Methodical Tooth Preparation for Predictable Esthetic Excellence
Stylus™ ATC air-driven handpiece technology combines constant torque with high speed for quality restorations.
By Robert Ritter, DMD
With a variety of esthetic materials available for tooth restoration today, it is important that the clinician understand the tooth reduction requirements for each material option in order to maximize the esthetic value and functional strength of the completed restoration. When porcelain-fused- to-metal (PFM) was the only esthetic restorative alternative for crown-and-bridge dentistry, preparation require ments were fairly standardized. Most clinicians and laboratory technicians agreed that the optimal axial reduction for PFM crowns was 1.5 mm. This allowed 0.3 mm of space for a metal substructure, 0.2 mm for opaquing porcelain, and 1 mm for an optimal thickness of porcelain for strength and esthetics. On the occlusal surface, 1.5 mm to 2 mm of space was required to develop proper occlusion and morphology while having a minimum of 1 mm of porcelain on the functional surface for strength and longevity.1,2
Today, the goal of the restorative dentist should be to use a material that yields the functional and esthetic result desired while removing the least amount of tooth structure.3 This article describes step-by-step techniques for the methodical preparation of conservative all-porcelain crowns using the latest in air-driven handpiece technology, the DENTSPLY/Midwest® Stylus™ ATC (DENTSPLY Caulk, www.dentsply.com).
Two Handpieces in One
The introduction of the air-driven handpiece by Dr. John Borden and DENTSPLY in 1957 revolutionized the way dentistry is delivered to patients. Using an air-driven, “high-speed” handpiece to prepare teeth quickly with less trauma to the tooth and patient represented a significant advance from its belt-driven predecessors. Electric handpieces have also been available that give the clinician more constant torque when cutting through various types of tooth structure and dental materials. The new Stylus ATC air-driven handpiece combines these two benefits into one instrument. Two new technologies—Speed Sensing Intelligence (SSI) and Superior Turbine Suspension (STS)—allow this one instrument to deliver constant torque at high speeds when performing various dental procedures that require a handpiece, specifically cutting enamel and dentin, and removing or sectioning through different types of restorative materials, including metal and zirconium.
All-Ceramic Crown Preparation
Conservative preparation can be made for teeth to be restored with esthetic ceramic (traditional feldspathic or lithium disilicate) and maintain proper anatomic contour. The “lamination effect” in conjunction with today’s adhesive resins, resin cements, and stronger restorative materials have made this process very predictable. For a bonded all-ceramic porcelain or lithium-disilicate (e.max®, Ivoclar Vivodent, www.ivoclarvivadent.us) crown, a minimum of 1 mm of axial tooth reduction will be sufficient. Incisally (anterior teeth), 1 mm to 1.5 mm of clearance is recommended. In the posterior regions, particularly in functional areas, 1.5 mm to 2 mm of space is still recommended for occlusal clearance. In many cases, bonded stacked ceramic or lithium-disilicate restorations will yield a durable and beautifully esthetic result.4-8
The following is the sequence of steps to prepare an all-ceramic stacked crown preparation using the Stylus ATC and Lowe Crown and Bridge Set (Axis Dental, www.axisdental.com).
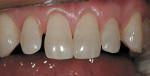
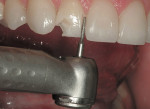
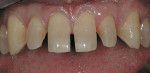
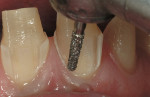
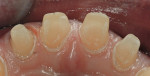
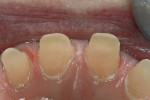
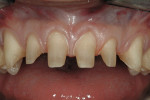
A thin, rounded cylinder diamond (SC856-014) is used to break proximal contacts. A thinner “needle” diamond (M849-009) can be used if the adjacent proximal surface is so close that contact cannot be broken without the diamond scoring the adjacent surface. It is important to break contact with the smallest diameter diamond possible to avoid over-preparation during the first pass of the instrument (Figure 1 through Figure 3; note that Figure 2 was taken from another case for example illustration purposes).
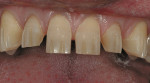
Using the same SC856-014 diamond as described in Step 1, vertical depth cuts are created in the middle and incisal one thirds of the tooth, following the angle of the facial plane in the incisal one third. The preparation should be multi-planar so that uniform reduction of the tooth is made and the resulting all-ceramic crown gives natural reflection as light passes through the facial surface. The diameter of the instrument at the tip is 1.2 mm; therefore this diamond should place a depth cut to approximately half its total diameter (about 0.6 mm) (Figure 4 ). The depth cuts are then “erased” by “painting” with the bur in a horizontal plane, reducing the tooth evenly on both sides of the depth cuts.
Depth cuts are then placed in the cervical plane with the SC856-014 to approximately half the depth (radius) of the end of the bur. The preparation finish line will be a rounded internal shoulder with a 90° cavosurface angle (butt-joint) (Figure 5). Depth grooves of 1 mm are placed on the incisal edge using the SC856-014 tapered cylinder diamond.
The incisal edge is then reduced with its edge forming an acute angle to the facial surface (incisal half) to allow for sufficient thickness of restorative material when the patient moves from a centric-relation occlusion position in protrusive and lateral excursions. A depth groove is then cut using the SC856-014 rounded cylinder diamond on the lingual surface following the natural contour of the tooth. Preparing an axial wall that is parallel or no greater than 6° will result in a preparation that will resist displacement of the crown during function. The cervical plane that is formed by preparation of the cingulum should diverge 10° to 15° from the cervical plane on the labial surface for reciprocal retention (Figure 6).
An elliptical-shaped diamond, C379-023, is then used to eliminate the depth groove in the lingual concavity only (middle and incisal one thirds of the lingual surface). The SC856-014 is used to reduce the cervical one third of the lingual surface and blend the finish line to both proximal aspects. The clinician should remember to keep the depth uniform in the axial direction.
The lingual reduction is verified by asking the patient to close in centric occlusion, then observing to check uniformity of lingual reduction as the patient moves forward in protrusive and lateral excursions with light incisal contact.
A 50-µm round, tapered, cylinder finishing diamond, F856-014, is used to refine and smooth the axial walls on all aspects of the preparation, followed by the incisal edge. Note that it is the same shape as the original super-coarse diamond used for gross reduction. A 50-µm elliptical-shaped finishing diamond, F379-023, is used to polish the lingual concavity of the preparation. The surfaces are shown after completion of the polishing step (Figure 7).
The final step in the polishing of the preparation is accomplished using an Enhance® composite polishing point (DENTSPLY Caulk). This step softens all the transitional angles of the preparation, eliminating potential stress concentrators in the ceramic crown.
Figure 8 shows a facial view of the completed all-ceramic crown preparations. This type of conservative reduction could also be used for a Captek™ (Precious Chemicals Co Inc, www.captek.com) PFM restoration due to the requirement for less reduction afforded by the thinness of the Captek coping and its gold color. Note the uniform thickness of the finish line circumferentially and overall smoothness of the transitional line angles. Bonded restorations do not depend on rough preparation surfaces to aid in cement retention of the restorations. The preparation should be as smooth as possible to increase accuracy of fit and ease of delivery.
Conclusion
Techniques have been described to successfully create conservative, predictable tooth preparations with most of today’s esthetic restorative materials and advanced rotary instrumentation. By following this methodical approach, taking a good final impression, and maintaining appropriate records, the clinician, with the help of the ceramic technician, is able to deliver consistent quality in esthetic dental restorations.
References
1. McLean JW. The Science And Art Of Dental Ceramics. Chicago, IL: Quintessence Publishing Co; 1980.
2. Chiche GJ, Pinault A. Metal ceramic crowns. In: Esthetics Of Anterior Fixed Prosthodontics. Chicago, IL: Quintessence Publishing Co; 1994:75-96.
3. Lowe RA. Preparation design: combining esthetics with function.Dental Products Report. 2002;36(1):64-65.
4. Chiche GJ, Pinault A. All ceramic crowns and foil crowns. In: Esthetics Of Anterior Fixed Prosthodontics. Chicago, IL: Quintessence Publishing Co: 1994:97-113.
5. Etman MK, Woolford MJ, Three-year clinical evaluation of ceramic crown systems: a preliminary study, J Prosthet Dent. 2010;103(2):80-90.
6. Guess PC, Strub JR, Steinhart N, et al. All-ceramic partial coverage restorations—midterm results of a 5-year prospective clinical splitmouth study. J Dent. 2009;37(8):627-637.
7. Wolfart S, Eschbach S, Scherrer S, Kern M, Clinical Outcome of three-unit lithium-disilicate glass-ceramic fixed dental prostheses: up to 8 years results. Dent Mater. 2009;25(9):e63-e71.
8. Lowe RA. Restoration of maxillary central incisors using OPC-3G. Contemporary Esthetics and Restorative Practice. 2001;5(12):46-53.
About the Author
Robert A. Lowe, DDS
Private Practice
Charlotte, North Carolina