Rubberized-Urethane Composite for Provisional Restorations
The next generation of provisional resin materials shows improved physical properties and increased flexural strength.
An important key to success in fixed prosthodontics is the fabrication of an anatomic and hygienic provisional restoration. Temporary or provisional fixed restorations are used to protect the underlying tooth preparation while the laboratory fabricates the definitive restoration. No matter what materials or techniques are used, temporary restorations fulfill seven key purposes.
Main Purposes of Provisionals
Positional Stability
The provisional restoration holds the position of the prepared tooth both occlusally and proximally.1-4 If the tooth or teeth that have been prepared shift after the impression is made, the restoration returned by the laboratory will very likely need more adjustment before cementation. In the case of a multiple-unit fixed partial denture (FPD), tooth movement can cause a misalignment of abutment teeth so that there can be no path of draw with the abutment teeth.
Esthetics
For restorations in the esthetic zone, provisional restorations provide the patient an esthetic trial to ensure that he or she likes the color, contour, length, width, and shape of the teeth before the final porcelain-metal or porcelain restoration is fabricated.
Function
The provisional restoration returns the tooth to proper occlusal function, allowing the patient to masticate normally.
Phonetics
In the anterior region, the provisional restoration must allow the patient to speak normally and not interfere with speech and the creation of sounds.
Hygiene
The provisional restoration must be fabricated so the patient can maintain oral health and also aid in the healing of soft tissues that have been traumatized during tooth preparation and impressioning.
Preparation Evaluation
The provisional restoration can help the clinician determine whether adequate clearance and reduction of the tooth preparation for the final restoration have been accomplished.
Thermal Protection/Sealing
Once cemented, provisional restorations provide protection to exposed dentin and pulp between treatment appointments as well as seal out any bacterial invasion.
Fabrication
Fabricating temporary restorations requires proficiency with a variety of materials and techniques that can be used to make well-adapted and functional provisionals for crowns, FPDs, inlays, or onlays.2-4
Over the past decade there have been many changes to the materials and techniques that are used to fabricate provisional restorations for fixed prosthodontics. For years the standard for fixed prosthodontic provisional restorations has been acrylic resins, usually polymethylmethacrylates (PMMA). It is usually difficult to time the setting and working stages of the polymerization reaction of acrylics because of the inaccurate method of dispensing and mixing the polymer powder and liquid monomer. Acrylic resins also have poor physical properties, are sloppy to use, shrink on polymerization, generate significant heat during polymerization, have an unpleasant odor while setting, and there have been reports of allergic reactions.3,5-8 Over time these resins show significant wear in occlusal function, are susceptible to breakage, exhibit poor fit, and can become discolored.9,10
To overcome these deficiencies, new temporary materials with improved physical properties—bis-acrylics and rubberized urethane—have been introduced to simplify the fabrication of provisional restorations.1,6,11-13 Bis-acryl composite resins are typically dispensed in a double-barrel tube configuration where the catalyst and base pastes are mixed in automixing tips. Bis-acryl typically has significantly less shrinkage than acrylic resin because of the presence of radiopaque glass fillers that improve the fit of the provisional restoration to the tooth preparation.12 These glass fillers also improve the wear characteristics of the material. One problem with bis-acrylics is their brittle nature and potential for color changes.13,14
Recently, rubberized urethanes (Tuff-Temp™, Pulpdent, www.pulpdent.com), which is a new category of provisional resin, was introduced. While the setting reaction of rubberized urethanes is similar to bis-acrylics, the change in chemistry with the rubberized urethane is the insertion of a synthetic rubber molecule into a diurethane dimethacrylate resin, which improves the resin’s physical properties and increased flexural strength when compared to a traditional bis-acryl.15
Rubberized urethane has a wear-resistant Vickers hardness of 514 MPa, a compressive strength measured at 200 MPa, and a flexural strength of 75 MPa. This flexural strength translates into fracture resistance (less brittle) and impact resistance in occlusal function when compared bis-acrylics, allowing the rubberized urethane to be used for long-span FPDs as well as single-unit provisional restorations. Also, the resin-matrix–optimized filler configuration contributes to minimal shrinkage as well as an elasticity that these authors have seen contributes to improved provisional retention. The Tuff-Temp material is dual-cured, allowing for light-curing once the restoration is removed from the mouth. It is available in 50-mL or 5-mL cartridges in six shades, including a bleaching shade. The advantages of the rubberized-urethane composite for provisional restorations include:
- Because it is a filled composite resin, it is more resistant to occlusal wear than unfilled acrylic resin.
- It sets rapidly, and can be removed from the mouth after 90 seconds.
- It is flexible, so insertion and removal is easier.
- It has a lower flexural modulus to withstand occlusal forces and breakage.
- Trims with burs, diamonds, and disks.
- Has minimal polymerization shrinkage for better adaptation to preparations and minimal heat of polymerization.
- Does not adhere to teeth.
- It is radiopaque.
- It is dual-cure so it can be used in a self-cure mode or with a curing light at chairside.
- It can be easily repaired with a provided optimized flowable provisional add-on resin.
- It exhibits excellent color stability and stain resistance.
- Available in six shades, it is esthetic and slightly translucent.
- It gives off little odor when mixed.
- It can be polished or glazed with paint-on resin glazes.
Clinical Technique
Tuff-Temp is a dual-cure provisional resin, so it will self-set or, if desired, it can be light-cured. Provisional restorations can be fabricated intraorally or in the dental laboratory. The paste–paste formulation in a double-barreled automixing system undergoes a polymerization reaction where the first phase goes from a free-flowing paste with a working time of 45 seconds that, using any template, adapts to the tooth preparation and becomes elastic within 90 seconds (setting time). The second phase of polymerization can either self-cure for 2 minutes, 45 seconds, or the resin can be light-cured for a fast final set. This final phase of polymerization allows the resin to reach its final hardness in less than 4.5 minutes after initial mixing so that the restoration can be adjusted.
As with other provisional materials, there is an oxygen-inhibition layer on the resin that is easily removed with an alcohol-soaked 2x2 cotton gauze or simply by applying an oxygen-inhibiting gel prior to light-curing the material. Some clinicians accelerate self-curing time and the oxygen-inhibition layer removal by placing the temporary in a warm water bath. The resin should be trimmed and shaped with a slow-speed handpiece using abrasive disks, acrylic burs, diamonds, and rubber polishers. The Tuff-Temp has a companion light-cure glaze (Tuff-Temp Glaze) that can be painted on the provisional restorations to achieve a smooth and lustrous appearance before cementation.
When preparing adjacent teeth for single crowns, it is usually easier to fabricate the provisional restoration for all preparations as one unit.
Case Report
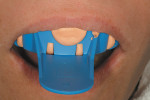
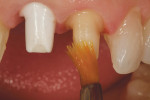
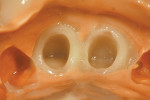
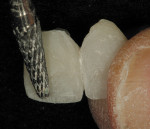
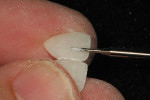
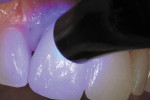
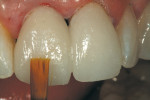
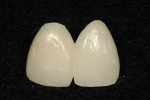
A template was created using a polyvinyl siloxane (PVS) heavy-bodied fast-setting impression material of a diagnostic wax-up in a disposable quadrant tray. The crown preparations were painted with a water-soluble lubricant and release agent (Wink, Pulpdent) to ensure easy removal of the provisional resin material when the template was removed (Figure 1). The PVS template of the maxillary central incisors was filled three quarters full using the automixing tip (45 seconds working time), filling the impression from the inside out. The PVS template was inserted for provisional restoration fabrication (Figure 2). Approximately 90 seconds after insertion (2 minutes, 15 seconds from the beginning of the mix) the impression was removed from the mouth. At this stage Tuff-Temp is slightly flexible and will pull over any undercuts or non-parallel preparations. When the template is removed the provisional restorations are usually in the impression (Figure 3). If the provisional restoration is still on the teeth, they can be teased off and then allowed to self-cure or be light-cured.
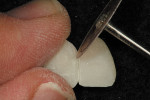
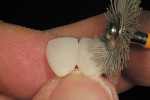
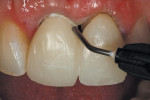
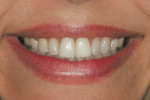
In this case, the provisional restorations were light-cured for 20 seconds and removed from the impression. The oxygen-inhibited resin layer was removed with alcohol. The restoration was finished and polished with an acrylic bur, diamond disks, and brushes and wheels with composite polishing paste before try-in (Figure 4 through Figure 7). After try-in, the restoration margins were adapted using a flowable light-cure add-on resin (Tuff-Temp Add-On Resin, Pulpdent) and light-cured (Figure 8 and Figure 9). The provisional was tried in and a resin glaze (Tuff-Temp Glaze) was applied and light-cured (Figure 10). The glaze creates an enamel-like smooth and lustrous surface (Figure 11). The highly esthetic anterior restoration was cemented with a eugenol-free provisional cement (PolyCarb WaterSet, Pulpdent) (Figure 12).
Conclusion
With the techniques described in this article, a clinician can reduce chair time by almost 30 minutes compared to using a self-cure acrylic resin for temporary crowns and bridges. These techniques will allow clinicians to fabricate high-quality, well-adapted, wear-resistant provisional restorations that are more esthetic than conventional acrylic resins.
Disclosure
This article was made possible in part by a grant from Pulpdent.
References
1. Strassler HE. In-office provisional restorative materials for fixed prosthodontics: Part 1- polymeric resin provisional materials . Inside Dentistry. 2009;5(4):62-67.
2. Gratton DG, Aquilino SA. Interim restorations . Dent Clin North Am. 2004;48(2):487-497.
3. Gegauff AG, Holloway JA. Interim fixed restorations. In: Rosensteil SF, Land MF, Fujimoto J, eds . Contemporary Fixed Prosthodontics. 4th ed. Maryland Heights, MO: Mosby Elsevier;2006:466-504.
4. Zinner ID, Trachtenberg DI, Miller RD. Provisional restorations in fixed partial prosthodontics. Dent Clin North Am. 1989;33(3):
355-377.
5. Powers J. Composite restorative materials. In: Craig RG, Powers JW, eds . Restorative Dental Materials. 11th ed. Maryland Heights, MO: Mosby Elsevier: 2002:231-258.
6. Driscoll CF, Woolsey G, Ferguson WM. Comparison of exothermic release during polymerization of four materials used to fabricate interim restorations . J Prosthet Dent. 1991;65
(4):504-506.
7. Fan PL, Meyer DM. FDI report on adverse reactions to resin-based materials . Int Dent J. 2007;57(1):9-12.
8. Altintas SH, Yondem I, Tak O, Usumez A. Temperature rise during polymerization of three different provisional materials . Clin Oral Investig. 2008;12(3):283-286.
9. Sham AS, Chu FC, Chai J, Chow TW. Color stability of provisional prosthodontic materials . J Prosthet Dent. 2004;91(5):447-452.
10. Young HM, Smith CT, Morton D. Comparative in vitro evaluation of two provisional materials . J Prosthet Dent. 2001;85(2):129-132.
11. Bis-acryl provisional materials . CRA Newsletter. 1997;21(2):3.
12. Provisional Materials . Adept Report. 1997;5(3):1-16.
13. Yilmaz A, Baydaş S. Fracture resistance of various temporary crown materials . J Contemp Dent Pract. 2007;8(1):44-51.
14. Rutkunas V, Sabaliasuskas V, Mizutani H. Effects of different food colorants and polishing techniques on color stability of provisional prosthetic materials . Dent Mater J. 2010;29(2):167-176.
15. Levine ED, Hack GD, Prymas SD. Using biomaterial investigative skills to assist in the clinical decision making process . J Dent Educ. 2011;75(2):190-256.
About the Authors
Howard S. Glazer, DDS
Private Practice
Fort Lee, New Jersey
Robert Lowe, DDS
Private Practice
Charlotte, North Carolina
Howard E. Strassler, DMD
Professor
Department of Endodontics, Prosthodontics, and Operative Dentistry
University of Maryland Dental School
Baltimore, Maryland