Outline of an Esthetic Case
Esthetic reconstruction of the maxillary arch, using the most advanced materials available, helps to achieve strength and replicated the qualities of natural teeth.
By Joseph L. Caruso, DDS, MS | Luke S. Kahng, CDT
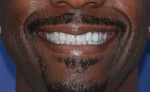
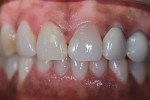
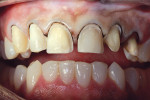
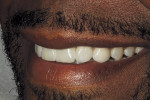
In the case presented in this article, a 44-year-old man consulted with the clinician for esthetic smile enhancement (Figure 1). His concerns were a fractured veneer on the maxillary right cuspid, recurrent decay on over-contoured porcelain-fused-to-metal (PFM) crowns on teeth Nos. 10 and 11, disparity of color on the maxillary anteriors, and the wish for a more masculine appearance.
Intraoral, extraoral, and temporomandibular joint clinical examinations were negative, and the patient enjoyed good health and took no medications. He experienced no allergies or known reactions to any dental medications, and his periodontal health was excellent with no pocketing in his dentition.
Clinical Analysis
Full-mouth digital radiographs revealed a missing porcelain laminate on the maxillary right cuspid, composite material on the mesial corner of tooth No. 9 to close the diastema between the central incisors, and an endodontic fill on tooth No. 8 with no periapical changes. In addition, a review of the radiographs revealed an impacted tooth lying horizontally in the maxillary left central and lateral area (Figure 2). A panoramic radiograph showed no pathology and indicated that no surgery was necessary. PFM crowns on teeth Nos. 10 and 11 were over contoured with extensive decay on the distal. No osseous defects were noted. Bone levels were excellent and no aberrant tissue levels were present.
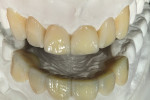
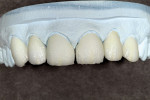
It was decided that the clinician would order a Kaleidoscope Treatment Plan Wax-Up™ (LSK121 Oral Prosthetics, www.lsk121.com) for confirmation of diagnosis and treatment planning suggestions (Figure 3). Both the clinician and the patient wanted to conservatively keep as much of the natural tooth structure as possible. They also agreed that they would like to prepare teeth Nos. 6 through 9 for porcelain veneers and place new full-coverage crowns on teeth Nos. 10 and 11. The patient was enthusiastic and fully accepted the clinician’s recommendations.
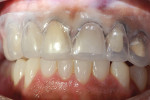
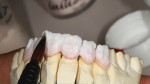
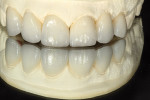
The technician’s wax-up provided the reduction coping necessary to allow the minimum but essential reduction to achieve harmony and a pleasant smile. The same reduction coping was also used for providing temporary acrylic restorations (Figure 4).
Communication is Essential
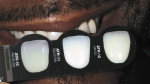
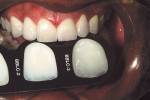
Communication between the patient, clinician, and laboratory is essential for functional and esthetic results and, in this situation, played a large role in the end result of this case. The technician traveled to the office to meet with the patient, understand his personality, and also his expectations. Custom shading was conducted at that time, and a series of photographs were taken. During custom shading, the patient was shown the amount of translucency and brightness of his color using the Chairside Shade Guide™ (LSK121 Oral Prosthetics) (Figure 5). Using this guide, the multiple choices available were easily illustrated for the patient. The patient chose between ATR 11 and ATR 12 (Anterior Translucency). To better ensure esthetics, function, and longevity of the restorations, as well as provide a happier patient, we can all benefit from this type of hands-on arrangement.
Preparation was begun using standard operating prosthetic procedures and diagnostic models were mounted using facebow and a Panadent Articulator (Panadent Corporation, www.panadent.com). Preparation for the laminate veneers was conducted in the gingival, midsection, and the incisal planes (Figure 6). Adequate reduction was necessary for esthetic restorations, requiring the appropriate amount of room. To prevent irritation and irreversible gingival tissue shrinkage, a medicated cord was placed into the sulcus. The margins of the teeth were carefully prepared with the cord in place to avoid gingival trauma. After preparation was completed, replacement of the two-cord technique was used for gingival retraction. Two full-mouth polyvinyl impressions were taken with custom trays. After the impressions were taken, centric relations were determined and facebow orientation was carried out with a Panadent articulator.
Laboratory Procedures
Florescence of the various GC ingots (GC America Inc., www.gcamerica.com) was measured under special lighting (Figure 7) to determine their color. After checking, the technician preferred to use GC Press material (GC America Inc.) for brightness and florescence. Figure 8 shows the appearance of the copings after divesting and pressing. Basic dentin bleaching color with modifiers was then applied (Figure 9). Using GC Initial™ Low Fusing porcelain (GC America Inc.), the final build-up was layered onto the copings (Figure 10). After polishing, the technician verified the color and shape of the restoration on the cast model (Figure 11).
After adequate time had elapsed, the final restorations were received.
Final Restorations
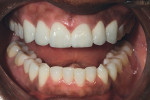
The provisionals were removed in the dental operatory using standard operating procedure. The final ceramics were then tried-in (Figure 12) for a translucency and color check with no adjustments required. The clinician bonded the restorations using the Ivoclar Variolink® System (Ivoclar Vivadent, Inc., www.ivoclarvivadent.com) with bonding protocol for all restorations. Variolink has a natural fluorescence within and luting material in a bleaching shade to further enhance vitality of the dentition. This helped with the masking of the dark color on endodontic tooth No. 8.
The patient was extremely pleased and delighted with the results. He was invited to and attended a lecture that the clinician and technician jointly presented about his case. His attendance greatly enhanced the presentation because his obvious happiness with the final outcome further supported the lecture synopsis.
All reconstruction patients are given a nightguard prosthesis as a precautionary measure to reduce the damaging effects of bruxating forces and to help lengthen the life of the restorations. However, knowing that proper incisal guidance was achieved with a wax-up, there was less concern over the possibility of fracturing from those forces.
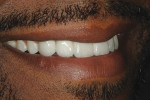
Two weeks after cementation, the restorations were checked in the mouth. Angulation, smile line, and incisal length (Figure 14 and Figure 15) were found to be pleasing and the patient’s full-face view shows his happy satisfaction with the final outcome.
Conclusion
Esthetic reconstruction of the maxillary arch, using the most advanced materials available, helped achieve strength and replicated the qualities of natural teeth. Science and technology have aided in the pursuit of duplicating natural tooth qualities such as translucency and florescence. Of note is the color disparity after the preparation of the dentin and how it varied because of the endodontic work for tooth No. 8 and the deep color of the dentin for tooth No. 6. Also, the long-standing PFM crowns on teeth Nos. 10 and 11 were not uniform in color or material. Science has addressed these optical differences in color with the newer materials and procedures available to the clinician and patient.
About the Authors
Joseph L. Caruso, DDS, MS
Private Practice
Chicago, Illinois
Luke S. Kahng, CDT
Owner LSK121 Oral Prosthetics
Naperville, Illinois