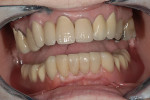
Diagnosis and Management of Porcelain-Induced Wear with Compensatory Eruption
Satisfying patient wishes and minimizing damage to surrounding dentition must be considered when prescribing porcelain-based restorations.
Mark L. Pitel, DMD
The exact reasons for it may be uncertain, but as we move into the second decade of the 21st century, dentists are encountering more patients who have successfully maintained all or most of their natural teeth well into their senior years. As such, everyone needs to be more concerned with the durability and long-term consequences of their treatment decisions. It may seem obvious that the most conservative treatment option that meets a patient’s clinical needs and preferences should always be the treatment of choice. Yet as dentists and patients churn through the cycle of restoration and re-restoration, the endpoint is often a porcelain-fused-to-metal (PFM) crown or bridge being retained by a natural tooth or dental implant.1 These restorations may be clinically appropriate, but cannot be considered conservative for the tooth being restored. The same holds true when these restorations are placed into occlusal contact with unrestored natural teeth or other dental work.
The increased popularity of cosmetic dentistry, with its emphasis on the bonded porcelain laminate or all-ceramic crown, has contributed to a growing number of natural teeth and other dental restorative materials that end up in occlusion with ceramic restorative materials. Dentists are trained that porcelains can cause more abrasive wear to natural teeth than other restorative materials.2,3 However, this process normally takes place very gradually, and may be difficult to recognize until considerable damage has already been done. The proximate damage can include loss of natural tooth structure, reduced longevity of opposing restorations, and even unfavorable changes to the vertical dimension of occlusion or the occlusal plane.4 Therefore, restorative treatment plans should always account for the presence and location of existing ceramic restorations. When new porcelain-based restorations are prescribed, it is very important for the restorative dentist to take the age of the patient and the condition of the opposing dentition into consideration. Once placed, the dentist must carefully monitor the patient for iatrogenic damages that may be caused.
Dental History and Current Findings
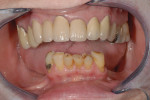
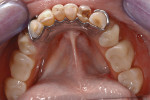
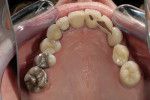
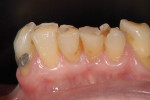
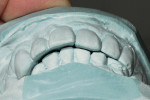
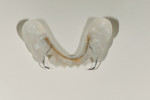
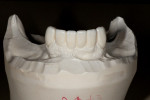
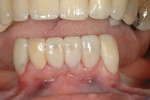
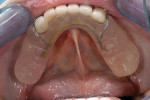
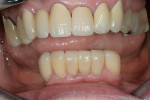
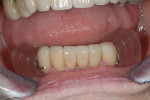
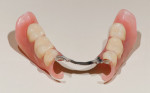
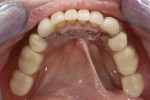
The case being discussed here is highly relevant because it documents clinical features commonly seen in the older, partially dentate patient. The 81-year-old female patient in this case lost all of her posterior mandibular teeth in the early 1960s, but has retained her mandibular anterior teeth from canine to canine (Figure 1). The missing posterior teeth were eventually replaced with a conventional removable partial denture (RPD) using a cast-metal frame and clasps, and acrylic denture teeth and saddles (Figure 2). The original mandibular RPD was replaced in 1974, and again in 1984, with similarly designed prostheses. The patient’s maxillary arch was better preserved. It was well restored to a first-molar occlusion with an assortment of PFM crowns and bridges, porcelain onlays, and a few amalgam fillings (Figure 3).
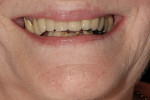
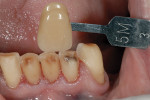
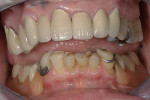
The plane of occlusion appeared to be very uneven, with significant extrusion of the maxillary premolars and molars bilaterally, and a significant cant from anterior to posterior and right to left (Figure 4). The extrusion was noticeably worse on the right side, which may have accounted for the right-to-left cant of the occlusal plane. The patient’s remaining mandibular anterior teeth were largely unrestored, but showed signs of significant wear and breakdown (Figure 5). As might be expected, the patient’s chief complaint was the poor condition and unesthetic appearance of her lower anterior teeth. Their condition was made particularly noticeable because the maxillary teeth were so well restored. Cases such as this one may have many viable restorative options, but any plan of treatment should begin with a detailed diagnosis of present conditions and a clear understanding of the etiology of any current pathology.
Diagnosis
Because the patient’s chief concern was the restoration of her mandibular anterior teeth, this was where diagnosis and case analysis began. These teeth showed obvious signs of wear, which can be etiologically linked to the use of full-coverage porcelain restorations on the opposing maxillary teeth, and a lack of a mutually protected occlusion.
Cases that involve significant wear always present specific challenges and concerns.5 In these cases, three critical questions must always be answered: Will there be sufficient vertical space available for the planned restorations? Will there be sufficient remaining tooth structure to support the planned restorations? What can be done to prevent the patient from damaging their new restorations in the same way they damaged their natural teeth?6
The patient must also be evaluated for changes to their vertical dimension of occlusion (VDO).7 One might automatically expect to find a loss of occlusal vertical dimension in cases of substantial wear, but this is not always the case. Many occlusion experts now believe that the losses from occlusal, incisal, and palatal surfaces are offset by compensatory eruption of the alveolar bone surrounding the worn teeth, except in cases of extremely rapid wear.8 These super-erupting teeth may result in a disruption to the plane of occlusion, but a stable VDO is usually maintained. True losses in VDO can be readily recognized by one or several of the following clinical signs or changes: severe wear of natural teeth; thinning of the lips; the tip of the nose appears too close to the chin prominence; the corners of the mouth downturn when the patient closes; there is heavy wrinkling in the patient’s chin and cheek areas; there is excess freeway space when the patient’s lips are lightly touching; and there are neuromuscular or TMJ complaints.
Except for wear, the patient in this case had none of the classic signs of a loss in VDO. In fact, these clinical findings can only be explained by the fact that the patient maintained a constant VDO throughout her life. To better comprehend how this could have occurred, it was necessary to explore how the patient may have deviated from the ideal. An ideal dental occlusion requires anterior–posterior coupling, or what has been commonly referred to as a “mutually protected occlusion.” The anterior teeth protect the posterior teeth and the TMJ by ensuring their disclusion during mandibular opening and eccentric movements via incisal guidance and canine rise.9 The posterior teeth in turn protect the anterior teeth by carrying the majority of the vertical occlusal load during function, and by maintaining the VDO.
Premature loss of this patient’s posterior mandibular teeth not only shifted heavier functional loads to the anterior teeth, but significantly destabilized her plane of occlusion. The tissue- borne removable partial dentures (RPDs) she wore for nearly 50 years may have improved cosmetics and function, but did not adequately support her occlusion.10 As the acrylic denture teeth slowly abraded, the opposing natural teeth super-erupted in order to maintain occlusal contact. Anteriorly, the patient’s natural mandibular teeth were opposed by porcelain restorations for an extended length of time, which would not be ideal under any circumstances. Without the benefits of a mutually protected occlusion, the mandibular teeth wore even faster.
Compensatory eruption of these teeth assured there was no overall change to the patient’s VDO. While the VDO may have been stable, the multiple areas subject to compensatory eruption allowed the occlusal plane to become badly distorted and canted. Unfortunately, definitive correction of the occlusal plane defects in this case could not be addressed with restorative dentistry alone. Adjunctive orthodontic intervention and possible periodontal surgery would be required to produce a level plane of occlusion. Regardless of the patient’s age, the additional value of these adjunctive options should always be considered and communicated to the patient.
Discussed below are the viable treatment options that could be considered in this case, and they are listed sequentially from most conservative to least conservative.
Option 1
The first, and most conservative, option considered was porcelain veneers on teeth Nos. 22 through 27, and reuse of the existing mandibular RPD.
The first objective was to address the patient’s chief complaint, and eliminate or further reduce the damage to the mandibular anterior teeth. To accomplish this, these teeth needed to be restored with porcelain for maximum durability and esthetics, and to help neutralize the excessive wear rate. Because the periodontal status and crown/root ratios of these teeth were favorable, the most conservative treatment option would be to simply place six porcelain laminate veneers on teeth Nos. 22 through 27. Although her existing partial denture was not especially esthetic or ideal for posterior support, it might be reused if the lingual surfaces of the mandibular teeth were not disturbed, and the metal retention clasps could be adapted or replaced to fit the new contours of teeth Nos. 22 and 27. Her mandibular anterior teeth easily met the requirement of sufficient tooth structure to properly retain the proposed restorations. However, a preliminary analysis of properly articulated diagnostic models demonstrated that the compensatory eruption left inadequate vertical space to esthetically or functionally restore those teeth. As such, this option had to be dismissed (Figure 6).
Option 2
The second option considered was to open the VDO, place porcelain veneers on teeth Nos. 22 through 27, and a new partial denture at the new VDO (ideally with porcelain teeth).
To address the vertical space deficiency for the planned restorations for teeth Nos. 22 through 27, the only available option would be to open the existing VDO. From a neuromuscular standpoint, this patient was asymptomatic, and was presumed not to have lost significant VDO. This meant that she would not be restored to a previous physiologic condition. Rather, she would be opened beyond where she had been functioning comfortably. Within limits, this is usually possible, as patients are remarkably accommodating. Altering the VDO, however, will always affect function, dental, and facial esthetics, and may cause unfavorable TM joint or neuromuscular symptoms as well as changes in speech.11 Therefore, it is imperative to clinically test even a minimal change in VDO, and validate that it can be well- tolerated by the patient before committing to the proposed treatment plan.12
Opening the VDO would solve the vertical space issue, but it would also greatly increase the complexity, cost, and time of treatment. Any change to the VDO also affects the anterior and posterior teeth. According to the literature, there is an approximately 1:3 vertical dimension increase ratio between the second molars and the central incisors, respectively.13 As such, there is a 3-mm opening created at the central incisor region for every 1-mm opening at the second-molar region. Analysis of the pretreatment study models indicates that 2 mm to 3 mm of additional space would be needed anteriorly, which means that an opening of nearly 1 mm would occur posteriorly. If this alteration were to be made to the VDO, the possibility of being able to reuse the existing mandibular RPD would be impractical. So, the reworking of the posterior occlusion meant that a new prosthesis would be required. The most conservative option would be to create a replacement prosthesis with porcelain teeth, to reduce wear rates and better stabilize the posterior segments.
Option 3
The third, and least conservative, option was to open the VDO, place porcelain veneers on teeth Nos. 22 through 27, and a complete implant reconstruction of the posterior dentition with PFM restorations.
Given how the patient’s existing RPD had contributed to current clinical conditions, it would seem prudent to offer a fixed treatment option that definitively addressed this problem. Absent of any mandibular posterior teeth, fixed bridges retained on natural teeth obviously could not be offered. Based on the location and extent of the patient’s missing teeth, PFM crowns supported by mandibular dental implants would be the only possible fixed restorative option that would come close to restoring anterior/posterior coupling and provide the function and proprioceptive advantages of natural teeth. Mandibular implants normally carry a very high rate of clinical success, if the patient is willing to accept the associated physical, financial, and temporal requirements. One possible concern with the clinical outcome was this patient’s long-term use of the oral bisphosphonate drug Fosamax to treat osteoporosis. Patients taking bisphosphonate drugs orally as opposed to intravenously are believed to carry a low risk of developing bisphosphonate-associated osteonecrosis (BON). However, patients who have used one longer than 3 years should be advised of an increased risk, or choose an alternate treatment plan.14 In this case, the patient decided not to assume the potential risks and additional clinical and financial requirements of dental implants. Therefore, this treatment option was declined.
Additional Treatment Considerations
Each treatment option can have many variations in a case such as this. For example, changing the individual porcelain laminate veneers on teeth Nos. 22 through 27 to a fixed porcelain-to-metal splint might be reasonable. This would permit more rigid support of the RPD and open up improved and esthetic retention possibilities such as precision or semi-precision attachments. However, this option is not as conservative as the prior treatment plans, and would significantly add to the time and cost of treatment. This option was considered and discussed, but ultimately declined by the patient.
Case Report
After considering all of the possible options, the patient agreed to the second treatment option. This called for an opening—approximately 2 mm to 3 mm anteriorly—in the vertical dimension of occlusion. To study the impact of this change on the occlusion and the patient’s ability to tolerate it, a temporary diagnostic/treatment partial denture was used. The denture was fabricated from clear orthodontic resin, which helped keep the cost down and made easy adjustments or additions to the occlusion possible (Figure 7). Wrought wire clasps were used to provide retention to the right and left mandibular canines. This allowed the treatment denture to be adjusted to fit her existing natural teeth, provisional restorations to be done, and to work temporarily with the final restorations. The patient wore the temporary partial denture for approximately 60 days without incident or development of any TMJ or neuromuscular symptoms.
With the new VDO confirmed clinically, a diagnostic wax-up of the proposed porcelain laminate veneers was prepared (Figure 8). Teeth Nos. 22 through 27 were conservatively prepared for porcelain laminate veneers using an incisal overlap design.15 Because these are all-ceramic restorations, the dentin shade and target enamel shades were communicated to the dental laboratory with clinical photographs of the shade tabs (Figure 9). The preparations were provisionalized with Venus® Diamond Flow (Heraeus Kulzer, www.heraeus-venus.com), a light-cured flowable composite, using the rapid esthetic provisional (RAP) technique, which has sometimes been referred to as the “shrink wrap” technique (Figure 10).16 The clasps of the temporary partial were adapted to the provisional restorations, so that the patient remained fully functional at the new VDO while the permanent restorations were fabricated (Figure 11). The porcelain veneers were fabricated with a lithium-disilicate pressable glass-ceramic, IPS e.max® Press (Ivoclar Vivadent, www.ivoclarvivadent.us/), and adhesively bonded to the preparations with a dual-cured resin composite veneer cement (Variolink® II, Ivoclar Vivadent), used without a catalyst in light- curing mode only.
The final porcelain veneers are shown in Figure 12. The case was now ready to move on to the clinical sequence in which a new mandibular RPD would be fabricated. The provisional partial was easily adapted to the newly seated veneers, and used for continuous posterior function while the definitive removable restoration was fabricated (Figure 13). The number and position of the patient’s remaining natural teeth presented a challenge in designing a partial with the necessary retention while maintaining reasonable esthetics. Because no special tooth or tissue preparation is required, a Valplast® partial denture (Valplast International Corporation, www.valplast.com) was prescribed to achieve better esthetics than the cast-chrome clasp design previously used.
While Valplast partials can be fabricated completely metal-free, a hybrid design with a cast-chrome major connector was used instead, with Valplast saddles and clasps (Figure 14). The cast major connector offers many advantages, including improved esthetics, better durability, and a thinner profile that should attract less plaque and have less impact on speech (Figure 15). The thermoplastic Valplast clasps can be fine-tuned using heat, and adjusted to maintain ideal comfort and retention at the delivery appointment or at any time in the future. Porcelain denture teeth (Trubyte vacuum-fired porcelain posteriors, DENTSPLY Trubyte, trubyte.dentsply.com) were prescribed, due to the history of wear on the patient’s acrylic denture teeth.17 The pretreatment and completed case comparison photographs are shown in Figure 16 and Figure 17.
The selected treatment option fulfilled the patient’s chief complaint with highly conservative porcelain-laminate restorations for her mandibular anterior teeth. Going forward, these should improve esthetics and function as well as limit additional breakdown and wear. The irregularities in the occlusal plane could not be completely addressed through this treatment option, but were definitely improved. Though not as ideal as a fixed posterior restoration, the new RPD should provide reasonable durability, esthetics, and function for many years. Ultimately, it is very important to customize the treatment for each case based on the patient’s chief complaint as well as the etiology of the present conditions.
Disclosure
The author has no conflict of interest or financial interest in any material mentioned in this article.
References
1. Brantley CF, Bader JD, Shugars DA, Nesbit SP. Does the cycle of restoration lead to larger restorations? J Am Dent Assoc. 1995;126(10):1407-1413.
2. Clelland NL, Agarwala V, Knobloch LA, Seghi RR. Relative wear of enamel opposing low-fusing dental porcelain. J Prosthodont. 2003;12(3):168-175.
3. Hudson JD, Goldstein GR, Georgescu M. Enamel wear caused by three different restorative materials. J Prosthet Dent. 1995;
74(6):647-654.
4. Oh WS, Delong R, Anusavice KJ. Factors affecting enamel and ceramic wear: a literature review. J Prosthet Dent. 2002;87(4):451-459.
5. Mizrahi B. Combining traditional and adhesive dentistry to reconstruct the excessively worn dentition. Eur J Esthet Dent. 2008;3(3):270-289.
6. Cutbirth Steven T. Increasing vertical dimension: considerations and steps in reconstruction of the severely worn dentition. Pract Proced Aesthet Dent. 2008;20(10):619-626.
7. Chacona RL. Enamel loss and occlusal vertical dimension. Causes and considerations for treatment. Dent Today. 2003;22(4):92-97.
8. Chu SJ, Karabin S, Mistry S. Short tooth syndrome: diagnosis, etiology, and treatment management. J Calif Dent Assoc. 2004;32(2):143-152.
9. Brose MO, Tanquist RA. The influence of anterior coupling on mandibular movement. J Prosthet Dent. 1987;57(3):345-353.
10. Reshad M, Jivraj S. The influence of posterior occlusion when restoring anterior teeth. J Calif Dent Assoc. 2008;36(8):567-574.
11. Mohindra NK, Bulman JS. The effect of increasing vertical dimension of occlusion on facial aesthetics. Br Dent J. 2002;192(3):164-168.
12. Bloom DR, Padayachy JN. Increasing occlusal vertical dimension—why, when and how. Br Dent J. 2006;200(5):251-256.
13. Rosenberg MM, Kay HP, Keogh BE, Holt RL. Periodontal and Prosthetic Management of Advanced Cases. Carol Stream, IL: Quintessence Publishing; 1988:82.
14. Grant BT, Amenedo C, Freeman K, Kraut RA. Outcomes of placing dental implants in patients taking oral bisphosphonates: a review of 115 cases. J Oral Maxillofac Surg. 2008;66(2):223-230.
15. Castelnuovo J, Tjan AH, Phillips K, et al. Fracture load and mode of failure of ceramic veneers with different preparations. J Prosthet Dent. 2000;83(2):171-180.
16. Pitel ML. A simple, rapid, high quality technique for aesthetic temporization of an Anterior Laminate Veneer or Crown. Dentistry Today. 1999;18(11).
17. Ghazal M, Yang B, Ludwig K, Kern M. Two-body wear of resin and ceramic denture teeth in comparison to human enamel. Dent Mater. 2008;24(4):502-507.
About the Author
Mark L. Pitel, DMD
Associate Clinical Professor and Director of Predoctoral and CDE Esthetics
Columbia University College of Dental Medicine
New York, New York
Private Practice
Poughkeepsie, New York