The Smile Makeover: How to Achieve the Illusion of Perfection
Esthetic dentistry means paying close attention to every detail before work is even begun.
Esthetic dentistry is not only about creating balance and harmony within a smile, but also has much to do with creating the illusion of perfection by using various dental materials and techniques. Smile design principles—such as determining the placement of the incisal edge, the development of pleasing width/height ratios, and the development of esthetic gingival contours—should be used to help achieve the desired goals.1,2 A narrow palate can be made to appear broadened by building out the ceramic or porcelain materials posteriorly. This would decrease the dark buccal corridor spaces that once highlighted that constricted arch form. Teeth themselves can be made to seem larger, smaller, wider, or narrower just by reshaping them to reflect the light differently. Teeth are only as wide as the height of contour to the line angles on the mesial and distal. Modifying these line angles will change the zone of reflection. A flatter surface will reflect more light to create a wider appearance, while tapering the edges will reflect less light, causing the tooth to appear narrower. Incorporating surface texture and natural translucency can help absorb or reflect light to make the tooth look more polychromatic and natural. The incisal edges of teeth should also be given texture and character to make it appear that the patient has chewed with them before. For older patients, craze lines can be added to teeth to make them appear more natural. This is part of the artistry that goes into a smile. In addition, one can create a softer, more youthful and more feminine appearance just by reshaping the incisal corners of the teeth—eg, rounding off the distal–incisal edges—and by modifying their heights—eg, making the lateral incisors 0.5 mm shorter than the central incisors. Rotating teeth can also add some natural qualities and give patients back some of the character of their old smile that they felt defined them in a good way.
This article explores how to work up, stage, and execute a smile makeover on an individual who has a deep overjet and a narrow, V-shaped maxillary arch.
Realistic Expectations
Patients often reach the point that they are not satisfied with their smile despite previous efforts to correct it. Many people were advised when they were younger to extract teeth to eliminate and prevent crowding of the arch. However, this can often result in a narrower smile with empty, dark buccal corridor spaces which displeases many patients when viewing photos of themselves. It wasn’t common practice years ago to expand the palate, which would have eliminated the need for extractions, flattened the nasal cavity (to allow for better breathing and less snoring), and created a rounder, more esthetically pleasing shaped face. Even today, many orthodontists expand the palate only when there is an edge-to-edge or crossbite position. However, given the desire for a broad smile, it may be beneficial to explore the possibility of palatal expansion for children. For those who do not have that opportunity, porcelain veneers are a great option to broaden and improve the esthetics of a smile.
For open-minded or curious patients, a mock wax-up can be done to demonstrate what a broader smile can look like and a putty template can be made to allow them to “try on” their potential new smile. This will help them envision the possibilities and have realistic expectations about what can be accomplished. When making diagnostic records, it is very important to take into account the occlusal cant, which is a form of asymmetry that becomes apparent when a person smiles, but is not perceptible in intraoral images or study casts. 3 This is why the facebow record is a critical tool for communicating asymmetry to the dental laboratory. Clinical results being sought are directly proportional to the communication skills between dentists and their laboratories.4 It is also suggested that the patient meet with the ceramist for a custom shade selection when appropriate.
Case Presentation
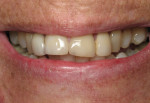
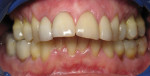
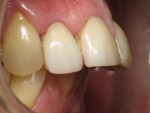
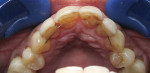
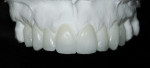
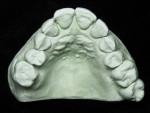
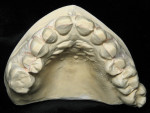
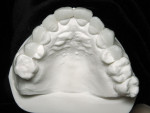
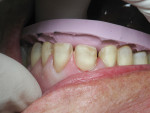
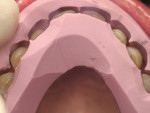
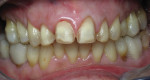
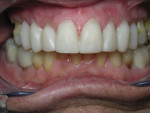
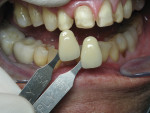
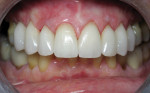
A 62-year-old female presented to the author’s office expressing dissatisfaction with her smile, saying she wanted it to be “whiter, straighter, and to not look so narrow and protruding” (Figure 1 through Figure 4). The patient was advised to see the orthodontist for a consultation to discuss all options to correct the crowding, overjet, and position of her teeth to provide a more predictable end result with the veneers. The patient was not interested in undergoing any orthodontics at this time, and because she had a nice profile, the author decided to take records for an esthetic wax-up to determine if he could create a more ideal smile using just porcelain veneers to round out the arch form and to make her teeth appear less protruding. When viewing her maxillary teeth from an occlusal view, the “V” shape of the arch was apparent (Figure 5); and when viewing her non-retracted smile, it was evident just how asymmetric she was. This patient showed more teeth on her left side and fewer on the right when smiling. In addition, she had a reverse curve of Spee, with her incisors not following the curvature of her lower lip.
In the absence of a temporary model (with the desired modifications) taken by the dentist, the ceramist usually creates wax-ups based on the initial models. They are typically returned with perfect symmetry by the dental laboratory; however, most people have some degree of asymmetry.5 This being said, if the temporary restorations are to be fashioned from the wax-up, the provisional restorations should be modified using the additive/reductive technique to give the teeth balance and complement the facial features, especially if the buccal corridor will be different on one side compared with the other. Minimizing the buccal corridor space on either side and modifying it to create the illusion of symmetry is a critical feature of smile design.5-9 A true testament of a successful smile makeover is an inability to readily detect the true imbalance of the patient’s facial features.
The patient had Class I molar relationships on both right and left sides, with her molars in more of an edge-to-edge position due to the narrow size of her maxilla. She had an 8-mm overjet, with flaring of the maxillary incisors and mandibular crowding with lingually inclined teeth in both arches. In addition, there was a maxillary midline shift of 1 mm to the right and a mandibular midline shift of 1 mm to the left.
The patient underwent a comprehensive oral examination and periodontal evaluation to ensure that the restorations were being built on a strong and healthy foundation. This patient did have several areas of caries that needed to be addressed, including the need for root canal therapy for teeth Nos. 14, 18, and 31, all of which would need subsequent core build-ups and crowns. In addition, tooth No. 30 was deemed non-restorable due to advanced recurrent caries, and the patient was referred to an oral surgeon to evaluate it for the placement of an implant. This patient did have a long history of smoking, which contributed to her condition. In addition, it was determined that she was a candidate for minor gingival recontouring in order to create a more even gingival line when smiling.
After consulting with the recommended specialists and advising and educating her regarding all of the treatment options, the next step was to take comprehensive records. This included diagnostic impressions, bite records, preoperative facebow record (using the Artex® articulator system [Jensen Dental, jensendental.com]), a full-mouth series of x-rays, and a complete set of photographs, as well as to have the laboratory create an esthetic wax-up to more accurately depict what could be achieved without orthodontics (Figure 6 through Figure 9).
Case Work-Up
A visual periodontal and occlusal assessment was performed. The author analyzed the patient’s case following the requirements for occlusal stability as outlined by Dawson. These include stable stops on all teeth when in centric relation, anterior guidance in harmony with the movements within the envelope of function, full posterior disclusion in protrusive movement, and no posterior interferences on the working or non-working side in canine guidance.10 It was known ahead of time that it would not be possible to achieve anterior coupling given the extreme overjet of her anterior teeth. Because the patient was asymptomatic and occlusally stable before treatment began, it was desirable to duplicate the previous comfortable bite.
First steps included an appraisal of the maxillary central incisors relative to the upper lip, as would normally be done when the treatment-planning sequence begins with esthetics.11 The length and horizontal edge position of her maxillary incisors were determined as well as possible, which would be tested and modified during the provisional stage derived from this diagnostic wax-up. Taking time to set up this incisal edge position is one of the most important diagnostic steps, and it saves time and prevents future problems. An error in the incisal position can cause restorations to break and result in a sore musculature from an uncomfortable envelope of function.12 The clinician should strive to create an incisal edge that would contact the inner vermillion border of the lower lip when pronouncing the letters “F” and “V.”13 The correct position should also allow for the air to flow naturally between the upper and lower incisors when creating the “S” sound.10
In an effort to create a more youthful appearance, the patient’s smile was designed so that her two maxillary central incisors would be just slightly longer than the laterals. Her cuspids supported the corners of her mouth and were approximately the same length as the central incisors.14 The author rounded the distals of her incisors to create a softer, more feminine appearance, and had the curvature of the lower lip be the guide for the ideal smile arc from central incisor to canine.15,16
Buccal and incisal putty stints were made to show the proper guidance in the preparation of the teeth (Figure 10 through Figure 12). In addition, a putty stint was fashioned from the wax-up to create a matrix for producing an exact replica to be used for the provisionals. The author had to modify the initial set of temporaries based on the initial wax-up after realizing that the patient's central and lateral incisors were brought in too much, causing her to lose some of the nice profile characteristics that she had previously. In order to correct this, slightly more material was added to the cervical third in order to maintain her lip support and keep her profile where it was originally. The additive/reductive technique was used to balance the harmony of the buccal corridors of her smile (Figure 13). A new impression of these modifications was sent to the laboratory to use as a guide for making the final restorations. The diagnostic wax-up, preparation model, and guides were fabricated and used to verify esthetic design, phonetics (while wearing temporaries), and adequate tooth reduction to achieve restorative needs.
The Restorative Phase
The old maxillary anterior splint that was present on the lingual surfaces of teeth Nos. 6 through 11 was removed, along with the moderate recurrent caries around the failing bonding that was securing the splint in place. The patient’s previous older veneers on teeth Nos. 7 through 10 were removed; teeth Nos. 5 and 12 had been removed previously for orthodontic reasons when she was younger. Teeth Nos. 4 through 13 were prepared for porcelain veneers according to the preparation model and diagnostic wax-up.
Final impressions were taken using Impregum™ and Permadyne™, both from 3M ESPE (3mespe.com), along with a bite registration and counter model. In addition, a stump shade photograph was taken to assist the laboratory in knowing how to layer the porcelain to attain the desired effects and selected shade (Figure 14).
The veneers were tried in to make certain that everything fit well. A rubber dam was used to create adequate isolation and to ensure a clean, dry, and easily accessible restorative environment. The prepared teeth were cleaned using Tubulicid (Global Dental Products, gdpdental.com) and flour pumice.
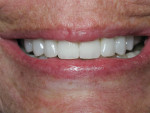
Surpass® (Apex Dental Materials, Inc., apexdentalmaterials.com) was subsequently used as the bonding agent, because some parts of the preparations were in dentin. The veneers were prepared with Interface (Apex Dental Materials) and Surpass 2 and then bonded with NX3 Nexus® clear cement (Kerr Dental Corporation, kerrdental.com), using the Veneer Styx® veneer positioning device (Cosmetic Innovations, Inc., ) for the final insertion of the veneers (Figure 15 and Figure 16). The excess cement was removed with a Schure 349 Lumineer Instrument (Patterson Dental, pattersondental.com), which does not scratch the porcelain surface, and the contacts were flossed and occlusion was checked in all excursions. A nightguard was made to help protect her investment. The patient said that she now feels self-confident and happy, and that she cannot stop smiling at everyone she meets (Figure 17 and Figure 18).
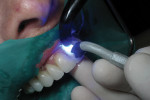
Tooth whitening had also been performed on her lower arch using the Zoom®! WhiteSpeed Light-Activated Whitening System (Philips Oral Healthcare, zoomwhitening.com). Her lower teeth were isolated, and the bleaching process was carried out in 4 rounds of in-office whitening, taking her from an A2/D2 shade to a B1 shade.
Conclusion
Esthetic dentistry means paying close attention to every detail before work is even begun. Each modification that can compensate for someone’s asymmetry and every facet of smile design that lends itself to balancing and harmonizing the smile will ultimately lend itself to the illusion of the perfect new smile for that individual.17
Rejuvenating a person’s smile has the power to inspire self-confidence and rebuild self-image. Patients look to the dental professional to make their smiles more beautiful and youthful. The creation of a beautiful smile has the power to help one find new love, land that new job, get that extra edge in business and networking, and to simply just live a happier and healthier lifestyle.
Disclosure
The author is Founder and President of Cosmetic Innovations, Inc., and inventor of Veneer Styx, a product mentioned in this article.
Acknowledgment
The author wishes to acknowledge ceramist Peter Kouvaris and his entire dental laboratory team for their guidance and support throughout the planning and execution of this challenging smile makeover and for helping the author to make a difference in this world one smile at a time.
References
1. Rufenacht CR. Fundamentals of Esthetics. Chicago, IL: Quintessence Publishing; 1990.
2. Levin EI. Dental esthetics and the golden proportion. J Prosthet Dent. 1978;40(3):244-252.
3. Sabri R. The eight components of a balanced smile. J Clin Orthod. 2005;39(3):155-167.
4. Griffen Jr JD. How to build a great partnership with the technician: simplified and effective laboratory communication. Contemporary Esthetics and Restorative Practice. 2006;10(7):26-34.
5. Peck S, Peck L. Selected aspects of the art and science of facial esthetics. Semin Orthod. 1995;1(2):105-126.
6. Moore T, Southard KA, Casko JS, et al. Buccal corridors and smile esthetics. Am J Orthod Dentofacial Orthop. 2005;127(2):208-213.
7. Roden-Johnson D, Gallerano R, English J. The effects of buccal corridor spaces and arch form on smile esthetics. Am J Orthod Dentofacial Orthop. 2005;127(3):343-350.
8. Graco A, Cozzani M, D’Elia L, et al. The smile buccal corridors: aesthetic value for dentists and laypersons. Prog Orthod. 2006;7(1):56-65.
9. Ritter DE, Gandini LG, Pinto Ados S, Locks A. Esthetic influence of negative space in the buccal corridor during smiling. Angle Orthod. 2006;76(2):198-203.
10. Dawson P. Functional Occlusion: From TMJ to Smile Design. St. Louis, MO, Mosby; 2006:181.
11. Spear F, Kokich VG, Mathews D. Interdisciplinary management of anterior dental esthetics. J Am Dent Assoc. 2006;137(2):160-169.
12. Hess L. The relevance of occlusion in the golden age of esthetics. Inside Dentistry. 2008;4(2):36-44.
13. Chiche GJ, Pinault A. Esthetics of Anterior Fixed Prosthodontics. Hanover Park, II: Quintessence Pub. Co; 1994:21.
14. Goldstein RE. Change Your Smile. Chicago, IL: Quintessence Publishing; 1984:6-22.
15. Parekh SM, Fields HW, Beck M, Rosenthal S. Attractiveness of variations in the smile arc and buccal corridor space as judged by orthodontists and laymen. Angle Orthod. 2006;76(4):557-563.
16. Sarver DM. The importance of incisor positioning in the esthetic smile: the smile arc. Am J Orthod Dentofacial Orthop. 2001;120(2):98-111.
17. Ker AJ, Chan R, Fields HW, et al. Esthetics and smile characteristics from the layperson’s perspective: a computer-based survey study. J Am Dent Assoc. 2008;
139(10):1318-1327
About the Author
Marc Lazare, DDS, MAGD
Clinical Attending–General Dentistry
North Shore University Hospital
Manhasset, New York
Private Practice
Cosmetic and General Dentistry
New York, New York