"No-Prep" Veneers
Demand and desire for more conservative preparations begins to drive this new area of esthetic dentistry.
As someone who has practiced restorative cosmetic dentistry for more than 25 years, the author has seen many trends regarding techniques and materials come and go. However, in recent years, a new trend has emerged that will not likely be reversed: the movement toward more conservative preparations and even no preparation for many cosmetic smile design cases.1,2 It is the author’s strong belief that this trend is here to stay as the consumer, when given a choice, will always seek out more conservative alternatives. In the world of medicine, there are numerous examples of this steady migration toward less invasive procedures; dentistry will undoubtedly follow the same path.
Case selection for “prepless” veneers is critical, and, clearly, additive-only restorations are not for every situation. The case types that may be well-suited for no-preparation veneers are:
- microdontia such as peg laterals, tooth-to-arch discrepancies, and, in general, undersized teeth.
- short, worn teeth that have lost volume due to occlusal wear, abrasion, erosion, or some combination of these factors.
- bicuspid extraction orthodontic cases where anterior teeth are overly lingualized and the arch form is narrow.
- large lips that create a big frame and allow enlargement of the teeth for proper proportion.3,4
Though our profession tends to lump minimal preparation and no preparation together as the same basic procedure, the average consumer sees the two as totally different—and so does the author. Both approaches have their place, and both can be very effective in creating beautiful, long-lasting smiles; however, a pure no-preparation case offers the patient a reversible option that, for many, is critical to moving forward with treatment. The author is aware that many dentists feel that no veneer is reversible and that some degree of “damage” is inevitable upon removing prepless veneers, but new technology such as the erbium laser offers the capability to “pop off” porcelain veneers by obliterating the composite cement.5 In addition, slow and meticulous use of diamond and carbide burs under magnification can remove porcelain veneers with an enamel alteration similar to orthodontic bracket removal. While technically there is some enamel alteration when viewed under magnification on a dry tooth, the practical effect is insignificant, especially from the patient’s perspective.
Even if the patient is agreeable to enamel reduction, this reduction can significantly alter the underlying tooth color, making it darker and more likely to shine through a very thin veneer, especially in critical zones such as the interproximal areas. With the average enamel thickness being 0.3 mm to 0.5 mm in the cervical area of the upper incisors, it takes very little preparation to considerably darken the underlying color and ultimately make the margin more visible.6 Enamel reduction can certainly offer improved contours in many cases, but it can also bring difficulty and compromise in color; it should always be carefully thought out in terms of benefit vs risk.
This article will focus on a pure “no-prep” approach, and the case that follows was done with absolutely no preparation to the teeth.
Patient History
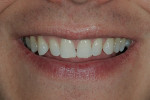
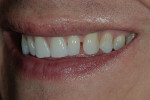
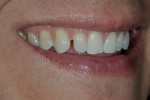
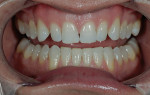
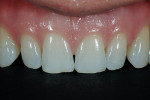
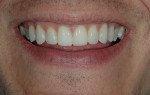
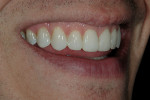
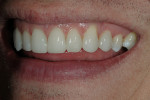
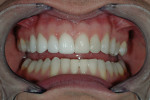
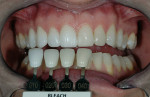
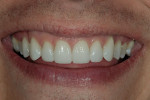
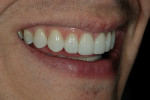
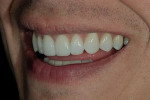
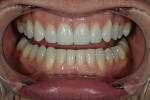
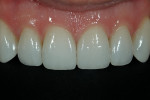
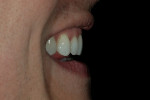
The patient was a 32-year-old male dentist who originally came to us to observe our computer software and then subsequently grew interested in our no-prep veneer approach to smile design. He had recently completed orthodontic treatment to correct alignment issues and improve his occlusion, and there were significant spaces remaining between the upper laterals and cuspids on both the right and left sides (Figure 1, Figure 2, Figure 3, Figure 4). The patient also expressed concern about the dark triangle between the upper centrals, and he specifically voiced his desire that there be little to no dark triangles once the work was completed. His basic goals were to enhance his present smile by eliminating the spaces and black triangles while brightening the color and repairing the worn and chipped incisal edges. Like so many patients in today’s world, he did not love his existing smile but also did not hate it enough to consent to reducing his teeth with a handpiece, especially if there was another way.
Clinical Data
The clinical examination revealed an overall healthy mouth with no evidence of periodontal disease. An oral cancer screening was negative, and a full radiographic series revealed no pathology. Several small to medium occlusal composites were noted in the posterior, but all appeared to be serviceable. The temporomandibular joint was healthy and asymptomatic, but slight wear was noted on upper and lower anterior teeth. Tooth No. 10 had a horizontal craze line in the incisal third, but was otherwise asymptomatic (Figure 5). Anterior guidance was present in both lateral and protrusive movements, and the occlusion was Angle’s Class 1 on both the right and left sides.
Diagnosis
The patient’s oral health was excellent, and the chewing system was stable and comfortable. The wear present on the anterior teeth provided evidence of a constricted envelope of function, but the Invisalign treatment appeared successful in improving stability of the occlusion and providing a comfortable “driveway.” Prepless veneers were an excellent treatment option for this patient due to the slight incisal wear, the overall narrow tooth size in relation to the arch width, the slight lingualized axial inclination of the upper anterior teeth, and the pleasing existing color (~030). Not only would they provide excellent esthetic results, but the fact that they were bonded to 100% enamel and were facial to the existing envelope of function are huge factors in terms of longevity and durability.7,8
Treatment Plan
To create the final treatment plan, a complete AACD-recommended photographic series was taken along with accurately mounted study models to thoroughly evaluate both esthetics and function. As always, the treatment plan was approached from the perspective of what is the least number of restorations necessary to accomplish the patient’s goals. After careful consideration, the following plan was created:
- Create eight composite prototypes (spot-etched) to provide the laboratory with an exact blueprint for final restorations and to allow patient to “test drive” the restorations
- Eight no-prep Durathin veneers (by Experience Dental Studio)
- Tray bleaching for the lower arch with 16% NiteWhite® ACP (Discus Dental, www.discus.com)
In some cases it would be necessary to do a composite mock-up in the mouth to verify that additive-only restorations will produce the desired visual outcome, but in this case both the patient and the author were confident enough to move forward without the mock-up. The custom composite prototypes will serve as the ultimate visualization for the patient, the dentist, and the laboratory.
Preparation
Obviously, with prepless dentistry there is no preparation with a high-speed handpiece, and the only minor alteration necessary in some cases is to smooth the incisal edges with a course Sof-Lex™ disc (3M ESPE, www.3mespe.com) to remove sharp internal surfaces, and that was done for this case. All of the teeth were then cleaned with an Enhance® polishing cup (DENTSPLY Caulk, www.caulk.com) to ensure there was no plaque or debris on the teeth. Two master impressions were captured with Precision® heavy- and light-body impression material (Discus Dental, www.discusdental.com). This is routine in the author’s practice so that he does not get the dreaded call from the laboratory to remove the prototypes and make a new master impression. A Kois Facial Analyzer was used for proper orientation in a Panadent articulator (www.panadent.com), and a centric relation bite was captured using Blu-Mousse® (Parkell, www.parkell.com). Shade photographs were taken of the existing color, and then it was time to focus on creating the prototypes.
Custom composite prototypes were fabricated by hand using Tetric Evo Ceram (Ivoclar Vivadent, www.ivoclarvivadent.com) shade Bleach L. spot-etching approximately 2 mm to 3 mm. This is a great composite for this application as it is very viscous and does not slump or stick to the composite instrument. The Bleach L color is also a great choice for providing a nice white hue (020 range) while maintaining enamel-like translucency. Both centrals were formed before curing to maintain symmetry, followed by both laterals, both cuspids, and then both bicuspids. In other words, two were done at a time before curing and moving to the next two teeth. Final contouring was done with burs and sandpaper disks to create proper line angles and facial anatomy, followed by polishing with a #12 Robinson Bristle brush and Diashine polishing paste (Brasseler USA, www.brasselerusa.com) (Figure 6, Figure 7, Figure 8). Once the prototypes were finished, the patient was dismissed and asked to “test drive” the prototypes for several days.
Laboratory Instructions
After the patient had time to evaluate the prototypes, a follow-up visit was scheduled in preparation for a hand off to the laboratory. The patient was very pleased with the prototypes, and, therefore, the architecture of the case was clearly established along with proper phonetics and occlusion. Photographs of the prototypes, along with an accurate polyvinyl impression, were taken so that the laboratory could copy the restorations with a silicone matrix of the model. The communication of color and incisal effects is much more difficult to do, but the prototypes do provide a great deal of information in the color arena as well. Through years of doing these cases, the laboratory knows which porcelain powders to use to match the 020 composite. If the patient desires a brighter or darker shade than the prototypes, adjustments are made in the powder selection to match the requested shade. Because the thickness of these restorations greatly affects the final shade, it is invaluable to have a reference in color using the same thickness as the final restorations.
In this case, the final instructions to the laboratory were:
- Eight feldspathic prepless veneers for teeth Nos. 5 through 12
- Copy the prototypes in shape, length, facial anatomy,
- Place the margins just slightly shy of the tissue line
- Make the shade a slightly brighter color than the prototypes; somewhere between 010 and 020
- Make incisal translucency and characteristics similar to the original teeth
Insertion and Finishing
After receiving the restorations from the laboratory, they were carefully inspected for overall integrity and then placed on the master model to compare visually to the prototype model. It is always wise to handle these delicate restorations over a foam pad to ensure that they do not fall on a hard surface and break. Following the author’s normal protocol, the patient was anesthetized to ensure comfort during the insertion process, as the chemicals and post-cementation finishing can be quite uncomfortable despite the fact that the teeth have not been prepared. The prototypes on the right side only were removed to compare the length, facial contours, etc of the prototypes to the final restorations (Figure 9). This is an important step to ensure that the laboratory duplicated the prototypes the patient approved. In addition, the shade was checked using clear try-in gel to verify that the color and effects were very close to what was ordered (Figure 10).
In this case, the laboratory matched the blueprint very nicely, so the remaining prototypes were removed and all of the veneers were placed on the teeth with clear try-in gel to verify overall esthetics, fit, and appropriate contacts. A rubber dam was then placed and the veneers were prepared along with the teeth using the exact same protocol as traditional veneers. Clear Variolink® cement (Ivoclar Vivadent) was used as the luting cement; it works nicely for thin veneers because they need a low-viscosity resin that requires minimal pressure to seat. All of the veneers were seated at once and spot-tacked into place with a 2-mm light tip. After the initial cement clean-up, the resin was completely polymerized.
The margins were finished into an “infinity margin” using “mosquito” finishing diamonds (Axis Dental. www.axisdental.com). Once the margins were no longer detectable with an explorer, they were refinished using the Optra-Fine intraoral porcelain polishing system (Ivoclar Vivadent) followed by a #12 Robinson bristle brush and Diashine polishing paste. Careful attention was given to not traumatize the tissue by using deflecting retraction instruments. In addition, continuous air was blown on the teeth while polishing to guard against overheating.
The occlusion was evaluated and adjusted in centric occlusion and in lateral and protrusive movements. The lingual margins were then smoothed with a diamond-impregnated pre-polisher wheel (Axis Dental), followed by a final polish with Robinson Bristle brush and Diashine polishing paste (Figure 11, Figure 12, Figure 13, Figure 14, Figure 15, Figure 16, Figure 17).
Conclusion
No-prep porcelain veneers have been around for more than two decades, and the incredible success of bonding porcelain to 100% enamel is well-documented.9,10 Now, there are refined techniques, new and improved materials, and better training in emulating nature so that the end result of prepless veneers can rival or exceed the results of traditionally prepared veneers. Contrary to common thinking, this style of dentistry is not easy; in fact, if done well, this approach can require more skill and expertise than traditional porcelain veneers.
Dr. John Kois is quoted as saying, “the best dentistry is no dentistry,” and that is certainly true.11 By minimizing risk factors, prepless dentistry can be an intensely rewarding procedure for both the dentist and the patient. Minimally invasive dentistry continues to be what patients want, and it continues to be one of the most exciting areas of the profession.
Disclosure
The author is a co-developer of Durathin prepless veneers and has received financial/material support for his work with Durathin prepless veneers.
Acknowledgment
The author would like to thank Mark Willes, co-developer of Durathin Veneers and owner of Experience Dental Studio, for the ceramic work featured in this article.
References
1. DiMatteo AM. Prep vs no prep: The evolution of veneers. Inside Dentistry. 2009;5(6):72-79.
2. Radz GM. Enhancing the esthetics through addition: No prep porcelain veneers. Oral Health. April 2009;23-30.
3. Strasseler HE. Minimally invasive porcelain veneers: Indications for a conservative esthetic dentistry treatment modality. Gen Dent. 2007; 55(7):686-694.
4. Wells DJ. Don’t we all do cosmetic dentistry? Dent Econ. 200797(4):106-109.
5. Morford C, Buu N, Finzen F, et al. Contemporary Topics in the Use of Erbium Lasers. Presented at: Academy of Laser Dentistry—Miami Conference. April 14-17, 2010.
6. Crispin BJ. Esthetic moieties: enamel thickness. J Esthetic Dent. 1993;5:37.
7. Friedman MJ. A 15-year review of porcelain veneer failure: A clinician’s observations. Compend Contin Educ Dent. 1998;19(6):625-632.
8. Kois, JC. Functional Occlusion I: Science Driven Management. Kois Center, Seattle, Washington.
9. Calamia JR, Calamia CS. Porcelain laminate veneers: Reasons for 25 years of success. Dent Clin N Am. 2007;51:399-417.
10. Calamia JR. Etched porcelain facial veneers: A new treatment modality based on scientific and clinical evidence. NY J Dent. 1983;53(6):255-259.
11. Kois JC. Treatment Planning I. Kois Center, Seattle, Washington.
About the Author
Dennis Wells, DDS
Private Practice
Nashville, Tennessee