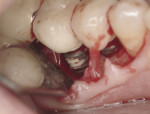
Implant Failures Caused by Cements
Salvaging compromised cases and preventing complications
When planning implant procedures, clinicians are faced with many options. Should they opt for a metal or ceramic restoration? Should they plan the implant treatment using digital means? Should they use a surgical guide? Should they use a cement-retained or a screw-retained restoration? Cement-retained implants offer many advantages over their screw-retained alternatives. They offer flexibility, can aid in correcting misaligned implants, and improve esthetics—even when the alignment is not ideal—especially in anterior regions of the dentition. However, they are associated with a unique set of disadvantages as well. First, it is much more difficult to remove a cement-retained restoration than a screw-retained implant intact if, for some reason, it has broken or the abutment screw has loosened. The other disadvantage—and the one that tends to cause the most issues for restorative clinicians—is that the retention of cement below the mucosal margin can lead to catastrophic implant complications.
Clinical Problems Caused by Excess Implant Cement
Barry Levin, DMD, says that implant cement can act like a foreign body in the mouth, “acting as a nidus for plaque and calculus accumulation.” He also explains that one of the reasons implant failure caused by excess cement in the mucosal margin can be so problematic is that, often, it is not immediately apparent that there is an issue. “Sometimes, the effects can be delayed for years after cementation,” he says. “The inflammatory lesions that develop can be devastating, and can result in severe bone loss and even the loss of the fixture.” Bone loss is perhaps the worst complication that can happen to a patient who has dental implants because if there is bone loss, the fixture may be lost. The loss of an implant not only causes significant pain, but also negatively affects the patient’s quality of life when he or she loses function of that implanted tooth.
Even if the excess cement does not cause bone loss, it may have detrimental effects on the patient’s soft tissue. According to Levin, “In esthetic areas in particular, this can severely disrupt implant treatment. Even if the implant remains osseointegrated, the resultant soft-tissue hyperplasia or recession can be an unacceptable outcome to both the patient and the clinician.”
If cementation issues contribute to implant failure, the options for the patient are extremely limited. Amanda Seay, DDS, a restorative dentist who specializes in esthetics, says that bone and tissue loss caused by excess cement can cause visual defects that are extremely difficult to repair. “When an implant is lost, patients must undergo bone and tissue grafts for up to a year before they can attempt to have another dental implant placed, and even then, the esthetic outcome is not predictable,” explains Seay.
Ways to Prevent Cementation-Related Implant Failure
The complications caused by cement in implant cases are often avoidable if the clinician takes the proper steps to ensure that there is no excess cement left below the mucosal margin. Restorative clinicians must be meticulous in their cement removal procedures. Levin suggests that clinicians follow up these procedures with radiographs to further ensure the complete removal of cement. “This method isn’t perfect,” says Levin. “The obvious shortcoming is that facial and palatal/lingual cement excess will not be visible on the radiograph, but it is still an improvement over visual and tactile inspection.”
Another way to avoid implant failure caused by excess cement is to use a custom abutment. Seay feels that this is one of the most important things clinicians can do to ensure the proper removal of implant cement. “Properly designed custom abutments give the clinician an anatomically shaped crown that facilitates the cleaning of cement. Also, they can be designed with supragingival margins to further ease the removal of cement.”
Maintaining Cement-Retained Implants
Even the most diligent of clinicians may sometimes miss residual sub-gingival cement in implant cases. For that reason, maintenance is extremely important for patients who have cement-retained implants. Signs of peri-implant inflammation often serve as a warning sign that there is excess cement below the gum line, and can let the clinician know that there is an issue before there is any radiographic bone loss. Other symptoms can include localized inflammation, progressively deeper probing depths, or slight bleeding. If these signs are caught early, the excess cement can be removed before irreversible damage occurs. Dr. Levin even recommends that patients with cement-retained restorations alternate between their periodontist’s office and their referring dentist for dental check ups, as a specially trained pair of eyes will catch these signs as early as possible. “Hard data is starting to emerge that peri-implantitis issues were much more prevalent in the patients who had implants placed in a periodontist’s office and then never returned to maintenance, compared to the ones who return on a regular basis,” he says.
Even if the patient is unable to return to the periodontist’s office for maintenance, the hygiene staff in the restorative clinician’s office should be well versed in the care of cement-retained restorations, as well as be aware of the symptoms of implant complications. “The scalers, curettes, and even prophy paste used on implants are different from those used on natural teeth, and these hygienists should be trained to search for the signs of inflammation as a part of their hygiene routine,” says Levin.
What To Do When Failure Occurs
When excess cement is the cause of implant failure, the clinician must act quickly to minimize damage. The first step is to remove the cement as soon as possible, and then the clinician should decontaminate the implant surface and remove the granulation tissue. Any retained cement has the potential to prevent healing and cause further problems.
According to Seay, if there is failure caused by implant cement, the patient must also take an active role in correcting the problem. “The patient must adhere to strict follow-up care, including home regimens that may include rinses or irrigants,” she explains. Seay does note, however, that this may not solve the issue, and access surgery or even resective surgery for wider defects may be necessary.
A Team Effort
Another way to minimize issues in cement-retained implant cases is to keep patients informed not only of the possible complications, but also to make them an active partner in the maintenance of their implants. “I always emphasize to my patients that implants must be a team effort,” says Levin. It is up to the patient to ensure that the implant is properly cared for between visits to the dental office, and the clinician must impress upon the patient the importance of this care.
Conclusion
Cement-retained implant restorations often offer superior esthetics, as well as other advantages compared to screw-retained alternatives. However, clinicians who place these prostheses must also be aware of the possible complications that may occur. Knowing the potentially devastating effects that excess implant cement below the gingival margin may have on the implant case, periodontists, restorative clinicians, and their staffs should all be diligent in looking for signs of failure, as well as in taking every precaution to avoid failure. When clinicians take the proper steps—such as using a custom abutment rather than a stock abutment, or even looking for excess cement on radiographs—implants are much more likely to serve patients for a much longer, and much more fruitful period of time.
The publishers and staff of Inside Dentistry could not bring the underlying concerns and trends affecting today’s dental practice and the general oral healthcare profession to the forefront without the insights shared by our knowledgeable interviewees. For their collective generosity of time and perspectives, we share our sincere gratitude.
Barry P. Levin, DMD
Private Practice
Elkins Park, Pennsylvania
Diplomate, American Board of Periodontology
Clinical Associate Professor
University of Pennsylvania
Philadelphia, Pennsylvania
aperiodoc@verizon.net
Amanda Seay, DDS
Private Practice
Mount Pleasant, South Carolina
seayamanda@gmail.com
The Importance of Using Custom Abutments
Amanda Seay strongly suggests that all clinicians placing cement-retained implants use custom abutments rather than stock abutments. If the abutment is specially designed for the patient, it is less likely that the clinician will have trouble removing excess cement. There are also other advantages to be noted. “Stock abutments may be cheaper than custom abutments, but overall, the time savings and superior dentistry we can perform with custom abutments make that cost difference practically nil,” she says. Since custom abutments are created by the laboratory, the clinician does not have to do anything except send the patient’s data to the lab. “While the lab cost is higher for a custom abutment, I believe that in the long run it saves my practice a lot of money because I don’t have to carry any inventory. Everything is taken care of by the lab, and I’m also saving chairtime because there are no fit issues. The abutment always drops right in.” When working on implant cases, whether cement-retained or screw-retained, Seay will only use custom abutments.