Dental Laboratory Communication in the Esthetic Age
Predictably satisfying clients and patients
At a time when patients’ knowledge and expectations of dentistry’s restorative capabilities can seem unrealistic, the relationship between the restorative dentist and dental laboratory is ever more critical. Everyone must work together to determine what is required to predictably satisfy even the most demanding patients. It has been the author’s experience over the past 15 years that there are four important keys to delivering the highest quality restorative dentistry: shared philosophy, shared knowledge, shared information, and communication tools.
Shared Philosophy
Dr. Ronald Goldstein wrote: “… taking steps to improve your appearance today is considered an investment in your health and well being, and it is as socially acceptable as it is personally gratifying.”1 This quote from one of the pioneers of esthetic dentistry expresses how the author thinks the restorative team provides value to our patients in today’s society. As a laboratory owner with an ongoing commitment to pursuing excellence in restorative dentistry, the author believes that our most successful long-term relationships have been with like-minded dentists.
Shared Knowledge
As a clinical instructor at the Kois Center and faculty member at The Pankey Institute, the author has had the opportunity to meet, learn alongside, and work with talented restorative dentists from all over the world. These are dentists with whom the author’s laboratory shares a passion for comprehensive patient care and long-term dental health strategies. Success for each case is developed and communicated in a systematic treatment plan that minimizes risk and is based on the best currently available scientific evidence.
With the dental laboratory and restorative dentist sharing foundation knowledge and a comprehensive system for treating patients, they are able to identify potential problems for creating complete esthetic and functional harmony in a thorough diagnosis. Potential problems may be addressed with a referral to other clinical specialties, such as orthodontists and periodontists, before the teeth are prepared. When a patient refuses to act on the team’s recommendations, and they are clearly informed of the consequences and compromises to the final outcome, and the risks for not meeting their esthetic expectations are shared.
Incredible benefits and opportunities exist today for a restorative team to share a similar knowledge base by attending clinical continuing education programs. Experiences with local clinical study groups and organizations such as the Seattle Study Club have helped the author’s laboratory deliver outstanding results with greater predictability. As restorative material choices and treatment protocols are determined, their impact on remaining tooth structure, the esthetic demands of the patient, and relevant scientific evidence are evaluated to deliver long–term predictability.
Shared Information
Esthetic treatment decisions are implemented by communicating vital information to improve restorative success. In order for the laboratory to express the patient’s vision for his or her smile in restorations, information vital to understanding the patient must be communicated. The information the author’s laboratory considers essential for treating any anterior dentition, or an esthetically aware patient includes:
The Patient’s Vision for Treatment
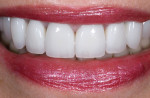
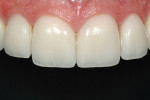
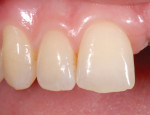
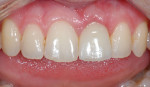
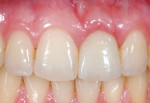
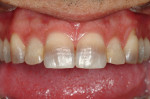
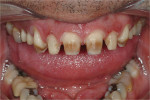
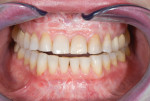
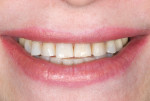
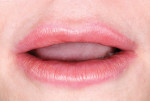
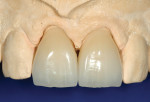
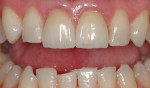
Although communicated by the patient to the dentist and clinical team, this needs to be shared with the laboratory. As patients do not always have the knowledge or insight to envision their completed restorations, using language more familiar to them helps considerably. The laboratory should ask patients how they want their teeth to look, either similar to bleached teeth (Figure 1), healthy natural looking teeth (Figure 2), or age appropriate teeth. Using a library of images for examples of each will help the patient visualize the final outcome. The laboratory’s job is then to translate the appropriate look into restorations the patient will love.
Study Cast of Provisional Restorations
When the patient is comfortable and happy with the provisional restorations, the information can be transferred to the laboratory with a study cast. The key information this cast relates to the laboratory is the incisal edge position (length and facial position), the position and cant of the midline, and basic tooth proportions and form. These esthetic and functional parameters are transferred to the articulator using a face-bow record and cross-mounting the study cast with the working models.
Color Communication
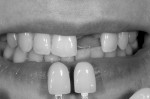
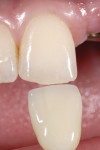
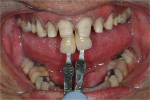
Vital elements to recreating tooth color are shade and value. Using black and white photography (Figure 3 through Figure 7) to demonstrate value is essential, particularly in single anterior restorations. Photographs of prepared teeth are helpful for veneer cases as the final color of the restorations will be influenced by the stump shade (Figure 8 through Figure 10). In order to accommodate patients’ bleaching, the author’s recommendation is to address bleaching earlier in the treatment plan. By the time the case is prepared for restorations the patient should be happy with the color of the adjacent and remaining natural teeth. In the author’s laboratory, patients are scheduled for a color match of anterior teeth a minimum of two weeks after they have finished bleaching. The color change during bleaching is not predictable and the laboratory can only match a color as the patient presents at the shade appointment.
Communication Tools
Many laboratories have clients from all over the globe, and as such, technicians do not often get to see patients in the laboratory before creating the restorations. In order for technicians to satisfy demanding patients and clients with high expectations, they need patient information relayed in a practical way. The following tools have proved invaluable to the author’s laboratory for delivering excellent quality esthetic dentistry:
Face-Bow
There have been few tools introduced into practice that have made as much of an impact for the author’s laboratory as the Kois Dento-Facial Analyzer (Panadent, www.panadent.com). This face-bow system situates the upper study cast in the articulator in the same relationship as the teeth to the face (Figure 11 through Figure 18), using esthetic planes and functional averages. This enables the technicians working on the case to have the appropriate esthetic information to establish the teeth level in the face and recreate the ideal tooth position as it has been established in the wax up, and then in the provisional.
Photography
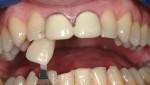
In many cases, having a correctly-exposed photograph to work from is as close as the laboratory can come to having the patient present. Laboratories should request that a shade tab is present in most of the photographs and never try to interpret a shade from a picture (Figure 19 through Figure 21). These photographs should aid the laboratory in developing natural characteristics, evaluating value, and finalizing surface texture in the restorations.
Recommended Cameras
A digital SLR camera with a dedicated macro lens and flash system is an excellent option for taking patient photographs. The author recommends using a 105-mm macro lens and a side mounted flash system. Flash systems that are lens mounted, such as a ring flash, create more flash highlights on the tooth surfaces and less depth perception in the incisal third of the teeth.
Laboratory Prescription
The prescription should always ask the right questions and the laboratory technicians are responsible for understanding and translating the information to the final restorations. Many of the cases seen in laboratories today are being treated one segment at a time, so all the information on the overall treatment plan is critical to keeping all the pieces fitting together to deliver a complete look.
Changing peoples’ lives by creating beautiful smiles is a team process. For the most demanding patients to be satisfied predictably, all the members of the restorative team have to communicate and function together seamlessly. With a shared philosophy, shared knowledge, shared information, and using better tools to communicate, it is possible to deliver esthetic restorations to best satisfy the patient and successfully market the laboratory’s services.
References
1. Goldstein R, Belinfante L, Nahai F . Change Your Smile. 3rd ed. Chicago, IL: Quintessence Publishing Co.; 1997.
About the author
Leon Hermanides, CDT
President
Protea Dental Studio
Redmond, Washington