G-aenial Universal Flo
Using a revolutionary, high-strength flowable composite for restoring small-to-moderate posterior Class II cavities.
The foundation of modern dentistry rests on early detection and minimal intervention. Digital radiography and caries detection devices available to clinicians allow the bacterial process of decay to be diagnosed much sooner than ever before. Insipient caries that has not yet breached the dentin–enamel junction can be detected and even reversed with remineralization pastes such as MI Paste™ (GC America, www.gcamerica.com). Early carious lesions that required surgical intervention can be prepared with minimally invasive preparations that merely remove the decay without regard to traditional mortise forms, mechanical retentive grooves, or undercuts or dovetails. Carious lesions should be conservatively dissected away from healthy tooth structure, and the resulting preparations are often highly irregular outline forms of varying depths and widths.
In the past, the selected direct restorative material dictated the preparation. The reverse is true with the concept of minimal intervention dentistry. Conscientious clinicians have long faced the conundrum of needing a strong, durable composite material, while desiring the handling properties of a flowable resin to adapt to these irregular preparations. Historically, flowable composite resins have merely been “watered-down” versions of their more durable restorative counterparts. The reduction of filler loading and increase in monomer content seen in many flowable composites permit these materials to flow, but often at the expense of reduced physical properties, color saturation, and polishability. These limitations have historically limited the use of traditional flowable resins, but advances in filler technology and handling have opened the door to expanded clinical indications.
Advantages of Flowable Composite Resins
The use of flowable composite resins as both a liner under conventional composite restorations and as the definitive final restoration in small Class I cavity forms has been well documented.1-4 Other common uses of flowable composites include pit-and-fissure sealants, bonding orthodontic brackets, intra- and extra-coronal splinting, and provisional restoration repair. Due to the diversified use of these materials, two classes of flowable composites have emerged. Brands that are designed for use primarily as a definitive restorative material are typically more viscous with less flow when compared to more fluid, less viscous brands designed primarily for use as liners, sealants, bracket cementation, and provisional repair.5
In general, flowable composites offer the primary advantage of superior adaptation to irregular cavity forms often found in small proximal boxes, narrow isthmuses, tunnel preparations, and undermined cavosurface margins when compared to traditional microhybrid and nano-composite materials.6 Additionally, flowable composites are typically more elastic formulations (low elastic modulus) and, therefore, produce less stress on the bond interface during polymerization.7,8 This makes this material ideal for use as liners, definitive restorative materials in high C-factor preparations, and for use in repairing Class V abfraction.9 Flowable resins are typically dispensed through a 19- or 20-gauge cannula via either a syringe or compule. This mode of delivery proves advantageous in that there is no need for condensing or adapting to lateral walls with a separate instrument.
G-aenial Universal Flo
Recently, GC America released a unique, highly filled flowable composite resin specifically designed to meet the demands of not only minimal intervention dentistry, but a broad range of clinical applications where high-strength flowable resins are the ideal restorative choice. G-aenial is unique in that, for the first time, strontium glass fillers with the smallest particle size seen in current flowables and composites (200 nm) are homogeneously dispersed in an amorphous complex. The use of spherical nano-fillers and nano-aggregates in composite resins are firmly established in composite technology.10 However, the use of nano-sized strontium glass fillers treated with a proprietary surface treatment offers the advantages of increased particle adhesion to the resin matrix (wear), increased flexural strength, deeper color saturation, and excellent polish and polish retention.11,12 The amorphous nano-particle formulation significantly enhances the physical properties of G-aenial. Several clinical studies conducted by GC America conclude that the wear resistance and flexural strength of this material exceeds not only most of the competitive brands of currently available flowables, but many nano- and microhybrid traditional restorative composites as well. Internal studies within GC America also indicate that volumetric shrinkage, polymerization shrinkage stress, fracture toughness, and elastic modulus are either comparable or superior to several major traditional posterior restorative materials, expanding the clinical indications of G-aenial to use in small to moderate Class I, Class II, Class III, Class IV, and Class V restorations.
Particularly noteworthy are G-aenial's handling characteristics. It is a highly thixotropic material that flows evenly and smoothly, yet stays in place at the point of application, even on vertical slopes. Whereas more fluid flowable materials tend to drip or run when placed in cavity preparations oriented against gravity, G-aenial remains adapted and stacks upon itself during application. This is particularly advantageous in Class III and Class V restorations where excess flow can lead to the material drifting out of the preparation, into interproximal spaces, and onto adjacent teeth. G-aenial Universal Flo is dispensed through a unique syringe that features a large arched-shaped ergonomic plunger that fits nicely in the palm of the hand. Rather than using a typical metal cannula, this material is dispensed through a long plastic nozzle with a fine tip so that access to tight, difficult spaces is enhanced. With superior physical properties, ideal flow and adaptation ad ease of dispensing, G-aenial is truly a universal flowable material.
Clinical Example
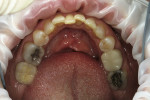
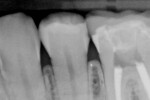
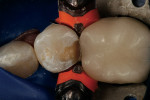
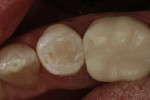
A female patient presented with a Class II distal carious lesion with distal–occlusal pit involvement on tooth No. 20 (Figure 1 and Figure 2). A simple box preparation was cut to access interproximal decay with a shallow extension onto the occlusal surface to remove the distal pit decay. A sectional matrix along with a Composi-Tight® Ring (Garrison Dental Solutions, www.garrisondental.com) was placed and a wedge was inserted into the V-shaped slot to seal the gingival margin (Figure 3).
G-aenial Universal Flo material was selected for the restorative material for this case primarily for its ease of use and impressive mechanical properties. The small cavity form fit the clinical indications for G-aenial, and because a strong contact was ensured by the use of the Composi-Tight system, there was no concern for creating a tight interproximal contact. The unique, extended tip ideally fits in small interproximal boxes and the favorable thixotropic properties of G-aenial Universal Flo permits intimate adaptation to an irregular, undulating cavity form such as this one. The volumetric shrinkage and shrinkage stress upon polymerization permit “bulk-filling” of small cavity forms, so restorations like the one presented here can be completed in seconds without the need for tedious incremental layering. G-aenial comes in 15 shades, including special cervical and bleach shades, and due to its high filler loading and the optical properties of strontium glass nano-particles, blends in nicely with the cavosurface margins and polishes to a high shine.
The bonding agent selected for this restoration was G-aenial Bond (GC America). A seventh-generation, single-bottle self-etching primer/adhesive. G-aenial Bond contains both a phosphoric ester monomer and 4-Met, similar to GC America's G-Bond, but is slightly more acidic (pH 1.5) and is also HEMA-free, which leads to greater enamel bond strengths.12 With shear bond strengths greater than 27 MPa on uncut enamel, it rivals several etch and rinse (total-etch) systems.12,13 For those who use a selective etching technique (etching enamel only) with self-etching adhesives, internal data demonstrates that the bond to dentin is not compromised if the phosphoric acid accidentally comes in contact with the dentin surface. The material is applied in a single coat, allowed to dwell for 10 seconds and the solvents are thinned and light-cured for 10 seconds. Total placement time is approximately 30 seconds. Once cured, G-aenial Bond is compatible with both light- and dual-cured composite systems.
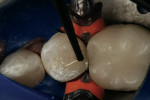
For this case, G-aenial shade A-1 was selected (Figure 4). G-aenial Bond was dispensed, applied in a single coat, allowed to dwell for 10 seconds, air-thinned and light-cured for 10 seconds (Figure 5). The plastic dispensing tip was attached to the G-aenial Universal Flow syringe and inserted into the cavity form. The thixotropic nature of the material permits an even amount of material to be dispensed into the cavity form with untoward continued flow after pressure has been released from the plunger. Beginning at the base of the proximal box, the preparation was backfilled (Figure 6), using the end of the tip to spread G-aenial Universal Flow across the floor and onto the walls of the preparation until the entire preparation was completely filled (Figure 7).
In the event of overfilling, it may be useful to use a small, clean microbrush to simply wipe away any excess material. G-aenial Universal Flo is then light-cured for 10 seconds (Figure 8).
Finishing and Polishing
The unique amorphous nano-filler and resin chemistry of G-aenial Universal Flo not only gives this material extraordinary physical properties, but excellent shade match and high polishability. The polishing technique for this material is similar to any traditional nano-hybrid restorative material. In this case, the anatomy was defined with a fine diamond bur, and a combination of an Enhance™ point (DENTSPLY Caulk, www.caulk.com) and a silicone-impregnated bristle brush were used (Figure 9 and Figure 10).
Conclusion
The final result is shown in (Figure 11). Note the seamless nature of the restoration without voids or white lines and the life-like luster. This particular restoration was completed in less than 10 minutes, primarily due to the speed and ease of dispensing G-aenial Universal Flow, its thixotropic flow and adaptation, and simplified polishing.
Until now, flowable composites lacked the handling and physical properties necessary for small to moderate posterior restorations like the one shown here. However, with unique filler and resin chemistry of G-aenial, clinicians may now expand the indications of this flowable material and expedite this common procedure for greater success and profitability.
References
1. Simonsen RJ. Preventive resin restorations (I). Quintessence Int. 1978;9(1):69-76.
2. Ibsen RI. Non-operative treatment for gingival erosion. Dent Surv. 1972;48(3):22-24.
3. Simonsen RJ, Landy NA. Preventive resin restorations: Fracture resistance and 7-year clinical results. J Dent Res. 1984;163-175.
4. Strassler HE. The new posterior composite resins. MSDA J. 1998;41(2):97-98.
5. Attar N, Tam LE, McComb D. Flow, strength, stiffness and radiopacity of flowable resin composites. J Can Dent Assoc. 2003;69(8):516-521.
6. Haak R, Wicht M, Noack M. Marginal and internal adaptation of extended class I restorations lined with flowable composites. J Dent. 2003; 31(4):231-239.
7. Unterbrink GL, Liebenberg WH. Flowable resin composites as “filled adhesives”: Literature review and clinical recommendations. Quintessence Int. 1999;30(4):249-257.
8. Labella R, Lambrechts P, Van Meerbeek B, Vanherle G. Polymerization shrinkage and elasticity of flowable composites and filled adhesives. Dent Mater. 1999;15(2):128-137.
9. Braga R, Hilton TJ, Ferracane JL. Contraction stress of flowable composite materials and their efficacy as stress-relieving layers. J Am Dent Assoc. 2003;134(6):721-728.
10. Garcia A, Lozano M, et al. Composite resins: a review of the materials and clinical indicatinos. Med Oral Patol Oral Cir Bucal. 2006; 11(E):215-220.
11. Hosoya Y, Shiraishi T, et al. Color characteristics of resin composites in different color modes and geometries. J Oral Sci. 2009; 51(1):123-130.
12. Suzuki T, Kyoizumi H, et al. Resistance of nanofill and nanohybrid resin composite to toothbrush abrasion with calcium carbonate slurry. Dent Mat J. 2009;28(6):706-716.
13. Hirano K, Yapp R, Power J, et al. Bond strengths to ground and un-ground enamel of G-aenial Bond. J Dent Res. 2011;90(Spec Iss A):3167.
About the Author
Jeff T. Blank, DMD
Private Practice
Fort Mill, South Carolina