Adhesive Cementation Redefined
Options abound, but versatility, ease of use, and high bond strength remain key
NOTE: Since this article was published, 3M has removed the crown indication for Lava™ Ultimate CAD/CAM Restorative. The product continues to be indicated for inlays, onlays (with an internal retentive design element), and veneer restoratives, per new instructions for use.
A great deal of attention is now being given to bypassing the traditional cements in the adhesive placement of indirect restorations. Traditional cements such as zinc phosphates, polycarboxylates, and resin-modified glass ionomers have served the profession well and will continue to be used. With the increasing usage of non-metal alternatives and the clinician’s desire to reduce the incidence of micro-leakage, however, adhesive resin cements will continue to grow in popularity.
Advantages of Adhesive Cements
Traditional cements have weak to nonexistent adhesive capacity, are soluble in the presence of fluids, have low compressive strengths, and cannot withstand wear in exposed marginal gaps such as cavosurfaces. Criteria for their success are dependent on the fit of the restoration, especially with respect to margin gaps, for which acceptable values of less than 100 µm have been described as early as 1966.1 The better the marginal adaptation, the more protected the cement, enhancing long-term outcomes. Traditional cements are generally dispensed as powder/liquid formulations requiring accurate dispensing and mixing, although some delivery systems now include auto-mix two-paste syringe formulations. They are commonly used for bridges, crowns, onlays, and inlays of all-metal or metal substructures and for the crystalline ceramic materials such as zirconia and alumina.
Compared with traditional cements, adhesive resin cements offer the distinct advantage of being able to create strong mechanical and chemical bonds to the tooth and restoration.2 Being generally insoluble, they will provide better resistance to leakage than the traditional cements. Filled with silica and zirconia particles of varying micron and submicron sizes, they also have the capacity to withstand wear in exposed margins such as onlays and inlays in the cavosurface areas.3 Lastly, being inherently adhesive chemically, they offer a level of confidence where retentive preparation aspects are not employed or cannot be obtained to assure that the restoration cannot be dislodged.
Adhesives and New Restoration Materials
Many laboratories are reporting that the majority of their single-unit crowns are now metal free, with the trend expected to continue. The replacements for metal in these restorations comprise varying substrates, including silica-based glasses (feldspathic, leucite reinforced, and lithium disilicate), resin-based composites, polymer-based ceramics, and structural metallic oxide ceramics (alumina and zirconia). In many to most cases, adhesive resin cements are being utilized for their placement.
Restorations made of the silica-based glasses, composites, and polymer-based ceramics are dependent on adhesion chemistry for support and improved strength, which traditional cements cannot provide. Some categories of ceramic materials are inherently brittle, and traditional cements are too weak compressively to support them adequately under load. Adhesion to these materials is achieved through micro-mechanical retention using hydrofluoric acid to dissolve some of the glass matrix to allow for infiltration of the resin cement or with mechanical surface abrasion using micron-sized aluminum oxide. In both cases, a separate chemical coupler such as silane must be employed to create covalent chemical bonds between the ceramic and resin cement interfaces. The silica-based ceramics also have varying levels of translucency and require cements that can be shaded in applications for veneers and thin-walled crowns. As the adhesive resin cements are technically composite resins with lower filler content to make them flow, they can be similarly shaded and used to influence the final outcome esthetically.
It is well established in the literature that the long-term success of these ceramic materials is directly attributed to adhesive placement, whether they are fabricated chairside (eg, CEREC®, Sirona Dental Systems, www.sirona.com)4,5 or through the dental laboratory (eg, Empress®, Ivoclar Vivadent, www.ivoclarvivadent.com) using materials such as VITA® VITABLOCS® Mark II (Vident, www.vident.com), IPS Empress® CAD and IPS e.max® CAD (Ivoclar Vivadent), and 3M™ Paradigm™ MZ100 (3M™ ESPE™, www.3mespe.com).6 With today’s renew-
ed interest in more minimally invasive treatment using non-metal alternatives, preparation forms lacking the traditional elements for retention can be employed, conserving precious tooth structure through the use of this class of materials in conjunction with these adhesive cements.
The structural metal oxide ceramics are also seeing rapid market growth (eg, Lava™ Zirconia, 3M ESPE; BruxZir®, Glidewell Laboratories, www.glidewelldental.com) for restorations, copings, frameworks, and implant abutments. Zirconia is an exceptionally strong material with a very high flexural strength and, like metal, a traditional cement can be employed for its placement. Preparation requirements for zirconia are for all practical purposes identical to those of metal, in that traditional retention and resistance forms must be achieved through the use of specific geometries, wall tapers should not exceed 8 to 10 degrees, and wall heights should equal or exceed 3 mm.7
However, a legitimate need for adhesion to zirconia exists when these retentive preparation parameters cannot be achieved for the tooth or implant, whether through error or intent. Unlike the silica-based glasses, the dense and glass-free crystalline structure of zirconia will not permit acid-etching or air abrading with aluminum oxide, making micromechanical retention impossible. Any level of adhesion to zirconia therefore must be achieved with a chemical approach, using acidic primers to create chemical bonds.
Understanding the Options
A wide variety of adhesive cement products exists today, with products differing considerably in terms of ease of use, application in certain clinical situations, and clinical performance. Due to the wide variety of needs dentists have when true adhesion is desired, many practitioners are forced to carry multiple product lines along with the required additional chemical products. Because of the myriad chemical intricacies of these products, it is next to impossible to predict all of the possible interactions between any given adhesive and cement; therefore, it is typically recommended to simply follow the manufacturer’s instructions regarding which products can be used in combination. This is especially the case with dual-cure cements and adhesives. Given the differences in materials and adhesives, it is no wonder that many dentists have a sense of confusion, making bonding relatively complex and cost inefficient.
One potential solution for this complexity is presented by a recently introduced adhesive resin dental cement, RelyX™ Ultimate Adhesive Resin Cement (3M ESPE), which is specifically designed to be used with Scotchbond™ Universal Adhesive (3M ESPE),
a single-component or “one-bottle” system designed for adhesion to virtually all materials and tooth substrate.8,9 Studies show that the cement has exceptional marginal integrity regardless of etch mode (total, self, or selective). Further studies also indicate its resistance to staining when exposed to coffee incubation, which is critical to the maintenance of restorations placed along the smile line.10,11
With the use of these ceramic-based materials now firmly established and growing, adhesive resin cements are garnering much interest and attention. Understanding their correct use and technique helps ensure marginal seals that are highly resistant to leakage, preventing the ingress of fluids and bacteria to prevent recurrent decay and retain the restoration for its intended life.
Case Report
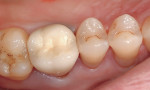
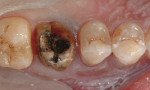
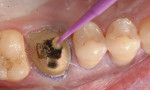
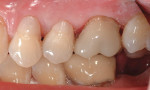
A patient presented for replacement of an 18-year-old porcelain-fused-to-metal crown due to suspected recurrent caries as a result of marginal leakage (Figure 1). A barrier was placed that remained throughout the entire procedure (Isolite, Isolite Systems, www.isolitesystems.com). The existing crown was sectioned and removed, with existing caries noted with evident leakage (Figure 2). Caries were removed and the preparation completed. A chairside computer-assisted design/computer-aided manufacture system was employed (CEREC® AC, Sirona Dental Systems) for the digital impressioning and subsequent fabrication of a replacement crown using a nano-ceramic block material (Lava™ Ultimate Restorative, 3M ESPE) with a filler load of 80% nano-clustered zirconia 4 to 11 nm and silica 20 nm in a polymer matrix. Using a proprietary process, this material exhibits a high flexural strength of 200 MPa, which is significantly higher than aluminous porcelains used for veneering purposes. It is also higher than chairside feldspathic and leucite-reinforced glass ceramics, making it an alternative choice where oven glazing is not desired and intraoral repair may be necessary at a later time.
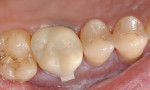
A selected shade A3 Lava Ultimate restorative was milled by the CEREC® MCXL milling unit and the crown was dry fitted to the preparation to verify fit (Figure 3). The intaglio of the restoration was air braded using CoJet Sand 30 µm (3M ESPE) to improve adhesion mechanically and chemically (50 µm aluminum oxide alternatively) per the manufacturer’s instructions for proper surface treatment of Lava Ultimate. The crown was pre-polished with a soft Abbott-Robinson bristle brush and a 5-µm diamond polishing paste (Diashine, VH Technologies, www.vhtechnologies.com).
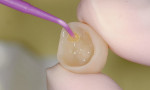
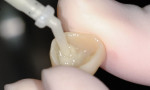
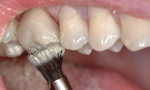
The assistant dispensed two drops of the adhesive, which contains the necessary components (including silane) to ensure a strong bond for the cement to its surface (Figure 4), into the supplied dispensing well and applied to the intaglio. Simultaneously, the dentist applied the adhesive in self-etch mode, as the application of phosphoric acid often produces tissue bleeding when inadvertent contact with it is made. When using the self-etch mode, bond strengths over greater than 25 MPa are achievable (3M, internal data).
The tooth was treated in the same fashion with Scotchbond Universal adhesive using a self-etch mode to etch, prime, and bond the tooth surface in one step (Figure 5). Application time to both restoration and tooth was 20 seconds, with subsequent 5-second air-thinning with moisture- and oil-free air to disperse the solvent. Shade A3 of the cement was chosen. In most cases for posterior teeth, transparent shades will be the most common choice.
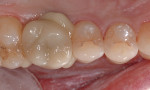
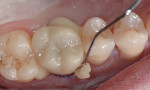
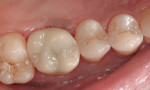
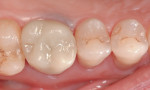
The cement was then dispensed through the auto-mix syringe bent tip into the lumen of the crown (Figure 6). The crown was seated and the cement was allowed to self-cure (Figure 7). Alternatively, a 2-second light application could be used to accelerate the gel set, as the cement is both self-curing and responsive to light polymerization. The cement excess was removed with an explorer in the gel phase (Figure 8); once complete, the final restoration was completely light polymerized for one cycle per tooth surface or five total. Occlusion was adjusted, and adjusted areas repolished using a soft prophy brush with Diashine (Figure 9). The paste was rinsed and the immediate postoperative result evaluated (Figure 10 and Figure 11). The patient was recalled 3 months postoperatively with no reported complications (Figure 12).
Conclusion
With the increasing emphasis on silica-based and crystalline ceramics, nano-ceramics, and composite indirect restorations, and with the continued use of metal-based restorations, the need for a versatile, easy-to-use, high-bond-strength resin cement is quite apparent. Versatility is an extremely important quality for an adhesive cement system in today’s practices, given the widely varying clinical situations and materials practitioners must handle. As adhesive resin cement systems have grown in popularity, dentists have frequently been required to inventory a large number of product New cement and adhesive combinations are available, however, to enable predictable outcomes using a repeatable and easy-to-master placement technique when an adhesive cement is either desired or clinically indicated, regardless of the material or restoration type chosen.
Disclosure
The author has received an honorarium from 3M ESPE for this article.
References
1. Christensen GJ. Marginal fit of gold inlay castings. J Prosthet Dent.1966;16(2):297-305.
2. Hikita K, Van Meerbeek B, De Munck J, et al. Bonding effectiveness of adhesive luting agents to enamel and dentin [published online ahead of print Jan 19 2006] . Dent Mater. 2007;23(1):71-80.
3. Krejci I, Lutz F, Gautschi L. Wear and marginal adaptation of composite resin inlays . J Prosthet Dent. 1994;72(3):233-244.
4. Fasbinder DJ. The CEREC system: 25 years of chairside CAD/CAM dentistry . J Am Dent Assoc. 2010;141(suppl 2):S3-S4.
5.Fradeani M, Aquilano A. Clinical experience with Empress crowns . Int J Prosthodont. 1997;10(3):241-247.
6. Fasbinder DJ, Dennison J, Heys D. Clinical evaluation of CAD/CAM-generated composite inlays: ten year report [abstract 379]. Presented at: IADR/AADR/CADR 89th General Session; March 16-19, 2011; San Diego, CA.
7. el-Mowafy OM, Fenton AH, Forrester N, Milenkovic M. Retention of metal ceramic crowns cemented with resin cements: effects of preparation taper and height . J Prosthet Dent. 1996; 76(5):524-529.
8. Shinohara MS, Azevedo C, De Goes M. Pre-etching dentin effects on morphology and bond strength of self-etching adhesives [IADR abstract 1659] . J Dent Res. 2012;91(spec iss B):1659.
9. Maeno M, Akiyama S, Ogawa S, et al. Bonding performance of recent all-in-one adhesive systems to abrasion-lesion dentin [AADR abstract 1306] . J Dent Res. 2012;91(spec iss B):1307.
10. Blatz MB, Zbaeren C, Mante F. Bond of a new self-etch adhesive to alumina and zirconia [AADR abstract 710] . J Dent Res. 2012;91(spec iss B):710.
11. Burgess J, Shah S, Cakir D, et al. Shear bond strength to restorative materials and tooth structure [AADR abstract 636] . J Dent Res. 2012;91(spec iss B):636.
Daniel J. Poticny, DDS
Adjunct Clinical Associate Professor
University of Michigan
Ann Arbor, Michigan
Private Practice
Grand Prairie, Texas