Coming Closer to Nature
Using opalescent lithium disilicate to match the optical properties of natural teeth.
By James Fondriest, DDS, FICD, FACD; and Matt Roberts, CDT
Restorative dentists continue to search for the ideal restorative porcelain to restore teeth in the esthetic zone. Ideally, it would be a material that is easy to work with, strong, and can faithfully duplicate the optical characteristics of each layer of a natural tooth. If the surface of the teeth were opaque, it would be far easier to replicate a natural appearance.1 Enamel, however, possesses varying amounts of anisotrophic translucency, which introduces many optical effects that are difficult to replicate with ceramic. One property of natural enamel that can create a highly complex visual display is opalescence. This case report shows how the new opalescent lithium-disilicate ingots with creative coping design and layering can help in the effort to create a natural restorative result.
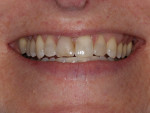
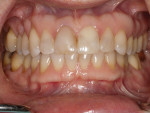
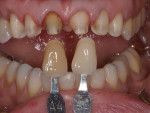
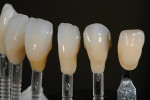
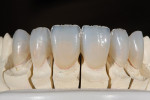
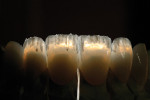
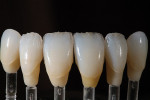
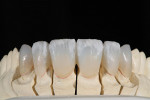
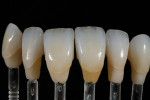
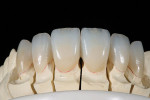
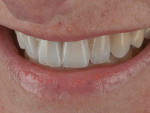
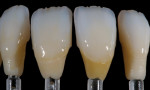
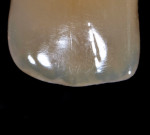
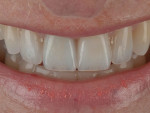
The patient desired to achieve a smile that was natural in appearance but more symmetrical and brighter than her existing teeth (Figure 1, Figure 2, Figure 3 through Figure 4). Bleaching had been only slightly effective. She wanted a "clean translucence" to her new smile but wanted to cover the chromatic "blotchiness" of her natural teeth. This patient had a very good grasp of the usual characteristics of natural teeth and wanted to duplicate them. She understood the natural phenomenon of chroma gradients that occur from the gingival crest to incisal edge and from the cuspids to the midline. She wanted an exaggerated chroma gradient, moving from the darker UL posterior teeth and getting much brighter going to the midline.
Maintaining as much natural tooth structure as possible is always a priority when performing restorative dentistry. While less tooth reduction is a desirable goal, there are times when more reduction better serves the overall restorative agenda. Prior to tooth preparation, the desired level of brightness and translucency is decided. The color and condition of the existing dentition as well as strength requirements are assessed. The amount of color change required of a bonded restoration will determine the amount of tooth reduction. The more change in color desired, the thicker the ceramic layer will need to be to provide adequate filtering of underlying color. The dentist-technician team makes choices about the depth of preparation, based on the masking ability of the preferred material selection.
A connective tissue graft was performed to fix the gingival clefts and lower the scallops above teeth Nos. 4 through 6 (Figure 5). Mixed coverage porcelain restorations were planned for teeth Nos. 6 through 11.
It was presumed that as preparation began, the chromatic blemishes within the teeth may actually increase in magnitude. It was explained that the depth of preparation that would be necessary for the chosen translucent porcelain to completely mask the dark spots depended on the severity of the discolorations within her teeth and the amount of color change being attempted in the treatment (Figure 6). Less preparation was done on the gingival portions of teeth Nos. 6, 7, 10, and 11 so that a chroma gradient could filter through the translucent porcelain, going from gingival to incisal (Figure 6).
The provisionals were too long and the patient agreed to allow some shortening from her original desired length. The reverse smile line was diminished more by shortening the length of the cuspids and premolars (Figure 7, Figure 8 and Figure 9).
In the Laboratory
After reading the prescription, reviewing the comprehensive PowerPoint presentation of the patient’s case, and examining the mounted casts of the provisional restorations and prepared tooth models, the laboratory process started by taking a silicon matrix of the provisional restorations. The prepared tooth model (working model) was treated with cement spacer and separator, and the matrix of the provisional model was carefully seated on the prepared tooth model. A small hole in the incisal edge of an anterior tooth was placed over the tip of a wax injector and the cavity was filled with wax (Yeti Beige Thowax Inlay Wax). This injection process transfers the shape, form, and function of the provisional restorations to the final wax-up. From this point, changes in the wax were made based on examination of the photos of the provisional restorations, the doctor’s requests from the lab slip, and instructions in the PowerPoint presentation (Figure 10).
Once the desired contour was achieved, the restorations were separated using a thin cutting blade and the incisal areas slightly reduced to allow room for micro-layering. This incisal cutback is performed in wax when working with lithium disilicate to eliminate the need for mass reduction of the ceramic material, which resists grinding more than conventional ceramics.
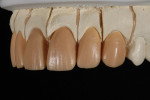
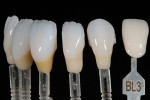
The restorations were then pressed (Figure 11) and de-vested. Composite dies representing the color of the patient’s prepared teeth were fabricated. The restorations were fitted to the working model and ground to final contour. Incisal cutback was refined to imitate internal lobe formation prior to color modification (Figure 12). The initial shade was evaluated on the composite dies (Figure 13 and Figure 14). The restorations exhibited a natural color of BL3 prior to staining, but were easily modified to a final desired color of A2 with the use of essence stains.
Once the shaded restorations were fired, a layer of glaze was applied and the restorations were placed back on the working model in preparation for layering the incisal effects with powdered ceramic (Figure 15). Color modification during the staining process was undertaken in the incisal areas as well as the gingival portions of the restorations, greatly enhancing the potential for color effects.
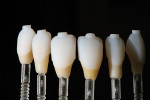
The authors’ layering strategy was designed to maximize the amount of pressed lithium disilicate present in the final restorations to create the strongest possible outcome for the patient. Ingot choice, in this case Opal 1 IPS e.max (Ivoclar Vivadent, www.ivoclarvivadent.com), was made to minimize the need for layering ceramic. The ingot itself allows the underlying color of the prepared teeth to provide much of the color for the final result. By having color come out from underneath and using the ceramic as a filter of this color, more natural light circulation through the teeth is achieved and a more natural final result is possible. The Opal 1 ingot displays optical properties very similar to natural enamel, filtering the underlying dentin colors like natural teeth. A very small amount of incisal layering can be used to enhance these pressed restorations to exhibit very dynamic incisal translucency.
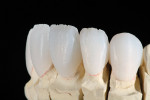
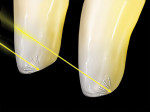
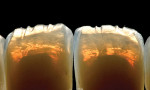
To maintain full control of incisal effects, the initial application of colored incisal ceramics is put into place and fired prior to filling out the incisal area to full contour. This build-up is kept very thin facial lingually, leaving room for enamel overlayering to complete the contour. Backlighting of the build-up shows the variations of translucency of the effect porcelains (Figure 16). Once fired, these effects can be evaluated and modified as desired, prior to finishing the full-contour build-up of the incisal area (Figure 17).
If changes are desired in the incisal effects, the ceramist has full access to modify them by grinding or adding additional effect ceramic. Once satisfied with the translucency and color pattern in the incisal, an appropriate enamel powder is used to accomplish the full contour (Figure 18 and Figure 19).
After firing the full-contour enamel application, it may be necessary to make small corrections prior to grinding in the layered incisal ceramics to match the contour of the pressed lithium disilicate. This needs to be undertaken with care to create an invisible transition between layered and pressed areas of the teeth (Figure 20).
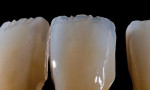
The restorations should then be placed back on the composite dies for final glazing. After the glaze firing, diamond polish can be used to create the desired surface luster to the ceramic. Backlighting displays the opalescent characteristics of this ceramic material (Figure 21), while front lighting shows the dynamic incisal effects possible with a micro-layered approach (Figure 22). Figure 23 shows the final restorations on the stone model, prior to delivery to the clinician.
Addressing Patient Expectations
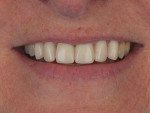
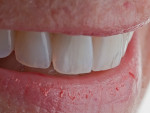
Cosmetic dentist-technician teams can differentiate themselves from competitors and thrive by listening to patients’ expectations and achieving the cosmetic results requested. With some clients, the level of critical judgment over the details can skyrocket. When this patient came into the authors’ office, she was using a magnifying mirror. She used the mirror to describe things she saw in her mouth and to describe her restorative desires. It is difficult to cover blotchy tooth stumps using translucent porcelain, or to provide both bright and translucent porcelain, or to create and blend a believable chroma gradient from A3 to OM3. With thoughtful tooth preparation and a pressed opalescent lithium-disilicate coping, most of this patient’s goals were met (Figure 24 and Figure 25).
Opalescence Explained
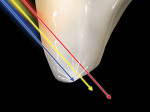
Opalescence can be described as a phenomenon whereby a material appears to be one color when light is reflected from it, and looks another color when light is being transmitted through it.2 A natural opal is an aqueous disilicate that breaks transilluminated light down into its component light spectrum by refraction. Opals act like prisms and refract (bend) different wavelengths to varying degrees (Figure 26 and Figure 27).
Translucent enamel displays the property of opalescence. Opalescence causes tooth enamel to reflect blue light back to the observer (Figure 28). Enamel has a primary mineral makeup of hydroxyapatite, which is crystalline calcium phosphate. Hydroxyapatite crystals align in organized, tightly-packed masses to form prismatic enamel rods. Refraction will occur as light passes through each enamel rod and at the surface of a tooth. The shorter wavelengths will bend more, and the longer wavelengths will bend less.1
Blue light tends to bounce around more or to scatter within the enamel body (Figure 29). The red-yellows do not bend as much at prismatic interfaces and a higher percentage will escape the enamel. The blue accumulates within the enamel, causing it to appear bluish even though it is intrinsically colorless.1,3,4 This also explains why the lingual view will be red-yellow, because all of the blue is filtered out and only the red-yellows transilluminate out of the lingual side.
The Fiberoptic Effect of Enamel
When light travels from one translucent material to another, the light will be either reflected at the surface or it will pass through the surface but gets bent as it passes. The more optically dense a translucent material is, the more light will enter and stay within its body. Diamonds are optically dense and their tendency to collect light makes them as valuable as jewels. For light to escape from one translucent material of high optical density (enamel) to another material of low optical density (air), the "critical angle" of incidence must be close to perpendicular. This means that any light rays closer to parallel to that boundary will not cross the boundary and will stay within and get reflected back internally. This effect is used in optical fibers to confine light within a cable. Light travels along the fiber bouncing off of the boundary. Because the light must strike the boundary with an angle greater than the critical angle to escape, once the light enters the fiber at a low angle virtually parallel to its walls, it will travel down the fiber without leaking out.
The opalescent effects of enamel brighten the tooth and give it optical depth and vitality.5 When natural teeth are illuminated, all of the visible wavelengths scatter to a certain degree and remain within the body of enamel. Incident light will enter one side of a tooth and scatter enough that when it reaches the opposite external surface of enamel, it does so at an acute angle. Significant amounts of all wavelengths will fail to escape, thus continuing to scatter within the body of enamel.6 Due to a higher optical density than other dental porcelains, this porcelain will act like a fiber-optic cable holding the light within its body just as enamel does. This gives the porcelain an improved ability to be both translucent and bright (Figure 30).
The Halo Effect
Another natural visual effect commonly mimicked in porcelain restorations is the halo effect. In natural teeth, it is caused by the reflection of red-yellow wavelengths off of the internal lingual incisal surface of enamel (Figure 31). The actual incisal enamel has no difference in colorants/stains than the rest of the body of enamel. The red-yellow light reflects/scatters off of the buccal-facing lingual incisal surface because it hits the surface at too low of an incidence angle to transilluminate. The scattering halo effect will occur in natural teeth when there is a buccal-facing lingual incisal surface of enamel at the right angle. Most unworn incisors will exhibit a halo but not all teeth with incisal wear facets will yield the visual halo effect. The wear facet must have a buccal-facing angle (Figure 32).
Technicians traditionally have created an artificial halo in porcelain restorations by employing more opaque porcelain or by laying stains into the incisal edge. These halo effects can be lost easily through wear of the restoration or by occlusal adjustments in crossover movements by the restorative dentist. Ideally, all visual effects of natural teeth should be re-created in restorations by using multi-layer ceramics with the same optical properties as the teeth being duplicated and not by employing stains.7
Due to the opalescent effects of this porcelain, the refractive characteristics are high and a natural halo will form without stain if light can reflect off of a scattering surface. As seen in Figure 33 and Figure 34, the technician created an internal angled surface at the incisal edge and interproximally with the pressed coping to scatter the red-yellows.
Metamerism
The light in which a porcelain restoration is viewed can affect its appearance. Metamerism is the phenomenon by which an artificial restoration can match under one lighting condition (in the laboratory or office), but appear different under other lighting.8 Natural teeth have the ability to opalesce more than most dental porcelains. The visual display seen depends on the nature and vector of the light source illuminating the object. A porcelain restoration might reflect light off of its surface exactly as enamel does in photographs at one angle but under different illumination and at many different angles, the two objects that previously looked identical might look quite different.9 It is not just the surface reflectivity that creates a good match but also how the light is scattered within the porcelain body. When reconstructing a tooth with dental porcelain, mimicking the layers of the tooth by employing materials with the same optical properties will minimize metamerism. The closer the optical properties of the two materials to be matched, the more successful the color match will be.10 Use of opaque surface stains to correct mismatches will increase metamerism because it limits the light entering the deeper layers of porcelain.11
Matching Natural Teeth optically
Often artificial restorations are most vulnerable to detection in natural sunlight. This opalescent porcelain has positive characteristics in bright, full-spectrum light. Closely assessing this patient’s anterior restorations at different vectors and with illumination from an opposing angle displays some of the optical effects that make this porcelain so interesting (Figure 35). As the incident light enters these restorations, the blue opalescent qualities appear superficially without placing blue stains within the ceramic layers. Along the incisal perimeter, a halo is evident. The blue opalescent properties of this porcelain accentuate the halo effect that the technician created by placing internal angles on the copings and the angled incisal edge facets that the dentist created, both of which scatter the red-yellow wavelengths.
The higher the optical density of porcelain is, the greater the optical depth and overall brightness becomes. Significant amounts of incident light are kept within the body of porcelain, failing to have the critical angle to escape.6 Red-yellow light that had transilluminated through the buccal layers of porcelain is being bent around the lingual surface of the restoration and shows as a brighter signal on the distal incisal surface of tooth No. 8. This is a manifestation of the fiber-optic effect of this porcelain.
The final result achieved the patient-driven agendas of morphological symmetry, chromatic uniformity with chroma gradients, translucency, and a natural incisal display with opalescent blue and an incisal halo.
References
1. Overheim RD, Wagner DL. Light and color. New York, NY: John Wiley and Sons; 1982
2. SundarV, Amber PL. Opals in nature. J Dent Tech. 1999;16(8):15-17.
3. Winter B. Visualizing the natural dentition. J Esthet Dent. 1993;5(3):102-117.
4. ten Bosch JJ, Coops JC. Tooth color and reflectance as related to light scattering and enamel hardness. J Dent Res. 1995;74(1):374-380.
5. Garber D, Adar P, Goldstein R, et al. The quest for the all-ceramic restoration. Quintessence Dent Technol. 2000;23:27-49.
6. Fondriest JF. Master’s technique level: shade matching a single maxillary central incisor. Quintessence Dent Technol. 2005;28:215-225.
7. Sieber C. In the light of nature. Quintessence Dent Technol. 1993;16:60-68.
8. Pensler AV. Shade selection: problems and solutions. Compend Contin Educ Dent. 1998;19(4):387-396.
9. Fondriest JF. Shade matching: the science and strategies. Int J Periodontics Restorative Dent. 2003;23(5):467-479.
10. Sproull RC. Color matching in dentistry. Part III. Color control. J Prosth Dent. 1974;31(2):146-154.
11. Freedman G. Color communication. J Can Dent Assoc. 1994;60(8):695-699.
About the Authors
James Fondriest, DDS, FICD, FACD
Founder and Owner
Lake Forest Dental Arts
Lake Forest, Illinois
Matt Roberts, CDT
Founder
CMR Dental Laboratory
Idaho Falls, Idaho