wetting agent that allowed exceptional sculpting. HEMA-free is a compelling benefit: If HEMA is present in the bonding agent, it could affect the long-term color stability of the final restoration.9 The composite was layered in 1-mm to 2-mm increments and light-cured for 20 seconds in a manner consistent with creating lifelike anatomy (Figure 13). The revitalization was completed using standard polishing protocols (Figure 14).
Conclusion
Blending science with the art of dentistry is now a reality. Evidence supports the use of highly polishable composite resins placed using a stratified placement technique which empowers dentists to accomplish esthetic restorative care for their patients. These clinical evaluations of a new product demonstrate their effective use for masking lingual darkness and enhancing polychromatic revitalization. By working together, dentists and manufacturers can continue to create products that meet the many challenges of esthetic restorative dentistry.
Disclosure
The author has received materials/product support and honoraria from Bisco, Inc.
References
1. Nakabayashi N, Kojima K, Masuhahra E. The promotion of adhesion by the infiltration of monomers into tooth substrates. J Biomed Mater Res. 1982;16(3):265-273.
2. Dörfer CE, Straehle HJ, Wurst MW, et al. The nanoleakage phenomenon: influence of different bonding agents, thermocycling and etching time. Eur J Oral Sci. 2000; 108(4):346-351.
3. Davidson CL, de Gee AJ. Relaxation of polymerization contraction stresses by flow in dental composites. J Dent Res. 1984;63(2): 146-148.
4. Van Meerbeek B, De Munck J, Yoshida Y, et al. Buonocore memorial lecture. Adhesion to enamel and dentin: current status and future challenges. Oper Dent. 2003;28(3): 215-235.
5. Schiltz MMY, Cincione F, De RijkWF, et al. Bond strength of single bottle adhesives to self-cured composites on dentin. Available at: www.bisco.com.
6. Anusavice KJ. Direct restorative materials. In: Anusavice KJ, ed. Phillips’ Science of Dental Materials. 11th ed. St. Louis, MO: Saunders; 2003:399-439.
7. Terry DA. The magic of light color. In: Groves RM, ed. Natural Aesthetics with Composite Resin. Mahwah, NJ: Montage Media; 2004: 4-17.
8. Paravina RD, Powers JP. Esthetic Color Training in Dentistry. St. Louis, MO: Mosby; 2004:75-77.
9. Radz GM. Conservative cosmetic dentistry—esthetic changes using the latest concepts in composite technology. Restorative Quarterly. 2001;4(2): 12-18.
10. Tseng KC, Weinberg GA, Woodlock DF. Dental adhesive—the foundation of esthetic dentistry. Gen Dent. 2007;55(7):698-712.
11. Carrilho MR, Tay FR, Sword J, et al. Dentine sealing provided by smear layer/smear plugs vs. adhesive resins/resin tags. Eur J Oral Sci. 2007;115(4): 321-329.
12. Sadek FT, Pashley DH, Nishitani Y, et al. Application of hydrophobic resin adhesives to acid-etched dentin with an alternative wet bonding technique. J Biomed Mater Res A. 2008;84(1): 19-29.
13. De Munck J, Van Meerbeek B, Braem M, et al. One-day bonding effectiveness of contemporary adhesives to bur-cut enamel and dentin [PhD dissertation]. An In Vitro and In Vivo Study on the Durability of Biomaterial-Tooth Bonds; 2004.
14. Terry DA. Adhesive preparation design. In: Groves RM, ed. Natural Aesthetics with Composite Resin. Mahwah, NJ: Montage Media; 2004:73-75.
15. Suh BI, Tay FR, Pashley DH, et a. Single-step adhesives are semi-permeable membranes. II. Morphologic and bond strength evidence. J Dent Res. 2002 (Spec Iss) Abstract 3829.
16. Chan DCN, Lo WW. Residual antimicrobial action of benzalkonium chloride-containing etchant [abstract]. J Dent Res. 1994;73 (Spec Iss): 226. Abstract 995.
17. De Munck J, Van Meerbeek B, Yoshida Y, et al. Four-year water degradation of total-etch adhesives bonded to dentin. J Dent Res. 2003;82(2):136-140.
About the Author
Kevin C. Kopp, DDS
Adjunct Clinical Associate Professor
Department of Restorative Dentistry
College of Dentistry
The University of Illinois
Chicago, Illinois
Private Practice in Prosthodontics
Elmhurst, Illinois