Maximum Esthetics, Strength, and Interlock Retention
Provisional restorations serve many uses during the transition from tooth preparation to final restoration.
Between tooth preparation and final restoration, provisional restorations provide esthetics, protect the patient from pain, help to maintain function such as speech and limited chewing, and help to maintain teeth position, gingival position, and gingival health.1-3
Provisional restorations are constructed of many different materials using many different techniques. They are constructed from acrylic, composite, Bis-acryl, polycarbonate, aluminum, heat-processed resin, or combinations of these materials. The materials are placed in a matrix and formed, sculpted from a block of material, or relined. Provisional restorations can be constructed directly or indirectly in the office or at a laboratory.
In the author’s experience, the restorative situation dictates which materials and techniques are used. There are single or multiple, anterior or posterior, and missing teeth to consider. Selection is based on strength, retention, esthetics, ease of construction, and cost (Table 1).
Retention versus Forces
The amount of retention a provisional will provide is a function of the surface area of the prepared tooth, the path of insertion and withdrawal, the strength of a temporary cement, the flexibility of the provisional material, and the strength of the temporary cement to the tooth and provisional surfaces.4-6 In addition, provisional material must resist fracture.
The intensity, duration, frequency, and direction of force (which includes compressive force straight down, shear force pulling upward, lateral forces on cusp inclines, and rotational forces on off-center impact) are analyzed. Ideally, a patient does not function on a provisional, but often it is unrealistic to expect that they will not to at least some extent.
Mechanical Interlocks
It is the experience of the author that retention is improved with mechanical interlocking. He invented dimple interlocking 19 years ago7 and interproximal interlocking 3 years ago. Dimple interlocks are created by drilling holes through a provisional to dimples in prepared teeth and placing composite into them. Interproximal interlocks are done by creating a slot interproximal preparation in a provisional and filling it with composite in such a manner to engage undercuts on an adjacent tooth.
Technique—Polycarbonate Provisional
The polycarbonate provisional is a preformed crown which comes in various sizes of mandibular and maxillary incisors, cuspids, and bicuspids. The polycarbonate provisional is trimmed to fit a space and then relined with acrylic to fit to a prepared tooth. It is the author’s experience that the facial surface is highly esthetic and should not be touched to maintain the high gloss so adjusting is done on mesial and distal surfaces, incisal and gingival surfaces, or from the lingual surface.8 Lingual adjustment is completed after relining so if the polycarbonate is perforated, acrylic remains.
Case One
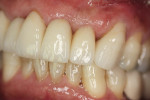
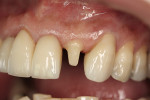
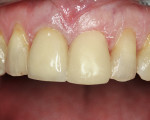
An all-porcelain crown on the maxillary left lateral incisor No. 10 was fractured (Figure 1). The crown was removed and the preparation was cleaned (Figure 2). The polycarbonate provisional was selected for its ease of construction, high strength, excellent esthetics, and it was an A2 shade. Calipers measured the mesial distal space between the cuspid and central incisor. The calipers at the determined setting measured the width of various polycarbonate crowns and the proper one was selected. It was tried on the prepared tooth but was too wide to be seated; however, it was also too short in an incisal–gingival dimension. The next larger provisional was selected knowing that an adequate amount of mesial–distal reduction could be accomplished. If the shorter provisional was selected, there would be an acrylic collar at the gingival area which would not happen with the larger polycarbonate crown.
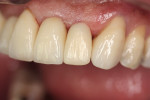
The mesial–distal surfaces were adjusted until the provisional seated. Vaseline was applied to the outer surface of the crown and to the prepared tooth so that acrylic would not adhere and chemical trauma would be minimized. A thin- to medium-viscosity mix of acrylic was placed in the provisional and it was seated on the prepared tooth. It was moved up and down in an incisal–gingival movement to disengage undercuts which would lock the acrylic upon setting. The provisional crown was removed as heat was generated by the acrylic setting. Excess acrylic was trimmed with sandpaper disks and the provisional was reseated on the tooth. The lingual occlusion was adjusted with a pear-shaped diamond bur and smoothed with a burlew wheel. The provisional was cemented with temporary cement (Figure 3).
Technique—Composite Veneered Provisional
The composite veneered provisional restoration provides maximum esthetics. It is preferred over the polycarbonate provisional when the tooth is not, or is substantially different than, an A2 shade or the tooth shape is significantly different.9,10 Composite veneering is preferred over other materials especially when they cannot match the shade of the surrounding teeth.9,10 A provisional restoration is constructed of acrylic, polycarbonate, or Bis-acryl materials in the usual method. The facial surface is reduced using an acrylic bur, sandpaper disk, or diamond bur depending on the material used. The correct shade of composite is selected and applied over the facial surface and finished.
Case Two
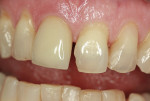
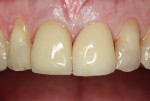
A patient fractured the maxillary right central incisor No. 8 (Figure 4). An all-porcelain zirconia crown was indicated. A Bis-acryl provisional restoration was constructed. The facial surface of the provisional crown was reduced about 1 mm to make room for the composite. Composite of an A3.5 shade was selected and rolled into a ball. The ball created a point contact to minimize trapped air as the composite spread over the facial surface. Excess was removed and final shaping was done with a composite instrument. Composite was shaped as close to the final contours as possible before light-curing. Final composite shaping and polishing was done after light-curing. Figure 5 shows the composite veneered provisional next to the final crown. Figure 6 and Figure 7 show the provisional and the final zirconia crown.
Technique—Acrylic Block
In the author’s experience, the acrylic block technique is ideal for situations that require a lot of work to construct a matrix, such as when there is a missing tooth, a tooth fractured to the height of the gingiva, or a matrix was not constructed before tooth preparation.1 Acrylic is mixed to a smooth, firm, doughy consistency, relined for an accurate fit, and hand carved. It is a quick, effective technique to construct a provisional restoration with experience and training.
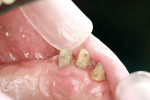
Case Three
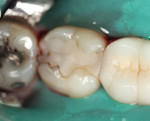
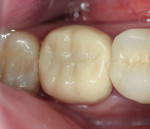
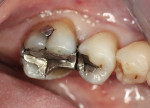
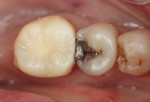
A mandibular left second molar, tooth No. 18, had a defective posterior composite (Figure 8). The composite was removed and decay was excavated. Upon final preparation, it was determined that a crown was required. A composite build-up was bonded and the tooth was prepared for a porcelain-fused-to-metal restoration. Acrylic powder was mixed into acrylic liquid in small amounts to wet all the particles. Powder was added in small increments and mixing continued until the acrylic was a doughy consistency and not sticky. Vaseline was applied to the tooth to avoid chemical trauma and acrylic adhering to the tooth.
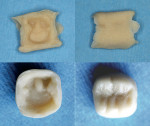
A small ball of acrylic was formed to the size of the second molar. It was pressed onto the prepared tooth such that material went interproximally and covered the facial and lingual surfaces. The patient bit to establish the occlusial height. The acrylic was removed while still in the doughy phase and a thin mix of acrylic was placed in it. The provisional was placed back on the tooth and the patient bit again. The facial and lingual acrylic layers were pressed as they expanded when the patient bit. As the acrylic hardened, the provisional was moved up and down to disengage the undercuts that acrylic would get locked into. The provisional was removed upon heat generation and setting. An acrylic bur trimmed the margins. Margins were trimmed while looking into the inner surface of the provisional. Excess acrylic was removed in the line angle areas, the facial and lingual was contoured, and the interproximal was shaped while avoiding contact areas. The marginal ridges and occlusal contours were completed.
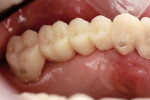
Final contouring was done while polishing with a rag wheel and flour of pumice at low speed. Facial and lingual surfaces were smoothed in mesial–distal and occlusal–gingival directions (Figure 9). The occlusal surface was polished with the edge of the wheel going into the grooves. The final provisional provided a very tight, accurate fit, strength, and good esthetics (Figure 10).
Technique—Interproximal and Dimple Interlocks
Interlocks, a term the author coined, create mechanical retention for provisional restorations.7 Dimple techniques are solid and reversible by removing composite material. The interproximal interlock engages undercuts in adjacent teeth but disengages when enough force is applied by the dentist when the provisional material flexes.
Case Four
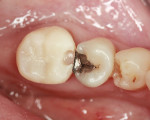
A fractured mandibular right first molar, tooth No. 30, required a crown (Figure 11). Composite was added to the fractured lingual cusp area and a triple-tray matrix formed. The tooth was prepared and a Bis-acryl provisional was constructed by placing material into the triple tray, seating it, and removing it after the initial cure (Figure 12). Bis-acryl remained elastic during the initial cure and was easily removed even if the undercuts were engaged. The provisional was trimmed and polished. A slot was cut into the mesial interproximal area (Figure 13). The provisional was cemented with temporary cement and excess was cleaned off. Composite was placed into the slot so that it engaged the undercut of the adjacent tooth to provide a mechanical lock (Figure 14). The slot extended just below the height of contour so that excess composite did not flow into the gingival area. The Bis-acryl was flexible enough that the composite would disengage when enough force was applied.
Case Five
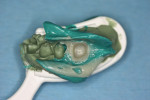
A patient presented with a defective full-arch maxillary bridge that replaced missing teeth Nos. 4, 8, and 12 through 14. The maxillary right lateral incisor, tooth No. 7, had a root fracture and required extraction. The maxillary left second molar was periodontally involved and required extraction. It was maintained during the transition phase to support a provisional restoration and would be extracted as an immediate partial denture. Study models were sent to a dental laboratory and a heat-processed resin provisional was constructed. At the laboratory, teeth on the maxillary model were reduced 1 mm to the gingival margin. The provisional was constructed on this model. Teeth must be reduced more than 1 mm to make room for acrylic to reline the provisional and prepared to the gingival margin so it can be fully seated.
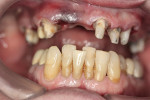
The existing bridge was removed, decay was excavated, and teeth were restored with post and cores. Final preparations were completed to accept a provisional restoration. Tooth No. 7 was extracted (Figure 15). The laboratory-processed provisional was tried over the teeth. It was difficult to get a perfect fit during the initial try-in, so several factors were evaluated. At each tooth and edentulous area, pressure was applied mesially and distally to see if a rock occurred. A rock at a tooth can occur if not enough tooth reduction occurs or reduction is above the gingival height (the height prepared on the model). Usually, more tooth reduction is done; however, reduction on the provisional at the margin is done when it is determined that the model was not reduced properly and the provisional is overextended. A rock can occur at an edentulous area if too much reduction was done on the model. Reduction on the pontic area of the provisional is done or edentulous tissue is removed, for example, when an ovate pontic is being created.
In this case, the provisional rocked on the left cuspid, tooth No. 11. Comparison to the model revealed that the model was overprepared, so reduction was done on the gingival area of the provisional. After final adjustments, a provisional would still have movement as there would be room for relining with acrylic. The occlusion and general seating should be close to ideal when a patient occludes onto the provisional before relining.
Vaseline was applied to the prepared teeth and to all outer surfaces of the provisional so that acrylic would not adhere. Acrylic was mixed to a medium consistency. It would flow, slowly, when it was the ideal consistency. The abutment teeth of the provisional were filled with acrylic and the provisional was placed over the prepared teeth. It was pressed in a gingival position to engage the teeth but left a few millimeters short of being fully seated. The patient then bit onto the provisional to fully seat it into the ideal position, guided by the occlusion. The provisional was moved up and down after a minute to minimize the chance of getting acrylic locked into undercuts.
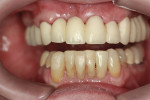
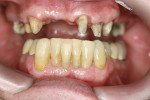
The provisional was removed and excess acrylic was trimmed with an acrylic bur and sandpaper disks. It was tried in the mouth several times to do final adjustments to occlusion and fit. The provisional was polished and finished (Figure 16). At 7 weeks after initial placement, the gingiva had healed nicely (Figure 17).
Permanent reversible fixation was completed with the dimple interlocks. Holes were drilled through a provisional at preselected teeth. Dimples would be placed into the teeth so there needed to be room for dimples without causing too much tooth destruction or pulp damage. The teeth in this case were all endodontically treated and would not be affected by dimples. It is ideal to have a tooth distal and a tooth mesial to dimpled teeth to minimize rocking and to have two dimples on each side of the arch.
The provisional restoration was placed over the teeth and a round, #6 bur in a slow-speed handpiece was placed into the holes through the temporary to form dimples. The bur drilled a shallow dimple of less than half the bur length for each hole (Figure 18). The provisional was removed and the dimples were refined. The provisional was cemented with temporary cement. Cement was cleaned with a No. 6 round bur from the holes and dimples and then composite was placed. The composite excess was removed and the remainder was light-cured (Figure 19). The composite was removed with a bur when the provisional was to be removed.
Conclusion
The use of multiple techniques can maximize provisional restorations for different situations. The combination of health, function, esthetics, cost, time, ease of use, retentive requirements, and strength are all determining factors.
Author’s Note:
Case photography used with permission of https://www.provisionalrestorations.com.
Disclosure
Dr. Chalifoux is the owner of provisional restorations.com.
References
1. Schwedhelm ER. Direct technique for the fabrication of acrylic provisional restorations. J Contemp Dent Pract. 2006;7(1):157-173.
2. Chalifoux PR. Provisional restorations using the Provipont system. Signature. 1994; Winter:8-13.
3. Donovan T, Cho G. Blueprint for Success. J Can Dent Assoc. 1999;65:272-275.
4. Kim Y, Yamashita J, Shotwell JL, et al. The comparison of provisional luting agents and abutment surface roughness on the retention of provisional implant-supported crowns. J Prosthet Dent. 2006;95(6):450-455.
5. Balkenhol M, Mautner MC, Ferger P, Wöstmann B. Mechanical properties of provisional crown and bridge materials: chemical-curing versus dual-curing systems. J Dent. 2008;36(1):15-20.
6. Yilmaz A, Baydaş S. Fracture resistance of various temporary crown materials. J Contemp Dent Pract. 2007;8(1):44-51.
7. Chalifoux PR. Reversible permanent fixation of temporary crown and bridges. Pract Perio Aesthet Dent. 1990;1(6):18-21.
8. Lu DP. Construction of temporary fixed partial dentures with prefabricated polycarbonate temporary crowns. Gen Dent. 1988;36(5):400-401.
9. Chalifoux PR. Aesthetics of the single anterior temporary crown. Pract Periodontics Aesthet Dent. 1991;3(5):15-18.
10. Chalifoux PR. Temporary crown and fixed partial dentures: new methods to achieve esthetics. J Prosthet Dent. 1989;61(4):411-414.
About the Author
Paul R. Chalifoux, DDS
Private Practice
Wellesley, Massachusetts