Leveraging Composite Characteristics to Produce Superior Results
Handling, color matching, and polishability are key in composite restorations
Indian Prime Minister Jawaharlal Nehru once said, “The highest type of efficiency is that which can utilize existing material to the best advantage.” In dentistry, these words ring especially true when undertaking direct composite restorations, whether in the anterior or posterior. Factors that can influence direct composite resin success include the skill of the operator; the size, depth, and location of the carious lesion; and material choices. Of these factors, material choices are the most easily changed. Ultimately, the handling characteristics and universal applicability of a composite resin may be the most important features influencing a dentist’s preferences.
The Challenges of Color Matching
An important element that impacts acceptance of esthetic composite restorations is color matching, also referred to as blending or the chameleon effect. Current composites consist of methacrylate resins with inorganic fillers that have a refractive index (RI) close to that of enamel and dentin.1,2 The RI is a measure of how rays of light bend when passing from one medium to another; in this case, passing from air to composite or tooth.3 This concept is further complicated when composite restorations are viewed under different light sources. The phenomenon in which two colors appear unequal under different illuminants is called metamerism or metameric failure (Figure 1).4
The challenges of blending restorative materials with natural tooth are complicated but can be mitigated by material choices and careful shade selection. For example, TPH®3 universal composite (DENTSPLY Caulk, www.caulk.com) has an RI of 1.52 to 1.55, whereas enamel and dentin have RIs of 1.63 and 1.54, respectively.1 Ideally, a restorative material that possesses both translucent properties and an appropriate RI should have a chameleon effect and create restorations indistinguishable from natural teeth.
Differences in color are often difficult to quantify and qualify. One measure of the distance between shades, called Delta-E (ΔE), was proposed to help standardize the difference between shade guides and restorative products.5,6 A ΔE difference of 0 to 1 is indistinguishable to the human eye. If the two shades (ie, tooth-composite or composite-composite) have a ΔE difference of greater than 4, it is a poor match.
A New Approach
A new composite called TPH Spectra™ (DENTSPLY Caulk) was designed to be a universal restorative material appropriate for all uses. It is based on the resin technology of TPH3 and contains nanohybrid and microfiller components. The result is a composite that has the potential to perform well in either the anterior or posterior, and should exhibit toothlike translucency, improved polishability, color stability, and good wear resistance.2,7,8 TPH Spectra also comes in two handling choices: a creamy light-viscosity formulation and a packable high-viscosity formulation. For both viscosities, the physical properties are similar.
To make shade selection simpler, TPH Spectra is available in the seven most popular shades: B1, A1, A2, A3, A3.5, A4, and C2. According to the manufacturer (DENTSPLY, internal data, 2012), the seven shades of TPH Spectra represent more than 80% of total sales from the previous TPH3 formulation. Because some practitioners may be overwhelmed by the number of current shades, the TPH Spectra Shade Guide was condensed. The Vita Classical Shade Guide (Vident, https://vident.com) has 16 shades, and the TPH3 shade guide had 26. Because only seven of the current 26 shades are regularly purchased, the ΔE value between shades was calculated to determine if the top seven shades could be used in place of another shade. Keeping the ΔE less than 4, it is possible to “cover” all the Vita shades with the existing TPH Spectra offerings (Table 1).9
Case 1
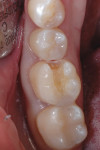
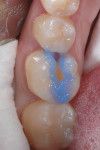
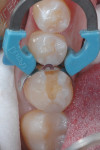
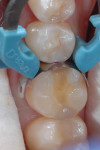
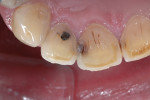
A 21-year-old woman presented for restoration of tooth No. 30. After verifying that there were no medical contraindications to treatment, the patient was anesthetized with 1 carpule of 4% Septocaine® with epinephrine 1:100,000 (Septodont, www.septodontusa.com). Caries excavation was completed with a 330 carbide bur and verified with Snoop™ caries detector (Pulpdent Corporation, www.pulpdent.com) (Figure 2). To maximize bond strength and minimize marginal staining and postoperative sensitivity, a selective-etch technique was chosen.10,11 Phosphoric acid (34%) was syringed around the enamel margins of the preparation (Figure 3). Prime&Bond Elect™ (DENTSPLY Caulk) was scrubbed into the preparation for 20 seconds then lightly air-dried for 5 seconds to remove the solvent. The tooth was isolated with Palodent® Plus (DENTSPLY Caulk) (Figure 4). Note the frosted appearance of the enamel margins after acid etching.
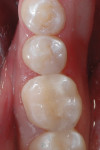
A layer of SureFil® SDR® Flow (DENTSPLY Caulk) was syringed into the preparation and then light cured for 20 seconds (Figure 5). The final restorative layer of TPH Spectra high-viscosity shade A3 was applied in 2-mm increments until the preparation was completely filled. Finishing and polishing of the restoration was completed with fluted composite finishing burs and Enhance® polishing points (DENTSPLY Caulk). The completed restoration displayed excellent color match and replication of natural tooth contour (Figure 6).
Case 2
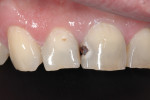
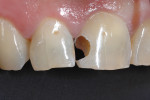
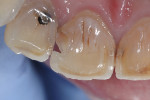
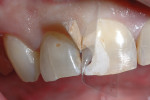
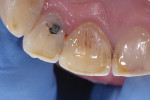
A 55-year-old man presented with a complaint of a “front cavity.” Intraoral examination revealed a cavitated lesion on the disto-facial surface of tooth No. 8 (Figure 7 and Figure 8). After verifying the medical history and x-rays, a direct composite resin restoration of the disto-lingual-facial surfaces was planned. Anesthesia was initiated with one carpule of 2% Xylocaine® Dental with epinephrine 1:100,000 (Dentsply Pharmaceutical, www.dentsplypharma.com). Caries excavation was completed with high-speed (330 bur) and low-speed (4 round bur) handpieces, and verified with Snoop (Figure 9 and Figure 10). A facial bevel was placed with a football-shaped diamond bur to increase retention and facilitate shade matching and blending.
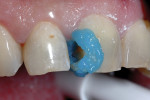
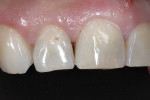
Because of the depth and size of the final preparation, a selective etch technique with Prime&Bond Elect was used. This technique was chosen to maximize enamel bonding while minimizing etchant contamination of dentin (mitigating postoperative sensitivity).10,11 The enamel was etched with 34% phosphoric acid for 20 seconds and then rinsed (Figure 11). Prime&Bond Elect was scrubbed into the preparation for 20 seconds followed by a 5-second air dry to remove the solvent. Isolation was achieved with a Mylar® strip (DuPont™, www.dupont.com) and Wizard Wedge® (Water Pik, Inc., https://professional.waterpik.com) (Figure 12). The patient’s shade was judged to be between A3.5 and A4 according to the Vita Classic Shade Guide. TPH Spectra low-viscosity shade A3.5 was selected and placed in 2-mm increments, followed by 15-second curing cycles. The final restoration was finished with fluted composite finishing burs and Sof-Lex™ discs (3M ESPE, www.3mespe.com) to achieve proper shape and contour. After occlusal adjustment, the composite was polished with Enhance and PoGo® (DENTSPLY Caulk, www.dentsply.com) (Figure 13 and Figure 14).
Conclusion
Practitioners can increase practice efficiency by selecting appropriate, quality materials. TPH Spectra is intended to provide the handling choices and excellent physical properties needed to consistently produce superior clinical outcomes.
Disclosure
Jason H. Goodchild, DMD, and Nicholas R. Conte, DMD, are employees of DENTSPLY Caulk.
References
1. Meng Z, Yao XS, Yao H, et al. Measurement of the refractive index of human teeth by optical coherence tomography . J Biomed Opt. 2009;14(3):034010.
2. Garg N, Garg A. Tooth preparation for composite restorations. In: Textbook of Operative Dentistry. New Delhi, India: Jaypee Brothers Medical Publishing;2010:260.
3. Refractive index. Encyclopaedia Britannica website. www.britannica.com/EBchecked/topic/495677/refractive-index. Accessed January 17, 2013.
4. Askary A . Fundamentals of Esthetic Implant Dentistry. 2nd ed. 2008. Hoboken, NJ: Wiley-Blackwell; 2008:282-283.
5. Wozniak WT. Proposed Guidelines for the Acceptance Program for Dental Shade Guides. Chicago, IL: American Dental Association; 2008:1-2.
6. O’Brien WJ, Groh CL, Boenke KM. A new, small-color-difference equation for dental shades . J Dent Res. 1990;69(11):1762-1764.
7. LeBlanc BJ. Nanohybrid composite restorations: dentistry’s most versatile solution . Dental Economics. 2009;99(5). www.dentaleconomics.com/articles/print/volume-99/issue-5/features/nanohybrid-composite-restorations-dentistry39s-most-versatile-solution.html. Accessed January 17, 2013.
8. Vargas M. Nanomicrohybrid composites make posterior placement easier . Dent Today. 2012;31(5):128-131.
9. Using TPH Spectra. TPH Spectra website. www.tphspectra.com/using-tph-spectra. Accessed February 27, 2013.
10. Ritter R. Using the selective etch technique for esthetic restorations . Inside Dentistry. 2011;7(3):102-103. www.dentalaegis.com/id/2011/03/using-the-selective-etch-technique-for-esthetic-restorations. Accessed January 23, 2013.
11. Perdigão J. New developments in dental adhesion . Dent Clin N Am. 2007;51(2):333-357.
Jason H. Goodchild, DMD
Private Practice
Havertown, Pennsylvania
Clinical Associate Professor
Department of Oral Medicine
University of Pennsylvania School of Dental Medicine
Philadelphia, Pennsylvania
Research Dentist, Clinical Research and Education
DENTSPLY Caulk
Milford, Delaware
Nicholas R. Conte, DMD
Director, Clinical Research and Education
DENTSPLY Caulk
Milford, Delaware