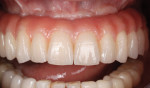
Meeting Patient Demands Head-On
Providing function and esthetics with implant-supported hybrid prostheses
The evolving expectations of today’s edentulous patient pose new challenges for the clinician and technician managing each case. The implant-supported hybrid prosthesis has become the restoration of choice for a wide variety of edentulous patients, and they now have more access than ever before to information about this solution. The dental team’s challenge is to provide the best function and esthetics for each patient.
Materials selection is a very important factor to consider in each case. Historically, patients opting for implant hybrid prostheses have had to choose between acrylic and denture teeth or a metal-based ceramic solution. Today, with advances in the science of highly filled composites and a new efficient injection fabrication technique, a new material option is available—composite veneered on a metal or zirconia frame. This composite-veneering option provides an upgrade in both esthetic customizability and wear resistance when compared to traditional denture teeth and acrylic. Due to the precision and predictability of a new injection fabrication technique, fabrication and management of such cases becomes simple and profitable for the laboratory. Plus, basic maintenance is performed by the dentist chairside.
In this article, we will examine a case from start to finish using the anaxFORM system (anaxdent, www.anaxdentusa.com) to transform one wax-up into the provisional, prototype restoration, and then the final composite-on-zirconia restoration.
The Case
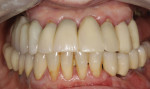
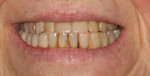
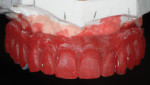
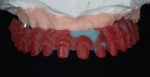
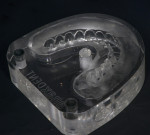
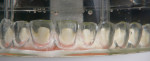
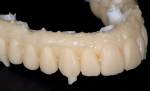
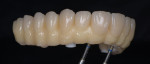
The 51-year-old female patient had a history of previous maxillofacial surgery, including placement of dental implants. The patient arrived at the dental practice with a box of models from previous phases of treatment. She was dissatisfied with her current maxillary restoration, a PFM bridge, as she reported a feeling of tension in her maxilla (Figure 1 and Figure 2). She also desired a metal-free restoration. These factors led the dentist and technician to suggest a bridge with zirconia framework in two sections and veneered with composite. The plan would be to fuse the two frame sections together with the composite, while retaining the option to adapt the restoration into two segments if the feeling of tension remained an issue.
Materials Selection
Use of composites to veneer the segmented zirconia framework effectively allowed the team to manage the patient’s fear of tension discomfort, without setting the case up for a difficult rework in the laboratory if the decision was made later to segment the bridge. The patient’s dental history suggested issues with proprioception, so a softer material that was also simple to repair was optimal for restoring the case.
Injecting a duplicate of the final wax-up directly onto the zirconia framework would be precise, predictable, and efficient. The technique for doing so involved use of anaxblend Flowable composite (anaxdent) and the anaxFORM Clear flasking system (anaxdent).
A hardness of 365 MPa and a flexural strength of 140 MPa made the highly filled composite a viable material choice. Also, due to the high esthetic demands of the patient, the wide range of shades in opaquers, dentins, enamels, and mass effects made the system attractive to the technician.
Wax-Up
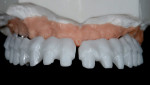
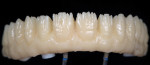
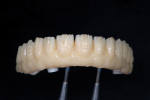
The full-contour wax-up (Figure 3) was transformed into a simple diagnostic provisional restoration that the patient wore for one year. During this time, the dentist worked with the patient and a physical therapist to ensure proper function. After this trial period, some minor adjustments were made to the wax-up, and a diagnostic provisional, or “prototype,” restoration was fabricated using New Outline PMMA and anaxgum pink composite (anaxdent) to test the functional and esthetic plan for the final restoration (Figure 4). After the patient happily wore the prototype bridge for a number of months, the dentist and technician could confidently move forward fabricating the final composite bridge.
Frame Design
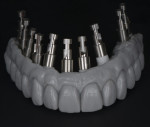
The technician designed the framework by capturing the final form and the vertical dimension of the wax-up in a device called the Verticulator (anaxdent). The technician then duplicated the wax-up in pattern resin (Figure 5) and cut the resin back to shape the frame (Figure 6), using the Verticulator to reference final form and vertical dimension throughout the cutback process.
Fabricating the Restoration
The technician filled the base of the anaxFORM Clear Flask with Matrix Form 60 silicone putty (anaxdent) then embedded the wax-up with analogs attached into the putty. The length of the analogs was trimmed due to space constraints. A clear flask was also available that accommodated a stone model, if working with models is preferred.
Next, wax rods were attached to the most distal molars and to the canine area, creating four sprue channels for the later injection process. A coat of Divorce silicone separator (anaxdent) was applied and the flask was closed (Figure 7). The technician then tightened the fixation screw to secure the lid in place. For the next step, the technician mixed Matrix Cast Clear silicone duplication material (anaxdent) in a vacuum mixer and slowly poured the silicone into the opening in the flask lid, filling the flask completely (Figure 8). From there, the flask was placed into a dry pressure pot at 2 bar (approximately 30 psi) for 30 minutes. Allowing the material to set in this pressurized environment captured all of the details in the wax-up and rid the matrix of air bubbles (Figure 9).
Once removed from the flask, the wax was removed from the frame and the technician prepared the zirconia frame for bonding with composite material. Creation Make Up stains (Jensen Dental, www.jensendental.com) were applied to characterize the framework (Figure 10), then a very thin layer of Creation HT-51 (Jensen Dental) was applied to provide a porcelain surface better suited for bonding to composite. Next, the ceramic layer was etched and silanated, and a thin layer of Bond LC (anaxdent) bonding fluid was applied to the frame and light-cured for one minute. If a metal frame is chosen for this technique, a metal primer is applied to the blasted/etched frame, and is then followed by the application and light-cure of a composite opaquer.
The frame was then mounted into the clear flask, and the lid—including the clear matrix of the wax-up—was reattached to the flask base with the tension screw, fixing the lid in place (Figure 12). The technician then used the 20 g Big Block syringe of anaxblend flowable composite (anaxdent) in dentin shade A3 to inject a duplicate of the wax-up into the flask, and placed the flask in a light curing unit for the recommended time, which varies based on type of curing unit. Prior to injecting, it is wise to heat the composite to approximately 55° C. The highly filled flowable composite is more viscous than traditional flows, and increasing the material’s temperature lowers the viscosity, enhancing the flow of the material even in narrower channels. A heater for the system is available, but placing the syringe in a hot area, such as near a ceramic furnace, for about 15 minutes prior to use can be sufficient.
It is also very important to use slow, constant pressure during the injection process in order to prevent voids. This is easily accomplished through the use of the anaxdent Universal Dispensing Gun. The Gun’s precision leaves little need for adjustment right out of the flask (Figure 13), and use of the larger 20 g syringe of composite is important in order to avoid introduction of air bubbles in larger restorations.
Next, the teeth of the dentin duplicate were cut back (Figure 14) and a thin layer of Bond LC was applied. The mass effects were built up using anaxblend Flow in CL-0 and anaxblend Colors White and Orange (Figure 15), then light cured completely.
The restoration was then placed back into the flask, and the lid with the clear matrix was fixed in place. The enamel layer was injected slowly and with constant pressure into the flask using anaxblend Flow in S59 shade. Again, heating the syringe prior to injection simplifies this process. If flow throughout the arch is interrupted at any point, the syringe can be removed and replaced into one of the other sprue channels to provide better access. The flask was then placed back into the curing unit, and once fully cured, the restoration was removed from the flask (Figure 16). The technician trimmed the resulting flash, and the gingival area was cut back to make room for pink composite layering (Figure 17).
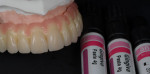
Since color variation is so vital to creating a natural reproduction of gingiva, direct layering of different pink composite paste shades was preferable to injection of pink composites. For this case, the technician used anaxdent’s anaxgum pink composite pastes, starting with a layer of Dark Pink to cover the darker interproximal areas and the mucogingival junction (Figure 18). Then, Orange Pink and Light Pink were applied to the roots (Figure 19) to reproduce the lighter, marginal gingiva. Additional characterization was accomplished by applying a bright red glaze, which was made by scraping red pigment from articulating strips and mixing the pigment with Skin Glaze light cure glaze (anaxdent) (Figure 20).
Finishing
Creating an ideal surface is essential in ensuring adequate durability of a composite restoration. To ensure full curing of the outermost layer, the technician applied Cover Gel (anaxdent) air inhibiting gel to the entire surface and cured the restoration one final cycle. This step removed most, if not all, of the smear layer. Any remaining residue can be removed with acetone. Then, a series of burs and disks (Figure 21) was used to create surface texture, and the entire composite surface was sealed with OPTIGLAZE™ Light Cure Glaze (GC America, www.gcamerica.com).
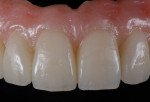
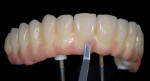
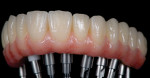
Images of the final, prosthesis outside the mouth (Figure 22) and intraorally (Figure 23 and Figure 24) revealed the natural esthetics of the composite material.
Maintenance Plan
Wear of the outer surface of the composite is expected over time, and as such the clinician planned annual recall appointments to maintain the surface of the composite and to make minor repairs chairside. The clinician also retained the prototype restoration, so if major repairs or changes were necessary in the future, the prosthesis could be removed and sent to the laboratory and the patient could wear the prototype in the interim.
When major laboratory repairs or changes are necessary, they can be managed easily, and, unlike ceramic restorations, augmentations with composite can be accomplished without any worry of compromising the integrity of the prosthesis. In this case, the technician retained the full contour putty matrix of the final wax-up formed in the Verticulator, so final form and vertical dimension could be duplicated and/or referenced if necessary.
Conclusion
As with any type of restoration, the more options dentists, patients, and technicians have, the better. Recent advances in composite materials, with their higher ceramic filler content and resulting increase in durability, make them a viable candidate for a veneering material in implant cases. Though building up entire arches of composite pastes is too time-consuming to consider as an option in most cases, the efficiency and predictability of this injection technique makes full-arch composite restorations an attractive option for the technician to offer as an alternative to ceramic.
Composite-on-zirconia and composite-on-metal hybrids have benefits that can make them the perfect fit for patients who have higher esthetic or functional demands than acrylic and denture teeth can provide. Though the surface of composite may require more frequent maintenance than ceramic or zirconia, basic maintenance is accomplished quickly and simply chairside.
Even with ceramic cases, over time, repair in the laboratory is required. With composite, this process is much simpler and less stressful when compared to ceramic. It can be completed without a series of appointments and at dramatically less cost to the patient and less stress on the restoration.
To learn more about this case, visit the link below for a video from Sébastien Mosconi. dentalaegis.com/go/idt405
About the author
Sébastien Mosconi
Owner
Oral Design French Riviera
Nice, France