A Restorative Option for the Dreaded Black Triangle
Specialized composite technique yields predictable and esthetic results
In the dental office, patients often hesitate to mention esthetic problems that cause them personal embarrassment. However, dentists who focus on esthetics have removed some of these barriers by initiating dialogues about issues like dark teeth and crowded teeth. In turn, this has given patients permission to ask questions and talk about their esthetic treatment options. Therefore, in the past 20 years we have seen a dramatic increase in the amount of esthetic treatments such as porcelain veneers, whitening of teeth, and adult orthodontics.
One very significant esthetic dilemma, the dreaded “black triangle,” has not received the same attention from our profession. This is despite the fact that the magnitude of the problem is substantial, considering that 30% of adults suffer from black triangles resultant from multiple etiologies.1-5 Moreover, a recent study found that patients rated black triangles as their third most disliked esthetic problem, following caries and dark crown margins.6 The surprise is that the study discovered that in the patient’s mind, black triangles were actually a bigger esthetic dilemma than crowded teeth or dark teeth.
It may be that dentists have not initiated dialogues with patients about the black triangle because its treatment has historically not been a part of mainstream dentistry. It may also be because dentists had very little confidence that it could be treated successfully. Because we now know that black triangles are in fact a primary concern for patients, it is the author’s hope that this article will help dentists gain confidence in the restorative/composite option as a predictable and healthy solution for treating black triangles.
Traditional Treatment
Following the publication of a few articles and the posting of a YouTube video regarding black triangles, the author heard from patients who felt that the solutions that had been proposed to them in the past, such as full crowns, porcelain veneers, or stripping of the teeth and pushing the teeth together, were extremely aggressive. Many of these patients felt that their dentists were very uncomfortable with the use of direct composite because of all the problems we have seen historically from the use of composite to try to close a black triangle. Indeed, even the phrase “close a black triangle” gives us a bit of a clue of why this procedure has failed in the past, both biologically and esthetically.
In the past, traditional restorative closure of the black triangle consisted of “pattycaking” a wing of paste composite from the facial aspect to essentially block the light. This decreased the amount of blackness in the interdental area, but led to multiple new problems, including staining, debonding, periodontal inflammation, and food impaction, among others.
Rethinking Our Approach
The brevity of this article precludes a comprehensive approach to this topic, but an abbreviated formula for success will be presented.
Use an Anatomic Matrix
A flat piece of Mylar has been the only matrix clinicians have had until recently. A new system of matrices, the Bioclear Matrix System (www.bioclearmatrix.com), has patented both the shape of the matrices and the resultant papilla regeneration process that occurs with their use. Implants, porcelain laminates, and crowns sometimes have aggressively curvaceous emergence profiles that are needed to close spaces along the gingival margin of these prostheses. When well planned, fitted, and smooth, the tissue response can be both dramatic and healthy. In the case presented below, both the anterior (with 0.7 mm of cervical profile) and the diastema closure (with 1 mm of cervical profile) were mixed and matched for the variety of spaces that were present.
Use Tips in Smaller Sizes
When injecting composite, using a smaller tip size enables the clinician to get composite into the small tooth-matrix interface. The initial composite to be placed, an esthetic flowable composite, is injected first with a size 20 gauge tip, and is considered the “wash” component. A “body” paste composite is then injected directly into the “wash” of flowable composite that was placed first but not light cured. This is similar to using light body and then heavy body impression material together.
Heat the Composite to 155°F
Composite manufacturers do not have official statements regarding heating of composites, but multiple studies7,8 have shown that heating composite to a temperature of 155°F improves flow, reduces microleakage, and aids in polymerization. However, mainstream dentistry has not been compelled to move to heated composite. Most clinicians have shied away from this heating (liquefaction of composite), as they simply did not see enough benefit. Today, however, we are learning that to integrate injection molding for procedures like the black triangle, heated composite has overwhelming benefits.
Heating of paste composite creates more microscopic vibration or movement of the molecules, allowing for improved flowability. This temporary liquefaction of paste composite is a welcome advancement in the placement of resin restorations. We clinicians are moving away from layering packing and stacking, and toward injection of a single load of composite. For the paste restorative used in this case, the author recommends heating to 155° to improve flowability. This technique can even be used with the flowable formula. The advantage of using this particular composite with heat is that the material can be used in both the posterior and anterior. Heating of the flowable is helpful because of the small space.
There is a reason that some of the “original masters” such as Dr. Paul Belvedere made their own flowable composite by mixing bonding resin and paste. Dentists need flowable composite, but not weak composite. Therefore using a flowable composite from a trusted manufacturer, and heating the composite while using it with a smaller tip can be a great help.
Change Your Mindset
The old school of dentistry thinks of paste composites as “packable.” In this way of thinking, the dentist is battling the composite to “pack” it into a preparation. However, the modern approach is a hydraulic driven model that uses injection molding and different viscosities of composites, allowing the composite to do the work.
Create an Infinity Edge Preparation
The traditional model of tooth preparation is to cut a box, which is supposed to have a clean margin at which composite will cleanly stop. When you inject composite into such a preparation, it naturally flows over the sides. The traditional method of dealing with this has been to polish the composite back to the margin line. However, in the technique described here, the approach is to “sand” the whole tooth and let the composite flow all around it. This is referred to as an infinity edge margin, which is thinner and thinner until it disappears, and provides both strength and esthetics. Practitioners should think in terms of a tooth-restoration interface, or TRI. This TRI is an area from 0.5 to 2 mm of lightly abraded and then etched enamel, which embraces composite’s tendency to flow past the old-fashioned notion of a clean margin.
Mix Flowable and Paste Composite with Injection Molding
Unfortunately, much of the focus for composite choice and use in black triangles has historically not helped dentists or patients achieve better outcomes. Often the focus has been on layering and translucency, and these issues for the most part distract the clinician from the real problems and real solutions available.
A better method involves using flowable composite and paste composite mixed with injection molding in a modified snowplow technique.9,10 The author’s recommended composites for treatment of black triangles are Filtek™ Supreme Ultra Universal Restorative (3M ESPE, www.3mespe.com) in a body shade and Filtek™ Supreme Ultra Flowable Restorative. These composites come in enamel, body, and dentin shades. The enamel is quite translucent and in general the author recommends avoiding these shades unless restoring the incisal edge of a tooth. On the other hand, the dentin shades are typically too opaque for this purpose. Therefore, the body shade becomes the go-to composite.
There are many factors to consider in the treatment of black triangles, but with these composites, combined with the infinity edge margin design, shade matching and translucency are not concerns. 3M ESPE’s flowable shades match the body composite. For treatment of the gingival half of the tooth, the author almost exclusively uses body shade composites, so it is fortunate that 3M ESPE has elected to use the body shade to match their flowable composites, and we find an excellent and invisible interface between the color and opacity of Filtek Supreme Ultra Flowable Restorative and Filtek Supreme Ultra Universal Restorative. This simplification in shade matching is a welcome asset for this challenging treatment of black triangles.
The choice of composites is important because of the need to have confidence in the final restoration’s invisibility and the matching shades of the flowable and paste composites. Due to high filler content and robust characteristics of these restoratives1, the small percentage of flowable composite combined with the paste composite in this technique has provided very robust and esthetically pleasing restorations. The author has treated hundreds of black triangle cases this way and this method has been taught to thousands of dentists thus far with remarkable success.
Case Presentation
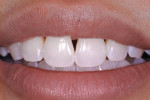
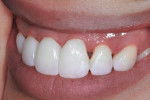
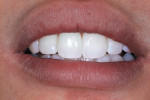
The patient featured in this article is a young professional who read about the author’s technique and within a week flew across the country for treatment (Figure 1). The patient had a beautiful smile, which in her perception was marred by black triangles. The principles described above were used to treat this case.
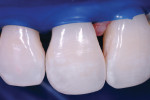
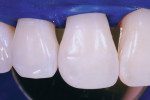
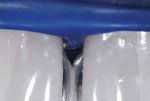
A rubber dam was placed prior to beginning the treatment. This heavy latex rubber dam (Hygenic Corporation, www.hygenic.com) serves a compressive purpose during the treatment. Figure 2 shows how the papilla between No. 7 and No. 8 was nicely compressed, but where the dam was torn the papilla between Nos. 8 and 9 presented as a problem. Figure 3 shows a new rubber dam in place. These images are shown to demonstrate how key placement of a heavy rubber dam can be to manage soft tissue.
The diastema closure matrices are available in multiple sizes; the smaller matrix was used for the distal of the lateral incisor. Generally, one space at a time is closed on the upper arch. This would entail, for example, a matrix on the distal of No. 8 and the mesial of No. 9.
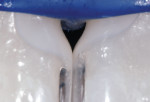
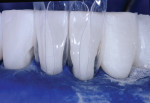
The heart of the process is the shape and smoothness of the matrix coupled with the injectability of ideal composites (Figure 4 and Figure 5). The matrix is partially teased open with the tips of the syringes of both flowable and paste composites, and then the matrix springs closed upon removal of the composite syringes. Figure 6 shows the case at a midpoint at which the rubber dam was removed for the patient to take a break.
Another key to success in the restorative option of treating black triangles is the diversity of shapes and sizes of the Bioclear Matrix. Lower incisor teeth are small. The miniscule lower incisor matrices are crucial when treating the lower arch (Figure 7).
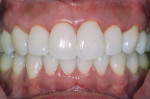
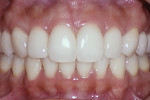
The immediate postoperative photo (Figure 8) shows instant remodeling of the gingiva with static tension of the appropriately formed composite surface. This immediate formation of a papilla is gratifying and will assure both the clinician and patient that the case will be successful (Figure 9 and Figure 10).
Discussion
The postoperative photos show that it is virtually impossible to tell where the composite starts and ends. No delineation between the flowable and paste composite is visible, and the incredible polish of the composite material and curvature of the Bioclear matrices together have created an ideal tissue response, as evidenced by the pink tissue and stippling that we see all the way to the tip of the papilla. If the tissue is pink and the surface is stippled, the tissue is healthy.
Using this technique, the composite is allowed to flow onto a completely blasted and etched tooth, and the featheredge margins allow the composite to cover approximately 60% of the native enamel. This 60% to 80% coverage that we typically see with the injection molding technique is a far cry from the little wing of composite pattycaked from the facial aspect. This dramatic change in the philosophy of integration of the composite, along with true papilla regeneration, completely changes the whole equation. The restorations are smooth, the tissue is healthy; there is no marginal staining and there is no food impaction.
The author adheres to a very strict protocol for this treatment, which allows the confidence to guarantee it to patients against stain and debonding for at least 10 years. This is based on two factors. First, the restorations are out of occlusion; and second, the author has dramatically shifted the enamel/dentin ratio of bonded surfaces. With the large volume of blasted and etched enamel that is engaged with the infinity edge margin, readers should have high confidence that they too can achieve similar success if the protocol is followed carefully. We trust enamel bonding and this technique shifts the dependence away from dentin bonding toward enamel bonding.
Conclusion
The black triangle is a situation in which there is not a traditional prep with a margin, which is one of the reasons it has been so challenging for dentists to treat. However, the lessons learned from optimal black triangle treatment—which can be summarized as long, thin infinity edge margins, balanced use of appropriate flowable and a creamy paste composite, and dedicated diastema closure Bioclear matrices—can be leveraged to create better, stronger, more esthetic restorations for every composite treatment, whether it be a Class I, II, III, IV or V—or this new class, which is additive dentistry.
One of the wonders of clinical practice is that we are presented with difficult situations in which no clean process has been developed. Clinicians must be creative, and from these struggles we often reach incredible discoveries that unlock possibilities across a much broader spectrum of problems than those presented in the original challenge that drove us to the necessity of invention.
The last and most important portion of this summary is the patient’s response 6 months after the procedure: “I feel like I’m a new person. My confidence is higher and my self-esteem is improved. It has made a huge impact on my life.”
Disclosure
Dr. Clark is the founder of the Bioclear Matrix System.
References
1. Tarnow DP, Magner AW, Fletcher P. The effect of the distance from the contact point to the crest of bone on the presence or absence of the interproximal dental papilla. J Periodontol. 1992;63(12):995-996
2. Holmes CH. Morphology of the interdental papillae. J Periodontol. 1965;36(6):455-460.
3. Kurth J, Kokich V. Open gingival embrasures after orthodontic treatment in adults: prevalence and etiology. Am J Orthod Dentofacial Orthop. 2001;120(2):116-123.
4. Ko-Komura N, Kimura-Hayasi M, Yamaguchi M, et al. Some factors associated with open embrasures following orthodontic treatment. Aust Orthod J. 2003;19(1):19-24.
5. Clark DJ, Kim J. Optimizing gingival esthetics; a microscopic perspective. Oral Health. 2005;April:116-126.
6. Cunliffe J, Pretty I. Patients ranking of interdental “black triangles” against other common esthetic problems. Europ J Pros Rest Dent. 2009;17(4):177-181.
7. Choudhary N, Kamat S, Mangala T, Thomas M. Effect of pre-heating composite resin on gap formation at three different temperatures. J Conserv Dent. 2011;14(2):191-195.
8. Daronch M, Rueggeberg F, Moss L, de Goes MF. Clinically relevant issues related to preheating composite. J Esthetic Restor Dent. 2006;18(6):340-350.
9. Clark DJ. Restoratively driven papilla regeneration. Can J Rest Dent Pros. 2008;Aug:40-46.
10. Clark DJ. The injection-molded technique for strong, esthetic Class II restorations. Inside Dentistry. 2010;6(1):68-76.
About the Author
David J. Clark, DDS
Private Practice
Tacoma, Washington