Minimal Invasion—Maximum Esthetics
Replacing a restoration that is nearly 30 years old with one that is esthetic, natural-looking, and metal-free.
By Benjamin Votteler, MDT; and Michael Fischer, DMD
In the case described in this article, the authors were presented with an extensive and, for the most part, trouble-free oral situation begging the questions of how and why was it being restored? The answer to the question “why” was very simple: the old restoration had served its purpose, plus the anterior esthetics could be improved. Therefore, the question of “how” was also answered. If it proved to be possible, the authors would prefer to use an adhesive bonded all-ceramic solution for this case. Veneers made of feldspathic ceramic can be built up freely on refractory dies and produced in very thin layers that will achieve all the necessary optical effects. This means that the patient can be offered maximum esthetics and function with minimally invasive preparations.
Case Presentation
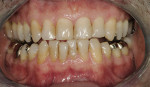
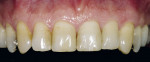
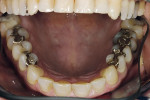
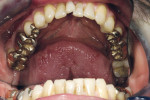
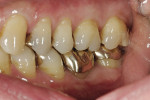
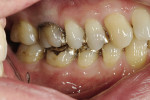
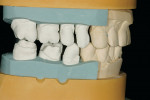
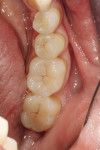
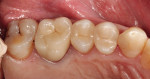
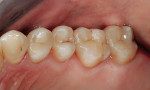
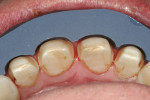
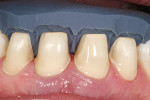
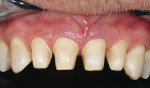
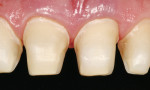
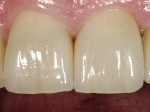
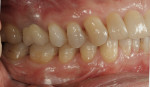
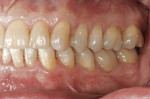
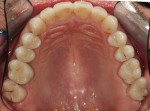
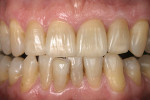
The 54-year-old patient presented at Dr. Fischer’s practice with a restoration that was nearly 30 years old: various and, for the most part, insufficient full-metal crowns, gold inlays and onlays, partial crowns in the molar and premolar area, as well as partial large composite fillings in the proximal and labial areas of the upper anterior teeth. The patient wanted a new, esthetically pleasing, but unnoticeable restoration (Figure 1, Figure 2, Figure 3, Figure 4, Figure 5 and Figure 6).
In the course of the pretreatment stage, the old acrylic fillings at teeth Nos. 12 and 22 were removed and, using a dam-matrix, built up with an adhesive composite. The patient had no functional problems with the old restoration and the canine guidance was in excellent working order; therefore, functional therapy was not necessary. The occlusal height had not lowered over the years, which meant raising the bite was not necessary. The upper anterior teeth needed only to be lengthened slightly because, in the resting position with the mouth slightly open, only about 1 mm of the anterior teeth was visible. The new restoration would need a total of 14 posterior teeth plus the four upper incisors; teeth Nos. 13 and 23 were natural, healthy teeth.
In order not to lose the vertical relationship and to keep the treatment steps manageable, the following treatment plan was made:
First visit: Prepare the posterior teeth in the first and fourth quadrant
Second visit: Fit the posterior teeth in the first and fourth quadrant
Third visit: Prepare the posterior teeth in the second and third quadrant
Fourth visit: Fit the posterior teeth in the second and third quadrant
Fifth visit: Prepare the upper anteriors
Sixth visit: Fit the upper anteriors
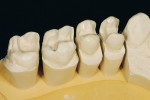
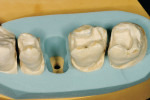
After preparation and taking impressions at the first treatment session, the models were produced in the laboratory. A sectioned model was made for the posterior teeth. The conically-prepared dies were duplicated, and duplicate dies made of refractory material were placed on the sectioned model using the silicon key taken from the plaster model for the location. It is important that the dies are marked with a hex in the proximal area. This secures the duplicate dies in their correct placement and provides a vertical stop because they do not have a pin (Figure 7, Figure 8, Figure 9 and Figure 10). The method described is very precise if the working order is thought through properly. After the glaze firing, the ceramic work should fit into the vertical relationship with very little adjustment.
After the degassing process of the investing material, the dies preparation border was marked with a fire-resistant pen and the first wash firing cycle followed. For this, primary author Benjamin Votteler used transparent shoulder material stained with food coloring to guarantee a thin and even ceramic layer on the die. This process was repeated so that a thin, shining, and homogeneous ceramic layer was placed on the die. In order to control the shrinkage of the ceramic during the main firing cycle, or to achieve an even shrinkage without any tearing, Votteler built up the ceramic in the isthmus area and under the cusp tips that would appear later on the dies at a pre-firing cycle (depending on the preparation shape, he uses opaque-dentin or dentin or a mixture of both).
After that, Votteler produced a good base by using a warmer and more translucent ceramic mixture in the occlusal area to mimic the natural appearance of the occlusal surface. Now he was ready to start the actual layering of the occlusal surface using different enamel and transparent materials. The layering process is only finished when the end result (a functional and natural-looking occlusal surface) is accomplished, taking into consideration the excursive movements for the ISS (immediate side shift) as well as the retrusion.
Because this patient showed no problems with function, the HCN (arbitrary transmission, puts the occlusal plane in the correct relation to the condyle course) was not established through axiography, but was transferred with the help of a protrusion register. The registration was transferred to the obligatory sectioned and mounted models using a skull-related transfer bow. The condyle housing was adjusted until there was contact with the “condylus” of the articulator. In cases such as this, where there is opposition in play (upper against lower), it is recommended—for a perfect occlusion—to do the consequent glaze firing first in one of the jaws.
The sandblasted and fitted ceramic restoration of the glazed quadrant was put back on the sectional model and fixed with TAC gel. In this way, the parts of the occlusion in the opposing jaw that have not been glazed could be adjusted; when this was done these were also glazed. It was necessary to make a full crown for tooth No. 26 because there had been a high loss of substance. It was decided to make a zirconium-dioxide crown, because the stability and the light dynamics of the material are very convincing.
Finally the last minute fine-tuning was completed: the proximal contacts were refined on a non-sectioned control model. After the finished restoration of this quadrant was fitted, Votteler moved to the next step—the upper and lower left posteriors. The procedure used to make the posterior teeth on the left side was carried out in the same manner already described. It is important that the mounted upper and lower models are equilibrated to achieve a satisfactory occlusion, corresponding to the occlusion protocol of the side that is already fitted.
Anterior Teeth
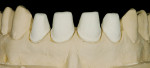
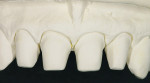
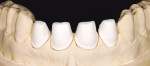
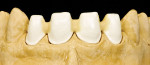
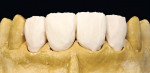
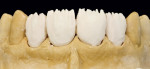
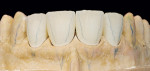
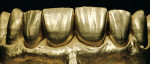
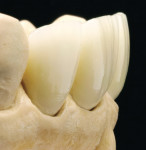
When this area had been completed and the restoration was fitted, the restorative team moved to the final part—the four upper anterior teeth (Figure 11, Figure 12, Figure 13 and Figure 14).
The preparation was done using silicone matrices as guides that were made in advance in the laboratory. This made it is easier to check the trimming of the tooth substance (Figure 15 and Figure 16). Palatally, there was no preparation for a hollow; it was only shortened incisally. In this way, a much stronger ceramic restoration can be achieved compared with a palatal hollow. The preparation border was also protected—as were tensions in the palatal concavity. The preparation was continued interdentally, whereby it took into account that the preparation did not end in the middle of the composite build-up, but rather it was continued all around (Figure 17 and Figure 18). The impression of the prepared anteriors was cast and a “Geller” model with loose dies as well as a solid model was made (Figure 19 and Figure 20).
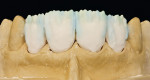
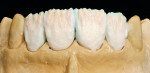
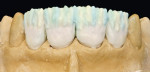
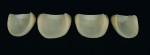
These model variations allowed the restorative team to create a good emergence profile, because information of the gingiva had not been lost. After the anterior teeth had been prepared with a wash as described earlier with dentin-shoulder transparent material and interdentally with opaque-dentin in the area of the labial hollow, it was then fired (Figure 21 and Figure 22). In the following first main firing cycles Votteler continued as follows: It was now fully built up with dentin-enamel (Figure 23), and then cut back (Figure 24), and the crown shapes were lengthened with enamel and transparent material (Figure 25).
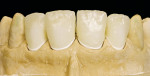
The internal characteristics were built in (Figure 26, Figure 27 and Figure 28); overlaying with enamel, transparent, and effect material (Figure 29). After the firing of the dies (Figure 30), Votteler completed a fixation firing cycle and painted enamel cracks and discolorations in. These were then fired at 100º degrees lower than the temperature of the dentin firing cycle. After that, a second firing cycle followed, which was done to create the appropriate shape and function (Figure 31, Figure 32, Figure 33, Figure 34 and Figure 35).
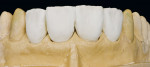
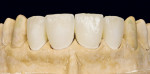
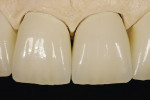
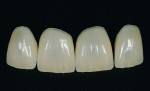
Only now were the shape and surface established (Figure 36 and Figure 37). In this very important step, one must consider the remaining natural teeth (Figure 38, Figure 39 and Figure 40). The finished veneers were secured to the master model and the occlusal movements are checked once again. The layering thickness of 0.5 mm to 1 mm labial shows impressively how little tooth substance was sacrificed (Figure 41, Figure 42 and Figure 43).
During the try-in at the laboratory or surgery appointment, a light carrier should always be used between the veneers and the teeth. Without this, the shade cannot be judged. Glycerine gel is a good option. If there is only a little time between the try-in and the final fit, Vaseline should not be used, as the oils in the Vaseline would impair the bond. These are not completely removed from the tooth even during the etching procedure or steaming with hot water.
After the composite fillings that were prepared in the pre-treatment stage had been sandblasted and newly rebuilt, the dentist cleaned the enamel surfaces and they were etched with phosphoric acid. An adhesive bonder was applied in three steps. While this process was being done, the veneers were etched with a 9% flowing acid and rinsed off after 90 seconds. Then, the veneers were cleaned in alcohol (in the ultrasonic device) and then silanated twice. After the build-up of the composite, one veneer after another was put into the correct position. It is important that the excess composite is removed carefully.
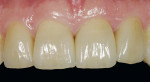
Before the polymerization, an air block should be applied at the preparation border. Finally the edges were cleaned manually, the occlusion was checked and fine-tuned as necessary. A few days after the fitting appointment, the teeth were hydrated again and the soft tissue had relaxed from the invasion. When all was said and done, the restoration looked very natural and lively (Figure 44, Figure 45, Figure 46, Figure 47, Figure 48, Figure 49 and Figure 50).
About the Authors
Benjamin Votteler, MDT
Leading Dental Technician
Dentaltechnik Votteler GmbH & Co
Pfullingen, Germany