Bonding of Zirconia Veneers
Achieving maximum adhesion with high-strength laminates.
By Jack D. Griffin, Jr., DMD
The dental profession continues to advance in cosmetic restorations that are highly esthetic, strong, and conservative. Zirconia has proven to be an excellent choice in esthetic/restorative dentistry but its bond to tooth structure has been minimal. Bonding of zirconia is now dependable using a surface adhesive primer, which allows for the use of veneers lined with this material. In the case presented in this article, veneers and full-coverage crowns were done to make smile enhancements using a new zirconia primer.
There are many choices for conservative cosmetic restorations, with the ultimate goal being a marriage between esthetics and durability.1 The ultimate success of a cosmetic case and patient satisfaction is accomplished with the proper union of restorative materials, well-planned tooth preparation, dependable bonding, biologically acceptable soft-tissue treatment, and accurate communication between the patient, dentist, and laboratory.2,3
Porcelain veneers have been placed for more than 20 years, meeting the esthetic desires of most patients.4,5 Despite the overwhelming success practitioners have with porcelain veneers, the profession constantly strives to improve their strength, longevity, and esthetics as with all restorations. In the last few years, there have been significant advances with indirect esthetic materials melding higher levels of strength and esthetics than ever before.6 Some of the popular "newer" tooth-colored indirect restorative materials include:
- Zirconia—no layering porcelain
- Zirconia—layering with porcelain
- Lithium-disilicate ceramic
- Leucite-reinforced ceramic
Zirconia as a Restorative Material
Zirconia has been widely used recently because of its non-metallic color, versatility, and exceptional fracture resistance with flexural strengths of more than 1,000 MPa. It has proven to be reliable in a wide variety of clinical situations, such as monolithic restorations without overlying porcelain and with more esthetic cases when add-on porcelain has been layered onto or pressed to the zirconia substrate.7,8
Bonding zirconium-based restorations cannot be done with the same methods of traditional glass-porcelain.9,10 Zirconia (ZrO2) is a silica-free, acid-resistant, polycrystalline ceramic that does not contain amorphous silica (SiO2), making it ineffective to traditional glass-etching treatments such as hydrofluoric acid (HFl) followed by silane.11,12
Bond strengths using differing methods, including sand blasting with aluminum oxide, silane treatment, or other chemicals provided a weak bond at best that deteriorates significantly with time.13-16 When preparation designs are retentive, as in the case of many full crowns, bonding to the zirconia becomes less important and more traditional cementation with dual-cure resin cements such as BisCem® (BISCO, www.bisco.com), Maxcem (Kerr Corporation, www.kerrdental.com), and RelyX™ Unicem (3M ESPE, www.3mespe.com) can be successfully used.
Using Zirconia to Increase Bond Strengths
In the cases with less retentive preparations, including veneers, the stable long-term bond of the restoration to the tooth becomes much more important to long-term success. Primers that address the specific needs of non-silica oxides (zirconia, alumina, and metal) are highly beneficial and warranted when traditional retention/resistance form is lacking.17,18
There are several commercial ceramic primers on the market today for use with zirconia, such as AZ Primer (Shofu Dental Corporation, www.shofu.com), Clearfil™ Ceramic Primer (Kuraray, www.kuraraydental.com), Metal/Zirconia Primer (Ivoclar Vivadent, www.ivoclarvivadent.com), and Z-Prime Plus® (BISCO). Each of these materials varies in formulation, clinical technique, and performance.
In the following case, the veneers were made with zirconia and customized with an overlaid porcelain: there was no internal layer of porcelain to which to etch and bond. These veneers were placed on minimally prepared teeth and bonded using a primer, Z-Prime Plus, which uses MDP and carboxylic monomers formulated specifically for zirconia, alumina, and metal.
Studies have shown that these phosphate monomers are very effective in improving cohesive zirconia bonding to resin cements.19,20 The phosphate monomers form the basis for chemical bonds between the zirconia and the primer allowing for a cohesive bond to the resin cement. This reliable bond is critical especially in a minimally retentive case such as veneers.
Case Report
There are three legitimate questions regarding veneers with a zirconia substrate. First, with the wide spread long-term success of traditional porcelain veneers, is there a need for the zirconia substrate? Secondly, what is the durability of the layering porcelain to the zirconia? And lastly, what is the best method for bonding the zirconia to the tooth?
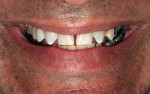
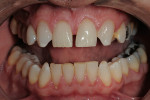
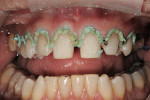
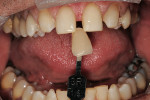
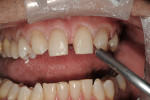
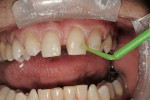
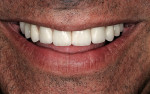
A gentleman who was born without maxillary lateral incisors wanted his spaces closed, whiter teeth, and a fuller, more pleasing smile (Figure 1). Most notable was a midline diastema, improperly positioned cuspids, and non-esthetic restorations (Figure 2). The upper molars and second bicuspids were lingually positioned and in cross bite and the gingival tissues were healthy with slight recession and no history of parafunctional habits. A treatment plan was made for veneers and full crowns from teeth Nos. 3 through 15.
Direct Mock-up and Tooth Preparation
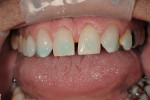
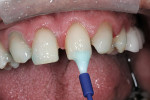
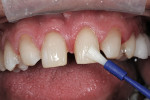
A direct composite mock-up was done before anesthesia and is important for guiding temporary fabrication, tooth preparation, esthetic and phonetic evaluation, and to be the first "preview" of desired treatment.21 The teeth were spot-etched and composite was added to check tooth proportions, phonetics, esthetics, and act as a color preview (Figure 3).22
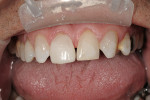
A single central incisor, tooth No. 8, was done first using a composite in a shade that the patient chose for his final restorations, and the midline position and cant were both checked (Figure 4). The remaining anterior teeth were then done and the phonetics were checked, the preliminary color was approved, and a signed record was made in the chart (Figure 5). A PVS impression of the mock-up was done for temporary fabrication.
Minimal tooth reduction was done with a medium-grit finishing diamond removing the mock-up material and staying in enamel wherever possible. All teeth were reduced in an "ideal" form in a 3-plane, rounded preparation beveled toward the facial to allow for incisal characterization by the laboratory and a definitive stop when seating.23 Teeth Nos. 13 through 15 were prepared for full-contour crowns.
A retraction paste (Expasyl®, Kerr Corporation) was then placed into the gingival sulcus for 5 minutes, rinsed off thoroughly, and the remaining residue was removed with alcohol on a microbrush (Figure 6). Two full-arch polyvinyl impressions were taken as well as a bite registration with horizontal and vertical alignment guides. A preparation shade was taken and photographed for the laboratory (Figure 7).
Transitional Restorations and IDS
Immediate dentinal sealing (IDS) is the definitive bonding and sealing of the tooth surfaces before temporaries are placed on the teeth. The best bond strengths to dentin are immediately after tooth preparation with a total-etch dentin bonding agent (DBA).24-26 This dentin bonding can diminish bacterial leakage leading to staining, sensitivity, and potential pulpal irritation during the temporization phase.27,28 IDS is often done before impressions are taken to decrease the chance of interference with final restoration seating which is particularly important for inlay/only type restorations where DBA could pool on internal line angles.29,30
The clinical advantages of IDS include:
- Highest bond strength to dentin is immediately after cutting
- Sealing dentinal tubules reduces sensitivity by sealing open tubules
- Sealing dentin reduces the chance of pulpal damage by bacterial habitation
- Reduces contamination of dentin by iron from microorganisms, blood, or chemicals
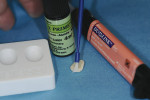
Etch, a dentin bonding agent, and a separating medium are all needed for IDS (Figure 8). In this case, immediately after tooth preparation, the entire prepared tooth surface was etched with 38% phosphoric acid, rinsed, and suction-dried (Figure 9). Several coats of DBA were placed (All-Bond 3®, BISCO) (Figure 10). Air was blown aggressively toward the gingiva to thin and remove the DBA solvent followed by light-curing (Figure 11).31
There is minimal chance of seating interference from the DBA because of the aggressive air thinning, the low film thickness of this DBA, and the lack of internal line angles such as seen with inlay/onlay type preparations. To further decrease the chance of temporary material adhering to the DBA, alcohol is used to remove the air-inhibited layer, rinsed, and repeated.32
A "hydrogel" separating medium, ProV Coat® (BISCO), was then painted on the teeth and temporaries were made with a dual-cure composite material (Luxatemp®, DMG America, www.dmg-america.com) inside the PVS matrix made from the mock-up (Figure 12).33 Trimming, polishing, and sealing were all done directly on the teeth. The "bleach shade" was what the patient desired and served as a second "preview." The patient was seen 5 days after preparation to have the temporaries adjusted and approved (Figure 13).
Placement of Zirconia Veneers
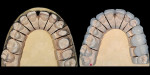
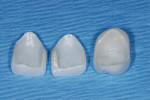
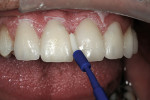
Preparation for zirconia veneers is consistent with preparations for traditional porcelain with 3-plane reduction with no sharp internal corners, slice preparations for diastema closures, and flattened incisal edges (Figure 14). The veneers were designed, milled, cut back, and layering porcelain was applied (Figure 15). This non-glass cannot be etched and bonded in a traditional manner (Figure 16). After try-in and cleaning with alcohol, the zirconia primer was placed into the restorations and then dried (Figure 17).
The teeth were pumiced and etched with phosphoric acid. DBA was then applied (All-Bond 3), air-thinned, and dual-cure composite luting material was applied onto the teeth and the veneers were seated. Clean up was done with brushes, a 204s scaler, gauze, and a composite knife after tack-curing (Figure 18). All restorations were then cured for 40 seconds from both the lingual and facial and the clean-up was finished (Figure 19).
Evaluation and Critique
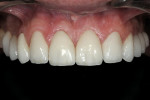
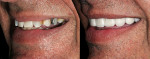
Zirconia substrate provides a very strong substructure for the overlying porcelain and the consistency of the materials for both anterior and posterior provide continuity in appearance (Figure 20). Conversions of the cuspids to the laterals, closing the space, and brightening the smile are all readily noticeable. Long-term questions with zirconia are its bond to the tooth and the adherence of the layering porcelain. After 2 years, the results are excellent in this case and bonding has been successful (Figure 21).
Acknowledgment
The author would like to thank Mr. Adrium Jurim at Jurim Dental Studio for his cosmetic work and understanding the principles of proper tooth anatomy and characterization.
Disclosure
Jack D. Griffin, Jr., DMD, has no financial interest in any way with the products, materials, or suppliers used in this article.
References
1. Rossmann JA, Cobb CM. Lasers in periodontal therapy. Periodontol 2000. 1995;150-164.
2. Tipton PA. Aesthetic tooth alignment using etched porcelain restorations. Pract Proced Aesthet Dent. 2001;13(7):551-555.
3. Dumfahrt H. Porcelain laminate veneers. A retrospective evaluation after 1 to 10 years of service : Part 1 – Clinical procedure. Int J Prosthodont. 1999;12(6):505-513.
4. Swift EJ Jr, Friedman MJ. Critical appraisal: porcelain veneer outcomes, part II. J Esthet Restor Dent. 2006;18(2):110-113.
5. Lee EA. Laser-assisted gingival tissue procedures in esthetic dentistry. Pract Proced Aesthet Dent. 2006;18(suppl 9):2-6.
6. Christensen GJ. The ceramic crown dilemma. J Am Dent Assoc. 2010;141(8):1019-1022.
7. Beuer F, Stimmelmayr M, Bernet W, et al. Prospective study of zirconia-based restorations: 3-year clinical results. Quintessence Int. 2010;41(8):631-637.
8. Guess PC, Zavanelli RA, Silva NR, et al. Monolithic CAD/CAM lithium disilicate versus veneered Y-TZP crowns: comparison of failure modes and reliability after fatigue. Int J Prosthodont. 2010;23(5):434-442.
9. Denry I, Kelly JR. State of the art of zirconia for dental applications. Dent Mater. 2008;24(3):299-307.
10. Conrad HJ, Seong WF, Pesun IJ. Current ceramic material and systems with clinical recommendations: a systematic review. J Prosthet Dent. 2007;98(5):389-404.
11. Blatz MB, Sadan A, Kern M. Resin-ceramic bonding: a review of the literature. J Prosthet Dent. 2003;89(3):268-274.
12. Dérand P, Dérand T. Bond strength of luting cements to zirconium oxide ceramics. Int J Prosthodont. 2000;13(2):131-135.
13. Ozcan M, Nijhuis H, Valandro LF. Effect of various surface conditioning methods of the adhesion of dual-cure resin cement with MDP functional monomer to zirconia after thermal aging. Dent Mater J. 2008;27(1):99-104.
14. Wegner SM, Kern. Long-term resin bond strength to zirconia ceramic. J Adhes Dent. 2000;2(2):139-147.
15. Kern M, Baroli A, Yang B. Surface conditioning influences zirconia ceramic bonding. J Dent Res. 2009;88(9):817-822.
16. Ernst CP, Cohnen U, Stender E, Willershausen B. In vitro retentive strength of zirconium oxide ceramic crowns using different luting agents. J Prosth Dent. 2005;93(6):551-558.
17. Griffin J, Suh B, Liang C, Brown D. Surface treatments for zirconia bonding: A clinical perspective. Canadian Journal of Restorative Dentistry and Prosthodontics. 2010;3(1):23-29.
18. Tanaka R, Fujishima A, Shibata Y, et al. Cooperation of phosphate monomer and silica modification on zirconia. J Dent Res. 2008;87(7):666-670.
19. Yoshida K, Tsuo Y, Atsuta M. Bonding of dual-cured resin cement to zirconia ceramic using phosphate aced ester monomer and zirconate coupler. J Biomed Mater Res B Appl Biomater. 2006;77(1):28-33.
20. Kern M, Barloi A, Yang B. Surface conditioning influences zirconia ceramic bonding. J Dent Res. 2009;88(9):817-822.
21. Mizrahi B. Visualization before finalization: a predictable procedure for porcelain laminate veneers. Prac Proced Aesthet Dent. 2005;17(8):513-518.
22. Mizrahi B. Visualization before finalization: a predictable procedure for porcelain laminate veneers. Prac Proced Aesthet Dent. 2005;17(8):513-518.
23. Gürel G. Predictable, precise, and repeatable tooth preparation for porcelain laminate veneers. Prac Proced Aesthet Dent. 2003;15(1):17-24.
24. Lee JI, Park SH. The effect of three variables on shear bond strength when luting a resin inlay to dentin. Oper Dent. 2009;34(3):288-292.
25. Mange P, Kim TH, Cascione D, Donovan TE. Immediate dentin sealing improves bond strength of indirect restorations. J Prosthet Dent. 2005;94(6):511-519.
26. Duarte S, de Freitas CR, Saad JR, Sadan A. The effect of immediate dentin sealing on the marginal adaptation and bond strengths of total-etch and self-etch adhesives. J Prosthet Dent. 2009;102(1):1-9.
27. Magne P. Immediate dentin sealing: a fundamental procedure for indirect bonded restorations. J Esthet Restor Dent. 2005;17(3):144-154.
28. Pashley EL, Comer RW, Simpson MD, et al. Dentin permeability: sealing the dentin in crown preparations. Oper Dent. 1992;17(1):13-20.
29. Magne P, So WS, Cascione D. Immediate dentin sealing supports delayed restoration placement. J Prosthet Dent. 2007;98(3):166-174.
30. Dillenburg AL, Soares CG, Paranhos MP, et al. Microtensile bond strength of prehybridized dentin: storage time and surface treatment effects. J Adhes Dent. 2009;11(3):231-237.
31. Stavridakis MM, Krejci I, Magne P. Immediate dentin sealing of onlay preparations: thickness of pre-cured dentin bonding agent and effect of surface cleaning. Oper Dent. 2005;30(6):747-757.
32. Papacchini F, Dall'Oca S, Chieffi N, et al. Composite-to-composite microtensile bond strength in the repair of a microfilled hybrid resin: effect of surface treatment and oxygen inhibition. J Adhes Dent. 2007;9(1):25-31.
33. PRO-V®. Provisional Restorative System. [Brochure]. Available at: www.bisco.com/Catalog/prov.pdf
About the Author
Jack D. Griffin, Jr., DMD
Private Practice
Eureka, Missouri