Sequencing Crown Lengthening and Orthodontic Treatment
The relationship between restorative dentist, periodontist, and orthodontist is critical through diagnosis and sequencing of treatment to finishing the case.
Along with the increased emphasis on interdisciplinary treatment planning, there is a concomitant need for greater cooperation between the restorative dentist and the supporting specialists. This is especially true for the interdisciplinary relationship between the restorative dentist, the periodontist, and the orthodontist. It is the purpose of this article to discuss the diagnosis and sequencing of treatment for a specific group of patients. These patients present with a need for orthodontic alignment of their teeth and have excessive gingival coverage of their clinical crowns due to altered passive eruption.
Altered passive eruption is a condition that was described by Coslet et al1 more than 30 years ago. They differentiated these patients into four categories based on the position of the alveolar bone in relation to the cementoenamel junction (CEJ) and the mucogingival junction. However, the clinical treatment of these patients is the same2,3; therefore, the term altered passive eruption will be used to describe all of the categories of excess gingival coverage of the anatomic crown.
To diagnose a patient with altered passive eruption, two criteria must be met. First, the tooth is short by measurement. The average length of the clinical crown of the normal maxillary central incisor is 10 mm to 11 mm.4 Second, the CEJ cannot be detected in the sulcus with the tip of an explorer. In a patient with a normal attachment apparatus, the CEJ can be detected in the sulcus due to its roughness, compared to the smoothness of the enamel. However, in the patient with altered passive eruption, the dentist can only feel smooth enamel all the way to the base of the sulcus. The CEJ cannot be felt because it is covered by the attachment apparatus.
The gummy smile is generally defined as more than 2 mm of gingival display in full smile. Tjan5 reported on the smile dynamics of a population in the second decade of life. He reported 2 mm or more of gingival display in 13.8 % of females and 6.8% of males. However, altered passive eruption is only one of four possible etiologies of the gummy smile. The other etiologies include short/hyperactive upper lip, dentoalveolar extrusion, and vertical maxillary excess.3 More recently, Konikoff et al6 reported on the prevalence of short clinical crowns due to excess gingival coverage of the anatomic crowns, based on the width-to-height ratio, in postorthodontic teenagers. They found 66% of the patients studied had a width-to-height ratio in maxillary central incisors greater than 80%. The normal width-to-height ratio is 75% to 80%.4 It is obvious from this data that there are many postorthodontic patients who would benefit from esthetic crown lengthening surgery.
In order to understand altered passive eruption, it is important to first understand the normal eruption process, which consists of two stages.7 The first stage is termed active eruption. As the crown of the tooth forms, it begins to erupt through the bone and soft tissue and grows down into the mouth. It continues to actively erupt until it couples with the opposing tooth into a stable occlusal relationship. At this point, for all practical purposes, active eruption is complete. Growth of the maxilla and mandible will continue, but eruption of the tooth out of the alveolar process is complete. However, at the completion of the active eruption process, the clinical crown may only be 5 mm to 6 mm in height. At this point, the second stage of the eruption process, termed passive eruption, begins. Passive eruption is the apical migration of the gingival tissue up the anatomic crown until it gets to within approximately 1 mm of the CEJ. At this point, the tissue stabilizes, resulting in an average of 10 mm to 11 mm in clinical crown length.
In altered passive eruption, the tissue does not migrate to its correct position 1 mm coronal to the CEJ. This results in excessive gingival coverage of the cervical enamel and a short clinical crown. Research has shown that the normal eruption process of the anterior teeth is essentially complete at approximately 15 to 16 years of age.8 It is at this age that esthetic crown lengthening surgery is generally recommended.
The diagnosis and surgical treatment of altered passive eruption may be complicated by the presence of orthodontic appliances. The common question arises as to the correct timing of the esthetic crown lengthening procedure, before, during, or after orthodontic treatment. If the excess gingival tissue makes it difficult or impossible to bond the brackets, the surgery must be done prior to orthodontic treatment.
However, if bracket placement is not a problem, the decision is based on the restorative treatment plan for the patient. In the first scenario, the patient is diagnosed with altered passive eruption, either before or during orthodontic treatment, but has no need for anterior restorative dentistry after completion of orthodontics. In this case, final tooth positions are dictated to the orthodontist by the correct incisal edge positions of the maxillary anterior teeth. Therefore, the case is not finished based on gingival levels, but rather incisal edge position. It is significantly more difficult to do the esthetic crown lengthening surgery with the orthodontic appliances in place. Therefore, in these patients, the surgery is accomplished after removal of the appliances.
In a second scenario, the orthodontic patient with altered passive eruption does require restorative dentistry at the completion of orthodontics, or there is doubt about the correct placement of the incisal edge positions. In these patients, the crown lengthening surgery must be accomplished during orthodontic treatment. The requirement for restorative dentistry is generally due to incisal wear or to a tooth/arch discrepancy, which results in small teeth with excessive interdental spacing. The teeth must be orthodontically positioned correctly both apico-coronally and mesio-distally prior to restoration. Because the incisal edge positions may be managed restoratively with composite or porcelain, the apical/coronal positions of the maxillary anterior teeth are dictated by the leveling of the CEJs. However, the orthodontist cannot level the CEJs because their positions are unknown due to the excessive gingival coverage. It is also imperative that the teeth be moved into the correct positions mesio-distally. This positioning is dictated by the width-to-height ratios of the teeth. However, the correct width-to-height ratios cannot be determined until the gingival tissue is moved to the correct position adjacent to the CEJs. For these reasons, it is imperative that the esthetic crown lengthening surgery be accomplished prior to removal of orthodontic appliances when the teeth will receive restoration at the completion of orthodontics. This allows the orthodontist to move the teeth into their correct positions so that the gingival tissue is level and the gingival line is in the correct position in the full smile, and the teeth are in the correct positions mesio-distally so that the restorative dentist may place restorations that are proportionally correct.
The timing of esthetic crown lengthening surgery is variable. It has been the author’s experience that when the crown lengthening surgery is done prior to placement of orthodontic appliances, a second-stage touch-up surgery is commonly required after de-banding. In addition, it is very difficult and commonly impossible to do the crown lengthening surgery when the teeth are crowded and/or rotated. The teeth must first be aligned orthodontically prior to the surgery. For these reasons, the surgery is usually accomplished approximately 6 months prior to de-banding. This gives the orthodontist time, after the surgical procedure, to move the teeth into their correct positions.
Case Presentation
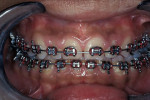
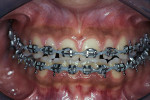
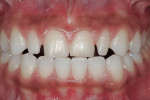
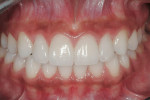
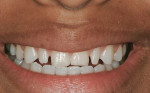
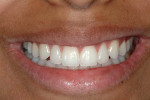
This 16-year-old patient presented with a maxillary tooth/arch discrepancy resulting in excess interdental spacing (Figure 1). She also presented with altered passive eruption on her maxillary anterior teeth as diagnosed by short clinical crowns and the inability to feel the CEJs in the sulci. Orthodontic treatment was begun to align the teeth, with emphasis on canine tooth positions and anterior guidance (Figure 2). Approximately 6 months prior to de-banding, esthetic crown lengthening surgery was performed on teeth Nos. 5 through 12 (Figure 3 and Figure 4). Note that the tooth positions were orthodontically changed both apico-coronally and mesio-distally after the surgical procedure. After debanding, porcelain veneer restorations were placed on teeth Nos. 7 through 10 (Figure 5, Figure 6, Figure 7, Figure 8).
Conclusion
It has been the purpose of this article to first discuss the prevalence of altered passive eruption in the adolescent orthodontic population. The second goal has been to present a rationale for timing of esthetic crown lengthening surgery in the orthodontic patient.
Acknowledgment
The author thanks Dr. Bloyce Britton for the orthodontic treatment and Steve McGowan, CDT, Arcus Dental Laboratory, for the porcelain veneer restorations.
References
1. Coslett JG, Vanarsdall R, and Weisgold A. Diagnosis and classification of delayed passive eruption of the dentogingival junction in the adult. Alpha Omegan. 1977;70:24-28.
2. Dolt AH, Robbins JW. Altered passive eruption: An etiology of short clinical crowns. Quintessence Int. 1997;28:363-372.
3. Robbins JW. Differential diagnosis and treatment of excess gingival display. Pract Periodont Aesthet Dent. 1999;11(2):265-272.
4. Gillen RJ, Schwartz RS, Hilton TJ, Evans DB. An analysis of selected normative tooth proportions. Int J Prosthodont. 1994;7: 410-417.
5. Tjan AHL, Miller GD, The JG. Some esthetic factors in a smile. J Prosthet Dent. 1984;51: 24-28.
6. Konikoff BM, Johnson DC, Schenkein HA, et al. Clinical crown length of the maxillary anterior teeth preorthodontics and postorthodontics. J Perio. 2007;78(4):645-653.
7. Gottlieb B, Orban B. Active and passive eruption of teeth. J Dent Res. 1933;13:214.
8. Morrow LA, Robbins JW, Jones WL, Wilson NHF. Clinical crown length changes from age 12-19 years: A longitudinal study. J Dent. 2000; 28:469-473.
About the Author
J. William Robbins, DDS, MA
Private Practice
San Antonio, Texas
Clinical Professor
University of Texas Health Science Center
San Antonio Dental School
San Antonio, Texas