Putting It Together: Integrating New Digital and Restorative Options
Understand how rapidly changing innovations work in tandem for patient-centered care
It used to be that choosing restorative materials for a patient was fairly simple. In the 1970s, if the restoration was for the posterior, cast gold was used; for the anterior, porcelain-fused-to-metal (PFM), or a prefabricated porcelain facing with cast gold was selected. In cases demanding very high esthetics, porcelain jacket crowns were fabricated with ceramic (eg, Vita Dur N) on foil and conventionally cemented in the mouth.1,2
The 1980s brought the evolution of bonded all-ceramic restorations fabricated using a refractory or foil technique. By the late 1980s and early 1990s, high-strength core materials such as alumina (eg, Vita In-Ceram®, Vident, vident.com; Procera™, Nobel Biocare, nobelbiocare.com) were introduced into dentistry; then came leucite-reinforced pressed ceramic (eg, IPS Empress®, Ivoclar Vivadent Inc., ivoclarvivadent.us; Authentic®, Microstar Dental, LLC, microstardental.com). In the late 1990s and early 2000s, many brands of zirconia core-based restorations (eg, Lava™, 3M ESPE, 3mespe.com) were introduced, with powdered ceramic layered over the core, or pressed ceramic applied to the core (eg, IPS e.max ZirPress®, Ivoclar Vivadent; CZR, Kuraray Noritake Dental Inc., noritake-dental.co.jp).3-5
In the late 1990s, dentistry also saw increased use of lithium disilicate (eg, IPS Empress® 2, IPS Eris®, Ivoclar Vivadent), and since 2000, the industry has witnessed a drastic increase in the use of lithium disilicate (eg, IPS e.max®, Ivoclar Vivadent) and monolithic zirconia (eg, BruxZir®, Glidewell Laboratories, glidewelldental.com). The development of high-translucency lithium disilicate and more translucent-colored zirconia materials has dramatically expanded the use of these materials in a monolithic or very conservatively layered form.6-8
Similarly, in the past decade implant technology has steadily developed and become more predictable. The relationships among implant position, bone levels, and gingival response have become much more clearly understood, resulting in an explosion of implant placements requiring restoration.9-11 Abutment selection for implants has evolved from cast gold and prefabricated titanium, to zirconia or hybrid zirconia and titanium. Now, lithium-disilicate abutments with titanium bases also are being used.
Digital dental technology also developed during this time. The early chairside CAD/CAM systems (Sirona, sirona.com), which seemed cumbersome and inaccurate, have evolved into mainstream solutions for same-day, in-office ceramic restorations that are becoming more widely used in dentistry. Patient charts, radiographs, photography, impression-taking, and restoration design have all transitioned from being primarily analog functions to being partly or totally digital procedures.12-14
The proliferation of digital impressions (eg, iTero™, Cadent Inc., cadentinc.com) and laboratory CAD/CAM software (eg, 3Shape A/S, 3shapedental.com; Dental Wings Inc, dental-wings.com), paired with milling and printing systems, has produced an almost endless series of choices for fabricating today’s restorative options.12,14 The newest technology is sometimes more accurate and efficient for producing restorations; however, situations still exist in which using new technology sacrifices accuracy and efficiency compared with traditional techniques. Such situations continually arise, and the balance is changing constantly.15,16
The challenge today is not only understanding the various restorative ceramic systems, but also finding the best manufacturing pathway to fabricate these materials to maximize their potential functional and esthetic properties. While integrating new manufacturing processes, clinicians need to also ensure that they are still following a sequence of treatment and communication steps that facilitate a high-quality and predictable restorative outcome for their patients.
This article outlines the strengths and weaknesses of various popular ceramic restorative materials and how today’s technology is utilized for their fabrication into restorations. Many options are available for use depending on a variety of case-dependent criteria. These options change rapidly as manufacturers update software and introduce product modifications and new milling or printing technology is launched.
Ceramic Materials Available Today
Today, two ceramic materials are experiencing the fastest growth: lithium disilicate and zirconia. PFM and gold restorations are steadily declining, while alumina core materials are being replaced with various zirconia-based applications. Leucite-reinforced pressed ceramics are still in use, but are being overtaken by the use of lithium-disilicate restorations. Feldspathic ceramic restorations fabricated on refractory or foil are also still used today. Examining the relative physical strength of each material helps in understanding usage.
In terms of flexural strength, feldspathic ceramic has a flexural strength in ranges of 80 MPa to 95 MPa. Leucite-reinforced pressed ceramics exhibit flexural strengths between 125 MPa and 175 MPa, depending on the research consulted. Lithium disilicate has flexural strengths between 360 MPa (milled) and 400 MPa (pressed). Alumina core material ranges between 500 MPa and 600 MPa of flexural strength. Zirconia demonstrates flexural strengths between 900 MPa and 1200 MPa. For PFM restorations, data are harder to quantify due to the restoration’s bilayer construction, but 1300 MPa is frequently cited in lectures.17,18
Considered superficially, this data would immediately endorse the use of zirconia or PFMs for durability, but the selection equation is more complex. Bilayered materials contain very strong core materials. However, to esthetically mimic natural dentition, they require application of a layering ceramic. Unfortunately, most layering ceramics are relatively weak, ranging from 85 MPa to 100 MPa. The result is an indestructible core or framework layered with a potentially layering ceramic that easily chips.17 Substructure design is critical for supporting the weaker layering ceramic.
Coefficient of thermal expansion and heating or cooling rates also play an important role in the success or demise of these restorations. Clinically, throughout the years the layering porcelain has chipped away from PFM, pressed over zirconia (also powder built), and layered alumina restorations (Figure 1 and Figure 2).19 Leucite-reinforced restorations that were used widely in the 1990s have fared well, but these also are being replaced.
Lithium disilicate was first introduced to the market as a fairly opaque material that required layering, and the combination of a 360 MPa core and 95 MPa layering ceramic produced a very high failure rate.6 The game changer with lithium disilicate occurred when translucency levels were increased, greatly reducing the need for layering ceramic; with the highest translucency levels, no layering is required.13,20 This now enables the use of a material with 360 MPa to 400 MPa that is etchable and bondable to tooth structure and can comprise most or all of the restoration volume.
The increase in flexural strength achieved by forgoing layering in the vulnerable areas of heavy function that were previously fabricated with weaker layering ceramic has yielded the highest success rates for any restoration used to date, with the exceptions of gold and monolithic zirconia. Current studies comparing 1.5-mm monolithic lithium-disilicate restorations to PFM crowns showed that lithium disilicate can withstand higher loads without fracturing than PFM crowns.21
Another characteristic of lithium disilicate that expands its usability in the mouth is its ability to be pressed into very thin veneers; two-tenths of a millimeter is possible, which makes it a good material for minimally invasive techniques or no-preparation veneers (Figure 3 and Figure 4).13,20 This had previously been the exclusive domain of feldspathic veneers fabricated on foil or refractory. Although the more durable and easier-to-fabricate lithium disilicate is popular for thin veneers, the potential to vary opacity throughout the restorations with feldspathic veneers still leaves a place for these restorations as being the most appropriate choice (Figure 5).8,20
Lithium disilicate is also being used for implant abutments, in which a titanium base with a chimney is used to interface with the implant and provide a positive seat for the screw. A lithium-disilicate top in the shape and color of a prepared tooth is bonded to this base, creating a hybrid abutment that approximates the appearance of a natural prepared tooth (Figure 6 and Figure 7).22,23
Zirconia restorations are used widely in dentistry today, as well. Early zirconia materials were opaque and white, requiring aggressive preparation and layering, much like PFMs. Very nice esthetic levels were possible, and, with strengths of 900 MPa to 1200 MPa, multi-unit bridges were possible. Substructure design to support the layering ceramic was critical to restoration success, as was slow cooling to prevent internal stress buildup within the bilayered restorations.5,7,17,19
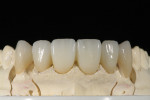
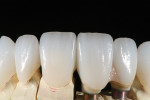
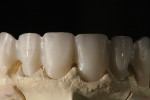
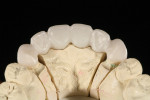
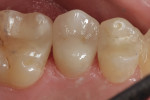
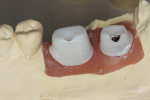
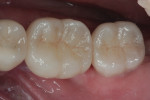
Today, many more translucent zirconia varieties are available from manufacturers. This reduces the need for layering ceramics, as well as the thickness of applied ceramic layers needed for an esthetic appearance (Figure 8 through Figure 11). The higher translucent zirconia is also being used in a monolithic stained and glazed format for full-contour posterior restorations.5,13,20
The low cost and high durability of this type of restoration, along with the potential for conventional cementation, have made it very popular in many segments of dentistry. Although monolithic zirconia looks better than older zirconia, it still falls short of the esthetics commonly achieved with monolithic lithium-disilicate restorations (Figure 12).5,13,20
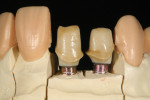
Implant abutments are another area for which zirconia is commonly used. Tooth-shaped, custom-designed zirconia abutments are frequently used to restore implants in the esthetic zone. Grey titanium abutments can show through a patient’s gingival tissue, creating an undesirable esthetic outcome. Zirconia abutments can serve as a platform for a layered zirconia crown or be used with a lithium-disilicate restoration (Figure 13 and Figure 14).5,13,20 Fracture around the screw seat has occurred in some zirconia abutments and must be a consideration for abutment selection. Hybrid zirconia abutments over a titanium abutment base and chimney are also used frequently with high success.22,23
Digital Technology
Although CAD/CAM creation and milling for dentistry has existed since the 1980s (eg, CEREC®, Sirona), digital technology did not broadly penetrate the market prior to the early 2000s. Digital photography and radiographs were the first major areas of penetration. The manufacturer Sirona has made steady progress with chairside milling and design over the past 20 years, improving ease of use and restorative quality. Materials and software development have interacted and influenced each other over the years (Figure 15).12,14-16
Early millable ceramics were fairly low-strength feldspathic glass or leucite-reinforced glass, which limited their use to inlays and low-stress crowns. This subsequently limited development of full-contour design software. Simultaneously, zirconia substructures were being used widely by dental laboratories, driving early software design toward substructure applications used for designing and milling zirconia frameworks for layered zirconia restorations.12,14-16
The introduction of monolithic lithium-disilicate and monolithic zirconia restorations brought an explosion of software development for full-contour design (Figure 16). Today, many companies sell software and/or milling equipment for designing full-contour restorations.
Implant abutment design for zirconia or titanium abutments has also benefited from full-contour software development. Once a full-contour restoration is designed for the edentulous space, the implant abutment can be designed within the full-contour crown, idealizing restorative thickness and support for the final implant-supported restoration (Figure 17). Easier-to-use software for full-contour design capability also benefits the design of zirconia restorations with strategic and minimal esthetic layering. By producing contours in the digital environment that closely approximate correct esthetics and utilizing more translucent zirconia, restorations can be created that are mostly monolithic zirconia and have only a thin bilayer of weaker layering ceramic applied to visible zones of the crown (eg, Diadem Precision Technology, diademprecision.com; and 3Shape).22,23
It is also possible to design a full-contour crown and split the file to produce a substructure and the full-contour top for the crown—either zirconia or printed metal for the substructure, and then a printed wax top that can fit over the substructure and pressed by conventional means.24,25 The industry is also seeing digital design of partial denture frameworks and digitally designed and milled full dentures. More applications will be integrated into the digital workflow in the future.
Digital impression technology adds to the digital design equations. The stereolithography (STL) file generated by digital impressions can now be sent electronically to the model fabrication facility and to restorative design software immediately after the impression is taken. Starting the restorative design before the model work is finished greatly compresses the time required to fabricate a restoration in the laboratory.
Software companies have added model fabrication features to their design software, allowing users to mark margins, separate working dies, and design the crown to go on the model in the digital environment. Then, the model can be tasked to a stereolithic printing system (Figure 18), and the digital restoration design exported to a milling machine on site, or a milling center anywhere in the world. The model can then be printed from a resin-like material (eg, Objet, Stratasys Ltd., objet.com; EnvisionTEC Inc., envisiontec.com), and the restoration can be milled from lithium disilicate or zirconia, fit to the model, and stained and glazed prior to delivery.
One digital impression system (iTero) utilizes its own milling centers to produce digital models. The result is a “Geller style” removable die model (Figure 19). These cases can be worked with by importing the STL file into design software, or by conventionally waxing and pressing restorations on them.
Computed tomography (CT) technology is also heavily used in digital design, with many companies offering software that can read bone density and location, then propose ideal locations for implants with consideration of the location of the final desired tooth and the patient’s osseous structure capable of supporting an implant. The outcome of this planning can be accurate surgical guides, resulting in correct implant placement in the patient’s jaw; abutments and restorations can then be premanufactured based on the predicted implant position and be ready to screw into place on the day of surgery.
Discussion
Today, integrating these innovations into a dental practice’s routine should be predicated on patient treatment goals. These include providing comprehensive, systematic treatment to predictably achieve patients’ expectations. By examining the patient’s needs, desires, and pre-existing condition, a series of steps can be proposed to achieve the final desired result. This involves specialists, laboratory technicians, and the treating dentist in the overall restorative planning.
Orthodontics, periodontics, and oral surgery are utilized prior to restorative treatment to move gingival levels and/or teeth and provide underlying osseous support for implants and gingival levels. To coordinate treatment, digital photographs, radiographs, CT scans where needed, and digital or conventional models and bite registrations can be shared. Keynote and PowerPoint® presentations can be used to effectively communicate between members of the restorative team over long distances or to accommodate busy schedules. SkypeTM, iChat®, or Messages are some of the available Internet-based video chat programs for discussing cases and transferring images. DropboxTM is a file transfer protocol (FTP) program that also is useful for sharing photographs or video clips.
Diagnostic treatment planning—either conventional wax-ups or digital designs—is utilized as a first restorative step. Both functional and esthetic considerations are worked out at this phase.
Functional movements are evaluated on an articulator, which is set up to mimic the patient’s envelope of function (Figure 20). This can be accomplished with conventional stone models, wax, and an articulator, or completed within the digital environment using software (eg, 3Shape). When working with the analog pathway, a silicone matrix of the conventional wax-up can be filled with provisional material and transferred to the mouth for validation of shape, position, and function.
With digital designs, the STL file of the design is transferred to a milling machine, and polymethyl methacrylate (PMMA) overlays are milled for transfer to the patient’s mouth (Figure 21). Today, most diagnostic work is still done with conventional wax-ups, but as digital impressions become more widely used, so will digital diagnostic design.
Preparation design and material selection are based upon the most appropriate material to meet the patient’s needs while preserving existing tooth structure and providing longevity. The author’s most frequently used material is high-translucency lithium disilicate. As long as underlying tooth color is not drastically dark, this material provides an ideal combination of strength, longevity, and esthetics.
The author’s primary fabrication process for single posterior restorations is digital design and milling (eg, 3Shape, Diadem, Sirona inLab). For larger anterior cases, a matrix of the provisional restorations and wax injection is used to create waxed and pressed restorations from lithium disilicate. Two- and 3-unit anterior bridges are also made with waxed and pressed lithium disilicate. Posterior bridges can be fabricated from milled lithium disilicate fused to a zirconia substructure. The author still uses PFMs occasionally, and gold remains a great posterior restoration.
Acknowledgment
The clinical photographs for this article are courtesy of Franklin Shull, DMD, Lexington, SC.
References
1. Haj-Ali R, Walker MP, Williams K. Survey of general dentists regarding posterior restorations, selection criteria, and associated clinical problems. Gen Dent. 2005;53(5):369-375.
2. Cardoso A, Almeida PJ, Fischer A, Phaxay SL. Clinical decisions for anterior restorations: the concept of restorative volume. J Esthet Restor Dent. 2012;24(6):367-383.
3. Kelly JR, Nishimura I, Campbell SD. Ceramics in dentistry: historical roots and current perspectives. J Prosthet Dent. 1996;75(1):18-32.
4. Giordano R. All-ceramic restorative systems: alumina-based core systems. J Mass Dent Soc. 2002;51
(2):30-35.
5. Giordano R, Sabrosa CE. Zirconia: material background and clinical application. Compend Contin Educ Dent. 2010;31(9):710-715.
6. Höland W, Schweiger M, Frank M, Rheinberger V. A comparison of the microstructure and properties of the IPS Empress 2 and the IPS Empress glass-ceramics. J Biomed Mater Res. 2000;53(4):297-303.
7. White SN, Miklus VG, McLaren EA, et al. Flexural strength of a layered zirconia and porcelain dental all-ceramic system. J Prosthet Dent. 2005;94(2):125-131.
8. Giordano R. A comparison of all-ceramic restorative systems. J Mass Dent Soc. 2002;50(4):16-20.
9. Adams D, Williams DF. A review of dental implants. Dent Update. 1985;12(8):480-484.
10. Smith DC. Dental implants: materials and design considerations. Int J Prosthodont. 1993;6(2):106-117.
11. Vouros ID, Kalpidis CD, Horvath A, et al. Systematic assessment of clinical outcomes in bone-level and tissue-level endosseous dental implants. Int J Oral Maxillofac Implants. 2012;27(6):1359-1374.
12. McLaren EA, Culp L, White S. The evolution of digital dentistry and the digital dental team. Dent Today. 2008;27(9):112-117.
13. Giordano R, McLaren EA. Ceramics overview: classification by microstructure and processing methods. Compend Contin Educ Dent. 2010;31(9):682-688.
14. Fasbinder D. Using digital technology to enhance restorative dentistry. Compend Contin Educ Dent. 2012;33(9):666-672.
15. McLaren EA. Using copy milling technology in restorative dentistry. Dent Today. 1997;16(3):80-85.
16. Guth JF, Keul C, Stimmelmayr M, et al. Accuracy of digital models obtained by direct and indirect data capturing. Clin Oral Investig. 2012 Jul 31. [Epub ahead of print]
17. Lin WS, Ercoli C, Feng C, Morton D. The effect of core material, veneering porcelain, and fabrication technique on the biaxial flexural strength and weibull analysis of selected dental ceramics. J Prosthodont. 2012;21(5):353-362.
18. Seghi RR, Daher T, Caputo A. Relative flexural strength of dental restorative ceramics. Dent Mater. 1990;6(3):181-184.
19. Saito A, Komine F, Blatz MB, Matsumura H. A comparison of bond strength of layered veneering porcelains to zirconia and metal. J Prosthet Dent. 2010;104(4):247-257.
20. McLaren EA, Whiteman YY. Ceramics: rationale for material selection. Compend Contin Educ Dent. 2010;31(9):666-672.
21. Lorenzoni FC, Martins LM, Silva NR, et al. Fatigue life and failure modes of crowns systems with a modified framework design. J Dent. 2010;38(8):626-634.
22. Silva NR, Thompson VP, Valverde GB, et al. Comparative reliability analyses of zirconium oxide and lithium disilicate restorations in vitro and in vivo. J Am Dent Assoc. 2011;142(suppl 2):4S-9S.
23. Martinez-Rus F, Ferreiroa A, Ozcan M, et al. Fracture resistance of crowns cemented on titanium and zirconia implant abutments: a comparison of monolithic versus manually veneered all-ceramic systems. Int J Oral Maxillofac Implants. 2012;27(6):1448-1455.
24. Smith R. Creating well-fitting restorations with a digital impression system. Compend Contin Educ Dent. 2010;31(8):640-644.
25. Goodacre CJ, Garbacea A, Naylor WP, et al. CAD/CAM fabricated complete dentures: concepts and clinical methods of obtaining required morphological data. J Prosthet Dent. 2012;107(1):34-46.
About the Author
Matt Roberts, CDT
Founder
CMR Dental Lab
Idaho Falls, Idaho