Dental Caries: Detection or Diagnosis?
The key to successful treatment lies in recognizing and dealing with the caries disease process, not just the end result.
Dental caries is a transmissible bacterial disease of the teeth that results from a pH-specific dysfunction of the biofilm. It is characterized by prolonged periods of low pH, resulting in net mineral loss of the teeth.1 The disease model is complex, with multiple factors playing a role in the process. Currently, multiple bacterial pathogens have been implicated in dental caries, expanding the mutans streptococci and Lactobacillus model.2,3 Additionally dental caries has recently been identified as having potential systemic effects on the body.4,5 Multiple studies now conclude that there are also hereditary factors involved in the dental caries process.6,7 Most recently, an older theory of dental caries has re-emerged; it proposes that dental caries is an inflammatory disease and occurs from inside the teeth.8 What is well known at this point is that dental caries is a complex disease, which continues to be the number-one disease among children in the United States and also plaques adults, often as a chronic disease.9-11
The dental profession has approached diagnosing and treating dental caries based mostly on a surgical or reparative model. Radiographs, oral examination, and instruments have been used to identify the early signs of the disease, and restorative procedures have focused on repairing the damage to the teeth. Currently, evidence-based dentistry (EBD) includes fluoride application recommendations to prevent dental caries as established by the American Dental Association (ADA) and recommends the routine use of fluoride varnish every 3 months on patients who are at moderate or high caries risk.12 Furthermore, the ADA has EBD recommendations for resin-based pit-and-fissure sealants for all “at risk” posterior teeth in both children and adults.13 Dentists should be routinely using new technologies for caries detection or the early identification of individual signs of the disease, and they also should be routinely using caries risk assessment to identify both patients who are at increased risk for dental caries and the individual risk factors for each patient in order to design an individual-specific treatment protocol.14
“Dental caries” is an often misused term. While dental caries is a disease process, the term is routinely used to describe white-spot lesions, cavitated carious lesions, or even radiographic radiolucencies. The term “caries” is incorrectly used to describe a multitude of things. “Caries detection” is a frequently misused phrase used primarily to describe the identification of cavitated carious lesions. A more technically correct term would be “carious lesion identification,” as dental caries is a disease. A simple analogy to understand this term might be that people get dental caries, while teeth get cavities or lesions. While this may seem trivial, it really merits discussion, because caries detection is a misnomer. Are we detecting a lesion in a tooth, or are diagnosing the disease within the individual? As the profession moves toward a risk-assessment-based model for diagnosing and treating dental caries, it is important to clarify the use of the terms “dental caries” and “caries detection.” A practitioner performing caries detection may identify signs of the disease—eg, a carious lesion in a tooth—without identifying the risk factors, other disease indicators, and diagnosing the disease in the patient. Restorative codes are not diagnostic codes. Therefore, practitioners researching caries detection technologies or caries risk assessment technology must decide what it is specifically they are trying to accomplish, because both technology types exist.
(Caries) Lesion Detection Technologies
Numerous new technologies have been developed recently to identify demineralization, the earliest sign of dental caries. Adding some of these new technologies to visual inspection and radiographic examination can improve detection and diagnostic outcomes. A recent study, however, compared the performance of fluorescence, radiography, visual examination, and the International Caries Detection and Assessment System (ICDAS) cavity classification system for accuracy in identifying lesion development at the D1 and D3 cutoffs. While the study report found that technologies contribute to the identification process, the authors cautioned that occlusal caries detection should be based primarily on visual inspection, while fluorescence-based methods may be used to provide a second opinion in clinical practice.15 For the practitioner, it makes sense to use multiple data points to make the best diagnostic decision for an individual patient, recognizing that visual inspection with magnification is still the strongest data.
Quantitative light fluorescence—now often referred to as QLF, or as laser-induced-fluorescence—has been reported in the dental literature for a long time. When laser light is directed at dental hard tissue, there is a shift in the wavelength of the light being emitted from the fluorescing tooth depending on the nature and density of the tissue. Laser light has the ability to provide transillumination of the tooth to identify demineralized zones.16
Digital imaging fiber-optic transillumination (DIFOTI) is a camera that identifies zones of demineralization and captures images of the illuminated tooth by recording the transmitted visible light.17 The exam can be made in real time as the practitioner moves the camera throughout the patient’s mouth. DIFOTI also has the advantage of being able to demonstrate changes in density interproximally.18 The DIAGNOdent (KaVo Dental. www.kavousa.com) is a 655-nm diode laser caries lesion detection device that was first introduced to aid in the identification of pit-and-fissure lesions.19 The device (Figure 1) is calibrated to the reflectance for each individual patient’s teeth, and there is both a two-digit and audible display. Many authors have previously described these hidden lesions, attempting to explain their cause and providing rationales for the best treatment. The DIAGNOdent brings additional quantitative data to the examination of occlusal pits-and-fissures, with recommendations for initial surgical intervention. Repeated studies indicate that the DIAGNOdent increases both the sensitivity and specificity in diagnosis when used as an adjunct to visual and radiographic examination.20 The Caries ID™ (Midwest Caries I.D.™ Detection, DENTSPLY Preventive, www.dentsply.com)) handheld device is also a diode or LED laser device that uses a wavelength of light to identify areas of demineralization. When zones of demineralization are displayed, the LED changes to a red color and there is also an audible beep tone. The Spectra instrument (Spectra® Caries Detection Aid system (Air Techniques, Inc., www.airtechniques.com<) is a laser caries illumination device that uses a 405-nm blue-violet LED or diode laser and an image-capturing technology. This illumination technology also is coupled with analytical (Visix) software, which then displays the zone of demineralization as a photograph of the tooth, and varying zones in differing colors of green, blue, red, orange, and yellow. The images can be stored, and then repeated examinations can demonstrate changes in the tooth. This can then provide objective data to determine the progression of lesions or the effectiveness of remineralization therapy.
Since the introduction of these technologies, several new caries lesion detection instruments are appearing in the dental market. The Canary system (Canary System™, Quantum Dental Technologies, www.thecanarysystem.com) (Figure 2) uses laser luminescence and photo-thermal radiometry to permit decay detection as deep as 5 mm inside the tooth and to a size as small as 50 µm. The new Carestream CS 1600 device (Carestream Dental, www.carestream.com.) (Figure 3) combines reflectance and fluorescence signals to help in the detection of suspicious incipient caries.
Caries Diagnosis Technologies
While the caries lesion detection technologies add potential diagnostic data for the dental practitioner, they are primarily designed to identify signs or indicators of the disease, and not to diagnose the patient’s risk level for the disease process itself. As the profession moves toward a risk-assessment–based diagnosis and treatment model for dental caries, new technologies aid in the diagnosis of the disease. The first step for a practitioner implementing this model is to begin with a standardized caries risk assessment form. While numerous caries risk assessment forms are available from a variety of sources, the form developed by John Featherstone MSc, PhD—who is professor of Preventive and Restorative Dental Sciences and dean of the School of Dentistry of the University of California at San Francisco—has been validated clinically. The form examines risk factors, disease indicators, and potential protective factors for each individual, collectively determining the patient’s overall caries risk status.
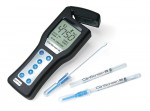
A new caries risk assessment form developed by CariFree (www.carifree.com) uses the risk factors and disease indicators from the Featherstone form. It is part of a new CTx System, and includes motivational interview questions along with a biofilm metric. For those practitioners who only want to screen known high caries risk patients, those forms are also available. For a biofilm metric, the CariScreen System (Figure 4) is a chairside real-time technology based on adenosine triphosphate-driven bioluminescence. This system has been demonstrated to correlate to the patient’s overall bacterial load on the teeth, levels of mutans streptococci, and independently to the patient’ caries risk status in independent studies.21-23 The Saliva-Check Salivary Testing Kit (GC America, www.gcamerica.com) is a real-time chairside test designed to check the quantity, pH, buffering capacity, and sugar metabolism potential of the patient’s saliva. These risk assessment forms and technologies are directed at identifying the potential risk factors, disease indicators, and the biofilm or systemic dysfunction of the patient. With the correct risk assessment diagnosed for the patient, appropriate targeted intervention therapies can be recommended to treat the disease.
Conclusion
The emerging biofilm science is changing how the dental profession looks at dental caries as a disease model. This more accurate but also more complex picture of dental caries anticipates the need for new technologies to better assess, detect signs (lesions), and diagnose signs of disease presence, progression, and activity levels. By early and accurate identification and diagnosis of dental caries, medical model therapies and minimally invasive surgical procedures provide patients with the best predictable treatment outcomes possible today.
References
1. Marsh PD. Dental plaque as a biofilm and microbial community—implications for health and disease. BMC Oral Health. 2006;(6 Suppl 1):S14.
2. Beighton D, Al-Haboubi M, Mantzourani M, et al. Oral Bifidobacteria: caries-associated bacteria in older adults. J Dent Res. 2010;89(9):970-974.
3. Tanner AC, Mathney JM, Kent RL Jr, et al. Cultivable anaerobic microbiota of severe early childhood caries. J Clin Microbiol. 2011;49(4):1464-1474.
4. Nakano K, Nemoto H, Nomura R, et al. Detection of oral bacteria in cardiovascular specimens. Oral Microbiol Immunol. 2009;24(1):64-68.
5. Abranches J, Miller JH, Martinez AR, et al. The collagen-binding protein Cnm is required for Streptococcus mutans adherence to and intracellular invasion of human coronary artery endothelial cells. Infect Immun. 2011;79(6):2277-2284.
6. Ozturk A, Famili P, Vieira AR. The antimicrobial peptide DEFB1 is associated with caries. J Dent Res. 2010; 89(6):631-636.
7. Wendell S, Wang X, Brown M, et al. Taste genes associated with dental caries. J Dent Res. 2010;89(11):1198-1202.
8. Southward K. The systemic theory of dental caries. Gen Dent. 2011;59(5):367-375.
9. Bagramian RA, Garcia-Godoy F, Volpe AR. The global increase in dental caries. A pending public health crisis. Am J Dent. 2009;22(1):3-8.
10. Kutsch VK, Cady C. MIX Disease: diagnosis and treatment. Inside Dentistry. 2009;5(7):80-83.
11. Takahashi N, Nyvad B. Caries ecology revisited: microbial dynamics and the caries process. Caries Res. 2008;42(6):409-418.
12. American Dental Association Council on Scientific Affairs. Professionally applied topical fluoride: evidence-based clinical recommendations. J Am Dent Assoc. 2006;137(8):1151-1159.
13. Beauchamp J, Caufield PW, Crall JJ, et al. Evidence-based clinical recommendations for the use of pit-and-fissure sealants : a report of the American Dental Association Council on Scientific Affairs. J Am Dent Assoc. 2008;139(3):257-268.
14. Young DA, Kutsch VK, Whitehouse J. A clinician’s guide to CAMBRA: a simple approach. Compend Contin Educ Dent. 2009;30(2):92-98.
15. Diniz MB, Boldieri T, Rodrigues JA et al. The performance of conventional and fluorescence-based methods for occlusal caries detection: an in vivo study with histologic validation. J Am Dent Assoc. 2012;143(4):339-350.
16. Kutsch VK. Lasers in dentistry: comparing wavelengths. J Am Dent Assoc. 1993;124(2):49-54.
17. Schneiderman A, Elbaum M, Shultz T, et al. Assessment of dental caries with Digital Imaging Fiber-Optic TransIllumination (DIFOTI): in vitro study. Caries Res. 1997;31(2):103-110.
18. Bin-Shuwaish M, Yaman P, Dennison J, Neiva G. The correlation of DIFOTI to clinical and radiographic images in Class II carious lesions. J Am Dent Assoc. 2008;139(10):1374-1381.
19. Khalife MA, Boynton JR, Dennison JB, et al. In vivo evaluation of DIAGNOdent for the quantification of occlusal dental caries. Oper Dent. 2009;34(2):136-141.
20. Goel A, Chawla HS, Gauba K, Goyal A. Comparison of validity of DIAGNOdent with conventional methods for detection of occlusal caries in primary molars using the histological gold standard: an in vivo study. J Indian Soc Pedod Prev Dent. 2009;27(4):227-232.
21. Pellegrini P, Sauerwein R, Finlayson T, et al. Plaque retention by self-ligating vs elastomeric orthodontic brackets: quantitative comparison of oral bacteria and detection with adenosine triphosphate-driven bioluminescence. Am J Orthod Dentofacial Orthop. 2009;135(4):426-427.
22. Hallett KB, O’Rourke PK. Oral biofilm activity, culture testing and caries experience in school children. Int J Paediatr Dent. 2009;(19 Suppl 1):4.
23. Fazilat S, Sauerwein R, McLeod J, et al. Application of adenosine triphosphate-driven bioluminescence for quantification of plaque bacteria and assessment of oral hygiene in children. Pediatr Dent. 2010;32(3):195-204.
V. Kim Kutsch, DMD
Private practice
Albany, Oregon