Part 1: The Road to Implant Abutments
The need for excellent biocompatibility and customizable shape and angulation
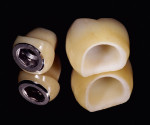
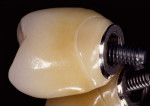
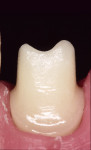
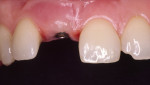
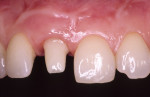
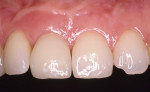
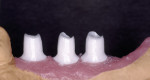
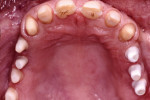
Implant abutments constitute the critical interface between osseointegrated implants and their prosthetic superstructure. They embody the sensitive transition from the implant through the peri-implant soft tissue to the oral cavity and the prosthetic restoration. Implant abutments therefore need to meet specific requirements, including high stability, long-term strength, and resistance to chemical action. They need to offer excellent biocompatibility and the ability to customize their shape and angulation. The exact nature of these requirements will depend on the implant site along the arch. Customized emergence profiles and shades and translucencies resembling those of natural teeth are considered essential to the reconstruction of satisfactory (notably anterior) aesthetics in the presence of A1 or A2 periodontal morphotypes.1,2 In addition, tooth-colored materials in the esthetic zone will also be beneficial in the event of adverse structural conditions giving rise to abutment exposure. Initial attempts to solve these exposure-related problems were sporadically made by layering sintered ceramics over titanium abutments, laying the foundation for subsequent delivery of all-ceramic restorations (Figure 1 and Figure 2). In 1993, Prestipino and Ingber presented a densely sintered abutment made of alumina, to be used as an all-ceramic alternative to metal-based abutments in the anterior segment.3 After taking a direct impression at implant level, cylinders of highly pure and densely sintered alumina ceramic cylinders were prepared, usually for restoration with all-ceramic crowns. Some of the laboratory procedures were very time-consuming. At the same time, the minimum thickness of the material could not be adequately controlled. Veneering ceramics fused to the surface were used for additive customization to establish an adequate emergence profile (Figure 3). An unprecedented level of esthetics and light transmission was achieved by combining these abutments with glass-ceramic crowns (Figure 4 through Figure 7).
Soon after the introduction of alumina abutments, the first experimental abutments made from partially stabilized zirconia became available. Like their alumina predecessors, these zirconia abutments would involve a time-consuming manual process of customization from the prefabricated cylinders in the dental laboratory (Figure 8 and Figure 9). The new zirconia abutments featured both a radiopacity similar to metals and a reduced hardness compared to the alumina variant.4 An investigation performed in vitro demonstrated that these zirconia abutments had a fracture strength approximately 2.5 times higher than that of their alumina counterparts.4
The highest fracture strength of metal-ceramic and all-ceramic crowns is, however, still observed on titanium abutments.5,6 Long-term clinical investigations confirmed that the stability of zirconia abutments was higher than that of alumina abutments.7 Similar findings were obtained among our own patients (Figure 10 through Figure 13). The literature reveals a beneficial effect on peri-implant soft-tissue conditions, as less bacterial adhesion was demonstrated on zirconia healing caps than on titanium ones.8 The development of CAD/CAM technology in recent years has opened up many new options for customizing implant abutments.9,10 Most attention has been devoted to titanium and zirconia.11 Implant abutments have also benefited from the numerous improvements brought about by advanced manufacturing techniques. This progress has led to standardized fabrication routines, industrial-grade prefabrication of high-quality restorative materials and automated control of minimum layer thickness. Compared to manual fabrication, the processing routines have become more conservative and faster. Not getting lost in a host of new fabrication techniques and design principles has become increasingly difficult for today’s users. The purpose of this review is to supply an overview of current approaches to fabricating custom implant abutments.
Classification of Abutments
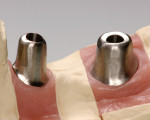
A general classification of implant abutments can be made by fabrication techniques, distinguishing between prefabricated abutments, castable/pressable abutments, and CAD/CAM implant abutments (Table 1). Implant manufacturers offer prefabricated abutments in various sizes, shapes, and angulations. Also, they are available as customizable and non-customizable versions. However, since the limits of customization are quickly reached with prefabricated abutments, users have long desired to modify the shape of abutments as freely as possible. An intermediary solution was provided in the form of HSL sleeves. These were designed so laboratory technicians can wax up an ideal geometry, which is then implemented in a precious metal using the lost-wax technique (Figure 14). Alternatively, pressable ceramics can be used for custom shaping, thus yielding press-on ceramic (POC) abutments. Oversized customizable abutment blanks (e.g., Telescope Abutment, Camlog Biotechnologies, Basel, Switzerland) would be another option (Figure 15). However, the effort that goes into processing these blanks is considerable. In addition, this type of customization involves a risk of inappropriate handling or damage to the material (whether titanium or zirconia) by overheating. Customized zirconia blanks should therefore be processed only under irrigation with copious amounts of water. To allow customization of titanium abutments under irrigation, one manufacturer (Komet, Brasseler, Lemgo, Germany) has developed a specialized set of cutters (original design by J. H. Bellmann) for use in irrigated laboratory turbines (Figure 16). This system greatly improves the performance of material reduction while minimizing heat development. CAD/CAM abutments are predominantly fabricated from titanium and zirconia.12 While titanium abutments are processed as monoblocks, all-ceramic abutments may be used either with or without a bonding base.
1. Abutments Implemented by CAD/CAM from Titanium Monoblocks
Figure 17 and Figure 18 illustrate this concept. Abutments implemented by CAD/CAM from titanium are offered by various manufacturers. For the time being, the computer-assisted manufacturing of these abutments can only be performed in dedicated milling centers (e.g., Straumann CAD/CAM, Leipzig, Germany; Nobel Procera, Göteborg, Sweden; Compartis ISUS, Hanau, Germany; Astra Atlantis, Möln - dal, Sweden). Manufacturers either use industrially prefabricated blanks of a semi-finished nature (i.e., with the implant-abutment interface already prefabricated to industrial standards) or finished abutments milled from a titanium block (i.e., with both the external shape and the interface already completed) for CAD/CAM implementation. Ready-made CAD/CAM abutments offer the advantage of not requiring any subsequent processing other than surface polishing with silicone rubber cups if required. This eliminates the need for expensive corrections and avoids the risk of damaging the material in the process.
2. Abutments Implemented by CAD/CAM from Zirconia
Zirconia CAD/CAM abutments may be fabricated with or without a titanium bonding base. Both variants have their specific advantages and disadvantages.
3a. Ceramic Abutments Without a Bonding Base
Like titanium abutments, those ceramic abutments that do not use a bonding base are also implemented from monoblocks by CAD/CAM (Figure 19).13 They are also supplied as semi-finished blanks with the abutment-implant interface already prefabricated in an industrial process. The external abutment geometry is custom-milled from the blank, utilizing the design data or the wax-up that the laboratory has generated for this purpose. CAD/CAM ceramic abutments without a bonding base have both advantages and disadvantages. A brief summary of these follows.
Advantages:
With no subsequent adjustments performed to the abutments, there is no risk of inflicting damage to the material.
White (i.e., tooth-colored) abutments will offer esthetic advantages for anterior implant restorations.
Perfect biocompatibility in the sensitive transition zone from implant to abutment.
Disadvantages:
No conical anchorage of the abutment screws, as these screws have direct contact with the ceramic material, thus being usually anchored in a perpendicular channel with parallel walls to avoid tensile stresses inside the ceramic abutment. These connections therefore carry a higher risk of screw loosening than the ones used in titanium abutments.
Ceramic abutments will generally involve a higher risk of facture than titanium abutments.
3b. Ceramic Abutments with a Bonding Base
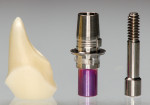
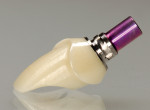
All-ceramic CAD/CAM implant abutments with a bonding base are fabricated from presintered zirconia either in a dental laboratory (e.g., inLab MCXL, Sirona, Bensheim, Germany; Everest, KaVo, Biberach, Germany) or in a milling center (e.g., Bego Medical, Bremen, Germany; 3M ESPE Lava, Seefeld, Germany) (Figure 20 and Figure 21).12,14 One approach is to use partially prefabricated “mesioblocks” of zirconia, designed as semi-finished blanks with the connection from abutment to bonding base already incorporated. Once the external geometry has been ground to shape, the abutments are densely sintered and connected to the bonding base. The bonding bases as such are industrially manufactured from titanium, hence offering the same fit as prefabricated titanium abutments. Again, a number of advantages and disadvantages should be considered.
Advantages:
Conical anchorage of the abutment screw inside the titanium bonding base, which reduces the risk of screw loosening.
Tightening the connection screws will not introduce any tensile stresses into the ceramic abutment.
Can be fabricated outside of milling centers (i.e., in laboratories and dental offices).
Low cost.
Disadvantages:
Additional effort of bonding the ceramic abutment to the titanium base.
Risk of debonding if inappropriately executed.
Reduced quality management by lack of industrial manufacturing.
Increased affinity to plaque formation (due to the bonding gap filled with composite) in the sensitive transition zone from implant to abutment.
4. Abutments Implemented by CAD/CAM from CoCr Alloy and Precious Metal on a Titanium Bonding Base
Bego additionally offers a CoCr alloy (Wirobond C+, Bego) as metal material for CAD/CAM bonding abutments. All CAD/Cast materials are also offered by this manufacturer. In the CAD/Cast process, resin restorations are fabricated in the milling center based on the CAD designs generated by the laboratory technician. These resin restorations are then cast using the lost-wax technique in an industrial process of vacuum pressure casting. Eight different precious alloys and one non-precious alloy (Wiron 99, Bego) are currently available for this purpose.
Editor’s Note
In “Part II: The Road to Implant Abutments,” the authors will discuss three strategies for producing patient-specific implant abutments using CAD/CAM technology. Both parts of this article were originally published in 2011 in EDI Journal as “Roads to Implant Abutments.”
Disclaimer
The techniques and uses described in this article do not necessarily comply with US federal rules, approved uses, and regulations regarding these products.
References
1. Jung RE, Sailer I, Hammerle CH, Attin T, Schmidlin P. In vitro color changes of soft tissues caused by restorative materials. Int J Periodontics Restorative Dent. 2007;27(3):251-257.
2. Muller HP, Eger T. Masticatory mucosa and periodontal phenotype: a review. Int J Periodontics Restorative Dent. 2002;22(2):172-183.
3. Prestipino V, Ingber A. Esthetic high-strength implant abutments. Part II. J Esthet Dent. 1993;5(2):63-68.
4. Yildirim M, Fischer H, Marx R, Edelhoff D. In vivo fracture resistance of implant-supported all-ceramic restorations. J Prosthet Dent. 2003;90(4):325-331.
5. Att W, Kurun S, Gerds T, Strub JR. Fracture resistance of single-tooth implant-supported all-ceramic restorations after exposure to the artificial mouth. J Oral Rehabil. 2006;33(5):380-386.
6. Glauser R, Sailer I, Wohlwend A, et al. Experimental zirconia abutments for implant-supported single-tooth restorations in esthetically demanding regions: 4-year results of a prospective clinical study. Int J Prosthodont. 2004;17(3):285-90.
7. Andersson B, Glauser R, Maglione M, Taylor A. Ceramic implant abutments for short-span FPDs: a prospective 5-year multicenter study. Int J Prosthodont. 2003;16(6):640-646.
8. Degidi M, Artese L, Scarano A, et al. Inflammatory infiltrate, microvessel density, nitric oxide synthase expression, vascular endothelial growth factor expression, and proliferative activity in peri-implant soft tissues around titanium and zirconium oxide healing caps. J Periodontol. 2006;77(1):73-80.
9. Blatz MB, Bergler M, Holst S, Block MS. Zirconia abutments for single-tooth implants – rationale and clinical guidelines. J Oral Maxillofac Surg. 2009;67(11 Suppl):74-81.
10. Beuer F, Schweiger J, Edelhoff D. Digital dentistry: an overview of recent developments for CAD/CAM generated restorations. Br Dent J. 2008;204(9):505-511.
11. Koutayas SO, Vagkopoulou T, Pelekanos S, et al. Zirconia in dentistry: part 2. Evidence-based clinical breakthrough. Eur J Esthet Dent. 2009;4(4):348-380.
12. Kurbad A. CAD/CAM-gestützte Suprakonstruktionen bei Implantaten in der ästhetischen Zone. Digital Dental News. 2008;2:40-45.
13. Dubs RA. Ästhetische Versorung eines Straumann RC Bone Level Implantats mit einem CAD/CAM-Sekundärteil aus Keramik. Straumann Starget. 2009;28-30.
14. Blanckenburg H, Wüstefeld F. Customised CAD/CAM abutments and crowns made of zirconium dioxide. Digital Dental News. 2007;1:36-43.