Nonsurgical Instrumentation: An Update
Advances have improved operator comfort and patient care
Diseases of the periodontium are a common presenting feature among patients in general dental practice. With improvement in medical and oral health, the prevalence of edentulousness in the population is declining.1 As tooth loss becomes less common, the importance of prevention, diagnosis, and treatment of periodontal diseases will increase, while retention of teeth into old age will likely create new challenges in the maintenance requirements of patients.
Periodontal diseases are multifactorial, involving microbial infection in a susceptible host, influenced by immune and genetic factors. Bacteria play a crucial role in disease etiology and their removal represents the focus of much of the strategy for treatment of periodontal diseases. Accurate assessment plays a key role in determining diagnosis and selecting appropriate therapy.
The purpose of this article is to reflect on rationale for nonsurgical treatment of chronic periodontal disease and to address instrument selection for nonsurgical treatment, as well as considerations that potentially affect the effectiveness of such therapy in everyday practice.
Periodontal Probing
Before diagnosis and treatment decisions can be made, thorough evaluation of the periodontal tissues must be conducted. Evaluation includes various measures, chief of which is measurement of probing depths. Interpretation of clinical charting should account for the limitations of probing. Measurements of clinical pocket depth obtained with the probe don’t usually coincide with histologic pocket depth. Manual probing may present reproducibility and accuracy issues related to features such as probing technique, probing force used, probe tip design, angle of insertion, location, precision of probe calibration, and inflammatory status of the periodontal tissues.2
Of noted importance is the inflammatory status of the tissues. Mean probe penetration is greater with increased probing force and with increased gingival inflammation.3 Reproducibility of probing measurements varies among patients and with operator experience. Pocket depth and location, access, and visibility are all highly important for reproducibility of probing measurements.4 Large deviations in probing depth are more commonly noted at deep pocket sites and, while infrequent, are clinically significant and may lead to altered decision making in diagnosis and treatment. Despite the limitations associated with clinical measurements, probing depth measurement serves as a useful clinical marker for predicting the outcome of treatment and as a potential marker for deterioration of periodontal health.
A number of probing systems were developed in the 1980s and 1990s to attempt to address issues, such as difficulty of standardizing probing force, reducing human error and variability (eg, Florida Probe® system, Florida Probe Corporation, www.floridaprobe.com). The use of modified probe tip designs with a controlled-force technique may also offer the potential for improvement of comfort level of patients undergoing periodontal probing.
Among the limitations of electronic probing systems were cost and the need to accommodate advanced electronic components, which inevitably led to a more cumbersome design than the manual probe. Recent developments in electronic probing have focused on ease of use and ergonomics (eg, Dolphin handpiece, Florida Probe Corporation).
Rationale for Instrumentation
It is well established that plaque bacteria play a key etiologic role in development of gingivitis5 and in the pathogenesis of periodontitis.6 Subgingival plaque bacteria have been associated with periodontal disease progression, as measured by alveolar bone loss.7
Periodontal pathogenic species in plaque and calculus exist as part of a complex biofilm. Through removal of dental plaque and calculus and consequent disruption of plaque biofilm, instrumentation helps to create an environment in which reparative immune responses are encouraged and destructive processes negated. Disruption of the plaque biofilm and consequent reduction of bacterial load creates an altered gingival environment that favors growth of commensal species associated with gingival health. Consequently, one of the goals of periodontal therapy is to control potentially pathogenic organisms in plaque biofilm via instrumentation; this has been associated with significant improvements in the clinical and microbiologic parameters of periodontal diseases.8 Furthermore, a 30-year follow-up of patients in a private dental office9 indicated that a preventive program involving oral hygiene control and instrumentation could maintain periodontal health of patients with chronic periodontal disease.
The importance of prevention and the need to enhance the results of care delivered in the dental practice is put in context by the high prevalence of periodontal disease in the US population. Based on a sample of 3,742 adults participating in the first national survey to use a full-mouth examination protocol for diagnostic accuracy (NHANES 2009-2010), a prevalence of periodontal disease of 47.2% was estimated for US adults aged 30 years or older. Increased prevalence of disease was noted for Mexican American and African Americans, older individuals, smokers, men, and those with lower educational attainment and lower socioeconomic status.10
Nonsurgical Instrumentation and Instrument Selection
Given that therapy for bacterial removal is necessary/desirable to engender a healthy gingival environment, it is practical to address methods for achieving this goal along with their effectiveness. Most commonly, therapy will involve a primary phase of nonsurgical treatment, involving supra- and subgingival instrumentation and instruction in self-performed oral hygiene measures. It has been demonstrated that subgingival debridement performed in the absence of oral hygiene results in lack of improvement of clinical parameters and rebound of unfavourable microbial species within a short period of time.11 Similarly, improvement in oral hygiene alone, in the absence of subgingival debridement, results in a suboptimal clinical response.12 Instrumentation may account for most of the improvement seen at deep sites after therapy involving plaque control and instrumentation.12
Periodontal instrumentation involves two distinct practices: scaling, defined as the removal of plaque/calculus from supra-/subgingival enamel surfaces, and root debridement, or the removal of subgingival plaque and calculus from the periodontal pocket without the intentional removal of tooth structure. Although bacterial virulence factors, such as endotoxin, do attach to and penetrate cementum, removal is possible with conservative instrumentation.13 Consequently, aggressive removal of “diseased cementum” (“root planing”) for the purpose of elimination of bacterial endotoxin is no longer routinely recommended.14 However, this terminology persists in the nomenclature and everyday discussion of treatment approaches.
Nonsurgical Approaches
Nonsurgical instrumentation may be carried out using a variety of instruments, which may be broadly divided into hand instruments and powered instruments. Some of the key features of these instrument types are addressed in Table 1.
Hand instruments include scalers, chisels, files, and periodontal hoes, in addition to universal and area-specific curettes. Perhaps the most widely used hand instrument is the Gracey curette. These are designed for specific areas of the mouth and have an offset blade with one cutting or working edge. The blade is curved in more than one direction to enhance adaptation to the root surface. A full set comprises nine double-ended instruments, but most practitioners accomplish instrumentation with a smaller selection of instruments.
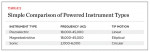
Both sonic and ultrasonic powered devices have been advocated for the removal of supra- and subgingival calculus. These instruments traditionally use water spray for irrigation but specialized tips also allow for antimicrobial agents to be used as irrigants. Differentiation of these instruments is primarily on the basis of vibration frequency.
Sonic scalers use air pressure to create mechanical vibration. The instrument tip responds by vibrating at a frequency between 2,500 and 16,000 Hz.15 Ultrasonic instruments are more commonly used and work on the principle of conversion of electrical to mechanical energy, resulting in high frequencies of vibration, disrupting plaque and calculus deposits. Water-cooling dissipates heat energy and may enhance debris removal, via the so-called “cavitation effect.” These instruments operate at frequencies between 18,000 and 45,000 Hz. Two types are recognized: magnetostrictive and piezoelectric.
Examples and key features of sonic and ultrasonic instruments are presented in Table 2.
It is recognized that efficiency of these instruments can significantly decrease in worn or shortened inserts. It is recommended to inspect inserts monthly for signs of wear; suppliers now generally provide instrument cards, whereby tip size can be measured against standardized reference diagrams to detect wear.
Potential hazards associated with use of powered instruments were reviewed by Trenter and Walmsley.16 Possible complications included the potential for thermal pulp damage; the authors concluded powered scaling should not be considered without irrigation, with a flow rate in the region of at least 20 to 30 mL/min. The authors found insufficient definitive information on the effects of cavitation activity in the cooling water on the hard tissues of the tooth, and the potential for handpiece vibration to affect operators with time, as seen in “vibration white finger” among pneumatic drill operators.16 Consensus indicates that these instruments should be used with low/medium power settings and with light force to avoid root damage.17 To decrease the hazards of aerosols, use of pre-procedural antiseptic mouthrinse (chlorhexidine 0.12%) and high-volume evacuation is recommended. It is prudent to consider hand instrumentation only in high-risk infective patients to reduce bacterial hazard of aerosol.16 Reports regarding the effect of ultrasonics in patients with pacemakers have been contradictory but it seems that any potential effects relate only to the magnetostrictive-type scalers. Although improved shielding of pacemakers may have negated much of this risk in recent years, it may still be prudent for practitioners to avoid use, or consult on use of magnetostrictive-type scalers in patients with pacemakers.16
Outcomes and Evaluation of Nonsurgical Therapy
Initial periodontal therapy, incorporating instrumentation and effective oral hygiene by the patient, is associated with expected decreases in bleeding and plaque levels, reduced probing depths, and improvement in periodontal attachment levels.4
A systematic review of the efficacy of machine-driven and manual subgingival debridement in treatment of chronic periodontitis did not disclose a significant difference between these modalities.18 The authors noted that most studies related solely to non-molar teeth and information on the effectiveness of machine-driven instruments on multi-rooted teeth was not available to enable comparison. Powered instruments were associated with a time advantage and no major difference in the frequency or severity of adverse effects between the modalities was found.
Research suggests that the amount of residual calculus and subgingival plaque is the same irrespective of whether a procedure has been performed using a hand instrument or an ultrasonic device.19 However, healing response to nonsurgical therapy for molar furcation sites is impaired relative to non-molar sites and molar flat surfaces.20 Molar furcations may also show a higher frequency of continued attachment loss following initial therapy.20
Removal of plaque virulence factors such as bacterial endotoxin is desirable but may be independent of complete calculus removal. Complete removal of subgingival calculus may not be predictably attainable following subgingival instrumentation.21 Small areas of calculus may be left behind and a significant number of surfaces may show residual calculus.21 Clinical success of treatment may be dependent on a “critical mass” of calculus rather than total elimination,13 although this does not negate the importance of removing the maximum amount of calculus possible. Agreement between examiners in detecting calculus after instrumentation is low.22 More calculus tends to be left behind on proximal surfaces, in deep sites, and in furcation areas.21
Waerhaug23 evaluated the effectiveness of subgingival instrumentation on a sample of “condemned” teeth and concluded that the chances of removing all subgingival deposits are high in pockets smaller than 3 mm. In pockets of 3 to 5 mm, the chances of failure are greater than success, and in pockets larger than 5 mm, the chance of failure to remove all deposits dominates. Furcation areas exhibit a complex and varying anatomy, and furcation entrances are often a dimension smaller than traditional curette tips.24 Access is consequently a key issue in providing effective treatment and has led to modifications in instrument design over time, particularly the development of smaller ultrasonic tips which may be favored as instruments of choice for furcation sites.19
Surgery has also been indicated for improved access for calculus removal and to address teeth with anatomical factors that limit effectiveness of root instrumentation eg furcations, root concavities, deep probing depths. A systematic review by Heitz-Mayfield and colleagues25 concluded that both scaling and root planing alone and open flap debridement are effective methods for treatment of chronic periodontitis. A series of longitudinal trials conducted at multiple centers from the late 1960s onward compared nonsurgical therapy with various surgical approaches. Analysis and interpretation of these studies is complicated by factors including differences in experimental design, treatment protocols, and methods of data collection. The effects of age and oral hygiene of subjects in these studies were also not consistently addressed. Overall, both surgical and nonsurgical approaches have been shown to result in similar mean improvements of clinical scores.19 Surgery may be more strongly indicated at deep pockets, where surgical therapy has been associated with greater pocket depth reduction and clinical attachment gain.25 Referral to a periodontist to determine if surgical therapy is necessary may be recommended if pockets >5 mm persist after instrumentation.
Many different intervals, ranging from 2 weeks to 6 months, have been advocated for performing re-evaluation.26 Based on a review of relevant studies, these authors suggested an ideal time for re-evaluation of 4 to 8 weeks post-therapy. This time allows time for re-establishment of junctional epithelium and connective tissue repair, but is likely to precede pocket repopulation by pathogenic bacteria as proposed by Magnusson and colleagues.11
Modifications/Adaptations
Nonsurgical instrumentation is an area for ongoing innovation among dental manufacturers with attention focused on improving operator comfort and efficiency of instrumentation.
Curettes and scalers have seen design modifications affecting handle, shank, and tip/blade.
-- Instrument handles. Handles have progressed toward use of wider, lighter weight handles with a more ergonomic design. Handles may be resin covered for a more comfortable grip (eg, elliptically shaped “cushion” grips) and may be textured for improved rotational control. These methods are claimed to reduce hand fatigue.
-- Instrument shank length. Elongated shanks may also allow improved access in deeper pockets (≥5 mm); positioning and fulcrum must be good to avoid over-stressing the instrument in use. Rigid Gracey curettes are more normally used for medium-to-heavy calculus removal. In these instruments, the shank diameter is fabricated to be thicker and less flexible than standard Graceys to reduce operator hand fatigue.
-- Instrument tip. Thinner, shorter blades have been produced for easier insertion, improved access, and control in deeper pockets (≥5 mm). Instrument tip materials may also be modified, such as that seen in EverEdge® Technology scalers and curettes from Hu-Friedy ( www.hu-friedy.com), which claims they stay sharper for longer than standard instruments and therefore require less time sharpening.
Many of the modifications in hand instrument design are now being incorporated into ultrasonics. Examples include the use of Swivel® inserts (Hu-Friedy), which remove the need to adjust magnetostrictive tips during use; longer grips for decreased hand fatigue; elongated tips for improved access; and the use of thinner, streamlined, and lightweight tips. Some powered scalers may also be fitted fiber-optic lighting for improved visual access during therapy.
Based on these designs, practitioners can adapt their periodontal instrument selection to design a personalized kit for provision of nonsurgical therapy. In addition to armamentarium for polishing and instrument sharpening, a simple kit might include the following (or equivalent):
-- Diagnostics: Double-sided mirror; periodontal probe (UNC-12); calculus explorer (ODU 11/12); nabers furcation probe
-- Supragingival scalers: Anterior sickle; universal
-- Gracey curettes: Anterior mini (1/2); cuspid/bicuspid/flat-surface (5/6); distal surface posterior (13/14); mesial surface posterior (15/16)
-- Ultrasonic inserts: Standard insert; slimline straight; slimline left- and right-curved
Instrument Sharpening
Efficiency and ease of use of hand instruments depends on sharpness of the working blade. This can be maintained through use of polishing stones, whose surface is made of abrasive crystals harder than the metal being sharpened. After use, instruments should be inspected for damage. Lubrication (eg, orange solvent) should be used before sharpening to decrease clogging of the abrasive surface from metal particles.
Correct sharpening technique may differ depending on the type of hand instrument selected (eg, scaler or curette) and is consequently technique sensitive. Blunt/incorrectly sharpened instruments may lead to ineffective calculus removal and may result in excessive forces being applied to the root surface, and a danger of metal fatigue or fracture as well as risk of excessive tooth surface removal. To facilitate the process, machined sharpening tools have been developed. Instruments are held in a set position against a mechanized sharpening wheel/blade, removing the need to calculate sharpening angles and speeding the process. Examples include: Rx System II Periodontal Set (Rx Honing Machine Corporation, www.rxhoning.com) and the Sidekick® Sharpening Kit (Hu-Friedy). These tools may hold particular value when sharpening duties are designated within a practice and in practices with high turnover of periodontal/maintenance patients.
Implant Maintenance
Appreciation of the potential for peri-implant and bone loss has increased in recent years with the knowledge that this may be a relatively common occurrence.27 Discussion of treatment approaches for treatment of peri-implant disease is beyond the scope of this paper. In brief, recent years have seen a variety of products developed, largely based on prevailing thought in the dental profession at the time. This has included indications for use of standard metal curettes/scalers, plastic and titanium curettes of varying hardness, and modified ultrasonic tips (sleeves). There is not clear consensus on a “gold standard” treatment regimen/instrument selection, and peri-implant disease is largely managed on a case-by-case basis. For peri-implantitis cases, assessed with peri-implant bone loss, referral/consultation with a periodontist may be prudent.
Conclusion
Nonsurgical instrumentation remains a key treatment approach for management of periodontal diseases. Hand instruments and powered devices are not mutually exclusive, but rather complement each other. Combining the advantages of both methods produces an optimal result and enables the operator to work ergonomically. While the rationale underpinning nonsurgical treatment and approaches to therapy has not changed significantly in recent years, clinicians should be aware of the variety of modifications made to improve the comfort and efficiency of the operator.
References
1. Hugoson A, Sjödin B, Norderyd O. Trends over 30 years, 1973-2003, in the prevalence and severity of periodontal disease. J Clin Periodontol. 2008;35(5):405-414. doi: 10.1111/j.1600-051X.2008.01225.x.
2. Robinson PJ, Vitek RM. The relationship between gingival inflammation and resistance to probe penetration. J Periodontal Res. 1979;14(3):239-243.
3. Larsen C, Barendregt DS, Slot DE, et al. Probing pressure, a highly undervalued unit of measure in periodontal probing: a systematic review on its effect on probing pocket depth. J Clin Periodontol. 2009;36(4):315-322.
4. Badersten A, Nilveus R, Egelberg J. Effect of nonsurgical periodontal therapy. II. Severely advanced periodontitis. J Clin Periodontol. 1984;11(1):63-76.
5. Loe H, Theilade E, Jensen SB. Experimental Gingivitis in Man. J Periodontol. 1965;36:177-187.
6. The pathogenesis of periodontal diseases. J Periodontol. 1999;70(4):457-470.
7. Grossi SG, Genco RJ, Machtei EE, et al. Assessment of risk for periodontal disease. II. Risk indicators for alveolar bone loss. J Periodontol. 1995;66(1):23-29.
8. Haffajee AD, Cugini MA, Dibart S, et al. The effect of SRP on the clinical and microbiological parameters of periodontal diseases. J Clin Periodontol. 1997;
24(5):324-334.
9. Axelsson P, Nyström B, Lindhe J. The long-term effect of a plaque control program on tooth mortality, caries and periodontal disease in adults. Results after 30 years of maintenance. J Clin Periodontol. 2004;31(9):749-757.
10. Eke PI, Dye BA, Wei L, et al; CDC Periodontal Disease Surveillance workgroup. Prevalence of periodontitis in adults in the United States: 2009 and 2010. J Dent Res. 2012;91(10):914-920.
11. Magnusson I, Lindhe J, Yoneyama T, Liljenberg B. Recolonization of a subgingival microbiota following scaling in deep pockets. J Clin Periodontol. 1984;11(3):193-207.
12. Cercek JF, Kiger RD, Garrett S, Egelberg J. Relative effects of plaque control and instrumentation on the clinical parameters of human periodontal disease. J Clin Periodontol. 1983;10(1):46-56.
13. Cobb CM. Non-surgical pocket therapy: mechanical. Ann Periodontol. Nov 1996; 1(1):443-490
14. Nyman S, Sarhed G, Ericsson I, et al. Role of “diseased” root cementum in healing following treatment of periodontal disease. An experimental study in the dog. J Periodontal Res. 1986;21(5):496-503.
15. Van Der Weijden, F. In: The Power of Ultrasonics. 2nd ed. Paris, France: Quintessence International; 2007.
16. Trenter SC, Walmsley AD. Ultrasonic dental scaler: associated hazards. J Clin Periodontol. 2003;30(2):95-101.
17. Arabaci T, Ciçek Y, Canakçi CF. Sonic and ultrasonic scalers in periodontal treatment: a review. Int J Dent Hyg. 2007;5(1):2-12.
18. Tunkel J, Heinecke A, Flemmig TF. A systematic review of efficacy of machine-driven and manual subgingival debridement in the treatment of chronic periodontitis. J Clin Periodontol. 2002;29 suppl 3:72-81; discussion 90-91.
19. Claffey N, Polyzois I, Ziaka P. An overview of nonsurgical and surgical therapy. Periodontol 2000. 2004;
36:35-44.
20. Nordland P, Garrett S, Kiger R, Vanooteghem R, Hutchens LH, Egelberg J. The effect of plaque control and root debridement in molar teeth. J Clin Periodontol. 1987;14(4):231-236.
21. Egelberg J. Periodontics. In: The Scientific Way: Synopses of Clinical Studies. 3rd ed. Malmo, Sweden: OdontoScience; 1999.
22. Sherman PR, Hutchens LH Jr, Jewson LG, et al. The effectiveness of subgingival scaling and root planning. I. Clinical detection of residual calculus. J Periodontol. 1990;61(1):3-8.
23. Waerhaug J. Healing of the dento-epithelial junction following subgingival plaque control. II: As observed on extracted teeth. J Periodontol. 1978;49(3):119-134.
24. Bower RC. Furcation morphology relative to periodontal treatment. Furcation entrance architecture. J Periodontol. 1979;50(1):23-27.
25. Heitz-Mayfield LJ, Trombelli L, Heitz F, et al. A systematic review of the effect of surgical debridement vs nonsurgical debridement for the treatment of chronic periodontitis. J Clin Periodontol. 2002;29 suppl 3:92-102; discussion 160-162.
26. Segelnick SL, Weinberg MA. Reevaluation of initial therapy: when is the appropriate time? J Periodontol. 2006;77(9):1598-1601.
27. Zitzmann NU, Berglundh T. Definition and prevalence of peri-implant diseases. J Clin Periodontol. 2008;35(8 Suppl):286-291. doi: 10.1111/j.1600-
051X.2008.01274.x.
About the Authors
Peter L. Harrison, BDentSc, DChDent
Department of Periodontology, University of Florida
College of Dentistry, Gainesville, Florida
Rodrigo Neiva, DDS, MS
Department of Periodontology, University of Florida
College of Dentistry, Gainesville, Florida