Optimizing Technology to Maximize Success
Replacing anterior maxillary teeth present clinicians and technicians
a new challenge in restoration treatment planning and fabrication.
By Robert E. Stover, DDS, MS; and Jamie Stover, CDT
If asked what the most difficult clinical challenge is in dentistry, high on the list for most dentists would be a full-mouth rehabilitation, a fixed-detachable (“hybrid”) prosthesis, or perhaps implant-bar retained overdentures. However, by far the most common answer is replacement of several anterior teeth. This can be a monumental challenge that requires balancing the patient’s perception of esthetics with proper clinical protocol for smile lines, gingival contours, orthodontic malalignment and the demands of careful soft-tissue management, complicated often by preexisting loss of supportive bone. Careful tooth preparation (which may need to be carried out on heavily restored or previously crowned existing teeth), careful occlusion management, and material choice make replacing anterior teeth one of the most difficult challenges dentists and technicians face. For the dental team, rapid innovations in dental laboratory technology and materials add a new challenging dimension to material selection and fabrication methods.
Case Presentation
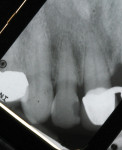
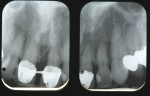
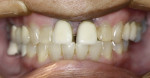
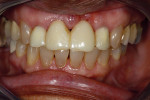
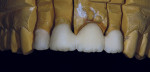
A 67-year-old woman presented with a failed crown on tooth No. 9, secondary to a large periodontal defect on the mesial aspect (Figure 1 and Figure 2). Tooth No. 9 exhibited Class III mobility, and through the years had a history of multiple restorations, crown placement, and, eventually, splinted porcelain-fused-to-metal (PFM) crowns. Mirroring the bone loss, there was extensive gingival recession at the mesial and facial aspects, exposing the root surface. Tooth No. 10 had been restored with a mesiofacial-lingual composite with an overhang and exhibited mesio-lingual recurrent decay. The patient’s esthetic objectives required closing a large diastema that had always bothered her and establishing proper tooth shape and desired color (Figure 3). Clinically, the splinted crowns displayed poor marginal adaptation, and the patient also desired to correct the position and color of the adjacent teeth.
A treatment plan was formulated that called for extracting tooth No. 9 atraumatically, grafting the extraction site for socket preservation and pontic site development, and fabricating an immediate provisional using an ovate pontic design to support the soft tissue during healing. In order to distribute space evenly across the incisors, an all-ceramic crown was treatment planned for tooth No. 7. After sufficient soft-tissue healing and satisfactory bleaching of her natural teeth, the patient would present to the laboratory for a custom shade match.
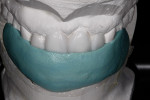
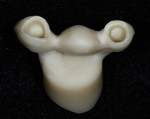
Because the patient was not in any pain, there was an opportunity to make a careful diagnosis before proceeding. Diagnostic impressions were made and the casts mounted using a facebow that had been corrected to the patient’s horizontal esthetic plane to allow analysis of occlusion. The facebow would be preserved throughout the case by using careful interocclusal records of each step and then cross-mounting. A diagnostic wax-up was completed (Figure 4) to incorporate the patient’s esthetic concerns about her existing smile as well as clinical parameters, including the smile line and incisal display in repose. Bleaching trays were fabricated from the impressions to begin the lightening process of the surrounding and opposing natural dentition. The patient was encouraged to review the wax-up and provide feedback on tooth form, shape, and position. These modifications were incorporated and the provisional matrix and reduction guides were fabricated (Figure 5). The provisional matrix was created using bite-registration material (Blu-Mousse®, Parkell, www.parkell.com) in a rigid tray. Only the occlusal surfaces of the maxillary posterior teeth and the full contours of the anterior teeth were indexed. This allowed accurate intraoral reproduction of the diagnostic waxing contours in the provisionals. Reduction guides were created from vinyl polysiloxane putty to index the adjacent teeth and project the contours of the wax-up against the tooth preparations to ensure adequate reduction for metal copings and porcelain (Figure 6).
On the day of surgery, the crown on tooth No. 8 was removed, teeth Nos. 8 and 10 were checked for decay, and the restorations were refined for parallelism. Additional buildup material was bonded and placed (LuxaCore Dual, DMG America, www.dmg-america.com). The crown on tooth No. 9 was removed and the tooth was sectioned in a buccal-palatal direction. The direction of sectioning was important because the residual buccal plate of bone is typically very thin and luxation should minimize buccal forces, thus avoiding fracture of any remaining bone. The root fragments were then “in-fractured” into the slot created by sectioning, and the pieces were removed. After thorough irrigation with sterile saline, cancellous particulate allograft of 250-nm to 1,000 nm (Puros, Zimmer Dental, www.zimmerdental.com) was mixed with patient blood and condensed into the residual tooth socket. The facial aspect of the gingiva was atraumatically dissected away from the buccal plate below the periosteum and a collagen membrane was contoured and placed below the flap (Figure 7). Excess particulate graft was placed below the membrane on the facial and the membrane was carefully sutured into place using 5-0 absorbable-coated polyglycolic sutures (Vicryl, Ethicon Inc., www.ethicon360.com).
The provisional was fabricated directly on the prepared teeth (Protemp™ II Bis-Acryl Provisional Material, 3M ESPE, www.3mespe.com), removed, and refined in the laboratory under a microscope to provide highly polished, well-adapted margins and an ovate pontic form. A jaw-relation record (Blu-Mousse) was made over the prepared teeth to cross-mount the solid master cast against the already mounted opposing diagnostic cast. The provisional was then cemented using a provisional cement (TempBond® NE™, Kerr Dental, www.kerrdental.com). The patient was given postoperative medications and returned the following day for an uneventful postoperative check. She was very pleased with the contours of the provisionals and was instructed to make notations about any corrections to form or contour, and appointed 1.5 weeks later for an esthetic analysis.
At that appointment, revisions were made to the provisionals per the patient’s specifications. She was able to return and continue to refine the provisional form until she was entirely pleased with the crown shape and position. This process also facilitated a careful analysis of her occlusion while in the provisional phase of treatment (Figure 8). The site was allowed to heal for approximately 2.5 months. After healing, the patient returned in order to take a bite registration and an alginate impression of the patient-approved provisionals. The cast of the provisional was cross-mounted against the mounted mandibular diagnostic cast and served as a guide for the final crown form. The provisionals were removed and a second impression was taken of the prepared teeth to capture the soft tissue contours in the developed pontic site, and stump shades were recorded (Figure 9). Bleaching of the natural dentition was acceptable to the patient and she was appointed at the laboratory for a custom shade.
Laboratory Procedures
So much technology is at the disposal of laboratories today that it makes it difficult for owners and managers to ascertain which hardware to purchase, which processes to adopt and employ, and how to keep profitable and competitive in today’s challenging business environment. Laboratories need to decide if they are doing the entire process in-house or outsourcing all or a certain parts of the process to another laboratory. With a reasonably minimal investment in a quality open-architecture scanner and design software, laboratories can improve productivity by eliminating steps traditionally done by hand, such as waxing and casting. These manual processes can be automated by converting the analog to a digital CAD design and exporting to a 3D wax printer, milling unit, or laser-sintering device. For this case, these newer methods were used for some steps of the fabrication process to streamline the restorative process and to provide a solid and esthetically correct foundation for layering porcelain.
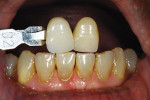
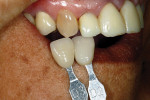
This case provided a couple of challenging aspects for the author. The pontic site was restored with a bone graft, leaving the tissue slightly imperfect. The restorative solutions chosen by the restorative team for the bridge spanning teeth Nos. 8 through 10 were IPS e.max® Zirpress (Ivoclar Vivadent, www.ivoclarvivadent.com) supported by a zirconia understructure and cut back for effect and translucent porcelains. An IPS e.max all-ceramic crown was selected for placement on tooth No. 7 (again with a cut-back). The preoperative impressions were taken and sent to the laboratory where they were poured and articulated. A diagnostic wax-up was fabricated to show not only the esthetic improvements, but also the functionality of the restorations. After teeth Nos. 7, 8, and 10 were prepared and the bone graft was performed to restore the extraction site of tooth No. 9, temporaries were fabricated from the diagnostic wax-up and worn by the patient for approximately 10 weeks, allowing the grafted site to heal. The patient returned for periodic checks during this time to check the function of the temporaries with specific attention paid to wear, and to address any esthetic changes requested by the patient. A final impression was taken reflecting the changes to the grafted area and tissue healing, and the stump shades were recorded. Next, the patient visited the laboratory for custom-shade photographs and shade determination (Figure 10 and Figure 11). The goal was to match the restorations to the surrounding natural dentition as seamlessly as possible, specifically to the incisal of the lower anteriors, while the gingival one third of teeth Nos. 7 and 10 would blend naturally with the cuspids. The shade selected was VITA D3 with more chroma at the gingival. The stump shades of the preparations were ND5 for teeth Nos. 7 and 10, and ND6 for tooth No. 8. The preparations on teeth Nos. 8 and 10 would be covered by the zirconia framework, which was also sintered in the VITA D3 shade. The IPS e.max crown on tooth No. 7 was pressed out of a D3 LT ingot to most accurately match the translucency of the zirconia understructure covering the other preparations.
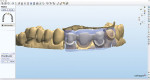
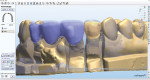
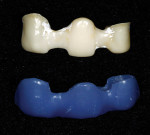
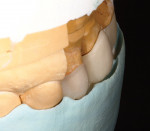
The models were scanned, including a model of the temporaries showing the final desired contour of the restorations. The zirconia framework was CAD designed simultaneously with the wax-ups for the bridge spanning teeth Nos. 8 through 10 and for the single IPS e.max unit for tooth No. 7 (Figure 12, Figure 13, Figure 14). A porcelain overlay was desired to achieve the esthetic goals of the patient. The cutback technique was used in the CAD design of all the wax-ups. Extra space was created on the inside of the bridge wax overlay to leave room for the layer of IPS e.max Zirliner (Ivoclar Vivadent) that would be applied onto the zirconia framework and fired to establish the proper bond when pressing the IPS e.max Zirpress bridge onto the framework. Once the design was completed, the zirconia framework was milled in-house from a Lava™ C.O.S. zirconia (3M ESPE) milling block, sintered, and final finished. While these steps were being completed, the wax overlay for the bridge and the wax-up for the single-unit tooth No. 7 were milled from a Lava Wax Block (Figure 15). Next, the IPS e.max Zirliner was applied in a thin, even layer on the surface of the zirconia framework and fired (Figure 16 and Figure 17). The wax overlay was then placed onto the zirconia framework and adapted to the margins. A matrix was created from the model of the temporaries, the wax-ups were all placed on the model, and the contour checked in the matrix (Figure 18, Figure 19, Figure 20).
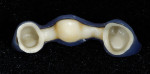
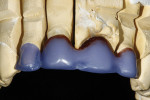
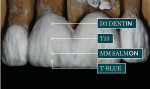
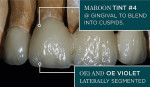
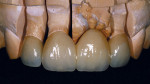
The milled wax bridge framework was invested and pressed using two IPS e.max Zirpress D3 ingots, while the single unit was invested and pressed out of a single small IPS e.max D3 LT ingot. The framework and single unit were all devested and the fit checked and established on the dies (Figure 21). The crowns were then placed on the model, and the final contour was checked in the matrix. Final contouring was completed in preparation for porcelain layering with IPS e.max Ceram (Ivoclar Vivadent) (Figure 22 and Figure 23). The porcelain application was completed for the first buildup with D3 Dentin, Mammalon Salmon, and a Translucent overlay of Ti3 and Transpa blue (Figure 24). The first porcelain application was fired and the second buildup of laterally segmented OE1 and OE Violet was completed and fired (Figure 25). The crowns were final contoured, some external maroon stain was applied at the gingival, and they were glazed and delivered (Figure 26).
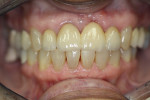
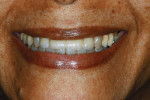
The patient presented for a try-in and was very pleased with the permanent bridge. The final result was a good match to her existing dentition in shade, shape, and translucency (Figure 27, Figure 28, Figure 29). Although a small gingival defect remained, it was expected to continue to resolve. The patient had a low smile line but was unconcerned with the gingival defect and wished to proceed with the final cementation. Final cementation was accomplished using RelyX™ Luting Plus (3M ESPE), a resin-modified glass-ionomer cement.
By tapping into innovative laboratory technologies, the technician was able to achieve a good result using a new, streamlined workflow process.
The authors would like to thank Sheryl Wolden, CDT, of Ziemek Dental Lab, for completing the final fabrication steps on this case, including the porcelain application as well as the custom-shade acquisition and resulting shade match.
About the Authors
Robert E. Stover, DDS, MS, FACP
Private Practice in Prosthodontics
Olympia, Washington
Jamie Stover, CDT
Laboratory Manager
Ziemek Aesthetic Dental Lab, Ziemek Milling Center, and Ziemek IDS
Olympia, Washington