Porcelain Onlays and CEREC® CAD/CAM
Technology removes the barriers to indirect restorations
What is an onlay? For some time, there has been a controversy about this question that caused confusion about the subject among practitioners. The official definition from the American Association of Dental Consultants is as follows:
An onlay is an indirect restoration (fabricated outside the oral cavity) that covers one or more cusps, extending through and beyond the cusp tip to the facial/lingual and proximal slopes of the covered cusps. It may be fabricated from any of the materials used for inlay restorations. It is implicit in this type of restoration that occlusion in all functional positions is supported by restorative material rather than the tooth structure of the covered cusps.1
In the past, using porcelain for intracoronal restorations was not particularly successful, mostly because of the lack of an effective cementation medium. The ability to etch porcelain with hydrofluoric acid, with the resulting bonding effect of composite resin to enamel and dentin, has made intracoronal restoration an ideal option compared with the compromises faced with amalgam, gold, direct composites, and full-coverage restorations.
Benefits of Porcelain Onlays
Studies have showed that compromised teeth restored with resin-bonded, etched porcelain developed strength and resistance to fracture equal to—and in some cases exceeding—that of unrestored teeth, with the added benefit of reduced microleakage.2
Accordingly, porcelain onlays are indicated in cases with large carious or traumatic lesions with enamel that is undermined to the extent that a full-coverage restoration becomes a necessity. The resin-bonded porcelain restoration will hold the remaining tooth structure and prevent further breakdown. When metal allergy is a factor, the bonded all-ceramic restoration is the alternative of choice.
In addition, cases in which it is difficult to attain a proper retention form may often be restored by taking advantage of the adhesive nature of the bonded restoration, as opposed to using more aggressive means of establishing retention, such as periodontal surgical crown lengthening or elective root canal treatments with post and core build-ups.
In addition, the option of the porcelain resin-bonded restoration is very attractive because of its advantages in terms of shade matching, inertness to the surrounding periodontal tissues (as porcelain’s polished surfaces accumulate less plaque than others), and resistance to wear.
Barriers to Use for Practitioners
Even with all these advantages, it is the author’s experience that porcelain onlay restoration is under-diagnosed by a lot of general practitioners. This may be due to the fact that more than one visit is required to prepare the cavity, take the impressions, and deliver the final restoration. Other factors that are potential barriers to the use of porcelain onlays include the time lapse in the laboratory between the preparation day and delivery date, the fabrication fees from the laboratory that are incurred, and the possibility of the emergency visits due to problems arising from the temporary restoration, which can add to the chair time needed and thus to the total cost of treatment. Pressure from patient time restraints is a reason why some clinicians choose direct restorations, but in cases with large carious or traumatic lesions, these eventually fail due to the size of the cavity or the stresses experienced that surpass the material’s physical properties.
Removing Barriers
Six years ago, the author was introduced to the CEREC® (Sirona, www.sirona.com) CAD/CAM system, which made it possible to overcome the two main disadvantages of indirect restorations: time and cost. After implementation, patient case acceptance and retention dramatically increased. This was because they could have a highly esthetic and durable restoration, whether an onlay, inlay, or a crown, in a single visit, without the need for messy impression taking or temporaries.
Digital imaging reduced the dimensional changes that can occur through the process of impression taking and casting the models, and this led to a more accurate final product. Postoperative complications were reduced, leading to increased patient satisfaction and improved cost control.
Case Example
A 36-year-old man who works in the police force presented with a fractured disto-lingual cusp of tooth No. 2 and a stress crack on distal marginal ridge (Figure 1) that occurred due to a blow to his face while restraining a person who was resisting arrest. He complained of feeling sharp edges and experiencing sensitivity to cold while drinking and even while breathing. The patient requested a temporary fix because he was tight on time.
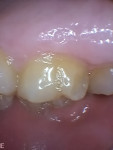
After examination, the author recommended a porcelain onlay and advised the patient that the treatment could be completed within the hour, which he readily accepted. The tooth was numbed, prepared, and imaged, and the onlay was milled, tried in, polished, and bonded all in approximately 45 minutes (Figure 2). The patient was very happy with the efficient, predictable, and esthetically pleasing outcome.
Conclusion
CAD/CAM allows for the fabrication of porcelain onlay restorations that are clinically superior in many situations; it also provides greater time efficiency and cost control benefits. In the author’s office, 90% to 95% of restorations currently performed are completed with CAD/CAM technology. It has been major financial advantage for the practice, taking lab costs down to an average of 3.9% at the end of 2012 and increasing patient satisfaction.
References
1. American Association of Dental Consultants Positions Committee. Position paper: defining and differentiating inlays and onlays. Paper presented at: AADC Annual Spring Workshop; May 2008; Scottsdale/Fountain Hills, Ariz.; 2008.
2. Saridag S, Sevimay M, Pekkan G. Fracture resistance of teeth restored with all-ceramic inlays and onlays: an in vitro study [published online ahead of print February 7 2013]. Operative Dentistry in-press. doi: https://dx.doi.org/10.2341/12-211-L.
About the Author
Rami G. Dimitri, DDS, FAGD, FICOI
Private Practice
Mira Loma, California