Alternative Implant Treatment
Mini dental implants can be used for denture stabilization in medically compromised patients.
Despite ongoing improvements in oral health, statistics show that edentulism will be a significant issue for patients and dental practices for decades to come. Within the next 50 years, the over-65 population is expected to grow to represent more than one-fifth of the total US population.1 Twenty-five percent of people 65 to 74 are edentulous in both arches.2 As the size of the senior population continues to swell, effective treatments for edentulism will likely be in high demand.
Only a few years ago, the options available to help edentulous patients attain denture stability and functionality were limited. Denture relines can provide limited help; however, they cannot prevent ridge resorption and are, thus, often a short-term solution. Stabilizing dentures with conventional implants offers a much higher level of retention, so much so that McGill University issued a consensus statement that “a 2-implant overdenture should become the first choice of treatment for the edentulous mandible.”3 However, conventional implant treatment requires a level of bone width and overall patient health that disqualifies many candidates for the procedure, particularly those who have been edentulous for many years. It is also a costly option, making it particularly difficult for patients living on fixed incomes to afford.
Originally accepted by the FDA in 1997,4 3M ESPE MDI mini dental implants (3M ESPE, www.3mespe.com; formerly the IMTEC Sendax MDI System), offer a solution that addresses many of the drawbacks of conventional implants while providing effective stabilization.5,6 Ranging in size from 1.8 mm to 2.9 mm, these implants can be placed in one 90-minute appointment and immediately loaded.7 Additionally, because of their smaller size, mini implants are suitable for many patients who do not qualify for conventional implants.8 The minimally invasive procedure presents a lower risk for medically compromised patients, and the small diameter makes the implants an acceptable treatment for patients who lack adequate bone width for traditional implants. Moreover, mini implants offer patients a more economical treatment for denture stabilization than standard diameter implants.9 General dentists can become certified to perform 3M ESPE MDI mini dental implant placement for denture stabilization in just a 1- or 2-day seminar.
While mini implants do not yet have the lengthy clinical record of conventional implants, the available research has been promising. One histological review of the implants at both 4 and 5 months post-insertion found that the bone was integrated to the implant at the light microscope level, and that it was “mature and healthy… more than one would expect in this amount of time from insertion of mini-dental implants with immediate loading.”10 Studies have found survival rates ranging from 91.2% to 96.3%,7,11,12 with one of the most recent studies, which followed more than 2500 implants, finding a 5-year survival rate of 94.2%.13 This record will likely only improve with time as more clinicians begin offering the treatment. The following case demonstrates the successful use of 3M ESPE MDI mini dental implants in a medically compromised patient.
Case Report
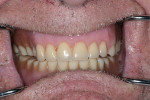
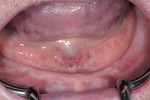
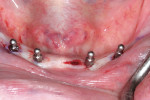
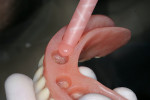
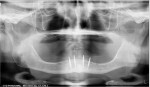
The 85-year-old male patient visited the practice with a loose set of dentures. The denture teeth were in poor condition, and the patient said that the lower denture was so loose he had difficulty eating (Figure 1). A complete oral examination was performed, including oral cancer screening. The patient, who had worn dentures since 1967, presented with a severely atrophic mandibular ridge with very little keratinized attached tissue. The ridge was so resorbed that the mental foramen was now on top of the ridge (Figure 2). A series of previous relines had been ineffective. The patient also had other health conditions, including heart disease, which had led to a porcine valve replacement and a pacemaker implantation. At the time of his initial visit, the patient was taking 8 daily medications, including Coumadin.
The patient wanted to quickly restore his chewing function and address the instability of his lower denture, and the risks and benefits of the options available were discussed. While regular-diameter implants would have addressed his stability problem, the treatment duration and cost was unappealing to the patient. Additionally, the invasiveness of the procedure would have been risky considering his medical condition. The possibility of relining his denture or creating a new set was also discussed; however, this would have provided only a short-term solution and his bone loss would have continued.
The benefits of mini dental implants were then discussed, including their ability to be quickly placed and immediately loaded, as well as the lower cost compared to conventional implants. Their lower level of invasiveness was also advantageous, especially given the patient's medical condition and use of blood thinners. The risks involved with the mini-implant procedure were discussed, which are similar to those for any surgical procedure, including the possibility of swelling, pain, and infection. Additionally, the author informed the patient of the lack of long-term data available on the outcomes compared to conventional implants, due to it being a relatively new procedure.
The patient decided to pursue mini implant treatment and, because his original denture was in such poor condition, he also agreed to the fabrication of a new denture for use with the MDI implants and attachments. The author obtained the patient's full medical history from his physician, as well as medical clearance for performing mini-implant surgery. The physician, who was unfamiliar with mini implants, was initially hesitant to authorize the procedure and strongly cautioned against the use of epinephrine, as it would increase the patient's heart rate. However, after the author explained the minimally invasive nature of the surgery and the extremely small amount of anesthetic required, the physician consented to the surgery.
A new set of dentures was created to properly restore the patient's vertical dimensions as well as esthetics. The patient was then instructed to wear the dentures for 2 weeks prior to the implant placement appointment and to stop taking Coumadin 5 days in advance of the procedure, as per his physician's direction. The patient was also given prescriptions for antibiotics and analgesics.
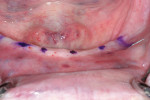
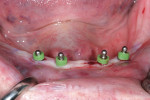
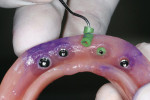
At the placement appointment, local anesthesia was delivered and the locations for each of the four implants were marked on the patient's tissue (Figure 3). Avoiding mandibular nerve injury is paramount in performing the mini-implant procedure in the anterior mandible. Although CT software technology is available that facilitates accurate implant placement, effective intraoral protocol can be used to achieve safe implant placement and avoid mandibular nerve injury. According to Greenstein and Tarnow, 60% of mandibles have an anterior loop extending 1 mm to 5 mm mesially from the mental foramen.14 To determine the locations of the neurovascular bundle and the mental foramina, the clinician can manually palpate and then mark their locations on the ridge with an indelible marker. From this marked location, the clinician is advised to move 8 mm mesially to establish the most distal mini-implant location. This amount of space from the mental foramen allows adequate room for the anterior loop, the radius of the mini implant, and space between the anterior portion of the anterior loop and the distal side of the mini implant in order to avoid injuring mandibular nerve.
Manual intraoral protocol in safely avoiding mandibular nerve damage can reduce the cost incurred by patients when compared to using a CT scan and a surgical stent created from the scanning process. In a university-based study consisting of 626 narrow-diameter implants placed by senior dental students under faculty supervision, no surgical stents were used.9 This study supports the fact that mini implants can be placed safely and successfully without surgical stents. However, the clinician can certainly incorporate CT and surgical stent technology into the treatment protocol if deemed clinically necessary.
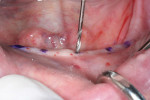
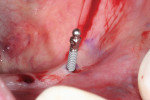
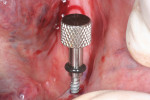
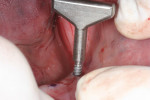
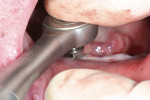
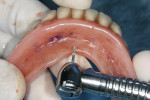
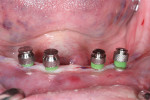
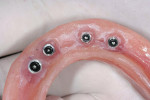
Following the 3M ESPE MDI surgical protocol, a pilot drill was used to lightly drill the entry points, penetrating the cortical plate (Figure 4). Pilot holes were drilled to a depth of one-third to one-half of the threaded length of the 2.4 mm by 13 mm MDI implants. The implants were inserted one by one into the pilot openings, followed by a clockwise rotation with a titanium finger driver (Figure 5 and Figure 6). Downward pressure was applied during the rotation to initiate the implants' self-tapping process. The finger driver was used until noticeable bony resistance was felt. At this point, the finger driver was replaced with a winged thumb wrench to create a greater amount of torque (Figure 7) and to thread the implant until it became difficult to turn. Finally, a ratchet wrench was used to make small incremental turns to finalize the insertion (Figure 8). The implants were inserted until the full length of the abutment head was visible above the gingival soft tissue, but no neck or thread portions of the implant were protruding (Figure 9). To enable immediate loading, the implants were ratcheted until they reached a resistance torque of at least 35 Ncm.
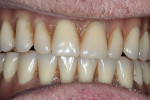
Placement of the four implants took approximately 30 minutes, during which time the patient remained comfortable and was even joking in the operatory. After the implant placement, the patient's denture was retrofitted to accommodate the implants. Four 5-mm openings were drilled into the lower denture in alignment with the position of the implants (Figure 10). Blockout shims were then trimmed to size and placed on each implant, in order to prevent denture pickup material from curing to the implant (Figure 11). Properly sized metal housings were placed on the implants and a passive fit was confirmed over the blockout shims (Figure 12). The denture was then tried in the mouth to confirm a passive fit over the implants and housings. The denture was removed, and a thin layer of adhesive was applied to the tissue-born side. SECURE Hard Pick-Up material (3M ESPE) was applied onto the metal housings and into the openings in the denture, and the upper and lower dentures were then seated in the patient's mouth (Figure 13). The patient was instructed to bite down with normal pressure, and the material was allowed to set for 7 minutes. The denture was then removed, and after it was confirmed that no voids were present, the blockout shims were removed from the implants (Figure 14). To complete the process, the denture was polished and seated, and the patient, who expressed satisfaction with the stability of his denture, was instructed not to remove it for 48 hours to prevent overgrowth of the tissue (Figure 15, Figure 16 and Figure 17).
The patient was instructed to resume taking his blood thinners 24 hours later. In a postoperative visit the following week he presented with no denture sore spots under the lower denture. He reported having minor soreness in the mandible for about a day after the implant placement, without any further discomfort. He also stated that he could now bite into regular hard food because his lower denture was stable and expressed high satisfaction with the entire procedure.
Patients who receive mini-implant treatments are automatically placed on a 6-month maintenance schedule, similar to dentate patients. During these appointments, several clinical parameters are evaluated, including effectiveness of home care, health of peri-implant tissues, stability of implants, fit of the denture over implants and the ridges, adequate retentiveness of the denture, integrity of o-rings, and patient comfort and satisfaction. Implants are carefully scaled with appropriate instruments and any necessary instructions are given to the patients. Patients treated in LeBarre's study reported very high postoperative satisfaction with the procedure.9
Discussion
This case shows a typical application for MDI implants and demonstrates their suitability for medically compromised patients for whom conventional implants present a more serious risk. The patient's physician, who originally believed his patient was seeking a conventional implant treatment with its invasive steps and long healing time, was initially reluctant to the patient receiving the treatment. Had there been no alternative implant therapy, this patient would have been left with a lower ridge that would continue to resorb, and even less ability to chew.
Many physicians seem unaware of what mini-implant treatment entails and often assume the procedure is similar to that for conventional implants. This frequently leads to hesitation on a physician's part to approve the treatment for elderly or medically compromised patients. However, in the author's experience, after personally speaking with physicians and clearly explaining the procedure to them, many are willing to give their consent. In this case, the physician's concern that epinephrine would be used to anesthetize the patient was allayed once he understood the small amount that would be needed. Additionally, the fact that the procedure is flapless and results in only a small amount of bleeding often helps physicians understand the lower level of risk.
Because the procedure is so minimally invasive, it is suitable for a broad pool of patients. The oldest patient that the author has treated with MDI implants was 98, and he has treated an additional 10 patients over the age of 90. Effective and efficient, the procedure can be a valuable treatment for edentulous patients and can make a significant improvement in their quality of life.15
Acknowledgment
The photographs in this case originally appeared in the Winter 2011 issue of Inclusive, a publication of Glidewell Laboratories. The article was titled, “Mini Dental Implants for Every Dentist” by Dr. Choi.
Disclosure
Dr. Choi is a paid consultant for 3M ESPE.
References
1. US Bureau of the Census. US interim projections by age, sex, race and Hispanic origin: 2000-2050. https://www.census.gov/ipc/www/usinterimproj/. Internet release date- March 18, 2004.
2. National Institute of Dental and Craniofacial Research, Centers for Disease Control and Prevention. Dental, Oral, and Craniofacial Data Resource Center. Annual Report—Oral Health US, 2002. Section 4: Tooth Loss. Page 35. https://drc.hhs.gov/report.htm.
3. The McGill consensus statement on overdentures. Quintessence Int. 2003;34(1):78-79.
4. Christensen GJ. The increased use of small-diameter implants. J Am Dent Assoc. 2009;140(6):709-712.
5. Christensen GJ. The ‘mini'-implant has arrived. J Am Dent Assoc. 2006;137(3):387-390.
6. Christensen GJ. The advantages of minimally invasive dentistry. J Am Dent Assoc. 2005;136(11):1563-1565.
7. Ahn MR, An KM, Choi JH, Sohn DS. Immediate loading with mini dental implants in the fully edentulous mandible. Implant Dent. 2004;13(4):367-372.
8. De Souza MM, Ram SM, Bhanushali K. Management of atrophic mandibular ridges with mini-dental implant system - a case report. Journal of Indian Prosthodontic Society. 5( 3):158-160.
9. LaBarre EE, Ahlstrom RH, Noble WH. Narrow diameter implants for mandibular denture retention. J Calif Dent Assoc. 2008; 36(4):283-286.
10. Balkin BE, Steflik DE, Naval F. Mini-dental implant insertion with the auto-advance technique for ongoing applications. J Oral Implantol. 2001;27(1):32-37.
11. Mazor Z, Steigmann M, Leshem R, et al. Mini-implants to reconstruct missing teeth in severe ridge deficiency and small interdental space: a 5-year case series. Implant Dent. 2004;13(4):336-341.
12. Bulard RA, Vance JB. Multi-clinic evaluation using mini-dental implants for long-term denture stabilization: a preliminary biometric evaluation. Compend Contin Educ Dent. 2005;26(12):892-897.
13. Shatkin TE, Shatkin S, Oppenheimer BD, Oppenheimer AJ. Mini dental implants for long-term fixed and removable prosthetics: a retrospective analysis of 2514 implants placed over a five-year period. Compend Contin Educ Dent. 2007;28(2):92-99.
14. Greenstein G, Tarnow D. The mental foramen and nerve: clinical and anatomical factors related to dental implant placement: a literature review. J. Periodontol, 2006;77(12) 1933-1943.
15. Griffitts TM, Collins CP, Collins PC. Mini dental implants: an adjunct for retention, stability, and comfort for the edentulous patient. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2005;100(5):e81-84.
About the Author
Raymond Choi, DDS
Private Practice
Tustin, California