Considerations for Ensuring Complete Anesthesia During Endodontic Care
Ali Allen Nasseh, DDS, MMSC, PC
Although an emphasis is placed in the literature on instrumentation and obturation techniques, we cannot forget that a basic aspect of providing care is our ethical obligation to render it painlessly. The Hippocratic Oath urges us to “First, do no harm.” So, why is it that these succinct words often fall upon deaf ears? Mention the word root canal in public and you get reactions ranging from palpitation and sweating to seizures and fainting. Over the past 20 years, the media has played a large role in equating the experience of root canal therapy with passing a kidney stone. Expressions such as, “I’d rather have a root canal than do this or that horrible thing,” have been rampant; the root canal experience has been the butt of jokes on television shows, in comedy clubs, and in advertisements.
The question we need to ask ourselves as professionals is: “Why?” Why should any of our patients suffer during this procedure? What is an acceptable level of anesthesia failure, and what should we do about it? Is pain during some procedures a necessity or a consequence of mismanagement? Is predictable, profound anesthesia a myth or a realistic expectation? This article explains some concepts in local anesthesia, outlines possible causes of its failure in patients undergoing root canal therapy, and proposes the goal that all root canal therapy can and should be performed completely painlessly intraoperatively.
Root canal therapy in a vital pulp requires a high degree of local anesthesia. Due to direct manipulation of the myelinated A-delta and the unmyelinated C-afferent sensory neurons during a pulpectomy, this procedure is capable of producing intense, sharp pain if performed under inadequate anesthesia.1 Root canal therapy in an irreversibly inflamed tooth requires an even higher degree of anesthesia and is more prone to failure.2 However, the belief by many clinicians that a mild amount of pain is possible in some teeth during the root canal procedure is based on 2 fundamental assumptions. The first is that complete local anesthesia of all teeth is not always possible due to various local and systemic factors, such as low pH, presence of inflammation, patient apprehension, etc. The second reason is a byproduct of the first; it follows that if all teeth cannot be treated painlessly, then some degree of pain is inevitable if such procedures are performed. Unfortunately, both of these assumptions are false and have resulted in many traumatized patients sharing their horror stories postoperatively with family and friends, thereby perpetuating the myth of the dreaded root canal procedure.
A review of the literature reveals variable success rates in achieving anesthesia in the mandible and the maxilla.1 Factors influencing anesthesia success or failure include, but are not limited to, anatomical anomalies,3 inflammation,4 low pH of the injection site,1,5 and psychological factors such as apprehension.6 Overall, many factors have been theorized regarding the cause of anesthesia failure.1,7-10 However, one thing is clear. Although some study results reveal anesthesia failure rates of up to 80% in teeth with inflamed pulps,2 clinicians should not conclude that such teeth cannot be anesthetized. Most studies measure the rate of failure by testing the tooth after 1 round of anesthesia. Additional anesthesia, with alterations in technique or adjunct anesthesia devices, would often anesthetize such teeth.
True anesthesia failures (i.e., primary, secondary, and adjunct forms of anesthesia delivered skillfully that fail to anesthetize the pulp) are rare occurrences. This means that initial anesthesia failure in a tooth requiring root canal therapy is possible, but to use such occurrences as an excuse to proceed without proper anesthesia is unconscionable. Adequate anesthesia can be achieved despite initial failure through patience, skillful delivery of the anesthetic, and understanding of the original cause of failure. Some factors that contribute to anesthesia failure are discussed, and remedies to overcome them are proposed.
Anatomical Factors
The goal of local anesthesia for root canal procedures is to anesthetize the pulpal neurons and the periapical area. This is best achieved by delivery of the local anesthetic at the root apex.7 However, the cortical bone of the body of mandible can essentially block the anesthetic during a local infiltration at the root apex. The maxillary cortical bone is generally thinner; diffusion of the anesthetic through this bone is more readily achievable. For this reason, infiltration in the maxilla achieves a higher success rate than the mandible, where the cortical plate covering the root is thicker. In the mandible, block anesthesia is recommended as a more predictable approach, but it requires a better understanding of the deep anatomy of the jaw and is more technique sensitive, accounting for why anesthesia failures are more common in the mandible.
In both jaws, when local anesthesia fails after the first round of administration, subsequent anesthesia should not be placed in the same site. It has been shown that anesthetic blockage of the pain signal occurs more predictably when a greater axon surface area is in contact with the same volume of anesthetic. This results from the cumulative effect of a gradual reduction in conduction velocity throughout that length.11 A failing anesthetic block should be followed by injection at a different location (e.g., proximal or distal) to allow the cumulative effect of the anesthetic to block the pain signal potential more effectively.
Maxilla
In the maxilla, where infiltration anesthesia achieves a high success rate, failures commonly occur in teeth with roots with severe palatal curvatures, such as maxillary first premolars and the palatal root of maxillary molars, where the root is an average of 10.69 mm lingual to the buccal plate.12 In order to effectively anesthetize the palatal root of molars, a Posterior Superior Alveolar (PSA) nerve block is necessary, in addition to the 1 cartridge of buccal infiltration. Administration of a few drops of anesthetic palatally is also recommended to prevent discomfort from the rubber dam clamp that impinges on the palatal tissue. For the maxillary first premolar, buccal infiltration should be accompanied by palatal infiltration for the palatal root. Maxillary anterior teeth that have roots reaching the floor of the nasal cavity, or lateral incisors that curve too far palatally, require a palatal block such as the Palatal Anterior Superior Alveolar (P-ASA) nerve block,13 an Anterior-Middle Superior Alveolar (AMSA) nerve block,14 or adjunct forms of anesthesia, such as the Periodontal Ligament (PDL) injection or intraosseous anesthesia. For other maxillary teeth, a single cartridge of anesthetic in the form of infiltration is all that is necessary.
Mandible
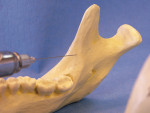
Local anesthesia in the mandible fails primarily because of inadequate proximity of the needle tip to the main trunk of the Inferior Alveolar Nerve (IAN). Poor understanding of the anatomy of the pterygomandibular fascial space, along with other problems among mandibles (e.g., needle deflection and anatomical variability), cause 10% to 15% failure with conventional blocks.1 Achieving bony contact with the lingula during the conventional mandibular block is crucial for success. Positioning the needle too anteriorly creates bony contact with the wrong area and causes anesthetic failure (Figure 1). If a first block fails, the next block should be placed somewhat more superior and posterior than the first.
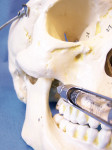
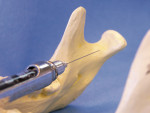
Alternatively, other block techniques (e.g., Akinosi and/or Gow-Gates)15,16 should be performed for the additional round of anesthesia (Figure 2a, Figure 2b). As a general rule, mandibular incisors are not anesthetized predictably with local infiltration. These teeth require mandibular blocks. Adjunct anesthesia techniques, such as intraosseous anesthesia, are also effective for such teeth.
Inflammation Factors
Inflammation and abscess in the involved teeth and surrounding area will act locally to increase circulation to the area and dilute the local anesthetic. Some prostaglandins, which are byproducts of the inflammatory process, sensitize nerve endings and reduce their threshold to stimulation. Inflammatory changes simply dilute the anesthetic and move it from the area more readily, causing potential anesthetic failures. Administering anesthetic injections into a site of inflammation or abscess is contraindicated. Not only can the abscess spread as a result of the injection, but it will dilute and transport the anesthetic faster, rendering it less effective. It is better to use blocks for sites of inflammation and infection so the nerve can be anesthetized proximal to the area of infection. For the maxilla, PSA techniques are preferable. Intraosseous anesthesia distal to the site of the infection is also beneficial in such situations.
pH Factors
For the local anesthetic molecule to work effectively, it must cross the axonal membrane and block the cytoplasmic end of sodium channels in neurons. The presence of a more acidic environment, which is the hallmark of inflammation and infection, increases the concentration of the ionic form of the anesthetic, which is then incapable of crossing the axon membrane.1 This reduces the effectiveness of the anesthetic molecules inside the axonal cytoplasm, where its action is required for proper anesthesia. The pH of an abscessed and severely inflamed area is highly acidic, reaching pH levels of up to 4.1 Anesthetic solutions with a lower pKa (i.e., dissociation constant) (e.g., Mepivacaine) may be more effective in such situations. Similar to cases where inflammation is present, regional blocks would be the preferable method of local anesthesia in such teeth, rather than injection.
Psychological Factors
Local anesthesia failures are more common in highly anxious patients. High anxiety levels can potentially reduce the pain threshold and cause local anesthesia failures.7 It is important that clinicians focus on patient relaxation through active listening, warmth, empathy, and a caring bedside manner. In cases where past dental experiences have created phobias, pharmacological prophylaxis in conjunction with local anesthesia is greatly beneficial. The use of nitrous oxide or an oral sedative is recommended in highly anxious patients. Local anesthesia failure would occur less frequently if these patients reach a baseline level of anxiety toward the treatment.
Adjunct Forms of Anesthesia
Today, technological advances enable us to predictably and efficiently deliver intraosseous anesthesia to the maxilla and mandible of those patients who cannot be anesthetized with conventional methods. Handpieces that perforate the cortical bone and deposit the local anesthetic into the medullary bone have solved the problem of diffusing the anesthetic across the impermeable cortical plate of bone. Such techniques have virtually eliminated the incidence of pain during root canal therapy in teeth where conventional anesthesia predictably fails. Many systems are available, with more yet to come. The goal is to streamline and facilitate local anesthesia delivery close to the periapex in a safe and effective manner.
However, intraosseous anesthesia procedures are invasive and should be used as an adjunct form of anesthesia when conventional anesthesia fails. Conventional anesthetics, performed skillfully, are capable of profound anesthesia in most teeth. Should a conventional block fail, intraligamentary injection could be attempted. If the intraligamentary injection also fails to provide adequate anesthesia, intraosseous anesthesia should be attempted first, prior to resorting to intrapulpal injections. As a rule, intrapulpal anesthesia is highly traumatic to the patient and should be avoided if possible. Interosseous anesthesia should be attempted first.
Testing Prior to Treatment
One thing practitioners can do to provide more humane treatment to patients is to test teeth with cold or an electric pulp tester prior to initiating an access opening. If a tooth responds in any way to thermal stimulation or the electric pulp test after administration of anesthesia and its onset, root canal therapy should not begin. Additional and adjunct forms of anesthesia should then be initiated and the tooth retested to determine the effectiveness of the anesthesia prior to access. This is the most important factor for painless root canal therapy. In this author’s experience, vitality testing prior to access opening is a potentially reliable method for estimating pulpal anesthesia. Starting the access opening and soliciting feedback from a patient via a bur is a breach of trust in the patient-doctor relationship.
Duration of Anesthesia
Although testing prior to initiating the procedure is imperative for pain management during root canal therapy, understanding that pulpal anesthesia lasts considerably less than tissue anesthesia is also another important consideration. Duration of effective pulpal anesthesia for Xylocaine 2% with 1:100,000 Epinephrine is no more than 60 minutes, whereas tissue anesthesia can be anywhere from 180 minutes to 300 minutes for the same dose.1 This means that prolonged treatments may result in diminished pulpal anesthesia and increased pain later in the procedure, especially during the obturation phase. It is important that the patient receive the practitioner’s undivided attention during the root canal treatment, and that interruptions be minimized. This further supports the thesis that the procedure should be performed not only effectively, but also efficiently.
Anesthetic Type
Despite what many think, most anesthetics with moderate duration are equally effective in producing profound pulpal anesthesia for root canal therapy.1 The key to success is a clear understanding of the anatomical, local, and psychological factors associated with each individual patient versus the type of anesthetic used. While combining an anesthetic with lower pKa (e.g., Mepivacaine 3%) with a traditional Lidocaine 2% with 1:100,000 Epinephrine, or even Articaine 4% with 1:100,000 Epinephrine, offers some added value, the anesthetic will only work if it is deposited in close proximity to the nerve bundle or close to the apex of the tooth planned for anesthesia.
Anesthetic Volume
Local anesthesia works by blocking the neuron’s sodium channels and preventing sodium inflow and the transmission of the action potential down the root axis.7 New research on sodium pump characteristics has revealed the presence of 2 subgroups (e.g., SNS and SNS2) that are more resistant to local anesthesia.17 A larger dose of anesthetic is necessary to overcome this resistance and allow effective blockage of the pain signal.
According to American Dental Association surveys, about 80% of root canals are performed by general dentists and about only 20% by endodontists. General dentists should realize that a higher volume of anesthetic is necessary to reach and maintain pulpal anesthesia for the duration of time it takes to perform root canal therapy. Often, root canal treatment is begun when removal of a large carious lesion results in pulp exposure and pain. In those situations, adequate anesthesia was delivered for a filling, not for a root canal. Questionable cases should be anesthetized effectively for root canal therapy, not fillings, so that treatment can be initiated and completed painlessly should subsequent treatment needs arise.
For mandibular molars, at least 2 cartridges of anesthetic should be delivered for a mandibular block, and an additional cartridge of anesthetic is also recommended for local infiltration. For maxillary molars, a minimum of 2 cartridges are also necessary: 1 cartridge for a PSA block and another for local buccal and lingual infiltration. For maxillary anteriors and most premolars, often a single cartridge is adequate if the procedure can be completed within 1 hour.
Conclusion
This article reviewed some of the causes of local anesthesia failure during root canal therapy and proposed some remedies. Although local anesthesia does fail occasionally, initiating or performing a root canal without complete anesthesia is not only unacceptable, it is morally unconscionable. It is the author’s belief that painless root canal therapy can be performed in all cases if particular attention is paid to the local anatomical, physiological, and psychological needs of each individual patient. Performing pulp testing after administration of anesthetics and prior to starting a procedure is necessary to confirm the depth of pulpal anesthesia. Furthermore, administering an adequate dose of anesthetic is important for performing the procedure painlessly for the entire duration. Making painless treatment a priority in the clinical practice, learning about the factors that cause anesthetic failure, and managing those instances effectively will enable all practitioners of good conscience to perform virtually painless root canal therapy at all times and in all patients.
References
1. Malamed S. Handbook of Local Anesthesia. 4th ed. St Louis: Mosby; 1994.
2. Cohen HP, Cha BY, Spangberg LS. Endodontic anesthesia in mandibular molars: a clinical study. J Endod. 1993;19(7):370-3.
3. Wilson S, Johns P, Fuller PM. The inferior alveolar and mylohyoid nerves: an anatomic study and relationship to local anesthesia of the anterior mandibular teeth. J Am Dent Assoc. 1984;108(3):350-2.
4. Walton R, Torabinejad M. Managing local anesthesia problems in the endodontic patient. J Am Dent Assoc. 1992;123(5):97-102.
5. Jastak JT, Yagiela JA, Donaldson D. Local Anesthesia of the Oral Cavity. Philadelphia: Saunders; 1995.
6. Fiset L, Getz T, Milgrom P, et al. Local anesthetic failure: diagnosis and management strategies. Gen Dent. 1989;37(5):414-7.
7. Hargreaves KM, Keiser K. Local anesthetic failure in endodontics: mechanisms & management. Endo Topics. 2002;1(1):26-31.
8. Kaufman E, Weinstein P, Milgrom P. Difficulties in achieving local anesthesia. J Am Denta Assoc. 1984;108(2):205-8.
9. Vandermeulen E. Pain perception, mechanisms of action of local anesthetics and possible causes of failure. Rev Belge Medicine Dent. 2000;55(1):29-40.
10. Vinckier F. What is the cause of failure of local anesthesia? Rev Belge Mede Dent. 2000;55(1): 41-50.
11. Fink B, Cairns A. Differential slowing and block of conduction by lidocaine in individual afferent myelinated and unmyelinated axons. Anesthesiology. 1984;60(2): 111-20.
12. Jin GC, Kim KD, Roh BD, et al. Buccal bone plate thickness of the Asian people. J Endod. 2005;31(6):430-4.
13. Friedman MJ, Hochman MN. P-ASA block injection: a new palatal technique to anesthetize maxillary anterior teeth. J Esthet Dent. 1999;11(2):63-71.
14. Friedman MJ, Hochman MN. The AMSA injection: a new concept for local anesthesia of maxillary teeth using a computer-controlled injection system. Quintessence Int. 1998;29(5):297-303.
15. Akinosi JO. A new approach to the mandibular nerve block. Br J Oral Surg. 1977;15(1):83-7.
16. Gow-Gates GA. Mandibular conduction anesthesia: a new technique using extraoral landmarks. Oral Surg Oral Med Oral Pathol. 1973; 36(3):321-8.
17. Roy ML, Narahashi T. Differential properties of tetrodotoxin-sensitive and tetrodotoxin-resistant sodium channels in rat dorsal root ganglion neurons. J Neurosci. 1992;12(6):2104-11.
About the Authors
Ali Allen Nasseh, DDS, MMSC, PC
Clinical Instructor
Harvard School of Dental Medicine
Assistant Professor
Tufts University School of Dental Medicine
Private Practice
Boston, MA
Email: endoman@mail.msendo.com