Full-Arch Restorations on CAD/CAM-Milled Titanium Bars
Successful case results using verified two-stage impression and screw-retained LC resin basebar techniques.
By Thomas Wade, CDT
In the exciting, relatively new and rapidly growing arena of screw-retained hybrid and attached overdentures on CAM-milled titanium bars, there are two procedures/techniques that are critical to obtaining consistent predictable and successful results. results.
First are the impressions and model work necessary to achieve the final verified master cast. The master cast will be laser-scanned to produce an accurate CAM-milled titanium bar that will passively seat and interface with all of the implants (or abutments) in the arch. The “weak link” in this process is not the CAD/CAM technology but rather the human element. The onus is squarely on the clinician and laboratory technologist to produce the most accurate, verified master cast scientifically possible. When that is achieved, the quality of the restoration with regard to fit (passivity), strength, weight, esthetics, and function will be unsurpassed, state-of-the-art restorative work.
The second key aspect of the fabrication process is properly constructed screw-retained basebars. These are nothing more than the implant version of the acrylic or light-cured resin baseplates that have been used in the fabrication of conventional dentures and partials for many years. The difference is that they are screw-retained on temporary cylinders in order to eliminate the unnecessary (and unwanted) palate and border extensions of conventional denture baseplates. They also provide for highly desirable “diagnostics” during the early stages of fabrication, especially on restorations for the maxilla where consideration of additional criteria exist, such as lip support, high lip (junction) line, tight air seal for phonetics, and patient hygiene in difficult areas. Because most patients will desire a fixed (detachable) screw-retained device over a removable attached overdenture, the basebars will also provide an early indication as to whether the screw shaft access holes will present an esthetic problem as well as allow checking for any other divergence, vertical height, or concave ridge lap (sanitary) issues.
Even with conventional dentures, the importance and diagnostic capabilities of well-made baseplates have oftentimes been overlooked. The baseplate is reduced to “just a layer of acrylic on the cast to support some wax for the bite and try-in.” However, if extensions and thicknesses are adjusted at the bite relation and try-in phase, the final prosthesis will already be “properly adjusted” at the time of delivery, or at least very close. This is even more crucial when technology comes into play and we are attempting to reverse-engineer the case by starting with the exact size and contours of the final device in our preliminary set-up and wax-up for laser scanning. When using CAD/CAM technology, the milled titanium bar (and attachments for overdentures) can be virtually and accurately designed within those parameters.
Two-Stage Verified Impression Technique
Obtaining the most accurate master cast possible for CAD scanning requires reducing the amount of distortion of the various materials used in the fabrication of the cast. The following technique seems to be widely accepted and provides consistent successful results.
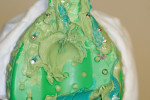
With the first preliminary impression, the clinician simply creates holes in a stock plastic tray (Figure 1) and makes the best impression possible. The technician then constructs a cast from that impression, retracting the impression copings from the preliminary impression, and accurately reseating them on the cast (Figure 2). Using a preformed rigid plastic bar stock for longer spans and pattern resin for short spans, everything is splinted together, creating an intraoral luting jig (Figure 3 and Figure 4). The case is then sectioned, using a thin disc, in favorable positions for clinician access and sequentially numbered (eg, R1-2-3-4-5-6L). This helps the clinician seat the device intraorally with ease and accuracy (Figure 5). The sections will then only need to be luted and splinted together with very small amounts of resin, which minimizes both patient discomfort (time and monomer intraorally) as well as distortion when the resin is polymerized. The luted jig will then be ready for an over impression using a medium/heavy body impression material. Over the course of the past 6 years, the technique and materials have evolved from GC Pattern Resin (GC America, www.gcamerica.com) (Figure 6), to GC pattern resin combined with pre-formed bar stock (Figure 7), to today’s low distortion Pi-Ku-Plast (Bredent, www.xpdent.com) and bar stock (Figure 8).
The laboratory then fabricates a precision custom tray with access holes for the impression copings that offers strong structural support for the impression material and as much extension of the screws as possible for good accessibility (Figure 9, Figure 10, Figure 11, Figure 12). The more divergent the shafts, the more “slop” is needed in the screw-access holes to allow for full, accurate seating of the tray (Figure 13 and Figure 14).
When the clinician returns the final verified impression to the laboratory for construction of the final verified master soft-tissue cast, use only Type IV die stone to reduce the amount of distortion that will be caused by expansion. Splinting the impression copings in the mouth not only minimizes distortion due to polymerization of the impression material, but also movement of the analogs due to expansion of the die stone as it sets. The importance of these steps cannot be overstated as the accuracy of the master cast is the single most critical factor in obtaining an accurate CAD-scanned/designed and CAM-milled implant bar that is a passive fit to minimize undesirable stress or forces on the implants.
Screw-Retained LC Resin Basebars
To further examine the advantages of screw-retained basebars over conventional baseplates when fabricating CAD/CAM-milled titanium bar restorations, the patient’s perception needs to be understood. Patients have invested a considerable amount of time and money for implant placement, not to mention the additional cost of the restorative procedure, all to escape the “dentures in a glass” scenario. Preliminary seating of a final size/contour device that is screw-retained and “fixed” is an instant indication and gratification that the investment is already paying off. It provides the clinician with a very stable device for establishing the vertical dimension of occlusion (VDO) at the records appointment, as well as at subsequent try-in(s). The device also provides the clinician with the additional benefit of diagnosing important criteria, especially in the maxilla, that determine if a screw-retained fixed-detachable will be feasible or if an attached overdenture is indicated.
Equally important for the technician is the fact that once the clinician and patient have approved the esthetics and bite of the set-up and it is time to laser-scan the device for CAD design of the bar, the technician is working with the specific contours that are expected of the final finished prosthesis. This is important with screw-retained hybrid bars, but even more critical when the case is an attached overdenture bar where additional space must be incorporated for a cast metal reinforcement mesostructure and attachments.
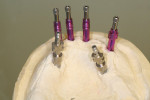
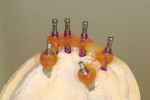
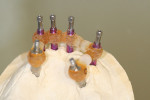
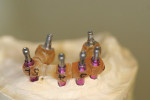
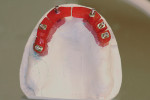
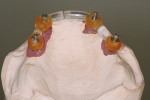
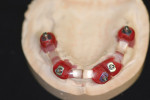
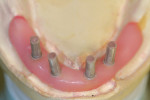
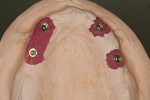
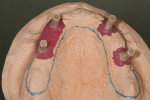
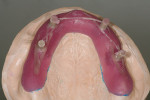
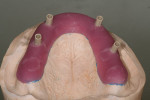
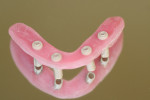
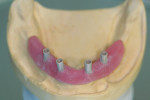
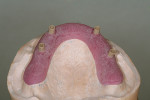
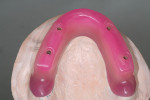
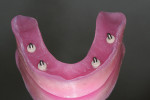
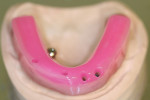
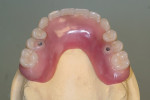
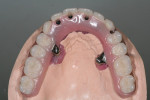
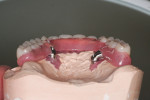
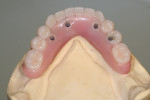
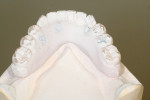
When fabricating a SR basebar, temporary copings, either titanium or plastic, are incorporated onto the master cast but always non-engaging. Although this device will function properly if cylinders are installed on all of the implants, it is more economical and efficient for the clinician as well as more comfortable for the patient, if only one cylinder per quadrant is used. This eliminates the need for removal and reseating of all of the healing abutments each time the clinician must obtain records or conduct a try-in(s). However, it is critical that the clinician provides the laboratory with a set of healing abutments identical to the ones that are in the mouth, so that the basebar fits precisely and rests on top of them to provide vertical support when the device is fully seated and screwed down (Figure 15, Figure 16, Figure 17, Figure 18). The exception to using this technique could be for a screw-retained hybrid where there is a need to assess the divergence and screw-access holes for all of the implants and their relationship to denture teeth that will be placed in proper esthetic and occlusal position during the next step of fabrication (Figure 19).
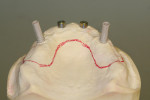
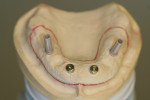
The desired extensions are then outlined on the cast and any undesirable undercuts blocked out with wax. This includes any space below the margins of the temporary copings and the driver holes on the top surface of any healing caps. This technique can be carried even one step further in the case of a SR-hybrid in which the clinician’s preference is to have the final mandibular restoration raised a millimeter or so off the tissue to allow the patient to clean underneath the device and around the implants by adding a layer of relief wax to the ridge (Figure 20).
A sheet of light-cured baseplate resin is then carefully adapted, ensuring that the material is well attached to the cylinders. If the vertical height is limited, or if there is an unsupported cantilever extension that would be cause for concern with regard to strength and possible breakage intraorally, then a relatively new but remarkable light-cure reinforcement material, Fiber-Force (Synca Direct Inc., www.fiberforcedental.com), can be used. Because both materials are light-cured, the reinforcement tape can be wedged between two layers of the baseplate material and around the cylinders, then the two materials cured simultaneously as long as enough time and/or cycles are used to ensure a thorough curing (Figure 21, Figure 22, Figure 23, Figure 24, Figure 25).
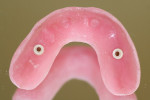
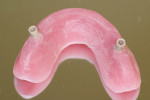
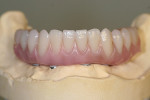
The cured basebar is then carefully finished to the anticipated extensions of the final restoration (Figure 26, Figure 27, Figure 28) and the wax rim applied to the basebar using guide pins (chimney screws) to help create the screw shafts in the wax (Figure 29, Figure 30, Figure 31, Figure 32). The same guide pins can be used at the processing stage to create the same shafts in the acrylic or denture teeth in the case of a SR hybrid. (They cannot be used in processing an attached overdenture.)
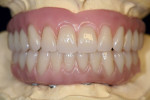
The next two stages of fabrication, VDO bite records for articulation and setting of the denture teeth with esthetic wax-up for try-in will closely mimic the procedures used for conventional dentures (Figure 33, Figure 34, Figure 35, Figure 36, Figure 37). Once the clinician and patient have approved the tooth arrangement and wax contours, and additionally, for a maxillary case, agreed to the type of device that best serves the patient’s esthetic, phonetic, lip support and hygienic requirements, the laboratory is then ready to laser-scan the verified master cast for implant position, tissue, and the device itself (Figure 38 and Figure 39).
These images are then married to provide the 3D virtual screen that is used to properly design and position the bar (as well as attachments in an overdenture) within the parameters of the device (Figure 40). This allows the bar to be milled in a very precise and predictable fashion. When the reverse-engineered milled bar is returned for final assembly and processing, all the components fit together in harmony with no surprises or obstacles to overcome.
About the Author
Thomas Wade, CDT
Owner
New Horizons Dental Laboratory
Broomfield, Colorado