Direct Resin Posterior Restorations
Allowing adequate time for proper technique and using excellent materials are critical to long-term success.
Direct Class II posterior composite restorations are extremely popular. Unfortunately, studies examining the longevity of posterior composite restorations tend to be dated with variable results. In a 2007 study published in the Journal of the American Dental Association, researchers found that small amalgams and composites performed similarly, but that 50% of 4+ surface composites failed over a 7-year period, compared to 28.2% for amalgam.1 It has been suggested that posterior composites should be limited to smaller fillings due to the relatively low fees that insurance allows, and the fact that larger posterior composites cannot be done properly in the time frame that these low fees justify.2 The same author suggested that the survival of composite restorations varied greatly from one practitioner to another, implying that these restorations are technique-sensitive. In a recent retrospective study of one dental practice (presumably with good technique), after 12 years, composite restorations had a greater survival rate for low-caries-risk groups than amalgam (1.8% failure for composite vs. 12.2% for amalgam).3
It has been the author’s observation that moderate to large composite restorations can be highly successful when the dentist allows time for proper technique and uses excellent materials. As with any restorative procedure, oral hygiene, caries susceptibility, parafunctional habits, and other factors play a role in the longevity of the work. Dentists must always strive to understand the etiology of the patient’s problem before offering solutions. Composite is not the answer to every problem, but neither are any of the other materials at the clinician’s disposal. It is important that clinicians be aware that when adequate time is allocated—with an appropriate fee for that time— it is possible to place composite restorations that offer excellent longevity and value.
Technical Challenges with Posterior Composites
Achieving predictably excellent results with posterior composites is possible. The following tips (denoted in italics) address common problem areas with posterior composites and include ideas to help manage these problems.
Wear loupes (at least 3.25x). Nothing makes it easier to work on very small spaces than magnification. Use a rubber dam whenever possible. The rubber dam controls moisture, movement of the cheek and tongue, and humidity in the working field. When placed routinely, time is actually saved during the procedure. For patients who are nervous about the dam, the dentist can let them know that its use will prevent them from ingesting the old amalgam/mercury (when removing an old amalgam) and that it helps the dentist place a restoration that will last more predictably. For patients who are claustrophobic, the dentist can offer to place an airhole (an approximately 1-cm hole toward the anterior). In the author’s experience, this has made acceptance by reluctant patients close to 100%.
Prepare with a round-ended, non-cross-cut bur. The author uses an 1157 or 1158. Round internal line angles reduce the chance of stress-crack formation and they increase the ease of adapting the composite. Inspect for internal cracks. Internally cracked cusps or pulpal floors often lead to complications. When internal cracks are present, full-coverage restorations are often recommended. Patients should be informed that as a result of the cracks, symptoms that could lead to the need for endodontic treatment may develop. This short conversation at the time of treatment makes it much easier to manage patient relations related to addressing those teeth that do develop symptoms. Ensure complete removal of caries in the proximal box region—especially if using minimally invasive concepts. Clearly, if infected dentin or enamel is present, the new restoration will suffer early failure.
Properly adapt the matrix band. Use contoured sectional matrix bands, and consider one proximal at a time. On a mesio-occlusal-distal (MOD), the author recommends placement of two matrices, but only one wedge and ring. Etch and apply bonding agent to the entire preparation, then layer composite occlusal to the contact that has the wedge and ring. Move the wedge and ring to the other proximal and complete the restoration. Clinicians should ensure that the matrix is intimately adapted to the proximal box cervical margin. Improved proximal wall adaptation (and reduced finishing time) can be achieved with use of matrices such as the Composi-Tight® Gold (Garrison Dental Solutions, www.garrisondental.com) Composi-Tight® 3D (Garrison), or the Triodent V3 Ring® matrix (Triodent, www.triodent.com). After placing the matrix, wedge, and ring, a ball burnisher is used to provide final adaptation of the matrix.
Always etch enamel and dentin when appropriate for the bonding agent. After etching and bonding, sparing use of a flowable restorative material will help create a seal at the proximal cavosurface margins (along the matrix band) and along the internal line angles in the preparation. This seal helps to nearly eliminate proximal flash or overhangs and greatly reduces finishing time. Provide additional curing time in the proximal box for the bonding agent, the flowable, and the first layer of composite. The added distance from the light reduces light intensity and increases necessary curing time. Also, dentists should ensure the light is not missing the mesial aspect of the proximal box on second molars.
The use of bulk-fill composites is not recommended. To date, results for these materials have been disappointing. However, if an effective material is developed and verified with independent testing in the future, these materials may become more useful. Carefully adapt each increment to avoid voids.
Choose a material that has low shrinkage and radiopacity, handles well, has low wear, high fracture toughness and other physical properties, and maintains surface polish. Advanced clinicians may try sculpting the final increment of composite to final contour to reduce finishing time. This technique also proves absolutely necessary for dentists who are using multi-shade techniques for anterior teeth. Placement of appropriate shades in the correct 3-dimensional space is necessary to arrive at the correct shade and effects. The ability to not overfill each layer makes it possible to attempt multi-shade restorations.
Clinicians who are interested in building artistic skill for multi-shade anterior composites should consider using a different enamel shade for the final layer in their posterior restorations. This involves taking a basic body shade from the cervical one third, with the final enamel layer generally one to two shades lighter and fairly thin. The benefit of using an enamel shade for the final layer goes beyond the need for posterior restorations. Clearly, these restorations are generally very esthetic as single-shade restorations. When a thin enamel shade is used for the final layer in posterior restorations, and it is sculpted to near-final contour prior to curing, the dentist is able to practice layering in a setting in which he or she cannot fail. By learning to judge the effect of a second shade on the appearance of the final restoration, the dentist can build skill that will make it much easier to be successful with anterior restorations.
The Importance of Material Selection
A primary consideration in the success of any restoration is the material with which it is created. For direct restorations in the anterior and posterior, dentists need a material that offers low shrinkage, radiopacity, handling that is sculptable without being sticky, low wear, high fracture toughness and other physical properties, and an ability to maintain surface polish.
There has been a recent trend toward using bulk-fill flowable products in large restorations to save time, but the lack of long-term data on this practice should warrant caution on the dentist’s part. The most popular bulk-fill flowable has low-shrinkage stress, but the actual shrinkage is still believed to be approximately double that of top nano-filled and microhybrid composites.
The hybrid/microhybrid/nanocomposite category contains many excellent materials, but they are not all the same. Manufacturer claims can make it difficult to differentiate these materials. Some products claim universality, but they do not hold a polish. Others deceptively claim that only one shade is needed (true for some cases but not others, unless the dentist’s standards are low). Some may feel too firm to some dentists, while others may feel too sticky.
Understanding the differences between various composites requires a review of the evolution of composite fillers. The category of a composite has a strong effect on its suitability for any given indication. As most dentists know, these materials are classified by the size of their filler particles.4 The earliest versions of composite, known as macrofills, contained particles with sizes ranging from 10 μm to 50 μm. While this relatively large particle size made these materials strong, it also contributed to difficulties in retaining surface smoothness and resulted in relatively low wear resistance.4 These materials were soon supplanted in the market by microfills, which offered outstanding long-term smoothness due to their particle size under 100 nm. The drawback with microfills, however, is in their strength.5 Microfills are created by combining filler and resin and then polymerizing the material, after which it is ground into particles and combined with additional filler and resin. The level of filler loading of these materials is too low for indications that require strength or wear resistance; they are, therefore, typically advised only for use in anterior areas, where they are not under stress.6
The categories of hybrid, microhybrid, and nanohybrid have since been developed to occupy the middle ground between microfills and macrofills, attempting to achieve a balance between esthetics and strength. As with microfills, milling and grinding techniques are used to create the particles used in these composites.4 Hybrids are formulated with 10-μm to 50-μm particles as well as additional particles of approximately 40 nm in size.4 Microhybrids and nanohybrids range from over 1 μm to less than 100 nm.4,6 These formulations are designed to achieve both good strength and wear resistance through high filler loading. The disparity in particle sizes, however, can give rise to a problem in polish retention, as individual particles can be plucked out of the restoration during wear. As the effects of this abrasion mount, these composites lose reflectivity and polish.6 Most of today’s composites fall into this category.
However, a different class of material offers properties that address the drawbacks of each of these categories. A nanocomposite, distinct from a nanohybrid, is engineered via a chemical process that creates molecular-sized particles from the bottom up. These particles are then made into nanosized fillers. This technology has been patented by 3M ESPE, which applies it in its Filtek™ Supreme line of composites, the most recent generation of which is Filtek™ Supreme Ultra Universal Restorative. This composite is entirely composed of nanosized particles, with a primary size of 20 nm, but it differs from a microfill in that individual nanoparticles attach to one another to form nanoclusters. These nanoclusters allow for higher filler loading and increase the composite’s strength. Furthermore, as the material wears, only individual nanoparticles are worn away from the nanoclusters, leaving nanosized voids. This gives the material the ability to maintain an excellent level of polish over the long term.7
It is important to understand these distinctions in order to avoid the problems associated with using any composite as a universal material. Most composites are not universal. In addition, the frequency with which the term “nano” is applied to composite materials makes it difficult for most clinicians to understand the distinctions between them. There are several good materials that offer reasonable strength, shrinkage, and handling characteristics. However, for long-term polish retention combined with strength, the properties of the nanocomposite discussed here set it apart as a genuinely universal material. The following technique description demonstrates the steps for ensuring long-term success with this type of treatment in a case that shows its use in a moderate-sized posterior restoration.
Technique
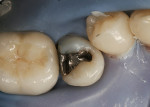
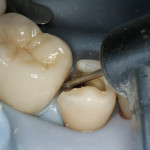
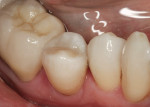
The patient seen here was going through a multi-year process of treating and repairing older dental work. Many teeth had failing amalgams without overt decay, but discoloration and small marginal discrepancies led the clinician to suspect decay for No. 29, the second to last tooth needing repair. The patient was also unhappy with the appearance of the amalgam in this tooth (Figure 1).
Recommended Technique
Use basic (occlusal) shade for smaller Class I and II composites. Mark occlusion to identify existing contact points. Administer anesthesia.
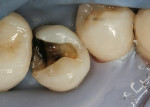
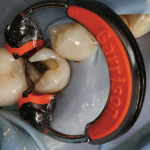
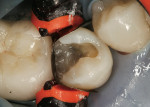
Place a rubber dam. This is not optional for predictable posterior composites. As noted above, cutting a 1-cm airhole just lingual to central incisors helps the claustrophobic patient tolerate the dam without compromising isolation. Using a new, round-end bur (such as an 1157), carefully remove old amalgam, if present (Figure 2). If there is an old composite, consider using a round-end diamond. (Using it dry allows the dentist to distinguish between tooth and composite, so that old composite is not left in the preparation, and also prevents over-preparation.)
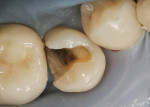
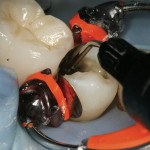
Remove decay (Figure 3). Evaluate the internal tooth structure for cusp or pulpal floor cracks. If pulpal floor cracks are present, a crown may be the treatment of choice. Consider extending the preparation to remove cracks that are through noncarious proximal walls. Refine the proximal boxes and internal preparation with rounded internal line angles. Rounding internal line angles reduces the odds of initiating cracks and optimizes the adaptation of the composite.
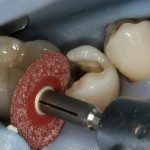
Place a slight bevel or exaggerated flair on the proximal box walls. Proximal walls must be free of decay and demineralization. It is possible that in a quest to be more conservative, dentists are sometimes incompletely removing damaged tooth structure, resulting in premature failure of the composite. This is not really a composite failure; it is a technique failure. Conservative preparations are desirable, but there must be sufficient preparation to ensure complete disease removal (Figure 4).
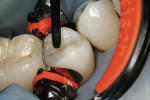
Place a slight bevel on the proximal box floor if it is still in enamel. If it is not in enamel, ensure a clean finish line (Figure 5). Polish adjacent old fillings if they are rough, and evaluate the margins with direct vision. Select and place a sectional matrix, wedge, and ring clamp. If it is an MOD, place one wedge lightly. Place only one ring clamp to the fully wedged side. After the first box is filled, the ring is switched to the other box before completing the composite placement (Figure 6).
Adaptation of the matrix to the tooth structure apical to the proximal box is essential, as is adaptation of the matrix to the full extent of the contact. In addition, adaptation of the matrix to the proximal walls is very helpful to reduce finishing time. At this stage, there should be a totally contamination-free restorative field; there should be no blood or saliva. Any contamination jeopardizes the longevity of the restoration (Figure 6 through Figure 11). Etch as appropriate for the bonding system being used. If etching, consider using chlorhexidine 2% after rinsing.
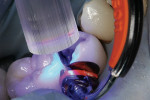
Apply a bonding agent—usually two coats—and light-cure. Provide an extended cure for this step and the first proximal layer to ensure an adequate proximal cure, due to the increased distance from the light tip to the material in the proximal box. Carefully apply a very thin layer of flowable composite along the matrix band–tooth interface (to create a seal) and along the internal line angles. Ensure that composite has flowed smoothly along the matrix band–tooth interface before curing (Figure 7). Cure composite and flowable in the proximal box for an extended time to compensate for the increased distance of the composite from the curing light (Figure 8 and Figure 9).
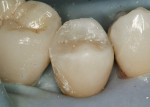
If the restoration is a MOD, complete composite placement against one matrix, then engage the second wedge and move the clamp to the second proximal. If there is not a threat of bleeding, consider removing the first sectional matrix. Layer composite in three or more increments with the final increment being the enamel shade, if using a separate enamel. Be careful to ensure that each layer is well adapted. The final layer can be sculpted to near-final contour prior to cure (Figure 10). Remove the clamp, wedges, and matrix (Figure 11). Do preliminary finishing and polishing, including evaluation of contact(s). Re-etch margins and seal with a very thin layer of bonding agent or gloss. Remove the rubber dam. Evaluate and adjust the occlusion (including upright chair position). Polish and show the patient the final results (Figure 12).
Discussion
Proximal box failures are most common with Class II composites. This can be due to recurrent decay, incomplete caries removal, margin failure due to a defective margin (poor adaptation or void), or leakage (bonding agent failure caused by under-curing or high polymerization stresses). Most of these problems can be avoided with excellent technique. Patients who have active caries (not just old failed fillings) must receive treatment and/or advice aimed at stopping the active caries process or they will continue to get caries— regardless of the restorative material.
Larger composites cannot be properly completed in the timeframe that is compensated for with standard insurance fees. Consider adjusting fees for larger composites rather than doing a poor job or just moving on to a crown. Moderate to large composites can save tooth structure and cost compared to the alternative onlay or crown, and they can be profitable to the dentist if fees are appropriately adjusted for the added complexity and time required.
For offices that have the freedom to apply a higher fee for direct restorations that require more time, communication is essential to help patients understand the value behind the treatment. In the author’s practice, patients are counseled regularly on the practice philosophy of performing minimally invasive dentistry, using the finest materials and adequate time for excellent technique. Patients are also informed that this philosophy does not always coincide with insurance reimbursement rates. In cases such as this, the aim is to provide a long-lasting restoration without removing healthy tooth structure, and this procedure takes time. Patients understand that the goal is not to simply charge more; it is to do better dentistry. By adjusting fees for the added complexity and time required for these restorations, moderate to large composites can save more tooth structure than the alternative onlay or crown, they can save the patient money over the alternative indirect restoration, and they can be profitable for the dentist.
Disclosure
Dr. Chyz is a stockholder in and an occasional unpaid consultant for 3M ESPE.
References
1. Bernardo M, Luis H, Martin MD, et al. Survival and reasons for failure of amalgam versus composite posterior restorations placed in a randomized clinical trial. J Am Dent Assoc. 2007;138(6):775-783.
2. Christensen GJ. Making Class II resin-based composite restorations predictable and profitable. J Am Dent Assoc. 2010;141(4):457-460.
3. Opdam NJ, Bronkhorst EM, Loomans BA, Huysmans MC. J Dent Res. 2010;89(10):1063-1067.
4. Ferracane JL. Resin composite—state of the art. Dent Mater. 2011;27(1):29-38.
5. Christensen, GJ. Categories of resin-based composite and respective brands. Clinicians Report. 2009;2(7).
6. Mitra SB, Wu D, Holmes BN. An application of nanotechnology in advanced dental materials. J Am Dent Assoc. 2003;134(10):1382-1390.
About the Author
Grant Chyz, DDS
Private Practice
Seattle, Washington