Determining the Best Protocol for Early Caries Lesions
An evidence-based guide to nonsurgical treatment
According to the National Institutes of Health, dental caries is an infectious disease, resulting in destruction by acid-forming bacteria found in dental plaque in the presence of sugar.1 Noteworthy is that caries progression is dependent upon time and personal factors such as oral hygiene, diet, saliva, fluoride exposure, education, socioeconomic status, and behavior.2 Like most diseases detected and diagnosed at the early stages, caries can be treated nonsurgically. Therefore, the practitioner is called upon to know the patient as a whole, detect and diagnose the disease at an early stage, and develop individualized treatment strategies.
Caries Risk Assessment, Detection, and Diagnosis
Modern caries management stresses personalized care. CAMBRA (caries management by risk assessment) takes into consideration the individual’s protective factors such as fluoride use, as well as risk or pathological factors such as poor oral hygiene and caries activity (Table 1). Managing caries by risk assessment takes into account the chances that the individual will have a new lesion and ways to prevent that occurence.3 Protective factors and risk factors are easily gathered from patients’ health history questionnaires. Caries activity is simply diagnosed by dental examination. After gathering the pertinent information, the dentist can categorize the caries risk status of a patient into low, moderate, or high. The evidence shows that the most important factor in predicting future risk is recent caries experience and current disease activity.1
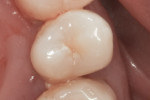
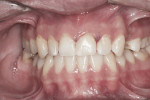
Modern dental caries management should focus on detection at earlier stages of the disease process (eg, non-cavitated caries lesion) and the practitioner’s ability to diagnose the lesion activity.4 At the early stages, caries lesion is non-cavitated (Figure 1 and Figure 2). It is macroscopically intact and is commonly referred to as an “incipient” or “white-spot” lesion. An incipient lesion can be defined as a subsurface layer lesion, with an apparently intact surface layer but having demineralization present beneath it.5 These lesions may appear not only as white but also as yellow and brown coloration. Initial incipient lesions are only seen visually when the teeth are dried, while more advanced lesions can be seen both wet and dried. If allowed to progress, the incipient caries lesion will eventually result in cavitation.
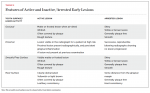
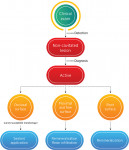
A caries activity diagnosis follows caries lesion detection. An active lesion is one that is progressing, whereas an inactive lesion has been arrested (Table 2). Because dental caries follows a dynamic but not necessarily continuous process, an active non-cavitated lesion can be arrested or stopped and can often be reversed by a nonsurgical approach (Figure 3).4
The so-called “medical model” requires that practitioners differentiate the caries disease process and shift the focus from an operative approach—ie, one geared towards caries removal—to a preservation approach geared towards infection control, management, and remineralization. The ultimate goal of the medical model is to avoid irreversible tissue damage and the need for restoration. This article focuses on noninvasive caries management interventions using fluoride and non-fluoride agents for treating early active caries lesions, based on the most current body of evidence.
Fluoride Agents
The benefits of topical fluorides are firmly established, based upon a sizeable body of evidence from not only randomized controlled clinical trials but also systematic reviews. Most evidence strongly suggests that its preventive effect is topical, affecting the demineralization-remineralization exchanges between tooth structure and the surrounding environment.4 The size of the reductions in caries increment in both the permanent and primary dentitions emphasizes the importance of including topical fluoride delivered through toothpastes, rinses, gels, or varnishes in any caries preventive program.6
Patient-Applied Fluorides
The following patient-applied options are currently available:
• 1,000-ppm fluoride dentifrice. Fluoride toothpaste has been supported by more than a half century of research. Dentifrices containing 1,000 ppm fluoride and above have consistently shown caries reduction in children and adolescents.6,7
• 5,000-ppm fluoride dentifrice. Dentifrices with higher concentrations of fluoride (1.1% NaF or 5,000 ppm) should be considered for at-risk patients. The evidence supports that dentifrices with 5,000 ppm of fluoride are significantly better than dentifrices with 1,100 ppm of fluoride at remineralization of root caries lesions in adults.7,8
• Fluoride rinse. The use of fluoride mouth rinses (0.05% NaF) by at-risk children and adolescents is effective in reducing caries, even if they drink fluoridated water and use fluoridated toothpaste.9
Professionally-Applied Fluorides
The following clinician-applied options are currently available:
• Fluoride gel. The application of fluoride gel (1.23% APF) has been shown to decrease caries incidence in children and adolescents and reverse root caries lesions in adults, and should, therefore, be recommended for caries risk patients.10,11
• Fluoride varnish. The application of fluoride varnish (5% NaF) shows a substantial caries-inhibiting effect on both young permanent and primary teeth.12
Non-Fluoride Agents
Non-fluoride products are generally antimicrobials and remineralizing/arresting agents. They can be categorized as follows:
Dental Sealants
Sealing non-cavitated lesions can effectively reduce their progression and the numbers of microorganisms in them.13 Developing a barrier between the biofilm and the caries lesion leads to the arrest of the lesion.4 Currently, two main types of dental sealants are available: resin-based sealants and glass-ionomer sealants. There is a large body of evidence supporting the use of resin-based sealants for pit-and-fissure caries prevention in permanent molars of patients at risk.13 There is no clear benefit of using a glass-ionomer–based dental sealant over one that is resin based. Moreover, the evidence level is lower than for a resin-based sealant. Pit-and-fissure sealants have been used successfully not only to prevent caries but also to manage non-cavitated caries lesions.
Xylitol
Xylitol is non-cariogenic and has an antimicrobial effect that is dose and frequency dependent. Xylitol can be delivered in a wide variety of vehicles such as lozenges, chewing gums, and toothpastes. Consuming 6 to 10 g of xylitol gum three to four times a day reduces mutans streptococci in plaque and saliva in adults (aged 18 to 73 years).14 In accordance with an American Dental Association evidence-based review, daily use of (5- to 8-g) xylitol lozenges two to three times a day after meals may reduce the incidence of coronal caries in children aged 5 years or older.15 Although xylitol consumption may be effective on children, the X-ACT showed that the daily use of lozenges containing 3 to 5 g of xylitol does not reduce caries increment among adults (aged 21 to 80 years).16
Chlorhexidine Rinse
The premise behind using chlorhexidine is based on its antimicrobial effect. Using a chlorhexidine rinse (0.12%) has been shown to reduce plaque and mutans streptococci in saliva. However, studies did not show that rinsing with chlorhexidine rinse (0.12% to 0.2%) has a substantial effect on the preservation of sound tooth structure. Up to now, there is no strong evidence supporting the use of chlorhexidine rinses in reducing dental caries.15
CPP-ACP
Calcium-based strategies are founded on calcium’s remineralization potential. The current level of clinical evidence is not adequate to support the use of casein phosphopeptide-amorphous calcium phosphate (CPP-ACP) as an alternative remineralization strategy.17
Resin Infiltration
The aim of caries infiltration is to soak up the porous lesion body with a low-viscosity resin to create a diffusion barrier and arrest caries progression.18 Resin infiltration is indicated for treating active non-cavitated proximal and free-surface lesions. The current evidence is favorable and shows that resin infiltration reduces caries lesion progression in non-cavitated interproximal caries lesions extending radiographically into the inner half of enamel up to the outer third of dentin18,19 and active white-spot lesions on free surfaces.20
Restoration Placement
Caries lesions may be detected at a relatively late point of development. Cavitated lesions that limit regular dental plaque removal are likely to progress. Therefore, the appropriate treatment for these lesions is surgical removal and restoration placement. Minimally invasive principles should be used during caries removal and cavity preparation to preserve as much tooth structure as possible. Hence, the choice of restorative material should be based on the size of the lesion and the caries risk of the patient.
Conclusion
The current standard of care is based on patient-centered disease prevention and management before there is irreversible tooth damage and the need for surgical treatment and restoration placement. The practitioner has the task of diagnosing the caries lesions at an early stage and providing treatment based on the best evidence available.
According to the most current evidence, fluoridated toothpastes, other topically applied fluorides, and pit-and-fissure sealants, along with behavior and dietary improvement, remain mainstays of early caries management. Lesion infiltration is an emerging alternative for treating active non-cavitated proximal and free-surface lesions.
References
1. National Institute of Health Consensus Development Panel. National Institutes of Health Consensus Development Conference statement. Diagnosis and management of dental caries throughout life, March 26-28, 2001. J Am Dent Assoc. 2001;132(8):1153-1161.
2. Amaechi BT, van Amerongen JP, van Loveren C, Kidd EAM. Caries management: diagnosis and treatment strategies. In: Summit JB, Robbins JW, Hilton TJ, Schwartz RS. Summitt’s Fundamentals of Operative Dentistry: A Contemporary Approach. 4th ed. Hanover Park, IL: Quintessence Publishing Co.; 2013.
3. Featherstone JD. The caries balance: the basis for caries management by risk assessment. Oral Health Prev Dent. 2004;2(suppl 1):259-264.
4. Fontana M, Cabezas CG, Fitzgerald M. Cariology for the 21st Century: current caries management concepts for dental practice. J Mich Dent Assoc. 2013;
95(4):32-40.
5. International Caries Detection and Assessment System. ICDAS website. www.icdas.org. Accessed May 20, 2014.
6. Marinho VC, Higgins JP, Sheiham A, Logan S. Combinations of topical fluoride (toothpastes, mouthrinses, gels, varnishes) versus single topical fluoride for preventing dental caries in children and adolescents. Cochrane Database Syst Rev. 2004;(1):CD002781.
7. Walsh T, Worthington HV, Glenny AM, et al. Fluoride toothpastes of different concentrations for preventing dental caries in children and adolescents. Cochrane Database Syst Rev. 2010;(1):CD007868.
8. Baysan A, Lynch E, Ellwood R, et al. Reversal of primary root caries using dentifrices containing 5,000 and 1,100 ppm fluoride. Caries Res. 2001;35(1):41-46.
9. Marinho VC, Higgins JP, Logan S, Sheiham A. Fluoride mouthrinses for preventing dental caries in children and adolescents. Cochrane Database Syst Rev. 2003;(3):CD002284.
10. Marinho VC, Higgins JP, Logan S, Sheiham A. Fluoride gels for preventing dental caries in children and adolescents. Cochrane Database Syst Rev. 2002;(2):CD002280.
11. Wallace MC, Retief DH, Bradley EL. The 48-month increment of root caries in an urban population of older adults participating in a preventive dental program. J Public Health Dent. 1993;53(3):133-137.
12. Marinho VC, Worthington HV, Walsh T, Clarkson JE. Fluoride varnishes for preventing dental caries in children and adolescents. Cochrane Database Syst Rev. 2013;7:CD002279.
13. Ahovuo-Saloranta A, Forss H, Walsh T, et al. Sealants for preventing dental decay in the permanent teeth. Cochrane Database Syst Rev. 2013;3:CD001830.
14. Milgrom P, Ly KA, Roberts MC, et al. Mutans streptococci dose response to xylitol chewing gum. J Dent Res. 2006;85(2):177-181.
15. Rethman MP, Beltrán-Aguilar ED, Billings RJ, et al; American Dental Association Council on Scientific Affairs Expert Panel on Nonfluoride Caries-Preventive Agents. Nonfluoride caries-preventive agents: executive summary of evidence-based clinical recommendations. J Am Dent Assoc. 2011;142(9):1065-1071.
16. Bader JD, Vollmer WM, Shugars DA, et al. Results from the Xylitol for Adult Caries Trial (X-ACT). J Am Dent Assoc. 2013;144(1):21-30.
17. Zero DT. Recaldent—evidence for clinical activity. Adv Dent Res. 2009;21(1):30-34.
18. Paris S, Hopfenmuller W, Meyer-Lueckel H. Resin infiltration of caries lesions: an efficacy randomized trial. J Dent Res. 2010;89(8):823-826.
19. Meyer-Lueckel H, Bitter K, Paris S. Randomized controlled clinical trial on proximal caries infiltration: three-year follow-up. Caries Res. 2012;46(6):544-548.
20. Senestraro SV, Crowe JJ, Wang M, et al. Minimally invasive resin infiltration of arrested white-spot lesions: a randomized clinical trial. J Am Dent Assoc. 2013;144(9):997-1005.
About the Author
Juliana da Costa, DDS, MS
Associate Professor
Restorative Dentistry Department
Oregon Health & Science University
Portland, Oregon