Removable Aligner Therapy Plus Conservative Porcelain Veneers
Achieving esthetic goals is possible without fixed orthodontic appliances using clear removable aligner therapy and minimally invasive porcelain veneers.
By Steven Glassman, DDS
Dentists need not be limited to orthodontic-only or restorative-only solutions to esthetic problems such as those experienced by the patient described in this article. The use of clear removable aligner therapy—in this case Invisalign® (Align Technology, Inc, www.invisalign.com)—in combination with conservative, indirect porcelain restorations, can be used together as an effective way to treat esthetic patient problems.
Evaluation
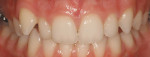
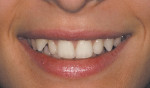
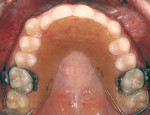
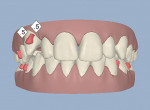
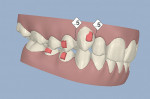
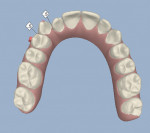
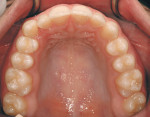
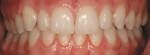
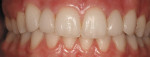
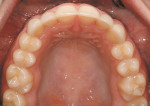
An 18-year-old woman presented in February 2009 for a second opinion. Her chief complaint was that the No. 6 canine was positioned high in the arch and in a labial position; she also had full bands on her molars (Figure 1, Figure 2, Figure 3, Figure 4, Figure 5, Figure 6, Figure 7, Figure 8, Figure 9). The treating orthodontist had recommended extracting tooth No. 6 to correct her crowding malocclusion. The patient had also consulted with a restorative dentist, whose treatment plan was to perform 10 porcelain restorations after endodontic therapy on tooth No. 6.
A full work-up was performed. A soft-tissue and temporomandibular joint examination was performed, and periodontal digital photographs were taken, cropped, and placed in a template. A set of study models and a facebow were also completed and then mounted in centric relation.
A full orthodontic evaluation was performed, which noted the following:
• A class II molar and canine relationship on the patient’s right side.
• A vertical issue to consider concerned the No. 6 canine that was high in the arch (about 2 mm) and flared labially.
• There was a slight class II (half a cusp) relationship on the patient’s left side in the canine and molar area.
• There was mild crowding on lower incisors from teeth Nos. 23 through 26.
• The upper and lower midlines did not concur.
• Rotations on teeth Nos. 5, 6, 20, and 29 were noted, with No. 6 being the most significant at over 30º.
• A slight tooth size discrepancy was noted on the maxillary laterals Nos. 7 and 10, with a chip on the mesial incisal edge of tooth No. 7.
Treatment Plan
Because the patient had refused fixed orthodontic appliances, clear removable aligner therapy was offered as a treatment modality. One method, Invisalign®, uses a software program called ClinCheck® (Align Technology) to visualize the prescribed treatment plan using the clear removable appliances. Aligners are worn full-time and removed only for eating and drinking. Each aligner is worn generally for 2 weeks.
Attachments and auxiliaries with elastics have been incorporated into the system to allow for more challenging movements such as extrusion, rotations over 30º, and root movements. Align Technology bases these movements on a database of more than 1 million patients as well as biomechanical research to optimize the forces delivered by the aligners via special features.
The patient was offered the following two options with Invisalign:
1. Class II elastics to achieve anterioposterior change, resulting in a class I molar and canine occlusion.
2. An esthetic-only solution that would address the patient’s chief complaint, the highly positioned tooth No. 6, as well as maxillary anterior leveling and mandibular crowding. The canine relationship would be improved through right-side interproximal reduction and retroclining tooth No. 6 into the arch.
In both treatment plans, the option of conservative restorative treatment was also included to treat the chipped edge of tooth No. 7 as well as the slight tooth size discrepancy. The patient, who was a performer, chose the second option because of its shorter treatment time and her concern that the class II elastics would be noticeable.
Invisalign Records Taken
Polyvinylsiloxane impressions (PVS), a silicone bite in centric occlusion, and eight photographs were submitted online with a prescription requesting a set-up based on the discussed treatment plan. The impressions were wrapped and shipped to Align Technology. From there, the impressions would be scanned with advanced technology and the digital information sent to Align Technology’s Costa Rica facility. A trained technician would create a 3-dimensional digital set-up based on the prescription.
ClinCheck Plan Review
A virtual set-up was created and visualized on the doctor’s portal through the Invisalign website, where doctors are given a unique username and login password.
Space was created using interproximal reduction totaling 1 mm mesial and distal to tooth No. 6 to allow the canine to retrocline into the arch. Power Ridges™ (Align Technology) for lingual root torque were placed on teeth Nos. 7, 8, and 9. Attachments were placed on teeth Nos. 5, 6, 20, 22, 28, and 29 to assist in rotations over 20º. Lower crowding was treated and canine relationships were improved.
The patient was seen at 6-week intervals to enable the clinician to monitor the fit of the aligners, check that the attachments were functioning, and assess the need for additional interproximal reduction. At the end of her 16th tray, the attachments were removed, five intraoral photographs were taken, and the case was evaluated for further treatment. It was decided that additional aligners would be needed to achieve the treatment goals, so additional PVS impressions were taken.
Second ClinCheck Plan
A second ClinCheck Plan was created for the doctor’s approval. Additional interproximal reduction was required to create more space to retrocline tooth No. 6 into the maxillary arch. Attachments were placed on teeth Nos. 5 and 6, and Power Ridges for lingual root torque were placed on teeth Nos. 8 and 9.
The patient was again seen at 6-week intervals, when the fit of aligners, attachment placement, and interproximal reduction was monitored.
Restorative Treatment
After the second phase of aligners was finished, an esthetic evaluation was made. Because of the age of the patient, a conservative approach was taken. After Invisalign treatment, there was a large incisal embrasure between teeth Nos. 6 and 7; in addition, as at the beginning of treatment, the incisal edge remained chipped on the distal. On both quadrants of the maxillary arch, the maxillary laterals appeared small due to the tooth size discrepancy, as noted in the diagnostic section above. Doctors proposed a treatment plan in which minimally invasive porcelain veneers would be placed on the canines and laterals. A diagnostic wax-up was performed on these teeth, leaving the centrals as they were.
From the diagnostic wax-up, a reduction guide was created for use in the preparation of teeth Nos. 6, 7, 10, and 11 for porcelain veneers. The case was scanned using a Cadent iTero™ scanner (Cadent Inc., www.cadentinc.com). This technology scans the prepared teeth from multiple angles and sends the scanned images to a milling machine off-site to create a durable die that the laboratory uses to fabricate the porcelain restorations. The matrix from the diagnostic wax-up was used to create provisionals using a bis-GMA material (Luxatemp®, DMG America, www.dmg-dental.com) that was spot-bonded on teeth Nos. 6, 7, 10, and 11. The patient returned a few days later to evaluate the provisionals. Once they were accepted, photographs and study models were taken and sent to the laboratory to provide additional information to the technician.
The patient was scheduled to try-in the case. After being anesthetized with local 2% Septocaine® (Septodont, www.septodontusa.com) with 1:100,000 epinephrine, the provisionals were removed and the case was tried-in with RelyX™ Veneer cement (3M ESPE, www.3mespe.com) try-in paste. Once the patient gave her approval, the porcelain veneers were cleaned, etched, silanated, and bonded with OptiBond® Solo Plus (Kerr Corporation, www.kerrdental.com) and clear RelyX Veneer cement. Afterward, the veneers were light-cured and excess cement was removed. The occlusion was checked for centric occlusion and excursions. An alginate impression was taken for an Essix®-type retainer (DENTSPLY Raintree Essix, www.essix.com) to prevent any relapse from the clear aligner therapy. The patient was instructed to wear these retainers full time until her next visit.
Finishing and Retention
The patient returned for a postoperative visit to check tissue response, contacts, and occlusion. The occlusion was checked (T-Scan® III, Tekscan Inc, www.tekscan.com) and a post-orthodontic occlusal adjustment was performed. At that time, PVS impressions were taken for a retainer system. The impressions were sent to Align Technology, where a stronger material retainer would be used for retention. The retainers are 30% stronger than the aligners and provide a series of four sets to be used over a 1-year period. The patient was instructed to wear her first two sets of retainers full-time for 6 months, followed by the second two retainers for nighttime wear only. The Align Technology retainer system’s proprietary material, ED4, is licensed under the name Vivera® (Figure 10, Figure 11, Figure 12).
Acknowledgments
The author would like to thank Dr. Debra Glassman, Jason Kim Dental Laboratories, and Align Technology for their assistance with this case.
About the Author
Steven Glassman, DDS
Private Practice
New York, New York