All-Ceramic Bonded Posterior Restorations
Implementing design and fabrication principles to achieve optimal esthetics and longevity.
By Gilbert Young, CDT
Merging natural-looking occlusal anatomy and proper function remains a challenge that some dentists and dental ceramists disregard. Some say that posterior restorations “are in the back of the mouth where nobody will see them,” and this has become their rationale in determining the degree of functional and esthetic quality for these restorations. However, posterior restorations provide an opportunity to exercise not only control and beauty in function, but artistic mastering of form and color. The predictability of indirect posterior all-ceramic bonded restorations has been questioned almost since the beginning of their use in restorative dentistry. However, the preparation design to properly deliver these types of restorations continues to be sometimes misunderstood. In the laboratory, some technicians lack knowledge of the sound principles of dental anatomy and occlusion and experience in working with them. Combined with high production quotas, this has often led to higher failure rates and functionally and esthetically compromised restorations, which has forced dentists and dental technicians to rely on materials and other processes to compensate for the deficiencies on both sides.
Relatively newer materials, such as pure lithium disilicate, appear to offer a promising future for these types of restorations. Yet, questions still remain about whether their success hinges on the strength of the material alone or if it also depends on additional factors, such as preparation design, bonding technique, and occlusal force management. Are any of these fac tors less important simply because there is now a material that allows dental technicians to rely on its relative strength alone?
If the goal is to restore dentition to the full extent of its definition, it would seem logical that adequate esthetics for the posterior region should be part of the final result. In the following paragraphs, the author will explore preparation design theory and principles and the corresponding fabrication technique for layered all-ceramic bonded posterior restorations.
Preparation Design Principles
Studies have shown that brittle restorative materials, such as dental ceramic, are strongest when under compression.1 Thus, a ceramic onlay with an even thickness of 1 mm to 2.5 mm, passively seated over a shallow concavity or saucer, will be in full compression under masticatory forces.2 This principle is applicable to any ceramic material. A flat object of uniform thickness can rest on another flat surface and support a given load on top of it without breaking (Figure 1). In a similar fashion, a restoration fabricated using the design and principles discussed, is capable of withstanding forces exerted upon it (Figure 2).
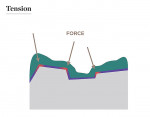
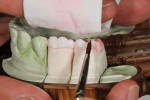
Standard “G.V. Black” preparation techniques provide the necessary mechanical retention for a posterior restoration for conventional cementation; however, the all-ceramic bonded restoration relies on chemical bonding for retention, which eliminates the need for residual cuspal outline for mechanical retention. Many dentists resist the idea of not having a retentive element on a restoration, leaving the preparation with enough convexities to create excessive tension on the ceramic once it is bonded (Figure 3 through Figure 5).
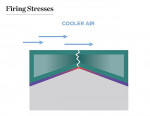
An increase in firing stresses is associated with the cooling of ceramic material, which is another potential problem with uneven thickness in an all-ceramic restoration (Figure 6). Thin areas cool faster than thicker areas (uneven contraction), creating stresses within the restoration. Sometimes these stresses remain in the restoration, but are not readily seen until much later—after the restoration has been seated for some time. Although conceptually acceptable, such preparations can be left with sharp angles and undercuts (Figure 7). Even if the final restorations might have an acceptable thickness, the inner surface will remain under tensile stress. Additionally, the small undercuts left on the preparation will have to be blocked out in the laboratory, resulting in a layer of bonding resin that is thicker than necessary.
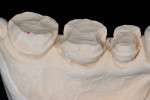
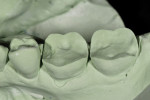
Figure 8 demonstrates the ideal preparation for all-ceramic bonded restorations.3 The minimal preparation for porcelain coverage on the buccal surface of the 2nd premolar and 1st molar maintain the natural width of the occlusal table. The buccal cusps of the restoration are supported on the flat surface of the buccal half of the preparation.
Brittle materials, such as dental ceramics, are subject to catastrophic failure under the right circumstances. Cohesive fractures or “chipping” of a ceramic restoration may have more to do with the quality and handling of the material by both the dentist and dental ceramist, ie, occlusal force management. Inert flaws and inclusions can also lead to failures, and are more or less controlled during the fabrication process. Strength in brittle materials is more of conditional material property,4 and flaws that affect strength can be introduced during the fabrication process or through grinding, when the restoration is adjusted during seating. How long a restoration will last depends on all of these factors.
Fabrication Method
The goal for both the dentist and dental ceramist is to deliver as conservative a restoration as possible that fits, functions correctly, is esthetically pleasing, and is strong once it is bonded. To avoid compromising the success of the restoration, the dentist must rely on the principals of preparation described above and adhere to a strict and methodical bonding system.
For the purposes of this article, the author will limit the discussion of this technique to the fabrication of all-ceramic bonded onlays. The use of this technique is limited only to restoring posterior teeth where:
An ideal thickness of 1 mm to 2.5 mm at the thinnest area of the restoration can be achieved, ie, the central fossa area.
• Margins are all supra-gingival or readily accessible at the time of seating.
• A rim of sound enamel is readily visible around the periphery of the preparation.
• The occlusal forces can be controlled and managed predictably.
• The dentist has a successful record of bonding all types of all-ceramic restorations.
• Proper preparation guidelines can be followed.
Refractory Die Technique
The use of refractory die materials offers significant advantages for the fabrication of all-ceramic bonded restorations. It is possible to fabricate conservative restorations with very delicate margins that allow for a seamless transition between the restoration and the natural tooth structure for both anterior and posterior restorations. The same ceramic used for porcelain-fused-to-metal restorations can be used with this technique. Color and esthetics can be managed from the inside out for every part of the restoration. It is not necessary to rely on surface colors that can wear or grind off. Restorations, such as no-prep veneers, one-surface laminates, three-quarter veneer crowns, and ceramic onlays, can all be fabricated with a high degree of marginal and fit accuracy using the refractory die technique.
Master Die Duplicating Technique
Precise model and die fabrication is key to creating an accurate all-ceramic onlay. The best techniques for accurately duplicating models and dies are those that allow easy and simple duplication of the master die within the master model, without excessive use of duplicating material and longer-than-necessary setting times. It is crucial to use a predictable refractory investment, such as G-Cera VEST (GC America, www.gcamerica.com), that is consistently mixed to manufacturer’s instructions.
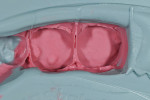
An accurate duplicating material consists of a vinyl polyether silicone, like a wash impression-type material, in combination with a lab putty (GCLT Laboratory Putty, GC America) to form an impression over the master die (Figure 9 and Figure 10). Because of the fast setting time and accuracy of the impression/duplicating material, this system is practical and economical for the refractory die technique.
Layering Technique for All-Ceramic Onlays
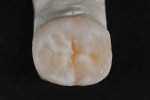
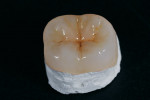
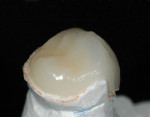
The ability to mimic and transition the color of the natural tooth structure to the restoration is one of the advantages of using the refractory die technique. It enables the dental technician to create a natural-looking restoration that is almost indistinguishable from adjacent natural teeth (Figure 11). Intraoral images that communicate to the ceramist the nuances in the shade and color of the patient’s natural teeth are key in creating a lifelike restoration. However, when fabricating occlusal onlays, certain anatomical features of the dentin and enamel layers are standard to any posterior tooth for this type of restoration. Knowing and understanding these features allows the ceramist to develop a simple layering system that will closely express the depth and vibrancy of the occlusal surface of a posterior restoration (Figure 12 and Figure 13).
The author’s technique for building and layering posterior all-ceramic onlays consists of three basic steps after the refractory die has been prepared for porcelain application.
Transition Color Layer
This step involves applying a thin layer of ceramic material (Figure 14), which consists of an intensified dentin color to mimic the color of the existing dentin and an incisal material to mimic the layer of enamel that surrounds the natural tooth. This step imparts depth and vitality to the restoration, and also procures an intimate adaption of the ceramic material to the refractory die during firing. This decreases the amount of “lifting” or detachment of the subsequent build-up (Figure 15). GC Initial™ Inside and Cervical Translucent (GC America) are adequate powders to express the transition color layer (Figure 16).
Dentin Body Build-Up
The selected dentin shade is modeled over the occlusal surface of the preparation. For the most part, the contour of the prepared tooth guides and dictates this step, making it impossible for the ceramist to over-contour the occlusal table. The cusps during this step are kept in minimal contact with the opposing model, but maintain their correct position and direction toward the corresponding contact areas on the opposing teeth. A slight imprint on the raw porcelain is all that is necessary to visually establish the correct position of the cusp tip (Figure 17). The key during this step is to avoid disturbance of the porcelain particles (“mushing”)—a common but often overlooked cause of excessive tearing in the porcelain during firing.
Moisture control is critical, as the refractory die must be kept rather wet to avoid possible infiltration of air bubbles into the ceramic material. After the dentin build-up is completed, slight tapping of the model will cause moisture to rise to the surface of the refractory die and the dentin build-up, thus allowing for settling and condensation of the dentin. Slight blotting with tissue paper causes further condensation while giving the build-up enough firmness to proceed with the cutback for incisal materials. The dentin is cut back at a 15˚ angle along its periphery on the labial and lingual-occlusal surfaces. The occlusal surface is cut back about 0.5 mm to allow enough space for the occlusal layering material. A diluted wash of chromatized pigment with a staining medium is applied to the central fossa area to add depth (Figure 18).
The dentin build-up is now layered with the corresponding incisal material. For all practical purposes, an incisal white material is a good choice for replicating the “whitish” appearance of the enamel layer in posterior restorations (Figure 19 through Figure 22). In an effort to be highly artistic, many ceramists mistakenly over-layer with too many translucent and effect ceramic materials. This can be detrimental as it can create a low-value or “grey rim” at the peripheral border of the occlusal table when the restoration is viewed from the occlusal aspect. A simple approach to layering the occlusal surface is not just easier and faster, but ultimately yields a much better result. The use of the white incisal, or a comparable substitute, is a simple and appropriate material for this step.
Further characterization of this layer is not necessary, unless the ceramist has to match adjacent teeth with a higher degree of accuracy. The occlusal ridges are best expressed with a 50% mixture of incisal white and dentin. Straight incisal must be avoided on the occlusal, as it tends to lack enough opacity and reflectivity to properly express the character of natural posterior anatomy. Once the occlusal surface is formed, further application of a more saturated white incisal material can be applied to those areas where no occlusal contact will occur, ie, the peripheral border around the lingual aspect. Otherwise, this material can be applied on the add-on or correction firing.
The whole build-up of the posterior onlay is done in one step on the first firing. This is because shrinkage of the ceramic will migrate toward the middle or the area of greatest mass. Ceramists often see shrinkage as a negative factor in ceramic layering, but “controlled shrinkage” is actually desired in this technique as it naturally creates the space necessary for subsequent layering material crucial to the realism of the restoration (Figure 23). At this stage, special incisal materials with a higher concentration of white can be applied to further express the whitish character of the ridges to create a more natural-looking restoration (Figure 24). Because all posterior teeth have a thick layer of enamel wrapping the dentin, this technique makes perfect sense.
Final Contouring and Glaze
The restoration is now adjusted with conventional grinding instruments. Occlusal adjustments to establish the correct number of centric contact points are monitored with an indicating stripe of a thickness that is no more than 20 mm. Premature contacts during excursive movements are monitored with the use of a thicker indicating stripe of about 40 mm. Final anatomy and expression of the interlobular fissures are expressed with the use of a sharp inverted cone and a point fissure carbide burr. Utmost care is observed during this step to avoid creating fissures that are excessively deep, which will not only look unnatural but can also impart excessive stress to the ceramic material.
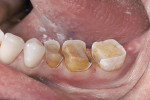
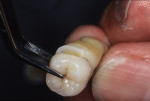
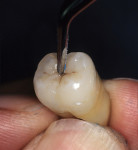
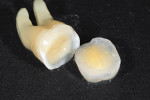
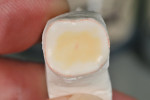
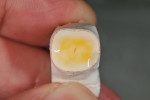
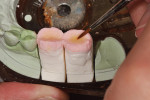
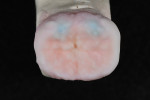
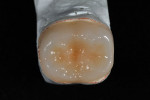
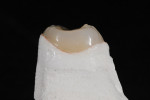
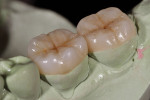
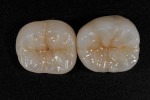
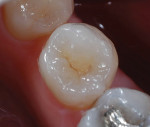
Figure 25 shows a restoration in which the bulk of the refractory die had to be eliminated before final firing because of its large size. This ensures proper maturing and integrity of the ceramic material, as excess refractory material acts as a heat sink. Figure 26 demonstrates the finished and seated onlay restorations after final glaze and divesting. Notice the integrity of the inner side of the restoration (Figure 27) and the natural resemblance to the color scheme of the prepared tooth (Figure 28). Using the transition color layering technique for posterior all-ceramic bonded restorations, it is possible to obtain an almost seamless bond between the natural tooth and the restoration (Figure 29 and Figure 30).
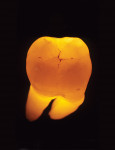
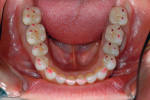
When transilluminated, the restoration becomes indistinguishable from the natural tooth (Figure 31). Figure 32 and Figure 33 depict the holding contact points and functional guides for a full-mouth reconstruction case with a combination of all-ceramic bonded onlays and crowns and PFM restorations. A balanced occlusion is key to the longevity of all-ceramic restorations.
Conclusion
The refractory die technique for layered all-ceramic bonded restorations is a simple and direct method for fabricating functional and esthetically pleasing restorations. The success of these types of restoration hinges upon understanding and controlling factors such as preparation design, fabrication procedures, occlusal management, dental anatomy principles, and bonding techniques. The patient’s genetic make-up and lifestyle may also contribute to the longevity of these types of restorations. Therefore, it is imperative that both the dentist and dental ceramist understand what is required of each of them to provide the best possible outcome for the patient.
The author would like to thank the team at GNS dental studio, Dr. Jimmy Eubank, Dr. Richard Alpert, and Steve McGowan, CDT, for their contributions in the preparation of this article.
References
1. Richerson DW. Modern Ceramic Engineering: properties, processing, and use in design. 2nd ed. New York, NY: Marcel Dekker Inc;1992:223.
2. Kelly JR. Clinically relevant approach to failure testing of all-ceramic restorations. J Prosthet Dent. 1999;81(6):652-61.
3. Eubank J. All-Ceramic Restorations—Preparation Guide for Seven Different Situations. Plano, TX: J. Eubank;2003.
4. Kelly JR. Perspectives on strength. Dent Mater. 1995;11(2):103-10.