Instant Orthodontics
A case report using direct resin composite for malpositioned anterior teeth.
Modern resin composite systems provide excellent strength, smoothness, color stability, and longevity. Because they often require minimal or no tooth structure removal, composite resin restorations are the treatment of choice in many unesthetic situations, including those of malpositioned anterior teeth.
There are several treatment alternatives for slight-to-moderate anterior tooth malpositioning. The first option to be considered should be orthodontic treatment, especially in younger patients with unrestored teeth. However, the cost or length of orthodontic treatment often makes this treatment undesirable for many patients. Recent literature suggests that minor tooth-alignment issues, such as facio-lingual displacement and crowding, may be resolved with indirect porcelain veneer restorations.1,2 However, others have questioned the value of this treatment because of the nonconservative nature of the indirect preparations.3,4
There are many cases where, in lieu of orthodontics, less-aggressive procedures such as bleaching and direct-bonded restorations can be combined to achieve excellent esthetic results with good longevity at an affordable cost. In many cases, composite resin restorations require minimal or, in some cases, no tooth structure removal. They also can be repaired or replaced more easily and less expensively then porcelain veneer restorations.1
This article will describe a malalignment case that was successfully treated with composite resin and discusses the steps that are critical to success with this procedure.
History
The patient, a 64-year-old woman, presented for an esthetic consultation stating that she wanted “straight teeth.” The patient confessed that she always covered her mouth when she laughed. She did not want to go through orthodontic treatment at her age and was seeking alternative treatment. Her dental history revealed regular dental visits with several moderate-sized direct restorations and crowns on posterior teeth.
Clinical Findings
A comprehensive examination of the patient revealed unrestored anterior teeth, good periodontal health, and no apparent areas of decay. Her gingiva was healthy with no bleeding upon probing. She presented with an Angle Class I posterior relationship and a 50% overbite in the anterior. The temporomandibular joint had no history of sounds or pain. Teeth Nos. 7 through 10 were in function only during protrusive movement.
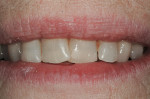
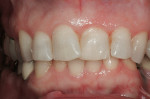
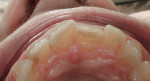
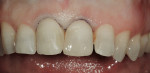
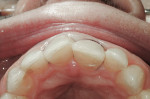
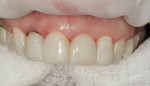
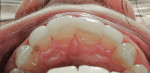
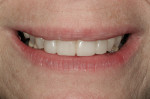
The esthetic findings included malaligned maxillary anterior teeth. Tooth No. 8 was rotated with the mesial line angle facial to the rest of the arch curvature. Tooth No. 9 was lingually positioned with a small overlap of tooth No. 8 on the mesial. The incisal third of tooth No. 10 was facial to the rest of the arch curvature (Figure 1 and Figure 2). The patient had a low lip-line smile covering the gingival areas of the maxillary anterior teeth (Figure 3).
Treatment Plan
The patient was provided with all alternative treatments options including the advantages, disadvantages, and relative costs of each treatment. She declined orthodontic treatment and selected the options of bleaching followed by realignment with direct resin composites.
Treatment
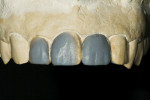
Preplanning is crucial to success in any dental procedure and direct realignment is no exception. Study casts are important to the success of composite resin restorations for several reasons in malalignment situations. First, the clinician can determine if any tooth structure needs to be removed from the malpositioned teeth before restoration placement. Second, an ideal wax-up can be performed, which helps the clinician to visualize the thickness and contours to be developed during the placement of the resin composite (Figure 4 and Figure 5). Wax-up models are also important for patient education and decision-making. An additional mock-up with resin composite can be done at chairside if desired.
An important step in restoring slight-to-moderate tooth malpositioning with resin composite is preoperative tooth whitening. To correct the malalignment to the desired arch curvature, enamel recontouring is often needed. To avoid creating a shade change difference in this case, preoperative tooth whitening is important. Color change after teeth whitening occurs throughout the dentin.5-7 By lightening the dentin shade similar to that of the enamel, any recontouring and thinning of the enamel does not produce a higher chroma effect. This establishes a good basic tooth color, thus eliminating the need for a thicker layer of composite to disguise discolorations.
Preoperative bleaching trays with 10% carbamide peroxide (Opalescence®, Ultradent Products Inc, https://www.ultradent.com) were delivered to the patient with instructions to use overnight. The tooth color recorded at baseline was shade A3 using the Vitapan® Classical Shade Guide (Vident, https://www.vident.com). After 2 weeks of use, the teeth had lightened to an A1 shade. The patient was satisfied with the shade, and was scheduled for composite resin veneer placement 2 weeks after bleaching completion.
The four maxillary incisors were restored to create the esthetic illusion of alignment. The mesio-facial line angle of tooth No. 8 and the incisal facial third of tooth No. 9 were reshaped using a medium-grit diamond. Figure 6 and Figure 7 show the maxillary incisors after the enamel recontouring. Notice that the overlap of tooth No. 8 was corrected before placement of the direct restorations. The teeth were isolated (OptraGate, Ivoclar Vivadent, https://www.ivoclarvivadent.com) and clear matrix strips were used to isolate adjacent teeth. Bonding was done one tooth at a time. A three-step, etch-and-rinse bonding system (OptiBond® FL, Kerr Dental, https://www.kerrdental.com), was used. Because all bonding surfaces were in enamel, the surface was thoroughly dried and only the adhesive was used. Teeth were etched with 37% phosphoric acid for 20 seconds, rinsed, and thoroughly dried. Adhesive was applied and light-cured for 20 seconds.
A nanofill composite resin composite (Filtek™ Supreme Plus, 3M ESPE, https://www.3mespe.com) in the A1 body shade was used to individually restore the facial contours of teeth Nos. 7 through 10. The material was placed and smoothed using a Gold Microfil Instrument (Almore, https://www.almore.com), an IPC instrument (Cosmedent, https://www.cosmedent.com) and a #3 sable brush. Composite resin additions also were individually placed to align the lingual contour of teeth Nos. 8 and 10. Placement of composite resin on the lingual surfaces is an important step for realignment as it helps to create a uniform thickness of the incisal edges when viewed from different angles. To accommodate thicker incisal edges, such as those established with this patient, the incisal edge needs to be inclined toward the lingual to result in better esthetics. Each restoration was light-cured for 40 seconds.
Contouring was done with finishing burs, coarse finishing discs (Sof-Lex™ XT, 3M ESPE), and finishing diamonds. Finishing strips (Epitex™ Strips, GC America, https://www.gcamerica.com) were used to polish the interproximal surfaces (Figure 8). Final polishing was done with polishing cups and points (Diacomp®, Brasseler USA, https://www.brasselerusa.com) followed by a polishing paste (Enamelize®, Cosmedent) using felt discs (FlexiBuff , Cosmedent).
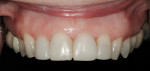
The finished composite resin restorations are seen in Figure 9 and Figure 10. The patient was very pleased with the outcome. The postoperative smile 11 months after treatment is shown in Figure 11.
Conclusion
This article describes an alternative treatment to orthodontics using resin composite. An outstanding cosmetic result can be achieved with resin-based composite restorations. Proper case selection, diagnostic casts, wax-up, and preoperative tooth whitening are all essential steps for success.
References
1. Christensen GJ. Veneer mania. J Am Dent Assoc. 2006;137(8):1161-1163.
2. Jacobson N, Frank CA. The myth of instant orthodontics: an ethical quandary. J Am Dent Assoc. 2008;139(4):424-434.
3. Heymann HO, Kokich VG. Instant orthodontics: viable treatment option or “quick fix” cop-out? J Esthet Restor Dent. 2002;14(5): 263-264.
4. Spear FM. The esthetic correction of anterior dental mal-alignment conventional vs. instant (restorative) orthodontics. J Calif Dent Assoc. 2004;32(2):133-141.
5. Joiner A, Thakker G, Cooper Y. Evaluation of a 6% hydrogen peroxide tooth whitening gel on enamel and dentine microhardness in vitro. J Dent. 2004;32(Suppl 1):27-34.
6. McCaslin AJ, Haywood VB, Potter BJ, et al. Assessing dentin color changes from nightguard vital bleaching. J Am Dent Assoc. 1999;130(10):1485-1490.
7. White DJ, Kozak KM, Zoladz JR, et al. Effects of tooth-whitening gels on enamel and dentin ultrastructure—a confocal laser scanning microscopy pilot study. Compend Contin Educ Dent. 2000;29(Suppl):S29-S34.
About the Authors
Ana Elashvili, DDS, MS
Assistant Professor
Department of Restorative Dentistry
University of Colorado School of Dental Medicine
Aurora, Colorado
Gerald E. Denehy, DDS, MS
Professor and Head
Department of Operative Dentistry
The University of Iowa, College of Dentistry
Iowa City, Iowa