Soft-Tissue Modification for Esthetic Results
The end result of cosmetic care is greatly enhanced when a frame is created that is balanced and properly positioned.
By Christopher J. Stevens, DDS
It is wonderful that dentistry has and can provide options. These options are great for clinicians but even more wonderful for the patients we are fortunate enough to serve. Restorative material options and tooth replacement options are part of everyday dentistry. Less common but no less important are choices available for tissue modification in cosmetic cases.
One of the first decisions that should be addressed is whether successful tissue positioning can be accomplished non-surgically, or if surgery such as osseous crown lengthening is required. Secondly, if only soft-tissue change is necessary, what tools are available to aid in those changes?
This author has used several different means over the years to change tissue position, depending on availability. These include rotary gingitage, electrosurgery, osseous crown lengthening, and laser modification. The case presented will demonstrate a thought process when determining, in consultation with the patient, what the best option will be for that individual.
Case Report
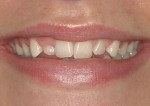
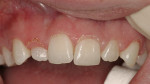
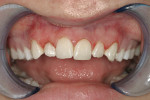
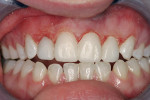
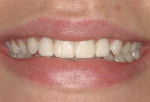
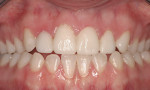
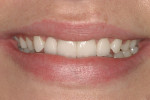
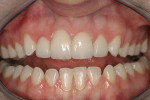
A 23-year-old woman presented to the author’s office on referral. She was a good friend of a patient who recently had her own smile enhanced. She presented with her mother and related the following concerns: she did not like that her two front teeth crossed; she did not like how small the tooth next to the front right one was; and she wanted her teeth to be whiter.
She related she previously had an option to get orthodontic correction but decided against it as it would have been during her senior year of high school. Another dentist had told her in the past that the small tooth on the right had never completely erupted. She related that she did not know how to smile as she had trained herself not to show her teeth when she smiled.
Clinical Esthetic Examination
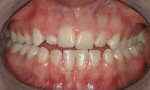
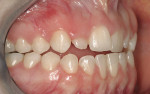
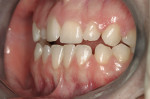
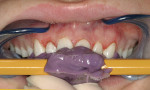
On examination, the author was able to appreciate her primary concerns (Figure 1, Figure 2, Figure 3 and Figure 4 ). Especially noticeable was the small visible size of the right maxillary lateral incisor. Additional observations were made, including irregular tissue heights on the central incisors, lingual inclination of the posterior segments contributing to a larger buccal corridor, and a low left cant relative to true horizontal.
Treatment Options
Various treatment options were discussed, including the number of teeth involved for the esthetic change as well as how to modify tissue heights. Digital cosmetic enhancement was performed with an option of the four anterior teeth or the twelve anterior teeth to include enhancement of the buccal corridor.
After digital photographic enhancement, the patient decided to treat the four anterior teeth. This decision was based on the buccal corridor not being a primary concern as well as a financial limitation. She also knew, after having discussed it in her consultation, that she would have the opportunity to treat more teeth at a later date.
Several concerns had to be addressed in regard to proper modification of the tissue. First was the excessive tissue on the right lateral incisor. Second was the significant difference between the central incisor gingival heights and malpositioned zeniths. Finally, consideration had to be given to the gingival cant, which was low on the left side.
Tissue Modification
The author’s goal was to have the zenith height of the central incisors level with the zenith height of the canines. The lateral incisors needed to be 0.5 mm to 1 mm lower. Further, the zenith position of the lateral incisors was in the middle of the long axis of the tooth, while the zenith position of the central incisors and canines was slightly distal to the long axis.
Relative to the tissue, the most challenging teeth would be teeth Nos. 7 and 9. The first decision was whether the tissue repositioning goals could be accomplished with soft-tissue modification only or would osseous surgery be needed. Periodontal measurements of the six anterior teeth were obtained. Tooth No. 7 had a 5-mm gingival pocket on the mid-facial and tooth No. 9 had a 3-mm mid-facial pocket measurement. It was determined that significant improvement could be made with soft-tissue changes only but the ultimate goal related above could not be achieved without osseous surgery.
There was much discussion about the pros and cons of each tissue option. It is this author’s opinion that prediction of the compromise is always better than excusing the compromise. Ultimately, it was the patient’s decision and she chose soft-tissue modification only. She realized the low left cant could not be entirely corrected, nor could the zenith heights of the central or lateral incisors be idealized. Despite this fact, an accurate portrayal of the end result via simulated digital smile enhancement demonstrated that a very satisfactory result could be obtained.
Preparation Visit
Use of an esthetic stick bite (more accurately, a horizontal stick reference) is of critical importance when changing gingival contours. The second tool used was the Smart US-20D CO2 laser (DEKA Laser Technologies, Inc., www.dekalasers.com) (Figure 5). This laser emits a wavelength of 10,600 nm, thus providing extremely high water-absorption characteristics, the major component of soft tissue. The peak power of the laser is as high as 320 W. DEKA’s proprietary UltraSpeed CO2 technology allows for shorter emission time and increased tissue relaxation time. This allows one to incise tissue with the speed of a scalpel while sealing blood vessels for a bloodless surgical field. The result is virtually no trauma to the surrounding tissues.
Using the repeat setting at 1.5 W and 50 Hz, along with the perio tip insert on the laser handpiece, an outline of the intended position could be drawn with guidance from the horizontal stick reference (Figure 6). Gingival zenith heights and positions were made to the pretreatment intention. In order to reduce bulk around the gingival margin after laser-assisted gingivectomy, laser peeling through low-level ablation was performed (Figure 7). The result of the soft-tissue management was verified with comparison to the stick reference (Figure 8). The concern over the remaining gingival height differential between the central incisors was reduced due to the low lip position during smiling.
Conventional veneer preparations were then accomplished. Digital impressions of the preparations were taken with the iTero™ (Cadent, Inc., www.cadent.biz) along with the virtual bite registration. Provisionals were fabricated using Integrity® (DENTSPLY Caulk, www.caulk.com). The patient was extremely pleased with the initial provisional phase (Figure 9).
A 10-day follow-up was scheduled to check healing and update the patient’s desires in provisional length and contours. Minor changes were made and an alginate was taken to relate these desires to the laboratory (Figure 10). Inspection of the tissue demonstrated healing to the desired contours (Figure 11).
Final Restorations
The provisionals were sectioned and removed after lingual anesthetization. The preparations were cleaned with Consepsis® scrub and liquid (Ultradent Products, Inc., www.ultradent.com). The final restorations were fabricated with IPS Empress® (Ivoclar Vivadent, www.ivoclarvivadent.com). They were fitted, both independently and as a group, to determine appropriate proximal contact, midline, length, and canting.
Once the patient accepted the restorations, they were removed, rinsed thoroughly, and etched with 37% phosphoric acid. Silane Primer (Kerr Corporation, www.kerrdental.com) was applied to the restoration followed by a translucent shade of RelyX™ Veneer Cement (3M ESPE, www.3mespe.com).
To prevent saliva contamination, a rubber dam was placed in a trough format and the palate was sealed with bite registration material. The teeth were etched for 12 seconds, washed, and moisture-controlled. OptiBond® Solo Plus™ (Kerr) was applied and conventional seating was accomplished. The patient was very pleased with the result (Figure 12 and Figure 13).
Conclusion
Gingival tissue is the frame for an esthetic smile. The end result of cosmetic care is greatly enhanced when a frame is created that is balanced and properly positioned. Clinical observations and patient input provide direction for care. In cases where alternatives exist, these must be discussed with the patient. When an option is chosen that is not ideal, the result must be demonstrated before the care is initiated allowing for predictable results. In this case, a soft-tissue-only option was chosen.
Having the proper tools, such as a CO2 laser, allows the clinician to achieve exceptional results even when the option chosen is not the provider’s primary choice. Some educators feel that there needs to be healing time before the veneer preparations are initiated. It is this author’s experience that, with the use of a CO2 laser, preparations can be done in the same visit as tissue framing. This technique creates a reduced healing time, reduced posttreatment discomfort, and stability in position and contours while healing.
Disclosure
The author is a paid consultant for DEKA Laser Technologies, Inc.
Acknowledgments
The author would like to thank Knight Dental Group of Oldsmar, Florida, for fabricating the restorations.
About the Author
Christopher J. Stevens, DDS
Private Practice
Sun Prairie, Wisconsin