Minimally Invasive Dentistry
Wynn H. Okuda, DMD
A natural evolution in cosmetic restorative dentistry.
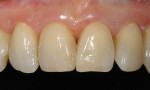
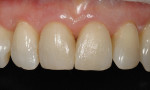
Over the last several years, the technological development of composite resins has made direct resin an even more viable long-term restorative material. Coupling this with the ability to eliminate the carious disease process is a good direction that may allow for a better approach to restorative care. In the evolution of cosmetic dentistry, it is important to explore progressive ideas so that clinicians can continue to preserve the dentition through minimally invasive care (Figure 1 and Figure 2).1 This concept of minimally invasive dentistry (MID) is also important as it relates to cosmetic dental treatment.
Minimally Invasive Dentistry in Cosmetic Restorative Treatment
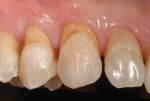
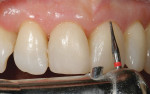
In correcting dental problems, one must understand the importance of approaching treatment in the right perspective. Understanding that caries is a bacterial disease process that must be first eliminated through methods of caries control is essential (Figure 3). With advances in material science, the ability to remineralize and heal demineralized tooth structure not only reduces future caries incidence, but it also allows for less tooth removal during the restorative phase.2,3
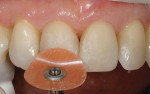
Adhesion dentistry allows for a modified cavity design to be used in comparison to the original G.V. Black classification. Modifications to existing cavity design should be based on preservation of natural dentition (Figure 4). Black's classification for cavity preparation was based, in part, on the need to create resistance form and retention form of the restorative material so that the restoration would not be dislodged. The requirements of Black's cavity design necessitated additional tooth removal for diverging internal axial walls and retentive grooves.2,4 However, with dental adhesives, additional tooth removal to create mechanical retention and resistance is no longer needed (Figure 5). With regard to restorative materials, its progress has also given dentists the opportunity to perform procedures with minimal invasion. With the newer composite resins now able to chameleon or blend to tooth structure more simply, predictable esthetic results can be attained (Figure 6, 7, 8).5 Finally, resin-modified glass ionomer (RMGI) can be used as a biomimetic substitute for dentin, therefore allowing the dentist to recreate dentition with less tooth removal.
Biomimicry in Dentistry
Historically, the lack of ideal esthetic dental materials did not readily allow for the use of a minimal-intervention model. Because materials of the past did not have as favorable physical properties (eg, optimal strength, etc) along with the esthetic qualities needed for long-term results, more aggressive treatment (such as indirect restorative procedures) had to be performed. However, with the recent progress of nano-technology in composite resins over the last several years, attaining biomimetic results with MID is now highly achievable.6
One of the challenges of biomimetic dentistry is to create predictable color harmony between the restorative material and natural tooth structure. In creating invisible restorations with composite resin, the clinician must understand color-hue, value, and chroma-and how it interrelates with the dentition.7-9 Translucency is also an important element that allows light to only diffusely pass through an object; therefore, creating depth of color.10
In natural dentition, different aspects of tooth structure will reflect, refract, and absorb wavelengths of light at different degrees (eg, enamel rods, dentinal tubules, dentino-enamel junction, etc). This is especially true for anterior teeth because light is readily abundant in comparison to its posterior counterparts.11
Therefore, for an esthetic material to mimic natural dentition, it must match the optical and physical properties of tooth structure. When the composite resin is able to match the optical properties of the surrounding tooth, a chameleon effect is achieved that renders the restoration "invisible." The new composite resins are showing great success because they visually reflect, refract, and absorb light in a similar manner to natural dentition. When esthetic materials (eg, composite resin, RMGIs, etc) are able to mimic the physical properties of the human dentition, biomimetic results can ultimately be attained.12,13
Recent Advances in Material Science
Recently, dental science has responded with new advancements in composite resin technology. The latest generation of nano-hybrid composite resins (eg, GC Kalore, GC America, https://www.gcamerica.com) is, in the author's opinion, a new plateau in cosmetic-restorative dentistry. With tremendous improvements on material chemistry, this new generation of composite resins includes a new and improved high-density radiopaque (HDR) prepolymerized filler and a proprietary interface between the resin matrix and the filler particles to make the material stronger and wear resistant.14 Furthermore, the reasoning behind this is to have better handling properties and amplified radiopacity.
For years, the advancements in composite resins have been in the area of filler particle technology. Much of the focus has been in changes to filler particle size, filler type, along with prepolymerized filler content and coating. In thinking outside the box, collaboration with DuPont Corporation yielded a new long-chain monomer in this nano-hybrid composite resin. The idea behind incorporating this new monomer was that it would help lower shrinkage stress, provide a harder restorative surface, and ensure better marginal integrity to reduce microleakage.15
Clinically, the author has observed that the surface does exhibit a harder, ceramic-like feel in comparison to composite resins of the past. In addition, this clinician has experienced that this nano-hybrid is easy to work with, polishes to a nice luster, and achieves highly esthetic results.
Use of Glass Ionomer in MID
The use of glass ionomers in MID is well-documented. Glass ionomer is a material that releases fluoride ions and demonstrates this anticaries property very effectively. When tooth surfaces are exposed to low pH on a long-term basis, demineralization occurs (Figure 9). The reduction of tooth surface integrity leads to enamel degradation and surface cavitation. Fluoride plays an important role in the strengthening process of tooth structure. In the presence of free fluoride ions, remineralization occurs with the formation of fluoroapatite, rendering the surface resistant to demineralization. Moreover, fluoride has further benefits as a mild bacteriostatic factor. A restorative material that releases fluoride ions can assist in protecting the tooth structure from demineralization.2,3,16
After removal of the bacteria-infected dentin, the use of RMGI (eg, GC Fuji II LC, GC America, Vitrebond™, 3M ESPE, https://www.3mespe.com) as a cavity liner provides a chemical- and light-cured bond to dentin as well as fluoride release (Figure 10).17,18 Adhesion of glass ionomer to normal dentin occurs through an ion-exchange mechanism as well as a hydrogen bonding or metallic-ion bridging to demineralized dentin. This provides a microleakage-free zone.4,19,20 With regard to the RMGI, an amorphous interfacial zone called the absorption layer is formed between the dentin and the RMGI.21 In proximity to affected dentin, glass ionomer creates a caries-resistant environment, remineralization of tooth structure, and good pulpal response.
As a biomimetic dentin substitute, RMGI can be used as a cavity liner or base before placement of composite resin. This direct technique with composite resin and RMGI is called the sandwich technique. This combination helps to reduce the amount of shrinkage stress between the direct resin restoration and the cavity preparation walls by approximately 20% to 50%.22 By using an incremental build-up technique with composite resin over the RMGI, a tremendous reduction in polymerization contraction stress can be attained (Figure 11).4,23
Clinical Applications
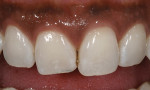
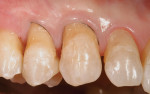
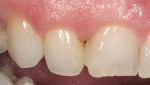
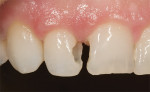
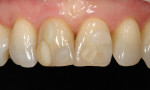
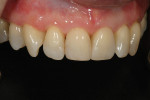
The patient in this case was a 46-year-old woman who presented with a failing composite resin along the right upper central incisor (No. 8) and a lingual angled left central incisor (No. 9) (Figure 12). Before treating the problem, it was important to first assess the reason for failure of the existing restoration. Whether the reason for failure is incorrect material selection, adhesive failure, cohesive failure, or a preparation design failure, it is important to understand the cause in order to prevent the problem from reoccurring. A restorative solution was recommended to the patient with long-term success in mind.
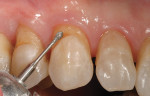
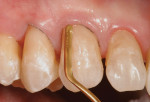
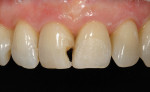
For MID, it was proposed to have an invisible Class IV restoration placed to immediately correct No. 8 and a composite veneer on No. 9 for proper facial inclination. Before tooth preparation, a comprehensive shade discovery was done to select the proper composite resin shades to be used to restore the teeth (Figure 13). Then, total removal of the failing composite resin restoration and decay was performed. For minimally invasive preparation purposes a caries detector (SEEK®, Ultradent Products, https://www.ultradent.com) was used so that only the infected caries was removed, leaving the affected dentin. A double-bevel margin was then performed along the facial so that blending of the final composite resin to the existing dentition could be attained.24 For tooth No. 9, only the surface of the enamel was roughened (Figure 14).
There are several "keys" to achieving a successful Class IV restoration. Proper understanding of composite resin shade selection, preparation design, and the sequence of composite-resin layering is important in attaining an accurate blending of the composite resin to the existing restoration. In addition, proper finishing and polishing technique is equally essential in obtaining a seamless and invisible esthetic restoration.
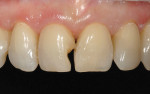
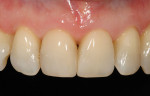
In restoring both teeth, the prepared sites were first pumice-cleaned with flour of pumice, then a clear matrix strip (Epitex, GC America) was placed interproximally before etching with 32% to 37% phosphoric acid (Uni-Etch®, BISCO, https://www.bisco.com). A dentinal adhesive (eg, ALL-BOND SE®, BISCO; G-BOND™, GC America, and CLEARFIL™ SE Bond, Kuraray Dental, https://www.kuraraydental.com,) was placed with all the matrices still in place. The clear matrix was used to prevent getting any adhesive onto the adjacent proximal surfaces of the tooth (Figure 15. Using the latest-generation of nano-hybrid composite resin (GC Kalore), a sequence of composite-resin layering was done to blend the composite resin to the existing tooth and create a polychromatic effect. Universal shade A-1 was placed along the lingual to mimic the lingual enamel coloration. Then, as a dentin replacement, opacious dentin shade (GC Kalore AO-2) was placed to assist in blocking out any shine-through of light (Figure 16). Using a free-hand sculpt technique, universal shade A-1 was sculpted over the opacious dentin composite resin with an emphasis on placing internal anatomy to simulate natural dentition. After placement of subtle characterizations with tints (Kolor + Plus®, Kerr Corporation, https://www.kerrdental.com), a neutral translucency (GC Kalore NT) was used as the final layer to create the chameleon effect (Figure 17 and Figure 18).25-27 For tooth No. 9, a simplified composite resin procedure was done with only A-1 and NT to restore its natural beauty.
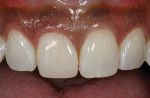
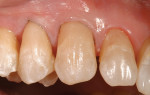
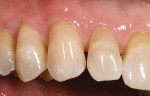
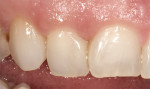
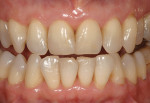
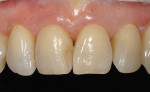
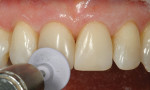
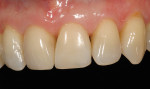
After final light-curing, esthetic contours were refined using aluminum-oxide finishing disks (SofLex™, 3M ESPE), finishing burs (composite finishing and polishing kit, Brasseler USA, https://www.brasselerusa.com) and finishing paste (micro-diamond polishing paste, Ultradent) (Figure 19, 20, 21). For a more simple polishing technique, using a micro-diamond polishing system can be used as well. By using proper technique and state-of-the-art dental materials, natural color, contour, and finish to mimic the natural tooth can be achieved (Figure 22, 23, 24, 25).28
Conclusion
In the development of MID, it is important to explore progressive ideas in order to preserve the natural dentition. With advances in innovative materials, new and improved clinical techniques are developed to meet these ideals. For example, the latest advancement in composite resins may offer long-term solutions to what was once considered a short-term restoration.
In cosmetic/restorative dentistry, clinicians have become accustomed to using a purely adhesive model in restoring tooth structure. However, with the progress of bioactive materials like RMGIs, clinicians can therapeutically control caries and heal demineralized dentition through remineralization procedures. Additionally, with the new generation of composite-resin restorative materials, cavity design can be modified so that minimal intervention can be attained without the sacrifice of strength and beauty.
References
1. Mount GJ, Ngo H. Minimal intervention: A new concept for operative dentistry. Quintessence. 2000;31(8):527-533.
2. Mount GJ. Minimal intervention dentistry: rationale of cavity design. Oper Dent. 2003;28:92-99.
3. Hicks J, Garcia-Godoy F, et al. Fluoride-releasing restorative materials and secondary caries. J Calif Dent Assoc. 2003;31(3):229-245.
4. Mount GJ, Ngo H. Minimal intervention: Advanced lesions. Quintessence. 2000;31(9):621-629.
5. Kugel G, Perry R. Direct composite resin: an update. Compend Cont Educ Dent. 2002;23(7):593-603.
6. Mitra SB, Wu D, Holmes BN. An application of nanotechnology in advanced dental materials. J Am Dent Assoc. 2003;134(10):1382-1390.
7.Ubassy G. Shape and color: The key to successful ceramic restorations. Quintessence. 1993.
8.Rufenaght CR. Fundamentals of Esthetics. Chicago, Ill: Quintessence Publishing Inc: 1990.
9. Sieber C. Voyage: Visions in Color and Form. Chicago, Ill: Quintessence Publishing Inc: 1994.
10. Magne P, Holz J. Stratification of composite restorations: systematic and durable replication of natural aesthetics. Pract Perio Aesthet Dent. 1996;8(1):61-68.
11. Terry D. Direct reconstruction of the maxillary anterior dentition with composite resin: a case report. Pract Perio Aesthet Dent. 1999;11(3):361-367.
12. Muia PJ. Esthetic restorations: improved dentist-laboratory communication. Carol Stream, Ill: Quintessence; 1993:141.
13. Fahl N, Denehy GE, Jackson RD. Protocol for predictable restoration of anterior teeth with composite resins. Pract Perio Aesthet Dent. 1995;7(8):13-21.
14. Evaluation on Kalore NanoHybrid composite resin. Reality Esthetics Publishing Company; Houston, Texas: April 29, 2010.
15. Clinician's Report. 2009;3(3).
16. Mount GJ, Ngo H. Minimal intervention: Early lesions. Quintessence. 2000;31(8):536-546.
17. Markovic DL, Petrovic BB, Peric TO. Fluoride content and recharge ability of five glass ionomer dental materials. BMC Oral Health 2008. BioMed Central Ltd. July 2008.
18. Yan Z, Sidhu SK, Mahmoud G, McCabe J. Continous fluoride recharging of glass ionomer. Abstract 649. 84th General Session of the IADR 2006, Brisbane Australia.
19. Lin A, McIntyre NS, Davidson RD. Studies on the adhesion of glass-ionomer cements to dentin. J Dent Res. 1992;71(11):1836-1841.
20. McLean JW. Dentinal bonding verses glass-ionomer cements. Quintessence. 1996;27(10):659-667.
21. Tay FR, Sidhu SK, Watson TF, Pashley DH. Water-dependent interfacial transition zone in resin-modified glass-ionomer cement/dentin interfaces. J Dent Res. 2004;83(8):644-649.
22. Trushkowsky RD, Gwinnett JA. Microleakage of Class V composite, resin sandwich, and resin-modified glass ionomer. Am J Dent.1996;9(3):96-99.
23. Davidson CL. Glass-ionomer bases under posterior composites. J Esth Dent. 1994;6(5):223-226.
24. Fahl N, Swift E. The invisible Class IV restoration. J Esthet Dent. 1989;1:111-113.
25. Duarte S, Perdigao J, Lopes M. Composite resin restorations: natural aesthetics and dynamics of light. Pract Proced Aesthet Dent. 2003;15(9):657-664.
26. Fahl N Jr. Achieving ultimate anterior esthetics with a new microhybrid composite. Compend Contin Educ Dent. 2000;26:4-13.
27. Lopes GC, Luiz CCV, Araujo E. Direct composite resin restoration: A review of some clinical procedures to achieve predictable results in posterior teeth. J Esthet Rest Dent. 2004;16(1):19-32.
28. Barghi N. Surface polishing of new composite resins. Compend Cont Educ Dent. 2001;22(11):918-924.