Decreasing the Learning Curve
Achieving predictable posterior composite restorations with a new advancement in resin technology.
By Parag Kachalia, DDS | Marc Geissberger, DDS
As a result of a tremendous push for the development of high-quality materials, today’s resins display phenomenal physical properties with high filler content, low shrinkage, and high strength. Unfortunately while materials improved, little change was realized in the areas of technique. To achieve repeatable long-term success, practitioners were still asked to undertake a multistep composite layering technique to minimize shrinkage stresses and increase resin polymerization under a well-isolated field.1,2 In this method, many studies have shown great success with posterior restorations; however, these recommended techniques require a substantial amount of chairtime relative to amalgam dentistry. Until recently, the only true advancements in terms of efficiency have been the result of using high-powered LED curing lights that decrease polymerization times by 50% relative to traditional quartz-tungsten halogen lights.3,4
Bulk-fill composites, such as Tetric EvoCeram® Bulk Fill (Ivoclar Vivadent, www.ivoclarvivadent.com) or Quixx® posterior restorative (DENTSPLY Caulk, www.dentsply.com), allow restorations to be filled in one increment up to 4 mm; however, these materials tend to be highly viscous, making adaptation to gingival box forms challenging. In addition, these types of resins are generally more translucent and in order to achieve complete polymerization, restored teeth may exhibit a slight grayish tone upon completion of finishing and polishing. In a hybrid technique, bulk-fill approach, DENTSPLY and Heraeus (www.heraeus-dental-us.com) both released products that can be thought of as highly filled flowable composites. DENTSPLY’s SureFil® SDR® flow and Heraeus’ Venus® Bulk Fill are both self-leveling composites that can be placed in 4-mm increments in Class I or II restorations before curing. Their self-leveling properties allow a substantial, highly filled base to be placed that exhibits low shrinkage stress. Each of these resin base layers must then be capped by a traditional methacrylate-based composite that is designed to take an occlusal load.
While each of the aforementioned material advancements have led to efficiencies relative to the traditional layering techniques, they both have their limitations. An ideal restorative material in the authors’ opinion would have the ability to flow to depths of Class I and Class II restorations yet maintain the body of traditional composites to allow anatomical form to be placed. This material would also have the ability to be cured in a substantial increment.
SonicFill™ (Kerr Corporation, www.kerrdental.com) appears to fulfill these criteria. This new advancement in resin technology addresses the technique-sensitive aspects of posterior composite dentistry by applying sonic energy to a nano-filled composite resin. A special handpiece that is connected via a MULTIflex air connection transmits energy to a special compule containing the SonicFill composite. As the energy is applied while depressing a rheostat, the viscosity of the SonicFill resin drops as it exits the unidose tip, allowing it to flow across a class I or II cavity preparation. While maintaining the unidose tip in the preparation, the SonicFill resin volumetrically fills the cavity form before being withdrawn. On removal of the SonicFill compule and corresponding sonic energy, the resin quickly returns to a more viscous form, allowing the placement of anatomical form and blending of the resin into the surrounding morphology. Once the practitioner has completed sculpting the composite, the entire increment of composite up to 5 mm can be cured.5 The SonicFill composite has a highly efficient curing mechanism and its reduced opacity allows it to reach a complete cure in 20 seconds with a light output exceeding 550 mW/cm2. In cases where portions of the restorative preparation may be greater than 5 mm away from the light source being used, two increments of SonicFill should be used to ensure adequate polymerization.
Generally speaking, most direct restorations are within the 5-mm zone described above. In this range, practitioners are able to achieve a significant amount of time savings without sacrificing quality when compared to the traditional layering technique, bulk fill with flowable liner, or the new highly filled flowable composites paired with a capping composite technique.
Technique Comparison
All the techniques mentioned require traditional adhesive steps, so this component of the restoration remains constant regardless of whether the practitioner chooses a total-etch or self-etch adhesive technique.
In a traditional layering technique of a restoration that is 5 mm in depth, four individual layers of resin will need to be placed and each layer will have its corresponding curing time. An initial 0.5-mm layer of flowable composite will be followed by three additional layers of a traditional composite ranging from 1.5-mm to 2-mm increments.6 In this technique, each layer of composite should be adapted and fully polymerized. Conservatively speaking, a practitioner may spend 45 seconds to place and adapt each base layer prior to curing each layer for 20 seconds. The final layer, in which more anatomical form is placed and the resin is blended into the surrounding tooth structure, may take approximately 1 minute.
In the technique using the new highly filled, low-shrinkage, bulk-filled flowable composites, two layers must be placed. It is recommended that the initial layer be placed 1 mm to 2 mm shy of the occlusal surface and cured. This initial layer has the benefits of settling and reaching the depths of the class I or class II preparation. After waiting for the composite to settle for approximately 15 seconds, the practitioner can fully cure this layer for 20 seconds. After curing, a capping layer of composite can be placed, contoured, and cured. Relative to a traditional layering technique, significant time can be saved because only two layers are placed in the average 5-mm restoration instead of four, as in the traditional layering technique.
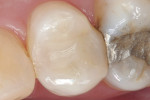
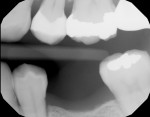
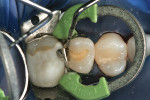
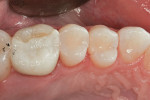
After traditional etching and bonding, a single layer of composite can be volumetrically placed in restorations up to 5 mm in depth. In a pilot clinical study conducted by the authors of this article at the University of the Pacific, Arthur A. Dugoni School of Dentistry, volumetric fill was achieved in an average of 40 seconds with the lowest time being 8 seconds. After the restoration was volumetrically filled, traditional anatomical form and contouring steps were taken before the restoration was completely cured. In the vast majority of cases a practitioner was able to completely restore a Class II restoration with proper anatomical form in less than 2 minutes. Final occlusal adjustment and polishing were in line with traditional materials and preferred techniques by the practitioner. These restorations were checked at recall intervals of 3 and 6 months. At these intervals, the restorations demonstrated a high chameleon effect as well as high a radiopacity on both small and large restorations (Figure 1 and Figure 2).
Technique in Detail
Administer the appropriate anesthesia for the tooth or teeth to be restored. While the anesthetic is taking effect, obtain the shade of the SonicFill composite to be used. Select a compule of composite from the available shades (A1, A2, andA3). Screw the selected composite onto the end of the SonicFill handpiece, ensuring that the compule has been tightened completely. Determine the speed at which the composite is to be expressed by rotating the speed dial to one of five speed settings (one is the slowest, five the fastest).
As with any adhesive restoration, proper isolation and infection control is essential to ensure long-term success. The tooth or teeth to be restored should be isolated using a conventional rubber-dam technique or a system such as Isolite. Ideally, multiple teeth should be isolated to help facilitate access during the preparation and restoration placement.
To help facilitate preparation and prevent adjacent tooth damage, the clinician should employ one of three devices designed for this purpose. The use of these protection devices not only prevents adjacent tooth damage, but they help to improve efficiency by allowing the clinician to create preparations more quickly. The three systems are WedgeGuard (Triodent, www.triodent.com); FenderWedge® (JS Dental Mfg., www.jsdental.com); and InterGuard® (Ultradent Products, Inc., www.ultradent.com).
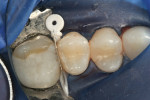
These wedges are also very effective at spreading adjacent teeth apart, which can aid in matrix placement and help to ensure a tight proximal contact. The tooth depicted in Figure 3 is being restored because of recurrent gingival decay.
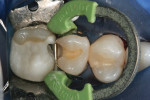
To obtain optimal anatomic contours, the authors strongly recommend the use of a sectional matrix system, such as the V3 System (Triodent) or Composi-Tight 3D™ (Garrison Dental Solutions, www.garrisondental.com).7 The bands in these system are curved to create appropriate embrasure form and help to establish a correct proximal contact. Proper placement of the matrix band itself can greatly enhance anatomic form. When selecting the matrix band, try to choose a band with occlusal–cervical height just taller than the preparation. This will allow the occlusal portion of the matrix band to be positioned at the height of the adjacent tooth. Too often clinicians attempt to employ a band that is too tall, positioning the occlusal edge of the band considerably higher than the adjacent marginal ridge height. When this mistake is made, it often leads to an overfilled restoration that will require considerable adjustment. Secure the sectional band with the systems accompanying wedge and ring. Burnish the proximal contact area of the band to the adjacent tooth’s proximal surface (Figure 4).
SonicFill composite is compatible with all adhesive techniques, which allows clinicians to easily adapt this new technology into clinical practice. It is very important to ensure that moisture is controlled during this portion of the restoration. Contamination can lead to premature failure and postoperative sensitivity. Following manufacturer’s instructions, place conventional fourth-, fifth-, or sixth-generation adhesive. In the case presented here, Optibond® Solo Plus™, a fifth-generation, two-step, total-etch system, was used.
Place the tip of the SonicFill compule in the deepest portion of the preparation. Step on the handpiece’s rheostat to begin the sonic activation and flow of the composite into the preparation. Use a fluid sweeping motion as the composite is expressed. Make sure that the tip of the compule is backed out of the preparation as the composite is expressed; this action will ensure that no voids are created during the placement. The rate of fill will vary depending on the speed selected. As you work with the system, you will be able to increase the speed at which you fill restorations. For restorations 5 mm or shallower, bulk fill the entire preparation (Figure 5). If the preparation is greater than 5 mm, fill the first 5 mm of the preparation, cure the material for 20 seconds, and then fill the remaining portion of the preparation.
After the composite has been expressed into the preparation under sonic vibration, the composite will quickly return to a sculptable, non-slumping state. Using a composite instrument, remove excess materials and establish occlusal anatomy. This can be accomplished quickly using an instrument such as the CompoRoller™ from Kerr. Once the composite has been appropriately contoured, cure the restoration for 20 seconds using a convention halogen or LED curing light.
Remove the sectional ring, wedge, matrix band, and rubber dam. Mark and adjust the occlusion. Finishing discs, such as OptiDisc® (Kerr Corporation), can be used to contour embrasures. Use a fluted carbide bur to adjust and modify the occlusal morphology as needed. Once the restoration has been appropriately contoured, final polishing can occur using any conventional rubber polishing points and cups for composite restorations (Figure 6).
Conclusion
All of the techniques presented in this article allow for the proper placement of posterior composites when the practitioner is properly trained and the learning curve is overcome. The SonicFill technology allows predictable and efficient posterior composite placement with a substantially decreased learning curve.
Disclosure
Dr. Geissberger has received an honorarium from Kerr Corporation for this article. Dr. Kachalia receives grant/research support from Sybron Dental.
References
1. Deliperi S, Bardwell DN. An alternative method to reduce polymerization shrinkage in direct posterior composite restorations. J Am Dent Assoc. 2002;133(10):1387-1398.
2. Nikolaenko SA, Lohbauer U, Roggendorf M, et al. Influence of c-factor and layering technique on microtensile bond strength to dentin. Dent Mater. 2004;20(6):579-585.
3. Busemann I, Lipke C, Schattenberg A, et al. Shortest exposure time possible with LED curing lights. Am J Dent. 2011;24(1):37-44.
4. de Jong LC, Opdam NJ, Bronkhorst EM, et al. The effectiveness of different polymerization protocols for class II composite resin restorations. J Dent. 2007;35(6):513-520.
5. Thompson J. Laboratory Research Report: Evaluation of SonicFill Composite. NOVA Southeastern University, October 2010.
6. Korkmaz Y, Ozel E, Attar N. Effect of flowable composite lining on microleakage and internal voids in Class II composite restorations. J Adhes Dent. 2007;9(2):189-194.
7. Saber MH, Loomans BA, El Zohairy A, et al. Evaluation of proximal contact tightness of Class II resin composite restorations. Oper Dent. 2010;35(1):37-43.
About the Authors
Parag Kachalia, DDS
Director of New Technologies
Course Director, Fixed Prosthodontics
University of the Pacific
Arthur A. Dugoni School of Dentistry
San Francisco, California
Marc Geissberger, DDS
Associate Professor
Chair of the Department of Restorative Dentistry
University of the Pacific
Arthur A. Dugoni School of Dentistry
San Francisco, California