Biodentine Tricalcium-Silicate Cement
Material is an active biosilicate technology for direct and indirect pulp-capping.
By Howard E. Strassler, DMD | Robert Levin, DDS
There is generally little agreement on the treatment of a carious exposed pulp for a vital permanent tooth.1,2 A recent systematic review of vital pulp therapy in vital permanent teeth with cariously exposed pulps reviewed success rates of direct pulp-capping.3 In this review, the success rate of direct pulp-capping was reported as > 6 months to 1 year, 87.5%; > 1 to 2 years, 95.4%; > 2 to 3 years, 87.7%; and > 3 years, 72.9%. Partial and full pulpotomy sustained high success rates up to > 3 years (partial pulpotomy, 99.4%; full pulpotomy, 99.3%). The conclusion of this review was that vital permanent teeth with carious pulpal exposures can be treated successfully with vital pulp therapy. A retrospective study of direct pulp-capping by dental students evaluating radiographic outcomes reviewed cases that were pulp-capped at least 3 years previously both from mechanical pulpal exposures and carious exposures.4 The treatment for pulpal exposures was the use of a calcium-hydroxide liner for pulp-capping covered with a thicker base and a definitive restorative material. The results indicated a success rate for mechanical exposures of 92.2% and for carious exposed pulps, 33.3%. Larger preparations had less success, Class II (56.1%) than Class I (83.8%). The clinical implications of this study was that direct pulp-capping was recommended after mechanical exposure with immediate placement of a definitive restoration while endodontic therapy was the choice of treatment if the pulp exposure was due to caries. Of interest, direct pulp-capping of carious exposures did have some level of success.
There are many factors that can guide the clinician in making the decision to pulp cap or not. First and foremost, the type of pulp exposure plays a critical role in the potential for success—is it a carious exposure or is it a mechanical or trauma-injury pulp exposure. For each clinical situation, clinical data needs to be collected and evaluated when making a decision, which includes past history of pain, radiographic evaluation, pulp-vitality testing data, what restoration is treatment planned for the tooth, will adjunctive measures be necessary to salvage the tooth (endodontic treatment, crown lengthening, crown vs. an implant) and financial considerations. The goal is to keep the tooth. Pulp-capping of vital mechanical and traumatic exposure of the pulp if the field is kept aseptic can have a reasonable chance of success. To these authors, the choice of direct pulp-capping of carious exposures in vital, asymptomatic permanent teeth and restoring a tooth is a better choice than extraction.
Today, finances are a considerable driving force for patients’ treatment decisions. If the patient for financial reasons cannot afford endodontic therapy, consideration should be given for vital pulp therapy to retain the tooth. Vital pulp therapy can include direct pulp-capping or performing a pulpotomy covering the root canal orifices with bioactive pulp-capping materials. Successful vital pulp therapy is dependent on dentin–pulp engineering strategies using materials that have progenitor cell potentials and also interact with other non-progenitor, or “supportive,” cells.5 Under severe caries lesions, progenitor cells may be activated by growth factors released after the acidic dissolution of carious dentin.5 These strategies can lead to dentin regeneration.
Recent studies evaluating a medical-grade, calcium-silicate–based material (Biodentine™, Septodont USA, www.septodontusa.com) and techniques for vital pulp therapy have been very positive. As part of the chemical setting reaction of Biodentine, calcium hydroxide is formed. These studies have evaluated this bioengineered anti-inflammatory direct pulp-capping material histologically. Biodentine demonstrated the ability to induce odontoblast differentiation from pulp progenitor cells. The resulting mineralized matrix had the molecular characteristics of dentin.6 A clinical evaluation over 6 to 35 months of Biodentine as a base and for pulp-capping demonstrated biocompatibility and longevity.7 The initial data is very promising.
Biodentine is different from the usual dental calcium-silicate “Portland cement” materials. The manufacturing process of the active biosilicate technology of Biodentine eliminates the metal impurities seen in the “Portland cement” calcium silicates. The setting reaction is a hydration of tricalcium silicate, which produces a calcium-silicate gel and a calcium hydroxide. In contact with phosphate ions, it creates precipitates that resemble hydroxyapatite.8 An evaluation of the dentin–Biodentine interface demonstrated microstructural changes. Using confocal microscopy, there was an increase in the carbonate content of interfacial dentin, which suggested intertubular diffusion and mineral tags of Biodentine hydration products creating a hybrid zone.9 Also, Biodentine sets faster than other calcium-silicate cements, allowing it to be used as a liner and a dentin substitute base under definitive restorative materials.
Case Report
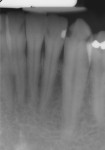
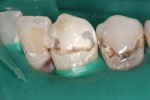
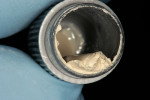
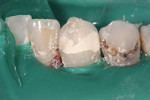
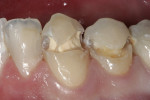
A 24-year-old patient presented with a deep carious lesion on the facial surface of the mandibular canine. There was no past history of pain, and the tooth pulp tested vital to EPT and cold test with no lingering pain. There was no radiographic evidence of periapical pathology (Figure 1). During caries removal with a spoon excavator hand instrument, a small carious pulpal exposure was visualized (Figure 2). Because there was no history of pain and the pulp was vital, the decision was made to do a direct pulp cap with Biodentine provided as tricalcium-silicate powder in a capsule. The Biodentine liquid is provided in a unit-dose form. The capsule was tapped on the tabletop several times to loosen the powder. After opening the dispensing bottle, five drops of the Biodentine liquid was added to the powder-containing capsule and the capsule was closed. The capsule was then mixed for 30 seconds at 4,200 rpm in an automatic mixer (triturator). When the capsule was opened, the mix had a putty-like consistency (Figure 3). The Biodentine was dispensed onto a mixing pad and was applied to the cavity preparation using an amalgam carrier. The cavity preparation was bulk-filled and the material was adapted and contoured using a plastic filling instrument, then allowed to set for 10 minutes. Excess restorative material was contoured with disks (Figure 4).
The primary author has been involved in physical property testing of Biodentine as a liner/base. During a typical restorative timeline, after liner/base placement, adhesive and composite placement, finishing and polishing, the restoration would not be functional for an additional 10 to 20 minutes. Based upon the physical properties, Biodentine can be placed as a liner–base, allowed to set for 5 minutes, and then the preparation can be restored with composite resin.
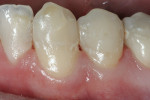
One month after placement, the tooth was evaluated for pulp vitality and tested normal to cold and EPT. The restorative material was removed, leaving a thin liner to not disturb the pulp cap, and the adjacent premolar was also prepared (Figure 5). The preparations were then restored with an etch-and-rinse adhesive and nano-hybrid composite resin (N’Durance®, Septodont USA) (Figure 6).
Conclusion
For caries-exposed vital pulps where there is already inflammation of the pulp, it is difficult to get a consensus on decision-making for direct pulp-capping. The goal for a permanent tooth with deep caries and the potential for exposure of pulp that is vital, asymptomatic, and exhibits no radiographic evidence of periapical infection is to maintain pulp vitality. An indirect pulp cap is preferable. A tricalcium-silicate cement (Biodentine) is a treatment choice. The patient needs to understand that the tooth is still at risk for need for endodontic treatment at a later time. Follow-up evaluations are crucial to evaluate pulpal vitality. To these authors, this innovative bioactive tricalcium-silicate cement is a “heroic” material. Its recommended clinical uses are for those clinical situations where the conditions are challenging and the prognosis is questionable. These clinical uses include restoring root perforations, restoration of internal and external resorption, and apexification.
References
1. Bergenholtz G, Spångberg L. Controversies in endodontics. Crit Rev Oral Biol Med. 2004; 15(2):99-114.
2. Ward J. Vital pulp therapy in cariously exposed permanent teeth and its limitations. Aust Endod J. 2002;28(1):29-37.
3. Aguilar P, Linsuwanont P. Vital pulp therapy in vital permanent teeth with cariously exposed pulp: a systematic review. J Endod. 2011;37(5):581-587.
4. Al-Hiyasat AS, Barrieshi-Nusair M, Al-Omari MA. The radiographic outcomes of direct pulp-capping procedures performed by dental students: a retrospective study. J Am Dent Assoc. 2006;137(12):1699-1705.
5. About I. Dentin regeneration in vitro: the pivotal role of supportive cells. Adv Dent Res. 2011;23(3):320-324.
6. About I, Laurent P, Tecles O. Bioactivity of Biodentine: a Ca3SiO5-based dentine substitute. J Dent Res. 2010;89:Abstract no. 165.
7. Koubi GF, Franquin JC, Colon P. A clinical study of a new Ca3SiO5-based material indicated as a dentine substitute. Conseuro 2009, Seville, Spain. March, 2009.
8. Colon P, Bronnec F, Grosgogeat B, Pradelle-Plasse N. Interactions between a calcium silicate cement (Biodentine) and its environment. J Dent Res. 2010;89:Abstract no. 401.
9. Atmeh A. Dynamic bioactive interface with dental tissues. 45th Meeting of the Continental European Division of the IADR (CED-IADR) with the Scandanavian Division (NOF). 2011; Abstract no. 1.
About the Authors
Howard E. Strassler, DMD
Professor
Department of Endodontics, Prosthodontics and Operative Dentistry
University of Maryland Dental School
Baltimore, Maryland
Robert Levin, DDS
Private Practice
Huntington Beach, California