Dental Lasers
To safely and effectively integrate lasers into their practices, dentists need a working knowledge of basic laser physics and biological interactions, proper training, and an awareness of the capabilities and limitations of the different types of lasers.
Lasers have been used in dentistry for more than 20 years. Recent technological developments are creating a host of innovative treatments in all disciplines of dentistry. Dentists who want to integrate lasers into their practices need to be familiar with the various devices’ capabilities and limitations. A solid understanding of basic laser physics and biological interactions is also very important. Proper training is paramount once practitioners decide to incorporate lasers into their practices.
Basic Laser Physics
The word laser stands for light amplification by stimulated emission of radiation. Lasers are characteristically emitted from a stimulated active medium, monochromatic, unidirectional, and coherent. A laser beam is created from a substance known as an active medium, which when stimulated by light or electricity produces photons of a specific wavelength. CO2 and erbium are examples of active media. Laser light is made of a single wavelength of light (ie, monochromatic), and all dental lasers are found in the visible or infrared portion of the electromagnetic spectrum. Once a laser beam is produced, it will travel in one direction (unidirectional), although the divergence of the beam varies by type of laser and the associated transmission hardware. Coherence is the property that not only is a laser a single wavelength, but also that all the peaks and valleys of each wave travel in unison.
Dental lasers can emit the beam as either a continuous stream or discrete pulses of photons. Continuous-wave emission mode means the laser is on the entire time it is turned on. In these lasers, peak power equals the wattage output displayed. There are two basic forms of pulsed laser modes: gated wave and free-running pulsed. A gated wave pulse is usually created with a shutter that blocks the laser beam of a continuous wave laser from reaching the handpiece and target tissue at varying speeds. The laser is on constantly, but the shutter device blocks the light from transmitting. Free-running pulsed lasers are not on constantly, but they emit photons in powerful bursts of energy measured in millionths of seconds. Each of these temporal emission modes has important characteristics when the laser energy interacts with tissues, which need to be understood well by the practitioner. Peak power can be a difficult concept to understand, but its importance cannot be overstated. Each pulse has a set amount of energy, usually the millijoules displayed on the unit. As shorter pulses are used, this same energy is effectively squeezed into a smaller space, which increases the peak power of the pulse. Yet the actual energy expended is identical. Hard-tissue dental lasers can have peak powers in the thousands of watts, and these short bursts of extreme power allow for the efficient cutting of enamel, dentin, and bone.
Laser/Tissue Interactions
Substances known as chromophores absorb the light energy when a laser beam is aimed at tissue. A chromophore is a specific substance that absorbs the laser energy and converts it into thermal or mechanical energy in order to do work. Examples of chromophores include water (CO2 and erbium lasers) and hemoglobin (diodes and Nd:YAG lasers). The transfer of energy from laser photons to chromophores creates usable energy to do work. Dentists need to understand the specific chromophore for the laser wavelength they are using in order to create the desired effect in the target tissue.
The thermal implications for the target tissue of the three pulse modes are profound. Thermal relaxation refers to the ability of the target tissue to absorb heat produced by laser interaction. In continuous mode, there is no thermal relaxation at all, and potentially damaging heat can build in the tissue quickly. Gated-wave mode presents basically a half on/half off exposure to laser energy, and the ability of the tissue to absorb the heat is limited. Thermal relaxation occurs the most when free-running pulsed lasers are used. Each pulse is temporally very short, anywhere from 50 to 1,000 millionths of a second. There is adequate time between each pulse to allow the tissue to absorb and dissipate the heat to minimize thermal damage. This lack of tissue heating results in the lowered postoperative discomfort and predictable healing seen after many laser procedures. It also contributes to the ability to perform many operative dentistry procedures and even some soft-tissue ones without local anesthesia. An excellent analogy is if a finger is moved rapidly through a candle flame it will not burn, as the tissue can absorb and dissipate the momentary high heat exposure. If the same finger is moved slowly through the flame it will get burned eventually. Placing the finger in the flame and holding it there will cause rapid thermal damage.
Types of Dental Lasers
There are currently five predominant types of lasers available for dentists: diode, Nd:YAG, Er:YAG, Er,Cr:YSGG, and CO2. Table 1 summarizes these lasers by their wavelength, chromophores, and target tissues.
Laser Procedures
Laser-assisted dental procedures offer many advantages to both the dentist and patient. Many restorative procedures can be completed without anesthesia or the high-speed handpiece. The elimination of these two anxiety-inducing treatment features creates a less stressful procedure for both patient and provider, particularly when treating children. Postoperative discomfort is greatly reduced when performing soft-tissue procedures such as gingivectomy, biopsy, and frenectomy. Lasers can also be used to treat oral diseases such as aphthous stomatitis and recurrent herpes through a process known as photobiomodulation. Erbium lasers’ ability to cut bone less traumatically than burs makes them an excellent instrument for procedures such as crown lengthening and surgical extractions. Incorporating lasers also allows the primary care dentist to refer fewer procedures to specialists as they become more experienced and properly trained.
There are a multitude of dental procedures that can be done with lasers. Below are five examples of procedures in which lasers were used.
Operative Dentistry
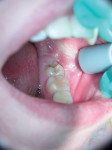
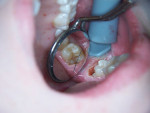
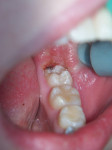
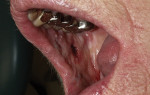
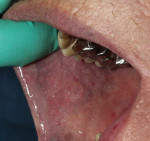
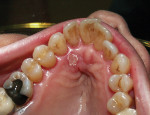
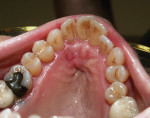
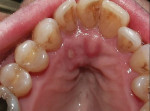
Caries was detected in the occlusal fissure of tooth No. 18 in a 14-year-old patient through visual/tactile inspection and use of the DIAGNOdent (DIAGNOdent, KaVo Dental, www.kavousa.com). The tooth had a fibrous operculum covering the distal half of the occlusal surface (Figure 1). Topical anesthetic was applied and a gingivectomy was performed using an Er:YAG tipless handpiece (LightWalker®, Technology4 Medicine/Fotona, www.lightwalkerlaser.com) (Figure 2). Once access was gained, the occlusal preparation was performed with the same laser, using the hard-tissue settings (Figure 3). The restorative portion of the procedure was achieved without local anesthesia, and the patient was comfortable throughout. The tooth was restored with GC Fuji IX™ GP Fast (GC America, www.gcamerica.com).
Endodontics
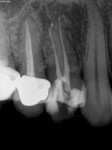
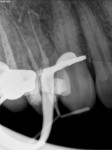
A laser-assisted irrigation process known as photon induced photoacoustic streaming (PIPS) has recently been developed for the LightWalker Er:YAG laser (Technology4Medicine/Fotona). Specially engineered tips are used along with extremely short digitally controlled pulses (50 millionths of a second) to create a powerful shockwave in the irrigant solution that is non-thermal.1 This energetic movement of solutions has been shown to more thoroughly clean the complex 3-dimensional root canal system than traditional irrigants.2 PIPS also allow for less aggressive instrumentation. Figure 4 and Figure 5 show a postoperative film of tooth No. 5 that was treated using the PIPS protocol. Multiple accessory canals are seen filled with cement (EndoREZ®, Ultradent) even though the canals were only prepared to a size 25 file.
Frenectomy
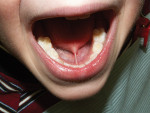
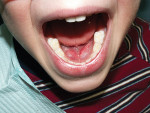
A 4-year-old patient with ankyloglossia and speech difficulties was treated with compounded topical anesthesia only and an Er,Cr:YSGG laser (Waterlase MD™, Biolase, www.biolase.com) (Figure 6 and Figure 7). The elimination of the needle and scalpel allows for a much lower anxiety procedure for both patient and provider.
Excisional Biopsy
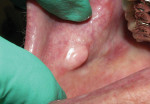
A fibroma on the buccal mucosa of a 70-year-old woman was excised with an Er:YAG laser (Technology4Medicine/Fotona), using only topical anesthesia (Figure 8 through Figure 10). No sutures were needed postoperatively. Excellent healing of the area was apparent 6 months after the procedure.
Recurrent Herpes Treatment
A 74-year-old woman who suffered from palatal herpes outbreaks two to four times a year received combined laser therapy using Nd:YAG and Er:YAG lasers (LightWalker) (Figure 11 through Figure 13). The Nd:YAG laser was used for photobiomodulation, and the Er:YAG was used to place a “laser band-aid” on the lesion. The patient experienced immediate and lasting relief. The picture on the right shows at 48 hours the lesion had already begun to re-epithelialize. These recurrent lesions were typically a 2-week ordeal for this patient.
Conclusion
Dentists who add lasers to their armamentarium find they can both expand the mix of procedures they provide and deliver them with predictably improved comfort for their patients. As with any new technology, proper training is paramount. Therefore, new laser dentists should pursue training opportunities provided by manufacturers and professional associations such as the Academy of Laser Dentistry.
Disclosure
Dr. Pohlhaus is currently a trainer for Technology4Medicine, LLC.
References
1. Peters OA, Bardsley S, Fong J, et al. Disinfection of root canals with photon-initiated photoacoustic streaming. J Endod. 2011;37(7):1008-1012.
2. DiVito EE, Colonna MP, Olivi G. The photoacoustic efficacy of an Er: YAG laser with radial and stripped tips on root canal dentin walls: An SEM evaluation. J Laser Dentistry. 2011;19(1):156-161.
About the Author
Steven R. Pohlhaus, DDS, FAGD
Private Practice
Linthicum Heights, Maryland
Dean’s Faculty
University of Maryland Dental School
Baltimore, Maryland
SOFT AND HARD TISSUE APPLICATION (1. through 3.) A gingivectomy was performed with the soft-tissue laser settings, then the occlusal preparation was performed with the same laser set on the hard-tissue settings.
RADIOGRAPHIC EXAMPLE (4. and 5.) Postoperative radiograph of tooth No. 5 after root canal using PIPS protocol with LightWalker Er:YAG laser.
CLINICAL EXAMPLES (6. and 7.) Frenectomy performed on 4-year-old patient with ankyloglossia and speech difficulties using topical
anesthesia only and an Er,Cr:YSGG laser. (8. through 10.) Patient before, at, and 6 months after fibroma excision with an Er:YAG laser. (11. through 13.) Lesion re-epithelialization had already begun 48 hours after this palatal herpes patient received combined laser therapy using Nd:YAG and Er:YAG lasers.