Simplifying Posterior Restorations
Achieve predictable and esthetic posterior restorations with a highly adaptive bulk fill composite.
Direct posterior fillings are the most common and frequently performed dental procedure.1,2 This does not change the fact that when the procedure is performed using direct composite resin, it requires twice the time as amalgam fillings and meticulous attention to technique. Among other considerations, alternately placing and curing multiple layers of composite is required to ensure complete polymerization and achieve a successful restoration.2-5
While this treatment modality has its advantages, it also has limitations. Polymerization shrinkage and inadequate adhesion cause marginal leakage and a persistent gap at the composite–tooth interface, resulting in postoperative sensitivity and caries.6 A a technique-sensitive protocol, if not performed correctly, can result in premature failure of direct posterior restorations.
Although some composites perform well in the anterior region due to their esthetic characteristics and high polishability, they lack the strength needed for posterior restorations. Others with limited esthetic qualities are better suited for posterior restorations based on their strength and wear characteristics.7 In the search for a material that eliminates many of these concerns, Tetric EvoCeram Bulk Fill was developed.8-10 Featuring a smooth consistency, it allows for enhanced cavity adaptation compared to other materials that often result in voids. Many of today’s bulk-fill composites reduce technique sensitivity, lessen the chances of shrinkage-induced failures,8-10 and demonstrate excellent handling and adaptability, resulting in the fast and easy placement of predictable and esthetic posterior restorations.11,12
Tetric EvoCeram® Bulk Fill (Ivoclar Vivadent, www.ivoclarvivadent.com) is comprised of layered silicates that produce a smooth and adaptable consistency, making it easy to fill cavity preparations up to 4 mm in one-layer applications, often eliminating the need for a flowable liner. In addition, polymerization has been intensified with the inclusion of the polymerization booster, which allows complete curing of 4-mm thick increments in 10 seconds while maintaining natural esthetics and adequate working time. Its composition also includes a shrinkage stress reliever, reducing the shrinkage stress distributed along cavity walls and surfaces, and the overall shrinkage volume experienced during polymerization.
Due to its adaptability and curability, it is possible to fill a Class II restoration in half the time with Tetric EvoCeram Bulk Fill compared to conventional materials. The composite conforms well to cavity walls and is easily contoured, allowing for anatomic detailing with conventional dental instruments and eliminating the need for additional equipment. Available in three universal shades (IVA for teeth in the “A” range; IVB for teeth in the “B” range; and IVW for quick deciduous fillings or light-colored teeth) and demonstrating an enamel-like translucency, Tetric EvoCeram Bulk Fill restorations blend seamlessly with natural dentition and are also easily polished to a high-gloss due to the material’s well-balanced filler composition. Tetric EvoCeram Bulk Fill provides the perfect combination of productivity, performance, and esthetics.
Case Presentation 1
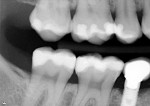
A 17-year-old woman presented with recurrent decay under a failing preventative restoration on tooth No. 30. The restoration had been performed about 10 years prior. She had not visited the dentist in more than 4 years. Radiographs revealed that the decay had moderately penetrated into the dentin layer.
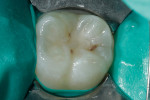
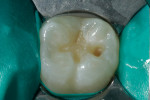
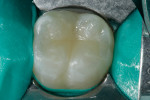
The patient was anesthetized using a 2% lidocaine block. A non-latex dam was placed and used as single-tooth isolation on tooth No. 30 (Figure 1). The existing restoration and decay were removed using a #330 bur (SS White Burs, Inc., www.sswhiteburs.comsswhiteburs.com), and sharp angles along the cavosurface margin were removed with a round #4 bur (SS White Burs, Inc.) (Figure 2).
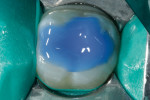
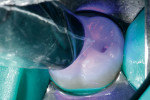
A 35% phosphoric acid-etch (Total Etch, Ivoclar Vivadent) was placed, agitated for 15 seconds, then thoroughly rinsed and lightly dried (Figure 3). Using a fourth-generation, two-step bonding system, the primer was agitated into the dentin for a full 10 seconds, then lightly dried to evaporate the alcohol. The adhesive was then applied onto the enamel and dentin, air-thinned, then cured for 10 seconds with an LED curing light (bluephase, Ivoclar Vivadent) (Figure 4).
Although the bulk-fill restorative (Tetric EvoCeram Bulk Fill) chosen for this case readily adapts to the cavity preparation, evaluation of the depth and size of the cavity is recommended to assess the appropriate amount of material required. Once preparation of the tooth is completed, a periodontal probe can be used to assess cavity depth. Another approach is assessing the depth based upon the length of the bur used to prepare the tooth.
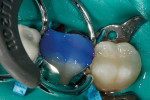
In this particular case, the deepest area of the preparation was 4 mm. Because this bulk-fill composite (Tetric EvoCeram Bulk Fill) cures up to 4 mm, it was applied in one single layer. Shade IVB (Tetric EvoCeram) was injected directly into the preparation until it slightly exceeded the margins, then was condensed to ensure intimate adaptation.
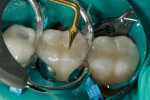
Once the material was placed, primary grooves and other detailed anatomy were incorporated into the tooth using a gold posterior occlusal instrument (Figure 5). A gold instrument was also used to smooth and blend the composite into the margins to eliminate the possibility of voids.
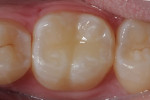
The restoration was light-cured for 10 seconds, then evaluated to ensure success before removing the rubber dam. The patient’s occlusion was checked and adjusted, and a final polish was performed using a series of diamond-impregnated silicone points and cups (OptraPol NG, Ivoclar Vivadent) (Figure 6). A high-gloss was achieved, eliminating the need for an additional layering composite and resulting in a strong, life-like restoration with good translucency, and accomplished with a simple and easy approach.
Case Presentation 2
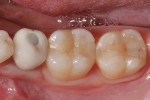
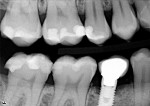
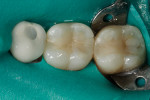
A 31-year-old woman presented with recurrent decay and rough margins/contours on teeth Nos. 30 and 31 (Figure 7). Radiographs revealed moderate decay on the distal of tooth No. 31 at an overhanging margin (Figure 8). The patient was anesthetized using a 2% lidocaine block. A non-latex dam was placed, leaving teeth Nos. 29 through 31 exposed (Figure 9).
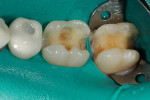
The existing restoration and decay were removed using a #330 bur, and sharp angles along the cavosurface margin were removed with a round #4 bur (Figure 10). A tofflemire band was placed on tooth No. 31.
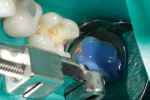
A 35% phosphoric-acid etch (Total Etch) was placed, agitated for 15 seconds, thoroughly rinsed, then lightly dried (Figure 11). Using a fourth-generation, two-step bonding system, the primer was agitated into the dentin for a full 10 seconds, then lightly dried to evaporate the alcohol. The adhesive was applied onto the enamel and dentin, air-thinned, then cured for 10 seconds with an LED curing light. A flowable composite was placed into the interproximal box as an initial layer, then light-cured a second time for 10 seconds. It should be noted that this particular bulk fill can be used with or without a flowable composite.
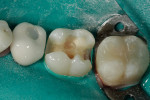
As with the previous case, the size and depth of the cavity was assessed to determine the appropriate amount of material required when using a bulk-fill composite. Because of the 4-mm depth, the bulk-fill composite was again applied in a single layer. The same shade was chosen, and the restoration performed according to the previous protocol and light-cured. Because the tofflemire band may have prevented complete curing of the restoration, once the band was removed, the restoration was light-cured from the facial and lingual of the interproximal areas to ensure a complete cure. A football carbide was then used to shape the contours and eliminate sharp angles (Figure 12). A sectional matrix system was then placed for tooth No. 30, and the same procedure performed (Figure 13 and Figure 14).
The restorations were evaluated to ensure completion, the rubber dam was removed, and the occlusion was checked and adjusted. A final polish was performed using a series of diamond-impregnated silicone points and cups (OptraPol NG), and a high-gloss was achieved, eliminating the need for an additional layering composite. The final restoration was life-like in appearance and exhibited superior radiopacity (Figure 15 and Figure 16).
Conclusion
Choosing a bulk-fill material that demonstrates excellent handling and material properties and facilitates easy placement, contouring, and polishing benefits dentists and patients by saving time while providing highly esthetic posterior restorations. Contrary to the characteristics of other bulk fills that often lack adaptability and make it difficult to attend to minute details, Tetric EvoCeram® Bulk Fill boasts excellent sculptability, allowing the addition of individual anatomic details. The optical properties contribute to true-to-life esthetics and allow dentists to fabricate restorations indistinguishable from the surrounding natural dentition. The numerous advantages demonstrated by Tetric EvoCeram® Bulk Fill, including dramatically reduced polymerization shrinkage, provide a fast and easy way to fabricate esthetic and predictable posterior Class II restorations.
References
1. Christensen GJ. Remaining challenges with class II resin-based composite restorations. J Am Dent Assoc. 2007;138(11):1487-1489.
2. Quellet D. Considerations and techniques for multiple bulk-fill direct posterior composites. Compend Contin Educ Dent. 1995;16(12):1212, 1214-1216, passim; quiz 1226.
3. Opdam NJ, Bronkhorst EM, Roeters JM, Loomans BA. Longevity and reasons for failure of sandwich and total etch posterior composite resin restorations. J Adhes Dent. 2007;9(5):469-475.
4. Lowe RA. The Search for a low-shrinkage direct composite. Oral Health Journal. March 2010.
5. Rodrugues Junior SA, Pin LF, Machado G, et al. Influence of different restorative techniques on marginal seal of class II composite restorations. J Appl Oral Sci. 2010;18(1):37-43.
6. Cheung GS. Reducing marginal leakage of posterior composite resin restorations: a review of clinical techniques. J Prosthet Dent. 1990;63(3):286-288.
7. Hervás-García A, Martínez-Lozano MA, Cabanes-Vila J, et al. Composite resins. A review of the materials and clinical indications. Med Oral Patol Oral Cir Bucal. 2006;11(2):215-220.
8. Roggendorf MJ, Krämer N, Appelt A, et al. Marginal quality of flowable 4-mm base vs. conventionally layered resin composite. J Dent. 2011;39(10):643-647.
9. Kuijs RH, Fennis WM, Kreulen CM, et al. Does layering minimize shrinkage stresses in composite restorations? J Dent Res. 2003;82(12):967-971.
10. Souza-Junior EJ, de Souza-Régis MR, Alonso RC, et al. Effect of the curing method and composite volume on marginal and internal adaptation of composite restoratives. Oper Dent. 2011;36(2):231-238.
11. Idriss S, Habib C, Abduljabbar T, Omar R. Marginal adaptation of class ii resin composite restorations using incremental and bulk placement techniques: an ESEM study. J Oral Rehabil. 2003;30(10):1000-1007.
12. Van Ende A, De Munck J, Mine A, et al. Does a Low shrinking composite induce less stress at the adhesive interface? Dent Mater. 2010;26
About the Author
Amanda Seay, DDS
Private Practice
Mount Pleasant, South Carolina