Medium Field of View CBCT Imaging and the General Practice
General dentists can benefit from 3-D capabilities.
Innovations in dentistry offer patients more options for treatment than ever before. In the past, general dentists referred many of these cases to specialty practices because they did not have the proper diagnostic tools to tackle the cases. One of the most integral parts of proper treatment for any procedure is having the most specific information on the patient's condition. Cone beam computed tomography (CBCT), or 3-D scan, provides a view of the mouth that gives more details regarding precise tooth positions, bone dimension and quality, temporomandibular joint (TMJ) disorders, and other dental conditions.1 General dentists can greatly benefit from 3-D capabilities, especially during times of down economics-it is beneficial to keep procedures in-house.
When making a decision on what radiographic modality should be chosen, doctors need to be keenly aware of ALARA (As Low As Reasonably Achievable) and set their own radiographic protocols for ALARA. One of the deciding factors of the selection of CBCT machine (Gendex GXCB-500 HD™-powered by i-CAT®) was that it is on the lowest end of the dosage scale for CBCT machines.2
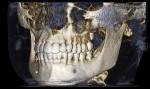
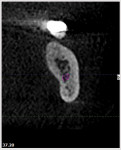
Embarking on some of the procedures that used to be "relegated for referral" takes confidence. While some practitioners need a full field, a medium field of view offers enough data to provide an expanded repertoire of procedures for most general dentists.3 The author's cone beam system has two diameters, 8 cm and 14 cm. Either of those options can be collimated from 2 cm to 8 cm in height. Typically, the 8 cm x 4 cm will give the author an arch. The 14 cm x 8 cm is helpful for TMJ evaluation and airway analyses (Figure 1), and there also is the option of an 8-cm x 8-cm scan. If the clinician needs a full field of view, images can be "stitched" together with the software. These size choices give the clinician flexibility to perform procedures that require exploration of certain areas.
As a general practitioner, the author feels confident reading scans within the medium field because the image data represents the area in which he works every day. With a 3-D format, the clinician can rotate or slice though the anatomy in any direction-views not possible with 2-D. Having a 3-D view increases the author's confidence level. With 2-D, too many "ifs" exist that could interfere with the smooth course of treatment. Dentists can change the "what ifs" of these cases to "what is" by using 3-D technology for procedures such as implants, impacted third molars, and root investigation, some of the most commonly performed procedures by general dentists.
Implants
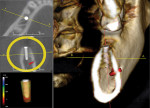
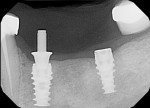
One of the fastest-growing areas of dentistry is the placement of dental implants.4 For implants, the author typically uses a standard 0.3-voxel, 8-cm x 8-cm scan for maxillary placement or 14-cm diameter scan for mandibular posterior implants. Together with implant software, cases can be planned out fairly easily (Figure 2). Having a CBCT scan can avoid implant placement that is non-parallel, too lingual, too buccal, too close together, or placed in sinuses or in inadequate bone.5 While the standard scan acquires information about the maxilla and mandible, in some implant or full-mouth rehabilitation cases, it would be prudent to include the TMJ complex and the paranasal sinuses as well. The adequate field of view should capture the region of interest, while avoiding the necessity for multiple scans, which increases the radiation dosage to the patient.6 Dentists need to be armed with enough information of the implant's proximity to the nerve and sinus, as well as width, depth, and height of the bone to avoid possible complications. If the scan is expanded to 14 cm, the clinician can trace from where the intra-alveolar nerve enters the mandible to see the beginning and the end of the nerve path.
Impactions
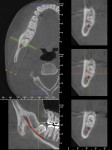
For impacted third molars, the author typically uses a 0.3-voxel, 14-cm x 8-cm, 8.9-second scan. This medium-resolution scan and the software allow the dentist to view the anatomy from many 3-D orthogonal views (sagittal, axial, or coronal planes). Oblique, curved-plane slicing or paging through the voxel layers allows visualization of internal anatomy. In impaction cases, it is vital to establish the relationship of the various dental structures to each other, such as adjacent teeth, the mandibular canal (Figure 3), fossae, sinuses, and alveolar ridge boundaries. Many times the pathology of the impaction is not visible with 2-D imaging, such as a supernumerary tooth or neoplasm, or pathology adjacent to or secondary to an impacted tooth, such as cysts, tumors, or inflammatory processes.7
Root Investigation
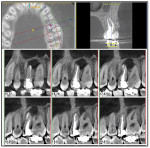
For endodontics, a 4-cm x 8-cm area usually suffices. The author often finds it important to have the full arch in view to compare the anatomy on the mirrored side.8 Sometimes a patient will arrive at the office with pain symptoms that point to a tooth that has already been endodontically treated. In this case, often by using axial slices, a poorly obturated or missed canal can be visualized that was undetectable on a 2-D image. To detect a condition such as a root fracture, the CBCT should be set on a higher resolution, typically 0.2 or 0.25 voxels. Unless the scan is needed for other purposes, the author narrows it down to one arch. By scrolling through the "TMJ viewer," he can visualize a buccal-to-lingual view and, in slices (Figure 4), he can rotate the tooth in question by 360°. In 3-D, all sides of the tooth that would be blocked by superimposition on 2-D can be viewed.
TMJ Dysfunction and Airway Studies
When evaluating TMJ dysfunction, the author can capture the nose, the upper airway, the mouth, and the hyoid bone. If a patient presents for evaluation with symptoms of obstructive sleep apnea (OSA), the author orders a 8-cm x 14-cm, 0.3- or 0.4-voxel scan which allows him to see all necessary structures, from the lower orbit to the epiglottis. The patient needs only to be correctly positioned to capture the area of interest for airway and TMJ studies.
Medium FOV gives the upper airway, including the sinuses and oral pharynx to the epiglottis, in the author's experience in more than 95% of the cases he sees in his general practice. For those tall and large individuals, two images can be stitched together. The few patients who fall in that category do not, in the author's mind, justify the additional expense of a full-field machine for typical general dentistry applications.
Furthermore, Hatcher et al report that 3-D imaging can identify narrowing of the airway.9 As a former critical care respiratory therapist, treatment of obstructive sleep apnea and airway analysis has always been a part of the author's dental practice. According to the American Academy of Sleep Medicine, obstructive sleep apnea (OSA) kills 38,000 people each year, and is undiagnosed in 80% to 90% of people who suffer from it.10 Recent developments in software allows for CBCT evaluation of the airway space, aiding in the treatment of OSA. There is a relationship between airway area and the likelihood of obstructive sleep apnea, according to Schendel and Hung in their respective articles.11,12
Case Introduction
Clinicians often struggle with what field of view would be most beneficial for their use when contemplating adding 3-D technology to their practice. The following case illustrates how a medium field of view unit should be appropriate for most practitioners.
Patient Profile
A 75-year-old man presented as an emergency visit with a chief complaint of a loose fixed partial denture (FPD) on the lower left, extending from teeth Nos. 17 through 22. The oral examination yielded the following findings:
- Abutments for bridge on teeth Nos. 17, 20, and 22
- Detached abutments on teeth Nos. 20 and 22
- Obvious swelling into buccal vestibule on tooth No. 20
- Stable periodontal and tmj systems
- Maxillary porcelain-fused-to-metal restorations throughout
- Excessive wear of mandibular anteriors
- No patient report of pain
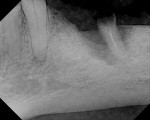
Digital periapical X-rays (DEXIS, https://www.dexis.com) were ordered to assess the abutment conditions. The patient was educated about the non-restorability of his current situation. The bridge was sectioned at the mesial of tooth No. 18 and the distal of tooth No. 22. An additional digital X-ray was taken of the pier abutment on tooth No. 20 to evaluate the height of bone (Figure 5).
Treatment options of removable partial denture vs implant-retained FPD were presented. The patient elected to have implants placed. A CBCT scan was ordered to evaluate available bone for implants.
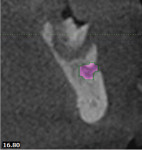
A cross-sectional slice shows the extent of bony destruction associated with tooth No. 20 and the position of the mental foramen (Figure 6). Because the scan encompassed both the mandible and maxilla, as the scan was read, additional findings were discovered for which the patient was unaware:
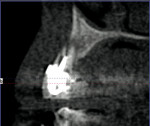
- Periapical pathology and root fracture of tooth no. 6 (Figure 7)
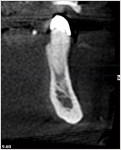
- A radiolucency of tooth no. 22 (Figure 8).
- An impacted third molar on tooth no. 32.
- An undercut of the mandible for implant positioning (Figure 9).
Because of the amount of bone destruction and the undercut of the mandible, guided surgery was prescribed.
Course of Treatment
Tooth No. 20 was removed with extensive debridement including use of a CO2 laser. The site was grafted and allowed to heal while root canal therapy was performed on tooth No. 22 (Figure 10). After 4 months, implants (NobelActive™ using the NobelGuide™ protocol; Nobel Biocare, https://www.nobelbiocare.com) were placed in the Nos. 19 and 21 sites (Figure 11 and Figure 12). After placement of the implant restoration, the cantilever would be removed and an additional implant would be placed in the No. 18 site.
Case Summary
Several typical situations present with older populations requiring extensive dental treatment, and a small field of view 3-D machine would have missed additional findings not associated with the chief complaint area. While the lower left area is first to be restored, a long-term approach to treatment can ideally be discussed instead of the "wait until something happens" approach.
Conclusion
Besides helping to develop new procedures, CBCT scans can also help to define what procedures may be too complicated to undertake. These should be referred to a colleague who will appreciate the patient bringing a copy of the most comprehensive radiography possible. CBCT imaging has opened many new doors for all dentists, but general practitioners can now take a step across the threshold to new and invigorating procedures, with increased confidence in successful outcomes.
References
1. Ganz SD. The reality of anatomy and the triangle of bone. Inside Dentistry. 2006;2(5): 72-77.
2. Ludlow JB, Ivanovic M. Comparative dosimetry of dental CBCT devices and 64-slice CT for oral and maxillofacial radiology. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2008;106(1):106-114.
3. Levato CM, Farman AG, Chenin D. Cone-beam computed tomography: a clinician's perspective. Inside Dentistry. 2009;5(5):66-73.
4. Levin RP. A breakthrough in implant dentistry. Dentistry IQ. 2009. Available at: https://www.dentistryiq.com/index/display/article-display/363108/articles/dental-economics/volume-99/issue-5/features/focus-on/a-breakthrough-in-implant-dentistry.html.
5. Fine D. Cone beam -awareness in 3 dimensions. Dental Tribune: Greater New York Dental Meeting. 2009;4(2).
6. Howerton WB. CBCT imaging: Discussing the field of view concept. Osseonews. 2009. Available at: https://www.osseonews.com/cbct-imaging-discussing-the-field-of-view-concept/.
7. Curley A, Hatcher DC. Cone beam CT -anatomic assessment and legal issues: The new standards of care. J Calif Dent Assoc. 2009;37(9):653-62.
8. Wong R. 3D for endodontics: Avoiding surprises down under. Dr. Bicuspid. 2009. Available at: https://www.drbicuspid.com/index.aspx?sec=sup&sub=img&pag=dis&ItemID=303126.
9. Hatcher DC. Cone beam computed tomography: craniofacial and airway analysis. Sleep Medicine Clinics. 2010;5(1):59-70.
10. American Academy of Sleep Medicine. Obstructive Sleep Apnea Fact Sheet. Available at: https://www.aasmnet.org/Resources/FactSheets/SleepApnea.pdf. Accessed August 23, 2010.
11. Schendel S, Hatcher D. Automated 3-dimensional airway analysis from cone beam computed tomography data. J Oral Maxillofac Surg. 2010;68(3):696-701.
12. Hsiag Tso H, Lee JS, Huang JC, et al. Evaluation of human airway using cone beam CT. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2009;108(5):768-776.
About the Author
Terry Myers, DDS
Private Practice
Belton, Missouri